Abstract
Background
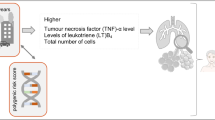
There is no research to prove the association between irritability and lung cancer, our study performed a Mendelian randomization (MR) approach to elucidate the causal relationship of irritability with lung cancer risk.
Methods
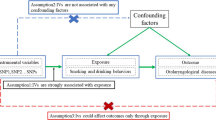
Genome-wide association studies (GWAS) data of irritability, lung cancer and gastroesophageal reflux disease (GERD) were downloaded from a public database for two-sample MR analysis. Independent single-nucleotide polymorphisms (SNPs) associated with irritability and GERD were selected as instrumental variables (IVs). Inverse variance weighting (IVW) and weighted median method were used to analyze causality.
Results
There is an association between irritability and lung cancer risk (ORIVW = 1.01, 95% CI = [1.00, 1.02], P = 0.018; ORweighted median = 1.01, 95% CI = [1.00, 1.02], P = 0.046), and GERD might account for about 37.5% of the association between irritability and lung cancer.
Conclusions
This study confirmed the causal effect between irritability and lung cancer through MR analysis, and found that GERD played an essential mediating role in this relationship, which can partly indicate the role of the “inflammation-cancer transformation” process in lung cancer.


Similar content being viewed by others
Data availability
All relevant data are within the manuscript and its additional files.
Abbreviations
- DC:
-
Dendritic cell
- DE:
-
Direct effect
- GERD:
-
Gastroesophageal reflux disease
- GWAS:
-
Genome-wide association studies
- IEU:
-
Integrative Epidemiology Unit
- IFN:
-
Type I interferon
- IVs:
-
Instrumental variables
- IVW:
-
Inverse variance weighting
- LD:
-
Linkage disequilibrium
- ME:
-
Mediation effect
- MR:
-
Mendelian randomization
- RCTs:
-
Randomized controlled trials
- SNPs:
-
Single-nucleotide polymorphisms
- TE:
-
Total effect
References
Amarnath S, Starr A, Chukkalore D et al (2022) The association between gastroesophageal reflux disease and non-small cell lung cancer: a retrospective case-control study. Gastroenterol Res 15(4):173–179. https://doi.org/10.14740/gr1537
Batty GD, Russ TC, Stamatakis E, Kivimäki M (2017) Psychological distress in relation to site specific cancer mortality: pooling of unpublished data from 16 prospective cohort studies. BMJ. https://doi.org/10.1136/bmj.j108. (Published online January 25, 2017)
Bell E, Boyce P, Porter RJ, Bryant RA, Malhi GS (2021) Irritability in mood disorders: neurobiological underpinnings and implications for pharmacological intervention. CNS Drugs 35(6):619–641. https://doi.org/10.1007/s40263-021-00823-y
Budisan L, Zanoaga O, Braicu C et al (2021) Links between infections, lung cancer, and the immune system. IJMS 22(17):9394. https://doi.org/10.3390/ijms22179394
Burgess S, Butterworth A, Thompson SG (2013) Mendelian randomization analysis with multiple genetic variants using summarized data. Genet Epidemiol 37(7):658–665. https://doi.org/10.1002/gepi.21758
Cain DW, Cidlowski JA (2017) Immune regulation by glucocorticoids. Nat Rev Immunol 17(4):233–247. https://doi.org/10.1038/nri.2017.1
Coccurello R (2019) Anhedonia in depression symptomatology: appetite dysregulation and defective brain reward processing. Behav Brain Res 372:112041. https://doi.org/10.1016/j.bbr.2019.112041
Eckerling A, Ricon-Becker I, Sorski L, Sandbank E, Ben-Eliyahu S (2021) Stress and cancer: mechanisms, significance and future directions. Nat Rev Cancer 21(12):767–785. https://doi.org/10.1038/s41568-021-00395-5
Emdin CA, Khera AV, Kathiresan S (2017) Mendelian randomization. JAMA 318(19):1925. https://doi.org/10.1001/jama.2017.17219
Herbella FA, Neto SP, Santoro IL, Figueiredo LC (2015) Gastroesophageal reflux disease and non-esophageal cancer. WJG 21(3):815. https://doi.org/10.3748/wjg.v21.i3.815
Hsu CK, Lai CC, Wang K, Chen L (2016) Risk of lung cancer in patients with gastro-esophageal reflux disease: a population-based cohort study. PeerJ 4:e2753. https://doi.org/10.7717/peerj.2753
Ioannidou A, Watts EL, Perez-Cornago A et al (2022) The relationship between lipoprotein A and other lipids with prostate cancer risk: a multivariable Mendelian randomisation study. PLoS Med 19(1):e1003859. https://doi.org/10.1371/journal.pmed.1003859
Karagas NE, Rocha NP, Stimming EF (2020) Irritability in Huntington’s disease. JHD 9(2):107–113. https://doi.org/10.3233/JHD-200397
Li L, Ren Q, Zheng Q et al (2022) Causal associations between gastroesophageal reflux disease and lung cancer risk: a Mendelian randomization study. Cancer Med. https://doi.org/10.1002/cam4.5498. (Published online December 8, 2022)
