Abstract
Purpose
Although intracorporeal anastomosis (IA) appears to guarantee a faster recovery compared to extracorporeal anastomosis (EA), the data are still unclear. Thus, we performed a systematic review of the literature with meta-analysis to evaluate the recovery benefits of intracorporeal anastomosis.
Materials and methods
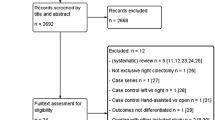
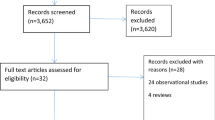
A systematic search was performed in electronic databases (PubMed, Web of Science, Scopus, EMBASE) using the following search terms in all possible combinations: “laparoscopic,” “right hemicolectomy,” “right colectomy,” “intracorporeal,” “extracorporeal,” and “anastomosis.” According to the pre-specified protocol, all studies evaluating the impact of choice of intra- or extracorporeal anastomosis after right hemicolectomy on time to first flatus and stools, hospital stay, and postoperative complications according to Clavien-Dindo classification were included.
Results
Sixteen articles were included in the final analysis, including 1862 patients who had undergone right hemicolectomy: 950 cases (IA) and 912 controls (EA). Patients who underwent IA reported a significantly shorter time to first flatus (MD = − 0.445, p = 0.013, Z = − 2.494, 95% CI − 0.795, 0.095), to first stools (MD = − 0.684, p < 0.001, Z = − 4.597, 95% CI − 0.976, 0.392), and a shorter hospital stay (MD = − 0.782, p < 0.001, Z = −3.867, 95% CI − 1.178, − 0.385) than those who underwent EA. No statistically significant differences in complications between the IA and EA patients were observed in the Clavien-Dindo I-II group (RD = − 0.014, p = 0.797, Z = − 0.257, 95% CI − 0.117, 0.090, number needed to treat (NNT) 74) or in the Clavien-Dindo IV-V (RD = − 0.005, p = 0.361, Z = − 0.933, 95% CI − 0.017, 0.006, NNT 184). The IA procedure led to fewer complications in the Clavien-Dindo III group (RD = − 0.041, p = 0.006, Z = − 2.731, 95% CI − 0.070, 0.012, NNT 24).
Conclusions
Although intracorporeal anastomosis appears to be safe in terms of postoperative complications and is potentially more effective in terms of recovery after surgery, further ad hoc randomized clinical trials are needed, given the heterogeneity of the data available in the current literature.



Similar content being viewed by others
References
Tinmouth J, Tomlinson G (2004) Laparoscopically assisted versus open colectomy for colon cancer. N Engl J Med 351(9):933–934. https://doi.org/10.1056/NEJM200408263510919
Jamali FR, Soweid AM, Dimassi H, Bailey C, Leroy J, Marescaux J (2008) Evaluating the degree of difficulty of laparoscopic colorectal surgery. Arch Surg 143(8):762–767. https://doi.org/10.1001/archsurg.143.8.762
Chang K, Fakhoury M, Barnajian M, Tarta C, Bergamaschi R (2013) Laparoscopic right colon resection with intracorporeal anastomosis. Surg Endosc 27(5):1730–1736. https://doi.org/10.1007/s00464-012-2665-x
Tarta CM, Bishawi M, Bergamaschi R (2013) Intracorporeal ileocolic anastomosis: a review. Tech Coloproct 17(5):479–485. https://doi.org/10.1007/s10151-013-0998-7
Simorov A, Shaligram A, Shostrom V, Boilesen E, Thompson J, Oleynikov D (2012) Laparoscopic colon resection trends in utilization and rate of conversion to open procedure: a national database review of academic medical centers. Ann Surg 256(3):462–468. https://doi.org/10.1097/SLA.0b013e3182657ec5
Carnuccio P, Jimeno J, Parés D (2014) Laparoscopic right colectomy: a systematic review and meta-analysis of observational studies comparing two types of anastomosis. Tech Coloproctol 18(1):5–12. https://doi.org/10.1007/s10151-013-1029-4
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097. https://doi.org/10.1371/journal.pmed.1000097
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range and the size of sample. BMC Med Res Methodol 5(1):13. https://doi.org/10.1186/1471-2288-5-13
Juni P, Witschi A, Bloch R et al (1999) The hazards of scoring the quality of clinical trials for meta-analysis. JAMA 282(11):1054–1060. https://doi.org/10.1001/jama.282.11.1054
Messori A, Maratea D, Fadda V, Trippoli S (2013) Using risk difference as opposed to odds-ratio in meta-analysis. Int J Cardiol 20(1):127. https://doi.org/10.1016/j.ijcard.2012.06.078
