Abstract
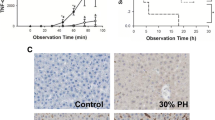
Liver dysfunction is a serious complication in the early phase following major liver resection or liver transplantation and might be aggravated by the translocation of bacteria and lipopolysaccharide (LPS). As a preventive strategy, granulocyte colony-stimulating factor (G-CSF) is prophylactically applied in patients who are subjected to major surgery. However, we previously demonstrated that G-CSF can induce LPS sensitization. In this study, we aimed to evaluate the effects of G-CSF pretreatment on hepatic microcirculatory disturbances and postoperative liver dysfunction after 70 % partial hepatectomy (PH) in rats. PH alone was well tolerated by all animals (100 % survival rate, slight liver damage and inflammation). LPS application after 70 % PH caused moderate inflammation, microcirculatory disturbances and hepatic damage and led to a 24-h survival rate of 30 % after the operations. In the G-CSF–LPS–PH group, all of the rats died within 4 h with severe inflammatory responses and liver damage (i.e., pronounced erythrocyte congestion and neutrophil infiltration). Portal hypertension and microcirculatory disorders (i.e., inhomogeneous perfusion, sinusoidal dilatation and reductions on functional capillary density) were more pronounced in the G-CSF–LPS–PH group. In conclusion, increased circulating LPS levels were associated with an imbalanced inflammatory response and microcirculatory dysfunction that preceded liver damage and subsequent dysfunction following surgery. G-CSF-pretreatment aggravated microcirculatory disturbances and liver damage, which might have been related to G-CSF-induced LPS sensitization.







Similar content being viewed by others
References
Adam R, Bhangui P, Vibert E, Azoulay D, Pelletier G, Duclos-Vallee JC, Samuel D, Guettier C, Castaing D (2012) Resection or transplantation for early hepatocellular carcinoma in a cirrhotic liver: does size define the best oncological strategy? Ann Surg 256:883–891
Baveja R, Keller S, Yokoyama Y, Sonin N, Clemens MG, Zhang JX (2002a) LPS-induced imbalanced expression of hepatic vascular stress genes in cirrhosis: possible mechanism of increased susceptibility to endotoxemia. Shock 17:316–321
Baveja R, Kresge N, Ashburn JH, Keller S, Yokoyama Y, Sonin N, Zhang JX, Huynh T, Clemens MG (2002b) Potentiated hepatic microcirculatory response to endothelin-1 during polymicrobial sepsis. Shock 18:415–422
Bernal W, Auzinger G, Dhawan A, Wendon J (2010) Acute liver failure. Lancet 376:190–201
Bo L, Wang F, Zhu J, Li J, Deng X (2011) Granulocyte-colony stimulating factor (G-CSF) and granulocyte-macrophage colony stimulating factor (GM-CSF) for sepsis: a meta-analysis. Crit Care 15:R58
Boermeester MA, Straatsburg IH, Houdijk AP, Meyer C, Frederiks WM, Wesdorp RI, van Noorden CJ, van Leeuwen PA (1995) Endotoxin and interleukin-1 related hepatic inflammatory response promotes liver failure after partial hepatectomy. Hepatology 22:1499–1506
Fang H, Liu A, Sun J, Kitz A, Dirsch O, Dahmen U (2013) Granulocyte colony stimulating factor induces lipopolysaccharide (LPS) sensitization via upregulation of LPS binding protein in rat. PLoS One 8:e56654
Helling TS (2006) Liver failure following partial hepatectomy. HPB (Oxford) 8:165–174
Huang H, Deng M, Jin H, Liu A, Dirsch O, Dahmen U (2011) Hepatic arterial perfusion is essential for the spontaneous recovery from focal hepatic venous outflow obstruction in rats. Am J Transplant 11:2342–2352
Kasravi FB, Wang L, Wang XD, Molin G, Bengmark S, Jeppsson B (1996) Bacterial translocation in acute liver injury induced by D-galactosamine. Hepatology 23:97–103
Keller S, Karaa A, Paxian M, Clemens MG, Zhang JX (2006) Inhibition of endothelin-1-mediated up-regulation of iNOS by bosentan ameliorates endotoxin-induced liver injury in cirrhosis. Shock 25:306–313
