Abstract
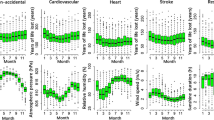
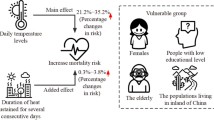
Few studies have examined the attributable fraction (AF) of temperature to mortality and Years of Life Lost (YLL), especially in developing countries. This study aims to explore the short-term effect of the cold and hot temperatures on the cause-specific YLL and mortality, discover the attributable contributions from the temperature variations, and identify the vulnerable populations in Weifang, China. Daily registered death information and meteorological data over the period 2010–2016 were obtained in Weifang, a northern Chinese city. Generalized additive Poisson and Gaussian regression models were used to assess the impacts of temperatures on both mortality and YLL, explore the AF of the temperature variations on mortality, after adjusting for other covariates. Both hot and cold temperatures have had significant negative impacts on cause-specific mortality counts and YLL, with heat presented an acute and short effect and the cold temperatures had delayed effects and lasted for several days. In terms of the attributable fraction calculations, the contributions from cold effects was higher than that of hot effects on non-accidental, cardiovascular, and respiratory deaths (YLL 10.88 vs. 1.23%, 19.58 vs. 1.71%, and 14.47 vs. 3.05%; mortality 13.97 vs. 1.65%, 19.20 vs. 1.59%, and 14.89 vs. 3.09%), respectively. The elderly and women and people with low education level were the most vulnerable. The findings will provide important scientific evidences and policy implications for developing adaptation strategies to reduce the adverse effect of cold and hot exposure in Weifang, in terms of resource allocation, healthcare workforce capacity building, and community health education, especially for the vulnerable groups.




Similar content being viewed by others
Abbreviations
- AF:
-
Attributable fraction
- YLL:
-
Years of life lost
- RR:
-
Relative risk
- OR:
-
Odds ratio
- AN:
-
Attributable number
- DALYs:
-
Disability-adjusted-life-years
- CDC:
-
Center for Disease Control and Prevention
- ICD:
-
International Classification of Diseases
- WHO:
-
World Health Organization
- GAM:
-
Generalized Additive Model
- DLNM:
-
Distributed lag nonlinear model
- MMT:
-
Minimum-mortality temperature
- CI:
-
Confidence interval
- TV:
-
Temperature variability
References
Basu R (2009) High ambient temperature and mortality: a review of epidemiologic studies from 2001 to 2008. Environ Health 8:40
Chen K et al (2016) Urbanization level and vulnerability to heat-related mortality in Jiangsu Province, China. Environ Health Perspect 124:1863–1869
Chen R et al (2018) Association between ambient temperature and mortality risk and burden: time series study in 272 main Chinese cities. BMJ 363:k4306
Curriero FC, Heiner KS, Samet JM, Zeger SL, Strug L, Patz JA (2002) Temperature and mortality in 11 cities of the eastern United States American. J Epidemiol 155:80–87
Donaldson GC, Keatinge WR, Saunders RD (2003) Cardiovascular responses to heat stress and their adverse consequences in healthy and vulnerable human populations. Int J Hyperth 19:225–235
Ezzati M, Hoorn SV, Rodgers A, Lopez AD, Mathers CD, Murray CJ (2003) Estimates of global and regional potential health gains from reducing multiple major risk factors. Lancet 362:271–280
Gasparrini A, Leone M (2014) Attributable risk from distributed lag models. BMC Med Res Methodol 14:55
Gasparrini A, Armstrong B, Kenward MG (2012) Multivariate meta-analysis for non-linear and other multi-parameter associations. Stat Med 31:3821–3839
Gasparrini A, Guo Y, Hashizume M, Lavigne E, Zanobetti A, Schwartz J, Tobias A, Tong S, Rocklöv J, Forsberg B, Leone M, de Sario M, Bell ML, Guo YLL, Wu CF, Kan H, Yi SM, de Sousa Zanotti Stagliorio Coelho M, Saldiva PHN, Honda Y, Kim H, Armstrong B (2015) Mortality risk attributable to high and low ambient temperature: a multicountry observational study. Lancet 386:369–375
Gasparrini A, Guo Y, Sera F, Vicedo-Cabrera AM, Huber V, Tong S, de Sousa Zanotti Stagliorio Coelho M, Nascimento Saldiva PH, Lavigne E, Matus Correa P, Valdes Ortega N, Kan H, Osorio S, Kyselý J, Urban A, Jaakkola JJK, Ryti NRI, Pascal M, Goodman PG, Zeka A, Michelozzi P, Scortichini M, Hashizume M, Honda Y, Hurtado-Diaz M, Cesar Cruz J, Seposo X, Kim H, Tobias A, Iñiguez C, Forsberg B, Åström DO, Ragettli MS, Guo YL, Wu CF, Zanobetti A, Schwartz J, Bell ML, Dang TN, van DD, Heaviside C, Vardoulakis S, Hajat S, Haines A, Armstrong B (2017) Projections of temperature-related excess mortality under climate change scenarios. Lancet Planet Health 1:e360–e367