Citrome L, Ketter TA (2013) When does a difference make a difference? Interpretation of number needed to treat, number needed to harm, and likelihood to be helped or harmed. Int J Clin Pract 67(5):407–411. https://doi.org/10.1111/ijcp.12142
Sterne JA, Egger M, Smith GD (2001) Systematic reviews in health care: investigating and dealing with publication and other biases in meta-analysis. BMJ 323(7304):101–105. https://doi.org/10.1136/bmj.323.7304.101
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56(2):455–463. https://doi.org/10.1111/j.0006-341X.2000.00455.x
Scatizzi M, Kroning KC, Borrelli A, Andan G, Lenzi E, Feroci F (2010) Extracorporeal versus intracorporeal anastomosis after laparoscopic right colectomy for cancer: a case-control study. World J Surg 34(12):2902–2908. https://doi.org/10.1007/s00268-010-0743-6
Milone M, Elmore U, Di Salvo E, Delrio P, Bucci L, Ferulano GP, Napolitano C, Angiolini MR, Bracale U, Clemente M, D’Ambra M, Luglio G, Musella M, Pace U, Rosati R, Milone F (2015) Intracorporeal versus extracorporeal anastomosis. Results from a multicentre comparative study on 512 right-sided colorectal cancers. Surg Endosc 29(8):2314–2320. https://doi.org/10.1007/s00464-014-3950-7
Shapiro R, Keler U, Segev L, Sarna S, Hatib K, Hazzan D (2015) Laparoscopic right hemicolectomy with intracorporeal anastomosis: short- and long-term benefits in comparison with extracorporeal anastomosis. Surg Endosc 30(9):3823–3829. https://doi.org/10.1007/s00464-015-4684-x
Vignali A, Bissolati M, De Nardi P, Di Palo S, Staudacher C (2016) Extracorporeal vs. extracorporeal ileocolic stapled anastomoses in laparoscopic right colectomy: an interim analysis of a randomized clinical trial. J Laparoendosc Adv Surg Tech 26(5):1–6. https://doi.org/10.1089/lap.2015.0547
Magistro C, Lernia SD, Ferrari G, Zullino A, Mazzola M, De Martini P, De Carli S, Forgione A, Bertoglio CL, Pugliese R (2013) Totally laparoscopic versus laparoscopic-assisted right colectomy for colon cancer: is there any advantage in short-term outcomes? A prospective comparative assessment in our center. Surg Endosc 27(7):2613–2618. https://doi.org/10.1007/s00464-013-2799-5
Marchesi F, Pinna F, Percalli L, Cecchini S, Riccó M, Costi R, Pattonieri V, Roncoroni L (2013) Totally laparoscopic right colectomy: theoretical and practical advantages over the laparo-assisted approach. J Laparoendosc Adv Surg Tech 23(5):418–424. https://doi.org/10.1089/lap.2012.0420
Fabozzi M, Allieta R, Contul RB, Grivon M, Millo P, Lale-Murix E, Nardi M (2010) Comparison of short- and medium-term results between laparoscopically assisted and totally laparoscopic right hemicolectomy: a case-control study. Surg Endosc 24(9):2085–2091. https://doi.org/10.1007/s00464-010-0902-8
Chaves JA, Idoate CP, Fons JB et al (2011) A case-control study of extracorporeal versus intracorporeal anastomosis in patients subjected to right laparoscopic hemicolectomy. Cir Esp 89(1):24–30. https://doi.org/10.1016/j.ciresp.2010.10.003
Roscio F, Bertoglio C, De Luca A, Frattini P, Scandroglio I (2012) Totally laparoscopic versus laparoscopic assisted right colectomy for cancer. Int J Surg 10(6):290–295. https://doi.org/10.1016/j.ijsu.2012.04.020
Hanna MH, Hwang GS, Phelan MJ, Bui TL, Carmichael JC, Mills SD, Stamos MJ, Pigazzi A (2016) Laparoscopic right hemicolectomy: short- and long-term outcomes of intracorporeal versus extracorporeal anastomosis. Surg Endosc 30(9):3933–3942. https://doi.org/10.1007/s00464-015-4704-x
Vergis AS, Steigerwald SN, Bhojani FD, Sullivan PA, Hardy KM (2015) Laparoscopic right hemicolectomy with intracorporeal versus extracorporeal anastamosis: a comparison of short-term outcomes. Can J Surg 58(1):63–68. https://doi.org/10.1503/cjs.001914
Lee KH, Ho J, Akmal Y, Nelson R, Pigazzi A (2013) Short- and long-term outcomes of intracorporeal versus extracorporeal ileocolic anastomosis in laparoscopic right hemicolectomy for colon cancer. Surg Endosc 27(6):1986–1990. https://doi.org/10.1007/s00464-012-2698-1
Anania G, Santini M, Scagliarini L, Marzetti A, Vedana L, Marino S, Gregorio C, Resta G, Cavallesco G (2012) A totally mini invasive approach for colorectal laparoscopic surgery. World J Gastroenterol 18(29):3869–3874. https://doi.org/10.3748/wjg.v18.i29.3869.
