Abstract
Background
Gaze training is an effective way of training basic laparoscopic skills, resulting in faster acquisition periods and more robust subsequent performance under pressure. The current study is a randomized control trial which examines whether the performance benefits of gaze training stand the test of time (delayed retention) and transfer to more complex skills.
Methods
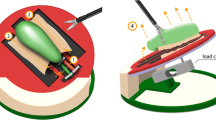
Thirty-six medical students were trained to proficiency (50 trials) on a one-handed laparoscopic task (picking and dropping balls) in either a discovery learning (DL) or gaze training (GT) group. Both groups performed the one-handed task in baseline, retention and delayed retention (1 month) tests. They also performed baseline, retention and delayed retention tests of a two-handed task (grasping and cutting). Performance (completion time) and gaze control (target locking) were assessed throughout.
Results
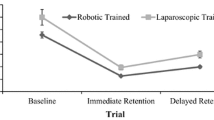
For the one-handed task, the GT group displayed superior performance at retention (p < .001), underpinned by more expert-like gaze control (p < .05). The GT group also displayed superior performance in the one-handed task at delayed retention (p < .005), underpinned by more expert-like gaze control strategies (p < .001). Although the DL group’s performance fell to 84 % of performance at retention, the GT group maintained performance at 100 % of retention. There were no differences between the groups for the two-handed task at retention (p = .140); however, at delayed retention, the GT group outperformed the DL group (p < .005) and displayed more expert-like gaze control (p < .001).
Conclusions
Novices trained to adopt an expert-like gaze control strategy were able to attain higher levels of performance more quickly than novices who learned by discovery alone. Furthermore, these skills were more durable over time and were transferable to more complex skills. Gaze training is a beneficial intervention to aid the acquisition of the basic motor skills required for laparoscopy.





Similar content being viewed by others
References
Gallagher AG, McClure N, McGuigan J, Crothers I, Browning J (1999) Virtual reality training in laparoscopic surgery: a preliminary assessment of minimally invasive surgical trainer virtual reality (MIST VR). Endoscopy 31:310–313
Scott DJ, Bergen PC, Rege RV, Laycock R, Tesfay ST, Valentine RJ, Euhus DM, Jeyarajah DR, Thompson WM, Jones DB (2000) Laparoscopic training on bench models: better and more cost effective than operating room experience? J Am Coll Surg 191:272–283
Wilson M, McGrath J, Vine S, Brewer J, Defriend D, Masters R (2010) Psychomotor control in a virtual laparoscopic surgery training environment: gaze control parameters differentiate novices from experts. Surg Endosc 24:2458–2464
Wilson MR, McGrath JS, Vine SJ, Brewer J, Defriend D, Masters RS (2011) Perceptual impairment and psychomotor control in virtual laparoscopic surgery. Surg Endosc 25:2268–2274
Law B, Atkins MS, Kirkpatrick AE, Lomax AJ, Mackenzie CL (2004) Eye gaze patterns differentiate novice and experts in a virtual laparoscopic surgery training environment. In: Duchowski AT, Vertegaal R (eds) Proceedings of the eye tracking research and application symposium, San Antonio, TX, March 22–24, 2004, pp 41–47
Wilson MR, Vine SJ, Bright E, Masters RS, Defriend D, McGrath JS (2011) Gaze training enhances laparoscopic technical skill acquisition and multi-tasking performance: a randomised, controlled study. Surg Endosc 25(12):3731–3739
Vine SJ, Masters RS, McGrath JS, Bright E, Wilson MR (2012) Cheating experience: guiding novices to adopt the gaze strategies of experts expedites the learning of technical laparoscopic skills. Surgery 152:32–40
Goddell KH, Cao CG, Schwaitzberg SD (2006) Effects of cognitive distraction on performance of laparoscopic surgical tasks. J Laparoendosc Adv Surg Tech 16:94–98