Liu CH, Chen Z, Chen K et al (2021) Lipopolysaccharide-mediated chronic inflammation promotes tobacco carcinogen-induced lung cancer and determines the efficacy of immunotherapy. Can Res 81(1):144–157. https://doi.org/10.1158/0008-5472.CAN-20-1994
Luo J, le Cessie S, van Heemst D, Noordam R (2021) Diet-derived circulating antioxidants and risk of coronary heart disease. J Am Coll Cardiol 77(1):45–54. https://doi.org/10.1016/j.jacc.2020.10.048
Mao JJ, Pillai GG, Andrade CJ et al (2022) Integrative oncology: addressing the global challenges of cancer prevention and treatment. CA Cancer J Clin 72(2):144–164. https://doi.org/10.3322/caac.21706
McCarthy WJ, Meza R, Jeon J, Moolgavkar SH (2012) Chapter 6: Lung cancer in never smokers: epidemiology and risk prediction models: lung cancer in never smokers. Risk Anal 32:S69–S84. https://doi.org/10.1111/j.1539-6924.2012.01768.x
Nooreldeen R, Bach H (2021) Current and future development in lung cancer diagnosis. IJMS 22(16):8661. https://doi.org/10.3390/ijms22168661
Ong JS, An J, Han X et al (2022) Multitrait genetic association analysis identifies 50 new risk loci for gastro-oesophageal reflux, seven new loci for Barrett’s oesophagus and provides insights into clinical heterogeneity in reflux diagnosis. Gut 71(6):1053–1061. https://doi.org/10.1136/gutjnl-2020-323906
Rees JMB, Wood AM, Dudbridge F, Burgess S (2019) Robust methods in Mendelian randomization via penalization of heterogeneous causal estimates. PLoS ONE 14(9):e0222362. https://doi.org/10.1371/journal.pone.0222362
Sanderson E (2021) Multivariable Mendelian randomization and mediation. Cold Spring Harb Perspect Med 11(2):a038984. https://doi.org/10.1101/cshperspect.a038984
Schabath MB, Cote ML (2019) Cancer progress and priorities: lung cancer. Cancer Epidemiol Biomark Prev 28(10):1563–1579. https://doi.org/10.1158/1055-9965.EPI-19-0221
Siegel RL, Miller KD, Wagle NS, Jemal A (2023) Cancer statistics, 2023. CA Cancer J Clin 73(1):17–48. https://doi.org/10.3322/caac.21763
Theodoropoulos DS, Pecoraro DL, Efstratiadis SE (2002) The association of gastroesophageal reflux disease with asthma and chronic cough in the adult. Am J Respir Med 1(2):133–146. https://doi.org/10.1007/BF03256602
Verbanck M, Chen CY, Neale B, Do R (2018) Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat Genet 50(5):693–698. https://doi.org/10.1038/s41588-018-0099-7
Wang YH, Li JQ, Shi JF et al (2020) Depression and anxiety in relation to cancer incidence and mortality: a systematic review and meta-analysis of cohort studies. Mol Psychiatry 25(7):1487–1499. https://doi.org/10.1038/s41380-019-0595-x
Wu F, Huang Y, Hu J, Shao Z (2021) Mendelian randomization study of telomere length and bone mineral density. Aging 13(2):2015–2030. https://doi.org/10.18632/aging.202197
Yang H, Xia L, Chen J et al (2019) Stress–glucocorticoid–TSC22D3 axis compromises therapy-induced antitumor immunity. Nat Med 25(9):1428–1441. https://doi.org/10.1038/s41591-019-0566-4
Yarmolinsky J, Wade KH, Richmond RC et al (2018) Causal inference in cancer epidemiology: what is the role of mendelian randomization? Cancer Epidemiol Biomark Prev 27(9):995–1010. https://doi.org/10.1158/1055-9965.EPI-17-1177
Yuan S, Larsson SC (2022) Coffee and caffeine consumption and risk of kidney stones: a Mendelian randomization study. Am J Kidney Dis 79(1):9-14.e1. https://doi.org/10.1053/j.ajkd.2021.04.018
Zhang Z, Wang Y, Li Q (2018) Mechanisms underlying the effects of stress on tumorigenesis and metastasis (Review). Int J Oncol 53(6):2332–2342. https://doi.org/10.3892/ijo.2018.4570
Acknowledgements
We wish to acknowledge the participants and investigators of the Integrative Epidemiology Unit (IEU, https://gwas.mrcieu.ac.uk/).
Funding
This study was supported by Natural Science Foundation of Shanghai, China (No. 22Y31920400, and 22ZR1462400) and Shanghai Frontier Research Base of Disease and Syndrome Biology of Inflammatory cancer transformation (2021KJ03-12).
Author information
Authors and Affiliations
Contributions
AQ, LB designed the study and drafted the paper. LJJ, YLZ, HLZ, YYH, YBG, LX critically revised the paper. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
No conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Qi, A., Jiao, L., Zhang, Y. et al. Irritability and risk of lung cancer: a Mendelian randomization and mediation analysis. J Cancer Res Clin Oncol 149, 8649–8654 (2023). https://doi.org/10.1007/s00432-023-04791-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-04791-2