Giorgini P, Di Giosia P, Petrarca M, Lattanzio F, Stamerra CA, Ferri C (2017) Climate changes and human health: a review of the effect of environmental stressors on cardiovascular diseases across epidemiology and biological mechanisms. Curr Pharm Des 23:3247–3261
Hajat S, Kovats RS, Lachowycz K (2007) Heat-related and cold-related deaths in England and Wales: who is at risk? Occup Environ Med 64:93–100
Hanna EG, Kjellstrom T, Bennett C, Dear K (2011) Climate change and rising heat: population health implications for working people in Australia. Asia-Pac J Public He 23:14S–126S
Huang C, Barnett AG, Wang X, Tong S (2012a) Effects of extreme temperatures on years of life lost for cardiovascular deaths: a time series study in Brisbane, Australia. Circ Cardiovasc Qual Outcomes 5:609–614
Huang C, Barnett AG, Wang X, Tong S (2012b) The impact of temperature on years of life lost in Brisbane, Australia. Nat Clim Chang 2:265–270
Huang C, Barnett AG, Xu Z, Chu C, Wang X, Turner LR, Tong S (2013) Managing the health effects of temperature in response to climate change: challenges ahead. Environ Health Perspect 121:415–419
Intergovernmental Panel on Climate Change, (2015) Climate change 2014: mitigation of climate change. Cambridge University, England
Kysely J, Pokorna L, Kyncl J, Kriz B (2009) Excess cardiovascular mortality associated with cold spells in the Czech Republic. BMC Public Health 9:19
Li J, Xu X, Wang J, Zhao Y, Song XP, Liu ZD, Cao LN, Jiang BF, Liu QY (2016a) Analysis of a community-based intervention to reduce heat-related illness during heat waves in Licheng, China: a quasi-experimental study. Biomed Environ Sci 29:802–813
Li Q, Wang HJ, Song Y, Ma J, Song JY, Guo Y (2016b) Association between children's forced vital capacity and long-term exposure to local ambient temperature in China: a national cross-sectional survey. Sci Total Environ 557-558:880–887
Li G, Huang J, Xu G, Pan X, Qian X, Xu J, Zhao Y, Zhang T, Liu Q, Guo X, He T (2017a) Temporal variation in associations between temperature and years of life lost in a southern China city with typical subtropical climate. Sci Rep-UK 7:4650
Li J, Xu X, Yang J, Liu Z, Xu L, Gao J, Liu X, Wu H, Wang J, Yu J, Jiang B, Liu Q (2017b) Ambient high temperature and mortality in Jinan, China: a study of heat thresholds and vulnerable populations. Environ Res 156:657–664
Li J et al (2018) Impact of ambient temperature on chronic non-communicable disease mortality in Jinan, China during 2007-2013: an attributable risk study. J Shandong University (Health Sci) 56(8):76–87
Liang H, Qiu H, Tian L (2018) Short-term effects of fine particulate matter on acute myocardial infarction mortality and years of life lost: a time series study in Hong Kong. Sci Total Environ 615:558–563
Liu C, Yavar Z, Sun Q (2015) Cardiovascular response to thermoregulatory challenges. Am J Physiol Heart Circ Physiol 309:H1793–H1812
Ma W, Chen R, Kan H (2014) Temperature-related mortality in 17 large Chinese cities: how heat and cold affect mortality in China. Environ Res 134:127–133
Madaniyazi L, Zhou Y, Li S, Williams G, Jaakkola JJK, Liang X, Liu Y, Wu S, Guo Y (2016) Outdoor temperature, heart rate and blood pressure in Chinese adults: effect modification by individual characteristics. Sci Rep-UK 6:21003
McKenna MT, Michaud CM, Murray CJ, Marks JS (2005) Assessing the burden of disease in the United States using disability-adjusted life years. Am J Prev Med 28:415–423
Mourtzoukou EG, Falagas ME (2007) Exposure to cold and respiratory tract infections. Int J Tuberc Lung Dis 11:938–943
Phung D, Guo Y, Nguyen HT, Rutherford S, Baum S, Chu C (2016) High temperature and risk of hospitalizations, and effect modifying potential of socio-economic conditions: a multi-province study in the tropical Mekong Delta region. Environ Int 92-93:77–86
Scovronick N, Sera F, Acquaotta F, Garzena D, Fratianni S, Wright CY, Gasparrini A (2018) The association between ambient temperature and mortality in South Africa: a time-series analysis. Environ Res 161:229–235
