Abstract
Background
A nomogram that integrates risk models and clinical characteristics can accurately predict the prognosis of individual patients. We aimed to identify the prognostic factors and establish nomograms for predicting overall survival (OS) and cause-specific survival (CSS) in patients with multi-organ metastatic colorectal cancer (CRC).
Methods
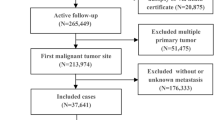
Demographic and clinical information on multi-organ metastases from 2010 to 2019 were extracted from the Surveillance, Epidemiology, and End Results (SEER) Program. Univariate and multivariate Cox analyses were used to identify independent prognostic factors that were used to develop nomograms to predict CSS and OS, and to assess the concordance index (C-index), area under the curve (AUC), and calibration curve.
Results
The patients were randomly assigned to the training and validation groups at a 7:3 ratio. A Cox proportional hazards model was conducted for CRC patients to identify independent prognostic factors, including age, sex, tumor size, metastases, degree of differentiation, stage T, stage N, primary and metastasis surgery. The competing risk models employed by Fine and Gray were used to identify the risk factors for CRC. Death from other causes was treated as a competing event, and Cox models were used to identify the factors for death to identify the independent factors of CSS. By incorporating the corresponding independent prognostic factors, we established prognostic nomograms for OS and CSS. Finally, we used the C-index, ROC curve, and calibration plots to assess the utility of the nomogram.
Conclusions
Using the SEER database, we constructed a predictive model for CRC patients with multi-organ metastases. Nomograms provide clinicians with 1-, 3-, and 5-year OS and CSS predictions for CRC, allowing them to formulate appropriate treatment plans.






Similar content being viewed by others
Data availability
The data that support the findings of this study are openly available in the SEER database (www.seer.cancer.gov).
References
Benitez Majano S, Di Girolamo C, Rachet B, Maringe C, Guren MG, Glimelius B, Iversen LH, Schnell EA, Lundqvist K, Christensen J, Morris M, Coleman MP, Walters S (2019) Surgical treatment and survival from colorectal cancer in Denmark, England, Norway, and Sweden: a population-based study. Lancet Oncol 20(1):74–87
Bianco FJ Jr (2006) Nomograms and medicine. Eur Urol 50(5):884–886
Bouche O, Conroy T, Michel P, Penna C, Tournigand C (2006) Metastatic colorectal cancer. Gastroenterol Clin Biol 30 Spec No 2:2s30-32s42
Camp RL, Dolled-Filhart M, Rimm DL (2004) X-tile: a new bio-informatics tool for biomarker assessment and outcome-based cut-point optimization. Clin Cancer Res 10(21):7252–7259
Chaffer CL, Weinberg RA (2011) A perspective on cancer cell metastasis. Science 331(6024):1559–1564
Hashiguchi Y, Muro K, Saito Y, Ito Y, Ajioka Y, Hamaguchi T, Hasegawa K, Hotta K, Ishida H, Ishiguro M, Ishihara S, Kanemitsu Y, Kinugasa Y, Murofushi K, Nakajima TE, Oka S, Tanaka T, Taniguchi H, Tsuji A, Uehara K, Ueno H, Yamanaka T, Yamazaki K, Yoshida M, Yoshino T, Itabashi M, Sakamaki K, Sano K, Shimada Y, Tanaka S, Uetake H, Yamaguchi S, Yamaguchi N, Kobayashi H, Matsuda K, Kotake K, Sugihara K (2020) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2019 for the treatment of colorectal cancer. Int J Clin Oncol 25(1):1–42
Iasonos A, Schrag D, Raj GV, Panageas KS (2008) How to build and interpret a nomogram for cancer prognosis. J Clin Oncol 26(8):1364–1370
