Abstract
Background
Gastroesophageal reflux disease (GERD) is a possible side effect of sleeve gastrectomy (SG). However, procedure selection for patients with GERD and risk factors for morbidity after bypass surgeries is complex. For patients with a preoperative GERD diagnosis, literature related to worsening postoperative symptoms is discordant.
Objective
This study evaluated the effects of SG on patients with pre-operative GERD confirmed through pH testing.
Setting
University Hospital, United States.
Methods
This was a single-center case-series. SG patients with preoperative pH testing were compared based on DeMeester scoring. Preoperative demographics, endoscopy results, need for conversion surgery, and changes in gastrointestinal quality of life (GIQLI) scores were compared. Two-sample independent t-tests assuming unequal variances were used for statistical analysis.
Results
Twenty SG patients had preoperative pH testing. Nine patients were GERD positive; median DeMeester score 26.7 (22.1–31.15). Eleven patients were GERD negative, with a median DeMeester score of 9.0 (4.5–13.1). The two groups had similar median BMI, preoperative endoscopic findings and use of GERD medications. Concurrent hiatal hernia repair was performed in 22% of GERD positive vs. 36% of GERD negative patients, (p = 0.512). Two patients in the GERD positive cohort required conversion to gastric bypass (22%), while none in the GERD negative cohort did. No significant postoperative differences were noted in GIQLI, heartburn, or regurgitation symptoms.
Conclusion
Objective pH testing may allow the differentiation of patients who would be higher risk for need for conversion to gastric bypass. For patients with mild symptoms, but negative pH testing, SG may represent a durable option.
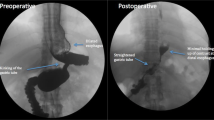
Graphical Abstract

Similar content being viewed by others
References
Carlin AM, Zeni TM, English WJ et al (2013) The comparative effectiveness of sleeve gastrectomy, gastric bypass, and adjustable gastric banding procedures for the treatment of morbid obesity. Ann Surg 257(5):791–797. https://doi.org/10.1097/SLA.0b013e3182879ded
Soricelli E, Iossa A, Casella G, Abbatini F, Calì B, Basso N (2013) Sleeve gastrectomy and crural repair in obese patients with gastroesophageal reflux disease and/or hiatal hernia. Surg Obes Relat Dis 9(3):356–361. https://doi.org/10.1016/j.soard.2012.06.003
Tutuian R (2011) Obesity and GERD: pathophysiology and effect of bariatric surgery. Curr Gastroenterol Rep 13(3):205–212. https://doi.org/10.1007/s11894-011-0191-y
Mandeville Y, Van Looveren R, Vancoillie PJ et al (2017) Moderating the enthusiasm of sleeve gastrectomy: up to fifty percent of reflux symptoms after ten years in a consecutive series of one hundred laparoscopic sleeve gastrectomies. Obes Surg 27(7):1797–1803. https://doi.org/10.1007/s11695-017-2567-z
Sheppard CE, Sadowski DC, de Gara CJ, Karmali S, Birch DW (2015) Rates of reflux before and after laparoscopic sleeve gastrectomy for severe obesity. Obes Surg 25(5):763–768. https://doi.org/10.1007/s11695-014-1480-y
Carter PR, LeBlanc KA, Hausmann MG, Kleinpeter KP, deBarros SN, Jones SM (2011) Association between gastroesophageal reflux disease and laparoscopic sleeve gastrectomy. Surg Obes Relat Dis 7(5):569–572. https://doi.org/10.1016/j.soard.2011.01.040
Himpens J, Dapri G, Cadière GB (2006) A prospective randomized study between laparoscopic gastric banding and laparoscopic isolated sleeve gastrectomy: results after 1 and 3 years. Obes Surg 16(11):1450–1456. https://doi.org/10.1381/096089206778869933
Peterli R, Wölnerhanssen BK, Vetter D et al (2017) Laparoscopic sleeve gastrectomy versus Roux-Y-Gastric bypass for morbid obesity-3-year outcomes of the prospective randomized swiss multicenter bypass or sleeve study (SM-BOSS). Ann Surg 265(3):466–473. https://doi.org/10.1097/SLA.0000000000001929
Daes J, Jimenez ME, Said N, Dennis R (2014) Improvement of gastroesophageal reflux symptoms after standardized laparoscopic sleeve gastrectomy. Obes Surg 24(4):536–540. https://doi.org/10.1007/s11695-013-1117-6