Poolton JM, Wilson MR, Malhotra N, Ngo K, Masters RS (2011) A comparison of evaluation, time pressure and multi-tasking as stressors of psychomotor surgical performance. Surgery 149(6):776–782
Vine SJ, Wilson MR (2010) Quiet eye training: effects on learning and performance under pressure. J Appl Sport Psychol 22:361–376
Vine SJ, Wilson MR (2011) The influence of quiet eye training and pressure on attentional control in a visuo-motor task. Acta Psychol 136:340–346
Vine SJ, Moore LJ, Wilson MR (2011) Quiet eye training facilitates competitive putting performance in elite golfers. Front Psychol 2:8
Grober ED, Hamstra SJ, Wanzel KR, Reznick RK, Matsumoto ED, Sidhu RS, Jarvi KA (2004) Laboratory based training in urological microsurgery with bench model simulators: a randomized controlled trial evaluating the durability of technical skill. J Urol 172:378–381
Gallagher AG, Ritter EM, Champion H, Higgins G, Fried MP, Moses G, Smith CD, Satava RM (2005) Virtual reality simulation for the operating room: proficiency-based training as a paradigm shift in surgical skills training. Ann Surg 241:364–372
Wulf G, Shea C, Lewthwaite R (2010) Motor skill learning and performance: a review of influential factors. Med Educ 44:75–84
Arthur W Jr, Bennet W Jr, Stanush PL, McNelly TL (1998) Factors that influence skill decay and retention: a quantitative review and analysis. Hum Perform 11:57–101
Stefanidis D, Korndoffer JR Jr, Markley S, Sierra R, Scott DJ (2006) Proficiency maintenance: impact of ongoing simulator training on laparoscopic skill retention. J Am Coll Surg 202:599–603
Grantcharov TP, Kristiansen VB, Bendix J, Bardram L, Rosenberg J, Funch-Jensen P (2004) Randomized clinical trial of virtual reality simulation for laparoscopic skills training. Br J Surg 91:146–150
Ritter EM, Scott DS (2007) Design of a proficiency-based skills training curriculum for the fundamentals of laparoscopic surgery. Surg Innov 14:107–112
Aggarwal R, Grantcharov TP, Eriksen JR, Blirup D, Kristiansen VB, Funch-Jensen P, Darzi A (2006) An evidence-based virtual reality training program for novice laparoscopic surgeons. Ann Surg 244:310–314
Aggarwal R, Crochet A, Dias A, Misra A, Ziprin P, Darzi A (2009) Development of a virtual reality training curriculum for laparoscopic cholecystectomy. Br J Surg 96:1086–1093
Salier U, Flanagan JR, Johansson RS (2005) Eye–hand coordination during learning of a novel visuomotor task. J Neurosci 205:8833–8842
Torkington J, Smith SG, Rees B, Darzi A (2001) The role of the basic surgical skills course in the acquisition and retention of laparoscopic skill. Surg Endosc 15:1071–1075
Gurusamy K, Agarwal R, Palanivelu L, Davidson BR (2009) Systematic review of randomized controlled trials on the effectiveness of virtual reality training for laparoscopic surgery. Br J Surg 96:1087–1093
Boehler ML, Schwind CJ, Rogers DA, Ketchum J, O’Sullivan E, Mayforth R, Quin J, Wohltman C, Johnson C, Williams RG, Dunnington G (2007) A theory-based curriculum for enhancing surgical skillfulness. J Am Coll Surg 205:492–497
Land MF (2009) Vision, eye movements, and natural behavior. Vis Neurosci 26:51–62
Acknowledgments
The authors would like to acknowledge Roy Chandra-Ramanan for his support in data collection, and Chenghua Lin for developing the STT software. This work was supported by a bilateral research grant from the Economic and Social Research Council, UK and the Research Grants Council, Hong Kong (RES-000-22-3016).
Disclosures
Dr. Vine, Mr. Chaytor, Mr. McGrath, Prof. Masters, and Dr. Wilson have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vine, S.J., Chaytor, R.J., McGrath, J.S. et al. Gaze training improves the retention and transfer of laparoscopic technical skills in novices. Surg Endosc 27, 3205–3213 (2013). https://doi.org/10.1007/s00464-013-2893-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-013-2893-8