Shaposhnikov D, Revich B, Gurfinkel Y, Naumova E (2014) The influence of meteorological and geomagnetic factors on acute myocardial infarction and brain stroke in Moscow, Russia. Int J Biometeorol 58:799–808
Steenland K, Armstrong B (2006) An overview of methods for calculating the burden of disease due to specific risk factors. Epidemiology 17:512–519
Xiang et al. (2018) Correlates of occupational heat-induced illness costs: case study of South Australia 2000 to 2014. J Occup Environ Med 60(9):e463–e469
Yang J, Ou CQ, Guo Y, Li L, Guo C, Chen PY, Lin HL, Liu QY (2015a) The burden of ambient temperature on years of life lost in Guangzhou, China. Sci Rep-UK 5:12250
Yang J, Yin P, Zhou M, Ou CQ, Guo Y, Gasparrini A, Liu Y, Yue Y, Gu S, Sang S, Luan G, Sun Q, Liu Q (2015b) Cardiovascular mortality risk attributable to ambient temperature in China. Heart 101:1966–1972
Yang J et al (2016) The burden of stroke mortality attributable to cold and hot ambient temperatures: Epidemiological evidence from China. Environ Int 92-93:232-238
Yang J, Zhou M, Li M, Liu X, Yin P, Sun Q, Wang J, Wu H, Wang B, Liu Q (2018) Vulnerability to the impact of temperature variability on mortality in 31 major Chinese cities. Environ Pollut 239:631–637
Zhang Y, Peng M, Wang L, Yu C (2018a) Association of diurnal temperature range with daily mortality in England and Wales: a nationwide time-series study. Sci Total Environ 619-620:291–300
Zhang Y, Yu C, Peng M, Zhang L (2018b) The burden of ambient temperature on years of life lost: a multi-community analysis in Hubei. China Sci Total Environ 621:1491–1498
Zhang Y, Xiang Q, Yu Y, Zhan Z, Hu K, Ding Z (2019) Socio-geographic disparity in cardiorespiratory mortality burden attributable to ambient temperature in the United States. Environ Sci Pollut Res Int 26(1):694–705
Zhu J, Zhang X, Zhang X, Dong M, Wu J, Dong Y, Chen R, Ding X, Huang C, Zhang Q, Zhou W (2017) The burden of ambient air pollution on years of life lost in Wuxi, China, 2012-2015: a time-series study using a distributed lag non-linear model. Environ Pollut 224:689–697
Acknowledgements
This study was supported by the Social Science Planning Research Project of Shandong Province (18CQXJ18), Medicine and Health of Shandong Province for Science and Technology Development Program (2017WS703, 2016WS0664), Science and Technology Project of Shandong Health Science and Technology Association, and State Key Laboratory of Infectious Disease Prevention and Control Program of China (2018SKLID306). The authors are grateful to the Weifang Center for Disease Control and Prevention sharing with us the information needed for this study.
Funding
This study was supported by the Science and Technology Development Program for Medicine and Health of Shandong Province (2017WS703, 2016WS0664), Social Science Planning Research Project of Shandong Province (18CQXJ18), and State Key Laboratory of Infectious Disease Prevention and Control Program of China (2018SKLID306).
Author information
Authors and Affiliations
Contributions
JL and XX conceived and designed the study; ZC, XH, NL, and XM collected the data; ZC, XH, CW, and QW performed the data analysis; JL and XX drafted the manuscript; QL and PB provided significant intellectual advice. PB helped revise the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Xin Xu, Zuosen Chen, and Xiyuan Huo are co-first authors
Highlights
• To our knowledge, the first few studies to explore the attributable fraction of ambient temperature on both mortality and YLL in China.
• Cold rather than heat contributed substantially to cause-specific YLLs and mortality.
• AF vulnerability on YLL and mortality to ambient temperature varied not only by classification of diseases, but also by demographic characteristics.
• Findings are important for public health decision-making and resource allocation due to extreme temperature in China.
Electronic supplementary material
ESM 1
(DOCX 39 kb).
Rights and permissions
About this article
Cite this article
Xu, X., Chen, Z., Huo, X. et al. The effects of temperature on human mortality in a Chinese city: burden of disease calculation, attributable risk exploration, and vulnerability identification. Int J Biometeorol 63, 1319–1329 (2019). https://doi.org/10.1007/s00484-019-01746-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00484-019-01746-6