Abstract
Purpose
This study investigated non-invasive indices of post-exercise parasympathetic reactivation (using heart rate variability, HRV) and sympathetic withdrawal (using systolic time intervals, STI) following different exercise durations.
Methods
13 healthy males (age 26.4 ± 4.7 years) cycled at 70% heart rate (HR) reserve for two durations—8 min (SHORT) and 32 min (LONG)—on separate occasions: HRV (including natural logarithm of root mean square of successive differences, Ln-RMSSD) and STI (including pre-ejection period, PEP) were assessed throughout 10 min seated recovery.
Results
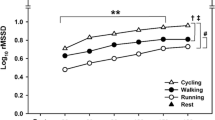
Exercise HR was similar between SHORT and LONG (146 ± 7 and 147 ± 6 b min−1, respectively; p = 0.173), as was HR deceleration during 10 min recovery (p = 0.199). HR remained elevated above baseline (p < 0.001) throughout recovery for both trials (SHORT 82 ± 13 b min−1; LONG 86 ± 10 b min−1, at 10 min post-exercise). Ln-RMSSD was similar at end-exercise between trials (SHORT 1.10 ± 0.30 ms; LONG 1.05 ± 0.73 ms; p = 0.656), though it recovered more rapidly following SHORT (p = 0.010), with differences apparent from 1 min (SHORT 2.29 ± 1.08 ms; LONG 1.85 ± 0.82 ms; p = 0.005) to 10 min post-exercise (SHORT 2.89 ± 0.80 ms; LONG 2.46 ± 0.70 ms; p = 0.007). Ln-RMSSD remained suppressed below baseline throughout recovery following both trials (p < 0.001). PEP was the same at end exercise for both trials (70 ± 6 ms), with exercise duration having no effect on recovery (p = 0.659). By 10 min post-exercise, PEP increased to 130 ± 21 ms (SHORT) and 131 ± 20 ms (LONG), which was similar to baseline (p ≥ 0.143).
Conclusions
Prolonged exercise duration attenuated the recovery of HRV indices of parasympathetic reactivation, but did not influence STI indices of sympathetic withdrawal. Therefore, duration must be considered when investigating post-exercise HRV. Monitoring these measures simultaneously can provide insights not revealed by underlying HR or either measure alone.


Similar content being viewed by others
Abbreviations
- ANOVA:
-
Analysis of variance
- b min−1 :
-
Beats per minute
- BMI:
-
Body mass index
- cPNA:
-
Cardiac parasympathetic neural activity
- cSNA:
-
Cardiac sympathetic neural activity
- DBP:
-
Diastolic blood pressure
- HF:
-
High frequency spectral power (0.15–1.50 Hz)
- HR:
-
Heart rate
- HRR60 :
-
Difference in heart rate between end of exercise and at 60 s of recovery
- HRV:
-
Heart rate variability
- LF:
-
Low frequency spectral power (0.04–0.15 Hz)
- Ln:
-
Natural logarithm transformation
- LONG:
-
Long duration exercise trial (32 min)
- LVET:
-
Left ventricular ejection time
- MAP:
-
Mean arterial pressure
- nu:
-
Normalized units (normalized to total spectral power)
- PEP:
-
Pre-ejection period
- Q :
-
Cardiac output
- RMSSD:
-
Root mean square of successive differences of R–R intervals
- RPE:
-
Rate of perceived exertion
- RPP:
-
Rate-pressure product
- RRI:
-
R–R interval
- SBP:
-
Systolic blood pressure
- SD:
-
Standard deviation
- SHORT:
-
Short duration exercise trial (8 min)
- STI:
-
Systolic time intervals
- SV:
-
Stroke volume
- SVR:
-
Systemic vascular resistance
- TP:
-
Total spectral power (0.04–1.50 Hz)
- VO2max :
-
Maximal rate of oxygen uptake
- VO2peak :
-
Peak rate of oxygen uptake achieved during an incremental exercise test
- VT1:
-
First ventilation threshold
References
Ahmed SS, Schwartz CJ, Levinson GE, Ettinger PO (1972) Systolic time intervals as measures of contractile state of left ventricular myocardium in man. Circulation 46(3):559–571
Barak OF, Klasnja A, Gacesa EP, Ovcin ZB, Grujic NG (2014) Gender differences in parasympathetic reactivation during recovery from Wingate anaerobic test. Period Biol 116(1):53–58