Pallati PK, Shaligram A, Shostrom VK, Oleynikov D, McBride CL, Goede MR (2014) Improvement in gastroesophageal reflux disease symptoms after various bariatric procedures: review of the Bariatric Outcomes Longitudinal Database. Surg Obes Relat Dis 10(3):502–507. https://doi.org/10.1016/j.soard.2013.07.018
DuPree CE, Blair K, Steele SR, Martin MJ (2014) Laparoscopic sleeve gastrectomy in patients with preexisting gastroesophageal reflux disease: a national analysis. JAMA Surg 149(4):328–334. https://doi.org/10.1001/jamasurg.2013.4323
Peterli R, Wölnerhanssen BK, Peters T et al (2018) Effect of laparoscopic sleeve gastrectomy vs laparoscopic Roux-en-Y gastric bypass on weight loss in patients with morbid obesity: the SM-BOSS Randomized Clinical Trial. JAMA 319(3):255–265. https://doi.org/10.1001/jama.2017.20897
Ashrafi D, Osland E, Memon MA (2020) Bariatric surgery and gastroesophageal reflux disease. Ann Transl Med 8(Suppl 1):S11. https://doi.org/10.21037/atm.2019.09.15
Gorodner V, Buxhoeveden R, Clemente G, Solé L, Caro L, Grigaites A (2015) Does laparoscopic sleeve gastrectomy have any influence on gastroesophageal reflux disease? Preliminary results. Surg Endosc 29(7):1760–1768. https://doi.org/10.1007/s00464-014-3902-2
Del Genio G, Tolone S, Limongelli P et al (2014) Sleeve gastrectomy and development of “de novo” gastroesophageal reflux. Obes Surg 24(1):71–77. https://doi.org/10.1007/s11695-013-1046-4
Rebecchi F, Allaix ME, Giaccone C, Ugliono E, Scozzari G, Morino M (2014) Gastroesophageal reflux disease and laparoscopic sleeve gastrectomy: a physiopathologic evaluation. Ann Surg 60(5):909–915. https://doi.org/10.1097/SLA.0000000000000967
Quake SYL, Mohammadi-Zaniani G, Musbahi A, Old O, Courtney M, Small P (2022) Routine use of esophago-gastro-duodenoscopy (EGD) in bariatric surgery-an international survey of our current practice. Obes Surg. https://doi.org/10.1007/s11695-022-06252-0.
Imam A, Asfour G, Imam R et al (2021) Hiatal hernia evaluation before bariatric surgery: should it be routinely done? Obes Surg 31(3):1013–1020. https://doi.org/10.1007/s11695-020-05092-0
Ghassemian AJ, MacDonald KG, Cunningham PG et al (1997) The workup for bariatric surgery does not require a routine upper gastrointestinal series. Obes Surg 7(1):16–18. https://doi.org/10.1381/096089297765556169
Georgia D, Stamatina T, Maria N et al (2017) 24-h Multichannel intraluminal impedance pH-metry 1 year after laparocopic sleeve gastrectomy: an objective assessment of gastroesophageal reflux disease. Obes Surg 27(3):749–753. https://doi.org/10.1007/s11695-016-2359-x
Balla A, Meoli F, Palmieri L et al (2021) Manometric and pH-monitoring changes after laparoscopic sleeve gastrectomy: a systematic review. Langenbecks Arch Surg 406(8):2591–2609. https://doi.org/10.1007/s00423-021-02171-3
Thereaux J, Barsamian C, Bretault M et al (2016) pH monitoring of gastro-oesophageal reflux before and after laparoscopic sleeve gastrectomy. Br J Surg 103(4):399–406. https://doi.org/10.1002/bjs.10089
Chern TY, Chan DL, Maani J, Ferguson JS, Talbot ML (2021) High-resolution impedance manometry and 24-hour multichannel intraluminal impedance with pH testing before and after sleeve gastrectomy: de novo reflux in a prospective series. Surg Obes Relat Dis 17(2):329–337. https://doi.org/10.1016/j.soard.2020.09.030
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Kinga Powers receives honoraria for speaking for Medtronic and Gore and consulting fees from Gerson Lehrman Group Inc. Aurora Pryor receives honoraria for speaking for Gore, Medtronic, and Stryker and travel reimbursements for consulting for Intuitive. Konstantinos Spaniolas is a Consultant for Intuitive and Medtronic. Ila Sethi, Aidan Aicher, Fareed Cheema, and Amy Rosenbluth have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sethi, I., Aicher, A., Cheema, F. et al. Postoperative outcomes for sleeve gastrectomy patients with positive pH-defined GERD. Surg Endosc 37, 6861–6866 (2023). https://doi.org/10.1007/s00464-023-10149-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10149-z