Jian-Cheng T, Shu-Sheng W, Bo Z, Jian F, Liang Z (2016) Total laparoscopic right hemicolectomy with 3-step stapled intracorporeal isoperistaltic ileocolic anastomosis for colon cancer: an evaluation of short-term outcomes. Medicine (Baltimore) 95(48):e5538
Trastulli S, Coratti A, Guarino S, Piagnerelli R, Annecchiarico M, Coratti F, di Marino M, Ricci F, Desiderio J, Cirocchi R, Parisi A (2015) Robotic right colectomy with intracorporeal anastomosis compared with laparoscopic right colectomy with extracorporeal and intracorporeal anastomosis: a retrospective multicentre study. Surg Endosc 29(6):1512–1521. https://doi.org/10.1007/s00464-014-3835-9
Erguner I, Aytac E, Baca B, Hamzaoglu I, Karahasanoglu T (2013) Total laparoscopic approach for the treatment of right colon cancer: a technical critique. Asian J Surg 36(2):58–63. https://doi.org/10.1016/j.asjsur.2012.09.004
Feroci F, Lenzi E, Garzi A, Vannucchi A, Cantafio S, Scatizzi M (2013) Intracorporeal versus extracorporeal anastomosis after laparoscopic right hemicolectomy for cancer: a systematic review and meta-analysis. Int J Color Dis 28(9):1177–1186. https://doi.org/10.1007/s00384-013-1651-7
Rondelli F, Trastulli S, Avenia N, Schillaci G, Cirocchi R, Gullà N, Mariani E, Bistoni G, Nova G (2012) Laparoscopic right colectomy more effective than open resection? A meta-analysis of randomized and nonrandomized studies. Color Dis 14(8):e447–e469. https://doi.org/10.1111/j.1463-1318.2012.03054.x
Ricci C, Casadei R, Alagna V, Zani E, Taffurelli G, Pacilio CA, Minni F (2017) A critical and comprehensive systematic review and meta-analysis of studies comparing intracorporeal and extracorporeal anastomosis in laparoscopic right hemicolectomy. Langenbeck’s Arch Surg 402(3):417–427. https://doi.org/10.1007/s00423-016-1509-x
Van Oostendorp S, Elfrink A, Borstlap W, Schoonmade L, Sietses C, Meijerink J, Tuynman J (2017) Intracorporeal versus extracorporeal anastomosis in right hemicolectomy: a systematic review and meta-analysis. Surg Endosc 31(1):64–77. https://doi.org/10.1007/s00464-016-4982-y
Wu Q, Jin C, Hu T, Wei M, Wang Z (2017) Intracorporeal versus extracorporeal anastomosis in laparoscopic right colectomy: a systematic review and meta-analysis. J Laparoendosc Adv Surg Tech A 27(4):348–357. https://doi.org/10.1089/lap.2016.0485
Lu X-Y, Zhao C-F, Zhang T-T et al (2003) The practicability of the Changhai Pain Scale in the clinical pain assessment. N J Chin HA 20:6–7
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196. https://doi.org/10.1097/SLA.0b013e3181b13ca2
Author information
Authors and Affiliations
Contributions
Milone M: conception, design, interpretation of the data, and drafting of the article; Elmore U, Vignali A, Gennarelli N, Manigrasso M, Burati M, and Milone F: acquisition, analysis, and interpretation of the data; Milone F and De Palma GD: interpretation of the data and critical revisions; Delrio P and Rosati R: critical revisions and final approval.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Electronic supplementary material
Supplementary Figure 1
(JPEG 153 kb)
Supplementary Figure F1
Funnel plots analysis. a) time to first flatus; b) time to first stools; c) hospital stay; d) Clavien I-II; e) Clavien III; f) Clavien IV-V (JPEG 205 kb)
Supplementary Table T1
Operative data (DOCX 20 kb)
Rights and permissions
About this article
Cite this article
Milone, M., Elmore, U., Vignali, A. et al. Recovery after intracorporeal anastomosis in laparoscopic right hemicolectomy: a systematic review and meta-analysis. Langenbecks Arch Surg 403, 1–10 (2018). https://doi.org/10.1007/s00423-017-1645-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-017-1645-y