Bennett T, Wilcox RG, Macdonald IA (1984) Post-exercise reduction of blood-pressure in hypertensive men is not due to acute impairment of baroreflex function. Clin Sci 67(1):97–103
Berntson GG, Cacioppo JT, Quigley KS (1991) Autonomic determinism—the modes of autonomic control, the doctrine of autonomic space, and the laws of autonomic constraint. Psychol Rev 98(4):459–487. doi:10.1037/0033-295x.98.4.459
Berntson GG, Cacioppo JT, Binkley PF, Uchino BN, Quigley KS, Fieldstone A (1994) Autonomic cardiac control.3. Psychological stress and cardiac response in autonomic space as revealed by pharmacological blockades. Psychophysiology 31(6):599–608. doi:10.1111/j.1469-8986.1994.tb02352.x
Berntson GG, Norman GJ, Hawkley LC, Cacioppo JT (2008) Cardiac autonomic balance versus cardiac regulatory capacity. Psychophysiology 45(4):643–652. doi:10.1111/j.1469-8986.2008.00652.x
Billman GE (2013) The LF/HF ratio does not accurately measure cardiac sympatho-vagal balance. Front Physiol. doi:10.3389/fphys.2013.00026
Borg GAV (1982) Psychophysical bases of perceived exertion. Med Sci Sports Exerc 14(5):377–381. doi:10.1249/00005768-198205000-00012
Burgess HJ, Penev PD, Schneider R, Van Cauter E (2004) Estimating cardiac autonomic activity during sleep: impedance cardiography, spectral analysis, and Poincare plots. Clin Neurophysiol 115(1):19–28. doi:10.1016/s1388-2457(03)00312-2
Cacioppo JT, Berntson GG, Binkley PF, Quigley KS, Uchino BN, Fieldstone A (1994) Autonomic cardiac control.2. Noninvasive indexes and basal response as revealed by autonomic blockades. Psychophysiology 31(6):586–598. doi:10.1111/j.1469-8986.1994.tb02351.x
Camm AJ, Malik M, Bigger JT, Breithardt G, Cerutti S, Cohen RJ, Coumel P, Fallen EL, Kennedy HL, Kleiger RE, Lombardi F, Malliani A, Moss AJ, Rottman JN, Schmidt G, Schwartz PJ, Singer D (1996) Heart rate variability—standards of measurement, physiological interpretation, and clinical use. Circulation 93(5):1043–1065
Casonatto J, Tinucci T, Dourado AC, Polito M (2011) Cardiovascular and autonomic responses after exercise sessions with different intensities and durations. Clinics 66(3):453–458. doi:10.1590/s1807-59322011000300016
Cole CR, Blackstone EH, Pashkow FJ, Snader CE, Lauer MS (1999) Heart-rate recovery immediately after exercise as a predictor of mortality. N Engl J Med 341(18):1351–1357. doi:10.1056/nejm199910283411804
Daanen HAM, Lamberts RP, Kallen VL, Jin A, Van Meeteren NLU (2012) A systematic review on heart-rate recovery to monitor changes in training status in athletes. Int J Sports Physiol Perform 7(3):251–260
De Scalzi M, De Leonardis V, Citi S, Cinelli P (1986) Relationship between systolic time intervals and arterial blood pressure. Clin Cardiol 9(11):545–549
Eckberg DL (1997) Sympathovagal balance—a critical appraisal. Circulation 96(9):3224–3232
Goldberger JJ, Le FK, Lahiri M, Kannankeril PJ, Ng J, Kadish AH (2006) Assessment of parasympathetic reactivation after exercise. Am J Physiol Heart Circ Physiol 290(6):H2446–H2452. doi:10.1152/ajpheart.01118.2005
Goldstein DS, Bentho O, Park M-Y, Sharabi Y (2011) Low-frequency power of heart rate variability is not a measure of cardiac sympathetic tone but may be a measure of modulation of cardiac autonomic outflows by baroreflexes. Exp Physiol 96(12):1255–1261. doi:10.1113/expphysiol.2010.056259
Green M (2010) Risk stratification effective use of ACSM guidelines and integration of professional judgment. ACSMs Health Fit J 14(4):22–28. doi:10.1249/FIT.0b013e3181e34908
Guerra ZF, Pecanha T, Moreira DN, Silva LP, Laterza MC, Nakamura FY, Lima JRP (2014) Effects of load and type of physical training on resting and postexercise cardiac autonomic control. Clin Physiol Funct Imaging 34(2):114–120. doi:10.1111/cpf.12072
Harris WS, Schoenfe CD, Weissler AM (1967) Effects of adrenergic receptor activation and blockade on systolic preejection period heart rate and arterial pressure in man. J Clin Invest 46(11):1704–1714. doi:10.1172/jci105661
Horton TJ, Pagliassotti MJ, Hobbs K, Hill JO (1998) Fuel metabolism in men and women during and after long-duration exercise. J Appl Physiol 85(5):1823–1832
Kaikkonen P, Nummela A, Rusko H (2007) Heart rate variability dynamics during early recovery after different endurance exercises. Eur J Appl Physiol 102(1):79–86. doi:10.1007/s00421-007-0559-8
Kaikkonen P, Hynynen E, Mann T, Rusko H, Nummela A (2010) Can HRV be used to evaluate training load in constant load exercises? Eur J Appl Physiol 108(3):435–442. doi:10.1007/s00421-009-1240-1
Kawada T, Ikeda Y, Sugimachi M, Shishido T, Kawaguchi O, Yamazaki T, Alexander J, Sunagawa K (1996) Bidirectional augmentation of heart rate regulation by autonomic nervous system in rabbits. Am J Physiol Heart Circ Physiol 271(1):H288–H295
Kawada T, Miyamoto T, Miyoshi Y, Yamaguchi S, Tanabe Y, Kamiya A, Shishido T, Sugimachi M (2006) Sympathetic neural regulation of heart rate is robust against high plasma catecholamines. J Physiol Sci 56(3):235–245. doi:10.2170/physiolsci.RP006006
Krantz DS, Manuck SB (1984) Acute psychophysiologic reactivity and risk of cardiovascular-disease—a review and methodologic critique. Psychol Bull 96(3):435–464. doi:10.1037//0033-2909.96.3.435
Kubicek WG, Karnegis JN, Gatterso RP, Witsoe DA, Mattson RH (1966) Development and evaluation of an impedance cardiac output system. Aerosp Med 37(12):1208–1212
Lee QY, Redmond SJ, Chan GSH, Middleton PM, Steel E, Malouf P, Critoph C, Flynn G, O’Lone E, Lovell NH (2013) Estimation of cardiac output and systemic vascular resistance using a multivariate regression model with features selected from the finger photoplethysmogram and routine cardiovascular measurements. Biomed Eng Online. doi:10.1186/1475-925x-12-19
Levy MN (1971) Sympathetic-parasympathetic interactions in heart. Circ Res 29(5):437–445
MacDonald JR, MacDougall JD, Hogben CD (2000) The effects of exercise duration on post-exercise hypotension. J Hum Hypertens 14(2):125–129. doi:10.1038/sj.jhh.1000953
Martinmaki K, Rusko H (2008) Time-frequency analysis of heart rate variability during immediate recovery from low and high intensity exercise. Eur J Appl Physiol 102(3):353–360. doi:10.1007/s00421-007-0594-5
McEwen BS, Wingfield JC (2003) The concept of allostasis in biology and biomedicine. Horm Behav 43(1):2–15. doi:10.1016/S0018-506X(02)00024-7
Mendonca GV, Fernhall B, Heffernan KS, Pereira FD (2009) Spectral methods of heart rate variability analysis during dynamic exercise. Clin Auton Res 19(4):237–245. doi:10.1007/s10286-009-0018-1
Mezzacappa ES, Kelsey RM, Katkin ES, Sloan RP (2001) Vagal rebound and recovery from psychological stress. Psychosom Med 63(4):650–657
Michael S, Jay O, Halaki M, Graham K, Davis GM (2016) Submaximal exercise intensity modulates acute post-exercise heart rate variability. Eur J Appl Physiol 116(4):697–706. doi:10.1007/s00421-016-3327-9
Miyamoto T, Kawada T, Takaki H, Inagaki M, Yanagiya Y, Jin YT, Sugimachi M, Sunagawa K (2003) High plasma norepinephrine attenuates the dynamic heart rate response to vagal stimulation. Am J Physiol Heart Circ Physiol 284(6):H2412–H2418. doi:10.1152/ajpheart.00660.2002
Nandi PS, Spodick DH (1977) Recovery from exercise at varying work loads—time course of responses of heart-rate and systolic intervals. Br Heart J 39(9):958–966
Nishiyasu T, Tan N, Morimoto K, Nishiyasu M, Yamaguchi Y, Murakami N (1994) Enhancement of parasympathetic cardiac activity during activation of muscle metaboreflex in humans. J Appl Physiol 77(6):2778–2783
Obrist PA, Light KC, James SA, Strogatz DS (1987) Cardiovascular-responses to stress.1. Measures of myocardial response and relationship to high resting systolic pressure and parental hypertension. Psychophysiology 24(1):65–78. doi:10.1111/j.1469-8986.1987.tb01864.x
Perini R, Orizio C, Comande A, Castellano M, Beschi M, Veicsteinas A (1989) Plasma norepinephrine and heart-rate dynamics during recovery from submaximal exercise in man. Eur J Appl Physiol Occup Physiol 58(8):879–883. doi:10.1007/bf02332222
Romijn JA, Coyle EF, Sidossis LS, Gastaldelli A, Horowitz JF, Endert E, Wolfe RR (1993) Regulation of endogenous fat and carbohydrate metabolism in relation to exercise intensity and duration. Am J Physiol Endocrinol Metab 265(3):E380–E391
Rousson D, Galleyrand J, Silie M, Boissel JP (1987) Uncorrected preejection period - A simple noninvasive measurement for pharmacodynamic screening of inotropic activity. Eur J Clin Pharmacol 31(5):559–562. doi:10.1007/bf00606630
Salomon K, Matthews KA, Allen MT (2000) Patterns of sympathetic and parasympathetic reactivity in a sample of children and adolescents. Psychophysiology 37(6):842–849. doi:10.1017/s0048577200990607
Seiler S, Haugen O, Kuffel E (2007) Autonomic recovery after exercise in trained athletes: intensity and duration effects. Med Sci Sports Exerc 39(8):1366–1373. doi:10.1249/mss.0b013e318060f17d
Sherwood A, Allen MT, Fahrenberg J, Kelsey RM, Lovallo WR, Vandoornen LJP (1990) Methodological guidelines for impedance cardiography. Psychophysiology 27(1):1–23. doi:10.1111/j.1469-8986.1990.tb02171.x
Stanley J, Peake JM, Buchheit M (2013) Cardiac parasympathetic reactivation following exercise: implications for training prescription. Sports Med 43(12):1259–1277. doi:10.1007/s40279-013-0083-4
Sunagawa K, Kawada T, Nakahara T (1998) Dynamic nonlinear vago-sympathetic interaction in regulating heart rate. Heart Vessels 13(4):157–174. doi:10.1007/bf01745040
Tarvainen MP, Ranta-aho PO, Karjalainen PA (2002) An advanced detrending method with application to HRV analysis. IEEE Trans Biomed Eng 49(2):172–175. doi:10.1109/10.979357
Tsuji H, Larson MG, Venditti FJ, Manders ES, Evans JC, Feldman CL, Levy D (1996) Impact of reduced heart rate variability on risk for cardiac events—the Framingham heart study. Circulation 94(11):2850–2855
Uijtdehaage SHJ, Thayer JF (2000) Accentuated antagonism in the control of human heart rate. Clin Auton Res 10(3):107–110. doi:10.1007/bf02278013
White DW, Raven PB (2014) Autonomic neural control of heart rate during dynamic exercise: revisited. J Physiol (Lond) 592(12):2491–2500. doi:10.1113/jphysiol.2014.271858
Zoccali C, Mallamaci F, Parlongo S, Cutrupi S, Benedetto FA, Tripepi G, Bonanno G, Rapisarda F, Fatuzzo P, Seminara G, Cataliotti A, Stancanelli B, Malatino LS (2002) Plasma norepinephrine predicts survival and incident cardiovascular events in patients with end-stage renal disease. Circulation 105(11):1354–1359. doi:10.1161/hc1102.105261
Acknowledgements
The authors would like to thank the participants who volunteered for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the University of Sydney Human Research Ethics Committee (HREC reference: 2014/894) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Communicated by Massimo Pagani.
Rights and permissions
About this article
Cite this article
Michael, S., Jay, O., Graham, K.S. et al. Longer exercise duration delays post-exercise recovery of cardiac parasympathetic but not sympathetic indices. Eur J Appl Physiol 117, 1897–1906 (2017). https://doi.org/10.1007/s00421-017-3673-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-017-3673-2