Abstract
Background
The syndrome of inappropriate antidiuretic hormone (SIADH) is usually treated with fluid restriction. This can be challenging in patients with obligate fluid intake for nutrition or medication. Pharmaceutical treatment with tolvaptan and urea is available but minimal paediatric data are available. We review the efficacy and safety of tolvaptan and urea in paediatric patients with SIADH.
Methods
Retrospective review of paediatric inpatients with clinical diagnosis of SIADH. Patients were identified from pharmacy records based on tolvaptan and urea prescriptions. Relevant information was extracted from patient electronic records. The main outcome measures included the number of days to sodium normalisation, the daily change in plasma sodium concentration, and the maximum increase of plasma sodium concentration in 24 h. Reported side effects were captured.
Results
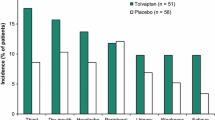
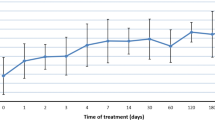
Thirteen patients received tolvaptan and six urea. Five patients had both agents (tolvaptan converted to urea). Tolvaptan led to plasma sodium normalisation in 10/13 (77%) within 6 days (median 2.5 days, range [1, 6]), with a median change of sodium concentration of 7 mmol/L (− 1, 14) within the first 24 h of treatment. Three patients experienced a change in plasma sodium > 10 mmol/l/day but had no apparent side effects. Urea led to sodium normalisation in 5/6 (83%) patients. The median number of days to normalisation with urea was 2 (1, 10) with a median change of plasma sodium concentration of 2 mmol/L (− 1, 6) within the first 24 h. All patients tolerated tolvaptan and/or urea without unexpected side effects.
Conclusions
Tolvaptan and urea appear to be safe and effective when fluid restriction is challenging in paediatric SIADH.
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information



Similar content being viewed by others
References
Ellison DH, Berl T (2007) Clinical practice. The syndrome of inappropriate antidiuresis. N Engl J Med 356:2064–2072. https://doi.org/10.1056/NEJMcp066837
Bockenhauer D, Zieg J (2014) Electrolyte disorders. Clin Perinatol 41:575–590. https://doi.org/10.1016/j.clp.2014.05.007
Downie ML, Lopez Garcia SC, Kleta R, Bockenhauer D (2021) Inherited tubulopathies of the kidney: insights from genetics. Clin J Am Soc Nephrol 16:620–630. https://doi.org/10.2215/CJN.14481119
Smith D, Moore K, Tormey W, Baylis PH, Thompson CJ (2004) Downward resetting of the osmotic threshold for thirst in patients with SIADH. Am J Physiol Endocrinol Metab 287:E1019–E1023. https://doi.org/10.1152/ajpendo.00033.2004
Chehade H, Rosato L, Girardin E, Cachat F (2012) Inappropriate antidiuretic hormone secretion: long-term successful urea treatment. Acta Paediatr 101:e39–e42. https://doi.org/10.1111/j.1651-2227.2011.02382.x
Dufek S, Booth C, Carroll A, Van’t Hoff W, Kleta R, Bockenhauer D (2016) Urea is successful in treating inappropriate antidiuretic hormone secretion in an infant. Acta Paediatr 106:513–515. https://doi.org/10.1111/apa.13697
Decaux G, Brimioulle S, Genette F, Mockel J (1980) Treatment of the syndrome of inappropriate secretion of antidiuretic hormone by urea. Am J Med 69:99–106. https://doi.org/10.1016/0002-9343(80)90506-9
Huang EA, Feldman BJ, Schwartz ID, Geller DH, Rosenthal SM, Gitelman SE (2006) Oral urea for the treatment of chronic syndrome of inappropriate antidiuresis in children. J Pediatr 148:128–131. https://doi.org/10.1016/j.jpeds.2005.08.031
Bichet DG (2012) What is the role of vaptans in routine clinical nephrology? Clin J Am Soc Nephrol 7:700–703. https://doi.org/10.2215/CJN.02990312
Aperis G, Alivanis P (2011) Tolvaptan: a new therapeutic agent. Rev Recent Clin Trials 6:177–188
Tuli G, Tessaris D, Einaudi S, De Sanctis L, Matarazzo P (2017) Tolvaptan treatment in children with chronic hyponatremia due to inappropriate antidiuretic hormone secretion: a report of three cases. J Clin Res Pediatr Endocrinol 9:288–292. https://doi.org/10.4274/jcrpe.4531
Marx-Berger D, Milford DV, Bandhakavi M, Van’t Hoff W, Kleta R, Dattani M, Bockenhauer D (2016) Tolvaptan is successful in treating inappropriate antidiuretic hormone secretion in infants. Acta Paediatr 105:e334–e337. https://doi.org/10.1111/apa.13415
Singh S, Bohn D, Carlotti AP, Cusimano M, Rutka JT, Halperin ML (2002) Cerebral salt wasting: truths, fallacies, theories, and challenges. Crit Care Med 30:2575–2579
Bockenhauer D, Aitkenhead H (2011) The kidney speaks: interpreting urinary sodium and osmolality. Arch Dis Child Educ Pract Ed 96:223–227. https://doi.org/10.1136/archdischild-2011-300115
Author information
Authors and Affiliations
Contributions
D.B conceptualised and supervised the project. F.V. and D.B. designed the study, collected, analysed, interpreted data and wrote the paper. D.A. and A.F. collected data, C.L. R.A. M.D, H.G., R.T., S.S. contributed data. All authors contributed to data interpretation, final manuscript preparation and reviewed the final version prior to submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Veligratli, F., Alexandrou, D., Shah, S. et al. Tolvaptan and urea in paediatric hyponatraemia. Pediatr Nephrol 39, 177–183 (2024). https://doi.org/10.1007/s00467-023-06091-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06091-w