Kawai K, Ishihara S, Yamaguchi H, Sunami E, Kitayama J, Miyata H, Watanabe T (2015) Nomogram prediction of metachronous colorectal neoplasms in patients with colorectal cancer. Ann Surg 261(5):926–932
Kong X, Li J, Cai Y, Tian Y, Chi S, Tong D, Hu Y, Yang Q, Li J, Poston G, Yuan Y, Ding K (2018) A modified TNM staging system for non-metastatic colorectal cancer based on nomogram analysis of SEER database. BMC Cancer 18(1):50
Kornprat P, Pollheimer MJ, Lindtner RA, Schlemmer A, Rehak P, Langner C (2011) Value of tumor size as a prognostic variable in colorectal cancer: a critical reappraisal. Am J Clin Oncol 34(1):43–49
Liu Z, Xu Y, Xu G, Baklaushev VP, Chekhonin VP, Peltzer K, Ma W, Wang X, Wang G, Zhang C (2021) Nomogram for predicting overall survival in colorectal cancer with distant metastasis. BMC Gastroenterol 21(1):103
Miyoshi N, Ohue M, Yasui M, Noura S, Shingai T, Sugimura K, Akita H, Gotoh K, Marubashi S, Takahashi H, Okami J, Fujiwara Y, Higashiyama M, Yano M (2016) Novel prognostic prediction models for patients with stage IV colorectal cancer after concurrent curative resection. ESMO Open 1(3):e000052
Park SY (2018) Nomogram: an analogue tool to deliver digital knowledge. J Thorac Cardiovasc Surg 155(4):1793
Robinson JR, Newcomb PA, Hardikar S, Cohen SA, Phipps AI (2017) Stage IV colorectal cancer primary site and patterns of distant metastasis. Cancer Epidemiol 48:92–95
Siegel RL, Miller KD, Fuchs HE, Jemal A (2022) Cancer statistics, 2022. CA Cancer J Clin 72(1):7–33
Tang M, Wang H, Cao Y, Zeng Z, Shan X, Wang L (2021) Nomogram for predicting occurrence and prognosis of liver metastasis in colorectal cancer: a population-based study. Int J Colorectal Dis 36(2):271–282
Wu WT, Li YJ, Feng AZ, Li L, Huang T, Xu AD, Lyu J (2021) Data mining in clinical big data: the frequently used databases, steps, and methodological models. Mil Med Res 8(1):44
Yu C, Zhang Y (2020) Establishment of prognostic nomogram for elderly colorectal cancer patients: a SEER database analysis. BMC Gastroenterol 20(1):347
Zauber AG, Winawer SJ, O’Brien MJ, Lansdorp-Vogelaar I, van Ballegooijen M, Hankey BF, Shi W, Bond JH, Schapiro M, Panish JF, Stewart ET, Waye JD (2012) Colonoscopic polypectomy and long-term prevention of colorectal-cancer deaths. N Engl J Med 366(8):687–696
Zhang ZY, Luo QF, Yin XW, Dai ZL, Basnet S, Ge HY (2016) Nomograms to predict survival after colorectal cancer resection without preoperative therapy. BMC Cancer 16(1):658
Zhang J, Yang Y, Fu X, Guo W (2020) Development and validation of nomograms for prediction of overall survival and cancer-specific survival of patients of colorectal cancer. Jpn J Clin Oncol 50(3):261–269
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Contributions
Study conception and design: XT and NH. Drafting of manuscript: NH, JJ, SH. Acquisition of data and critical revision: HR, XY, YY, YZ. Revision of manuscript, and final approval of manuscript: XT, GX.
Corresponding author
Ethics declarations
Conflict of interest
Dr. Nan Hu, Dr. Jiao Jiang, Dr. Shu Huan, Dr. Huiting Rao, Dr. Xin Yang, Dr. Yi Yuan, Dr. Yanlang Zhang, Dr. Guodong Xia, Dr. Xiaowei Tang all have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tang, X., Hu, N., Huang, S. et al. Prognostic nomogram for colorectal cancer patients with multi-organ metastases: a Surveillance, Epidemiology, and End Results program database analysis. J Cancer Res Clin Oncol 149, 12131–12143 (2023). https://doi.org/10.1007/s00432-023-05070-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-05070-w