Abstract
Background
Intracorporeal anastomosis (IA) is associated with reduced surgical site infection (SSI) and other postoperative complications in laparoscopic right colectomy (LRC). However, evidence is inadequate for IA in laparoscopic left colectomy (LLC). This study aimed to determine the effect of IA and extracorporeal anastomosis (EA) on SSI and other short-term postoperative complications in LLC.
Methods
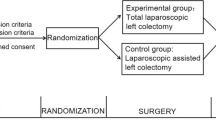
In this retrospective multicenter propensity score-matched (PSM) cohort study, we enrolled consecutive patients who underwent LLC with IA (TLLC/IA) and laparoscopic-assisted left colectomy with EA (LALC/EA) at two medical centers between January 2015 and September 2021. Propensity score matching with a 1:2 ratio was employed. The primary outcome was SSI occurrence. Secondary outcomes were operating time, intraoperative hemorrhage, other postoperative complications, and pathological outcomes.
Results
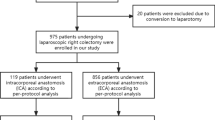
Overall, 574 and 99 patients received LALC/EA and TLLC/IA, respectively. After PSM, 84 patients with TLLC/IA were matched with 141 patients with LALC/EA. Thirty patients (13.3%) patients experienced SSI (17.0% in LALC/EA vs 7.1% in TLLC/IA). IA was associated with a reduced risk of overall SSI and superficial/deep SSI compared with EA after PSM, with OR of 0.375 (95% CI, 0.147–0.959, P = 0.041). and 0.148 (95% CI, 0.034–0.648, P = 0.011), respectively. Multivariate analysis of unmatched patients indicated similar results. In the analysis of secondary outcomes, LALC/EA may have a shorter operating time (absolute mean difference − 13.41 [95% CI, − 23.76 to − 3.06], P = 0.002) and a higher risk of intraoperative hemorrhage (absolute risk difference 4.96 [95% CI, − 0.09 to 9.89], P = 0.048).
Conclusions
IA in LLC is associated with a reduced risk of overall SSI and superficial/deep SSI. However, it may require a longer operating time.
Graphical abstract


Similar content being viewed by others
References
Lacy AM, Delgado S, Castells A, Prins HA, Arroyo V, Ibarzabal A et al (2008) The long-term results of a randomized clinical trial of laparoscopy-assisted versus open surgery for colon cancer. Ann Surg 248(1):1–7
Bilimoria KY, Bentrem DJ, Nelson H, Stryker SJ, Stewart AK, Soper NJ et al (2008) Use and outcomes of laparoscopic-assisted colectomy for cancer in the United States. Arch Surg 143(9):832–840
Nelson H, Sargent DJ, Wieand HS, Fleshman J, Anvari M, Stryker SJ et al (2004) A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med 350(20):2050–2059
Allaix ME, Degiuli M, Bonino MA, Arezzo A, Mistrangelo M, Passera R et al (2019) Intracorporeal or extracorporeal ileocolic anastomosis after laparoscopic right colectomy: a double-blinded randomized controlled trial. Ann Surg 270(5):762–767
Bollo J, Turrado V, Rabal A, Carrillo E, Gich I, Martinez MC et al (2020) Randomized clinical trial of intracorporeal versus extracorporeal anastomosis in laparoscopic right colectomy (IEA trial). Br J Surg 107(4):364–372
Swaid F, Sroka G, Madi H, Shteinberg D, Somri M, Matter I (2016) Totally laparoscopic versus laparoscopic-assisted left colectomy for cancer: a retrospective review. Surg Endosc 30(6):2481–2488
Milone M, Angelini P, Berardi G, Burati M, Corcione F, Delrio P et al (2018) Intracorporeal versus extracorporeal anastomosis after laparoscopic left colectomy for splenic flexure cancer: results from a multi-institutional audit on 181 consecutive patients. Surg Endosc 32(8):3467–3473
Pisani Ceretti A, Maroni N, Sacchi M, Bona S, Angiolini MR, Bianchi P et al (2015) Laparoscopic colonic resection for splenic flexure cancer: our experience. BMC Gastroenterol 15:76
Achilli P, Perry W, Grass F, Abd El Aziz MA, Kelley SR, Larson DW et al (2021) Completely intracorporeal anastomosis in robotic left colonic and rectal surgery: technique and 30-day outcomes. Updates Surg. 73(6):2137–2143
Carlini M, Spoletini D, Castaldi F, Giovannini C, Passaro U (2016) Laparoscopic resection of splenic flexure tumors. Updates Surg 68(1):77–83
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR, Guideline for Prevention of Surgical Site Infection (1999) Centers for disease control and prevention (CDC) hospital infection control practices advisory committee. Am J Infect Control 27(2):97–132
Berríos-Torres SI, Umscheid CA, Bratzler DW, Leas B, Stone EC, Kelz RR et al (2017) Centers for disease control and prevention guideline for the prevention of surgical site infection. JAMA Surg 152(8):784–791