Kim JB, Han AR, Park EY, Kim JY, Cho W, Lee J, Seo EK, Lee KT (2007) Inhibition of LPS-induced iNOS, COX-2 and cytokines expression by poncirin through the NF-kappaB inactivation in RAW 264.7 macrophage cells. Biol Pharm Bull 30:2345–2351
Kimura F, Shimizu H, Yoshidome H, Ohtsuka M, Kato A, Yoshitomi H, Nozawa S, Furukawa K, Mitsuhashi N, Sawada S, Takeuchi D, Ambiru S, Miyazaki M (2006) Circulating cytokines, chemokines, and stress hormones are increased in patients with organ dysfunction following liver resection. J Surg Res 133:102–112
Klune JR, Dhupar R, Cardinal J, Billiar TR, Tsung A (2008) HMGB1: endogenous danger signaling. Mol Med 14:476–484
Lemoli RM, Catani L, Talarico S, Loggi E, Gramenzi A, Baccarani U, Fogli M, Grazi GL, Aluigi M, Marzocchi G, Bernardi M, Pinna A, Bresadola F, Baccarani M, Andreone P (2006) Mobilization of bone marrow-derived hematopoietic and endothelial stem cells after orthotopic liver transplantation and liver resection. Stem Cells 24:2817–2825
Liu A, Dirsch O, Fang H, Sun J, Jin H, Dong W, Dahmen U (2011) HMGB1 in ischemic and non-ischemic liver after selective warm ischemia/reperfusion in rat. Histochem Cell Biol 135:443–452
Liu A, Fang H, Dirsch O, Jin H, Dahmen U (2012) Oxidation of HMGB1 causes attenuation of its pro-inflammatory activity and occurs during liver ischemia and reperfusion. PLoS One 7:e35379
Lundblad R, Nesland JM, Giercksky KE (1996) Granulocyte colony-stimulating factor improves survival rate and reduces concentrations of bacteria, endotoxin, tumor necrosis factor, and endothelin-1 in fulminant intra-abdominal sepsis in rats. Crit Care Med 24:820–826
Madrahimov N, Dirsch O, Broelsch C, Dahmen U (2006) Marginal hepatectomy in the rat: from anatomy to surgery. Ann Surg 244:89–98
Mochida S, Ogata I, Hirata K, Ohta Y, Yamada S, Fujiwara K (1990) Provocation of massive hepatic necrosis by endotoxin after partial hepatectomy in rats. Gastroenterology 99:771–777
Ogata T, Yamashita K, Horiuchi H, Okuda K, Todo S (2008) A novel tumor necrosis factor-alpha suppressant, ONO-SM362, prevents liver failure and promotes liver regeneration after extensive hepatectomy. Surgery 143:545–555
Palmes D, Minin E, Budny T, Uhlmann D, Armann B, Stratmann U, Herbst H, Spiegel HU (2005) The endothelin/nitric oxide balance determines small-for-size liver injury after reduced-size rat liver transplantation. Virchows Arch 447:731–741
Quigley M (1994) Bacterial translocation in acute and chronic portal hypertension. Hepatology 20:264–266
Rensing H, Bauer I, Zhang JX, Paxian M, Pannen B, Yokoyama Y, Clemens MG, Bauer M (2002) Endothelin-1 and heme oxygenase-1 as modulators of sinusoidal tone in the stress-exposed rat liver. Hepatology 36:1453–1465
Singer G, Urakami H, Specian RD, Stokes KY, Granger DN (2006) Platelet recruitment in the murine hepatic microvasculature during experimental sepsis: role of neutrophils. Microcirculation 13:89–97
Sonin NV, Garcia-Pagan JC, Nakanishi K, Zhang JX, Clemens MG (1999) Patterns of vasoregulatory gene expression in the liver response to ischemia/reperfusion and endotoxemia. Shock 11:175–179
Ulloa L, Messmer D (2006) High-mobility group box 1 (HMGB1) protein: friend and foe. Cytokine Growth Factor Rev 17:189–201
van den Broek MA, Olde Damink SW, Dejong CH, Lang H, Malago M, Jalan R, Saner FH (2008) Liver failure after partial hepatic resection: definition, pathophysiology, risk factors and treatment. Liver Int 28:767–780
van Leeuwen PA, Hong RW, Rounds JD, Rodrick ML, Wilmore D (1991) Hepatic failure and coma after liver resection is reversed by manipulation of gut contents: the role of endotoxin. Surgery 110:169–174
Wahl JR, Goetsch NJ, Young HJ, Van Maanen RJ, Johnson JD, