Abstract
Background
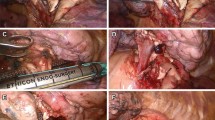
Video-assisted thoracoscopic lobectomy with lymphadenectomy is considered one of the most effective treatments for early non-small cell lung cancer. We developed a novel approach for lobectomy in patients with right upper lung cancer through simplified synchronous disconnection of pulmonary arteries and veins. This study aimed to evaluate the feasibility, efficacy, safety, and cost-effectiveness of this minimally invasive technique in managing right upper lobectomy.
Patients and methods
From March 2016 to September 2017, 62 patients with right upper lung cancer underwent lobectomy via simplified synchronous disconnection of pulmonary arteriovenous by video-assisted thoracoscopic surgery. All patients were followed up for 6–12 months after the procedure through clinic visits or telephone/e-mail interviews.
Results
Of the 62 patients (mean age, 57.2 ± 8.7 years), 28 were men (45.2%) and 34 (54.8%) were women. All procedures were successfully performed by thoracoscopy, with a mean operating time of 66.2 ± 9.0 min. The mean blood loss was 40.3 ± 19.5 mL. Only 1 (1.61%) patient required blood transfusion. The mean number of endoscopic linear stapling devices used was 2.6 ± 0.7. The mean number of lymph nodes harvested was 16.0 ± 1.6. Postoperative pneumonia was encountered in 4 (6.45%) patients. There was no postoperative mortality. The mean length of hospital stay was 5.3 ± 1.3 days. Six-month follow-up revealed an excellent clinical result and degree of satisfaction.
Conclusions
Simplified synchronous disconnection of pulmonary arteries and veins is a feasible, economical, safe, and effective therapeutic procedure for right upper lung carcinoma. This novel procedure shows promise as a viable surgical approach for right upper lobectomy.





Similar content being viewed by others
References
Cox ML, Yang CJ, Speicher PJ, Anderson KL, Fitch ZW, Gu L, Davis RP, Wang X, D’Amico TA, Hartwig MG, Harpole DH Jr, Berry MF (2017) The role of extent of surgical resection and lymph node assessment for clinical stage i pulmonary lepidic adenocarcinoma: an analysis of 1991 patients. J Thorac Oncol 12:689–696
Wang GS, Wang Z, Wang J, Rao ZP (2014) Uniportal complete video-assisted thoracoscopic lobectomy with systematic lymphadenectomy. J Thorac Dis 6:1011–1016
Mu JW, Gao SG, Xue Q, Mao YS, Wang DL, Zhao J, Gao YS, Huang JF, He J (2016) A propensity matched comparison of effects between video assisted thoracoscopic single-port, two-port and three-port pulmonary resection on lung cancer. J Thorac Dis 8:1469–1476
Sakuraba M, Miyamoto H, Oh S, Shiomi K, Sonobe S, Takahashi N, Imashimizu K, Sakao Y (2007) Video-assisted thoracoscopic lobectomy vs. conventional lobectomy via open thoracotomy in patients with clinical stage IA non-small cell lung carcinoma. Interact Cardiovasc Thorac Surg 6:614–617
Liu L, Che G, Pu Q, Ma L, Wu Y, Kan Q, Zhuge X, Shi L (2010) A new concept of endoscopic lung cancer resection: single-direction thoracoscopic lobectomy. Surg Oncol 19:e71–e77
Lin JB, Chen JF, Lai FC, Li X, Qiu ML (2016) Transareolar pulmonary bullectomy for primary spontaneous pneumothorax. J Thorac Cardiovasc Surg 152:999–1005
Ke H, Liu Y, Zhou X, Xue Q (2017) Anterior fissureless uniport vs. posterior intra-fissure triple-port thoracoscopic right upper lobectomy: a propensity-matched study. J Thorac Dis 9:3866–3874
Rogers LJ, Bleetman D, Messenger DE, Joshi NA, Wood L, Rasburn NJ, Batchelor TJP (2018) The impact of enhanced recovery after surgery (ERAS) protocol compliance on morbidity from resection for primary lung cancer. J Thorac Cardiovasc Surg 155:1843–1852
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61:69–90
Verstegen NE, Oosterhuis JW, Palma DA, Rodrigues G, Lagerwaard FJ, van der Elst A, Mollema R, van Tets WF, Warner A, Joosten JJ, Amir MI, Haasbeek CJ, Smit EF, Slotman BJ, Senan S (2013) Stage I-II non-small-cell lung cancer treated using either stereotactic ablative radiotherapy (SABR) or lobectomy by video-assisted thoracoscopic surgery (VATS): outcomes of a propensity score-matched analysis. Ann Oncol 24:1543–1548
Sepesi B, Gold KA, Correa AM, Heymach JV, Vaporciyan AA, Roszik J, Dmitrovsky E, Liu X (2017) The influence of body mass index on overall survival following surgical resection of non-small cell lung cancer. J Thorac Oncol 12:1280–1287
Powell HA, Tata LJ, Baldwin DR, Stanley RA, Khakwani A, Hubbard RB (2013) Early mortality after surgical resection for lung cancer: an analysis of the English National Lung cancer audit. Thorax 68:826–834
Lewis RJ, Caccavale RJ, Sisler GE, Mackenzie JW (1992) One hundred consecutive patients undergoing video-assisted thoracic operations. Ann Thorac Surg 54:421–426