Akamatsu H, Omori T, Oyama T, Tori M, Ueshima S, Nakahara M et al (2009) Totally laparoscopic sigmoid colectomy: a simple and safe technique for intracorporeal anastomosis. Surg Endosc 23(11):2605–2609
Nepal P, Mori S, Kita Y, Tanabe K, Baba K, Sasaki K et al (2021) Modified delta-shaped anastomosis via the overlap method using linear staplers for colon cancer. J anus, rectum colon 5(1):107–111
Haas EM, de Paula TR, Luna-Saracho R, Smith MS, LeFave J-PJ (2021) Robotic natural-orifice intracorporeal anastomosis with extraction (NICE procedure) for complicated diverticulitis. Surg Endosc 35(6):3205–3213
Minjares-Granillo RO, Dimas BA, LeFave J-PJ, Haas EM (2019) Robotic left-sided colorectal resection with natural orifice IntraCorporeal anastomosis with extraction of specimen: the NICE procedure. A pilot study of consecutive cases. Am J Surg 217(4):670–676
Ntourakis D, Kykalos S, Michalinos A (2020) Laparoscopic left hemicolectomy with intracorporeal colosigmoid anastomosis: a technical note. Asian J Surg. https://doi.org/10.1016/j.asjsur.2019.07.020
Ohmura Y, Suzuki H, Kotani K, Teramoto A (2020) Intracorporeal hemi-hand-sewn technique for end-to-end anastomosis in laparoscopic left-side colectomy. Surg Endosc 34(9):4200–4205
Schrag D, Cramer LD, Bach PB, Cohen AM, Warren JL, Begg CB (2000) Influence of hospital procedure volume on outcomes following surgery for colon cancer. JAMA 284(23):3028–3035
Ishizuka M, Shibuya N, Takagi K, Hachiya H, Tago K, Shimizu T et al (2021) Postoperative complications associated with intra- versus extracorporeal anastomosis for laparoscopic right colectomy. Am Surg. https://doi.org/10.1177/00031348211023417
Martinek L, You K, Giuratrabocchetta S, Gachabayov M, Lee K, Bergamaschi R (2018) Does laparoscopic intracorporeal ileocolic anastomosis decreases surgical site infection rate? A propensity score-matched cohort study. Int J Colorectal Dis 33(3):291–298
Hennessey DB, Burke JP, Ni-Dhonochu T, Shields C, Winter DC, Mealy K (2010) Preoperative hypoalbuminemia is an independent risk factor for the development of surgical site infection following gastrointestinal surgery: a multi-institutional study. Ann Surg 252(2):325–329
Scarborough JE, Mantyh CR, Sun Z, Migaly J (2015) Combined mechanical and oral antibiotic bowel preparation reduces incisional surgical site infection and anastomotic leak rates after elective colorectal resection: an analysis of colectomy-targeted ACS NSQIP. Ann Surg 262(2):331–337
Althumairi AA, Canner JK, Pawlik TM, Schneider E, Nagarajan N, Safar B et al (2016) Benefits of bowel preparation beyond surgical site infection: a retrospective study. Ann Surg 264(6):1051–1057
Ling ML, Apisarnthanarak A, Abbas A, Morikane K, Lee KY, Warrier A et al (2019) APSIC guidelines for the prevention of surgical site infections. Antimicrob Resist Infect Contr 8:174
Zaman S, Mohamedahmed AYY, Ayeni AA, Peterknecht E, Mawji S, Albendary M et al (2022) Comparison of the colonic J-pouch versus straight (end-to-end) anastomosis following low anterior resection: a systematic review and meta-analysis. Int J Colorectal Dis 37(4):919–938
Cleary RK, Kassir A, Johnson CS, Bastawrous AL, Soliman MK, Marx DS et al (2018) Intracorporeal versus extracorporeal anastomosis for minimally invasive right colectomy: a multi-center propensity score-matched comparison of outcomes. PLoS ONE 13(10):e0206277
Selvy M, Mattevi C, Slim K, Pezet D, Pereira B, Le Roy B (2020) Intra-versus extracorporeal anastomosis in laparoscopic right colectomy: a meta-analysis of 3699 patients. Int J Colorectal Dis 35(9):1673–1680
Acknowledgements
We thank Yanhua Wu from the Clinical Research Department of the First Hospital of Jilin University for providing statistical guidance in this study.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Dr. Yuchen Guo, Ms. Kexuan Li, Prof. Liang He, Prof. Weihua Tong, Dr. Yan Chen, Prof. Bin Wu, Prof. Guole Lin, Prof. Huizhong Qiu, Prof. Lai Xu, Prof. Yi Xiao, and Prof. Quan Wang have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Guo, Y., Li, K., He, L. et al. Surgical site infection after intracorporeal and extracorporeal anastomosis in laparoscopic left colectomy for colon cancer: a multicenter propensity score-matched cohort study. Surg Endosc 37, 6208–6219 (2023). https://doi.org/10.1007/s00464-023-10093-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10093-y