Ettinger DS, Bepler G, Bueno R, Chang A, Chang JY, Chirieac LR, D’Amico TA, Demmy TL, Feigenberg SJ, Grannis FW Jr, Jahan T, Jahanzeb M, Kessinger A, Komaki R, Kris MG, Langer CJ, Le QT, Martins R, Otterson GA, Robert F, Sugarbaker DJ, Wood DE (2006) Non-small cell lung cancer clinical practice guidelines in oncology. J Natl Compr Cancer Netw 4:548–582
Sato Y, Tezuka Y, Kanai Y, Otani S, Yamamoto S, Tetsuka K, Sohara Y (2008) Novel retractor for lymphnode dissection by video-assisted thoracic surgery. Ann Thorac Surg 86:1036–1037
Tsuboi I, Hayashi M, Miyauchi Y, Iwasaki YK, Yodogawa K, Hayashi H, Uetake S, Takahashi K, Shimizu W (2014) Anatomical factors associated with periesophageal vagus nerve injury after catheter ablation of atrial fibrillation. J Nippon Med Sch 81:248–257
Baste JM, Haddad L, Melki J et al (2015) Anterior subcarinal node dissection on the left side using video thoracoscopy: an easier technique. Ann Thorac Surg 99(4):e99–e101
Jung H, Oh TH, Cho JY, Lee DH (2017) Mid-term outcomes of single-port versus conventional three-port video-assisted thoracoscopic surgery for primary spontaneous pneumothorax. Korean J Thorac Cardiovasc Surg 50:184–189
Chu X, Xue Z, Zhang L, Hou X, Ma K (2010) Primary report of lobectomy with single utility port complete video-assisted thoracoscopic surgery [In Chinese]. Zhongguo Fei Ai Za Zhi 13:19–21
Migliore M (2003) Efficacy and safety of single-trocar technique for minimally invasive surgery of the chest in the treatment of noncomplex pleural disease. J Thorac Cardiovasc Surg 126:1618–1623
Gonzalez-Rivas D, de la Torre M, Fernandez R, Mosquera VX (2011) Single-port video-assisted thoracoscopic left upper lobectomy. Interact Cardiovasc Thorac Surg 13:539–541
Gonzalez D, Paradela M, Garcia J, Delta Torre M (2011) Single-port video-assisted thoracoscopic lobectomy. Interact Cardiovasc Thorac Surg 12:514–515
Ji C, Xiang Y, Pagliarulo V, Lee J, Sihoe ADL, Kim H, Zhang X, Wang Z, Zhao W, Feng J, Fang W (2017) A multi-center retrospective study of single-port versus multi-port video-assisted thoracoscopic lobectomy and anatomic segmentectomy. J Thorac Dis 9:3711–3718
Miyazaki T, Yamasaki N, Tsuchiya T, Matsumoto K, Hatachi G, Kitamura Y, Obata T, Doi R, Machino R, Nagayasu T (2016) Management of unexpected intraoperative bleeding during thoracoscopic pulmonary resection: a single institutional experience. Surg Today 46:901–907
Zhou ZL, Zhao H, Li Y, Li JF, Jiang GC, Wang J (2013) Completely thoracoscopic lobectomy for the surgical management of bronchiectasis. Chin Med J (Enl) 126:875–878
Mazzella A, Olland A, Garelli E, Renaud S, Reeb J, Santelmo N, Falcoz PE, Massard G (2017) Video-assisted thoracoscopic surgery is a safe option for benign lung diseases requiring lobectomy. Surg Endosc 31:125
Amar D, Munoz D, Shi W, Zhang H, Thaler HT (2010) A clinical prediction rule for pulmonary complications after thoracic surgery for primary lung cancer. Anesth Analg 110:1343–1348
Wang S, Li X, Li Y, Li J, Jiang G, Liu J, Wang J (2017) The long-term impact of postoperative pulmonary complications after video-assisted thoracic surgery lobectomy for lung cancer. J Thorac Dis 9:5143–5152
Geller AD, Zheng H, Mathisen DJ, Wright CD, Lanuti M (2018) Relative incremental costs of complications of lobectomy for stage I non-small cell lung cancer. J Thorac Cardiovasc Surg 155:1804–1811
Lugg ST, Agostini PJ, Tikka T, Kerr A, Adams K, Bishay E, Kalkat MS, Steyn RS, Rajesh PB, Thickett DR, Naidu B (2016) Long-term impact of developing a postoperative pulmonary complication after lung surgery. Thorax 71:171–176
Acknowledgements
The authors would like to thank Hugh McGonigle, from Liwen Bianji, Edanz Group China, for editing the English text of a draft of the manuscript. This study was approved by the Institutional Review Board and Ethics Committee of the First Affiliated Hospital of Fujian Medical University (No. 2016-03, March 2016).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Jian-Bo Lin, Ming-Lian Qiu, Chun-Jin Lin, Xu Li, Jian-Feng Chen, Fan-Cai Lai and Bo Liu have no conflicts of interest or financial ties to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Video 1
Simplified synchronous disconnection of pulmonary arteries and veins for RUL procedure. (MPG 472704 KB)
Rights and permissions
About this article
Cite this article
Lin, JB., Qiu, ML., Lin, CJ. et al. Simplified synchronous disconnection of pulmonary arteries and veins for right upper lobectomy. Surg Endosc 33, 2015–2023 (2019). https://doi.org/10.1007/s00464-018-06659-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-06659-w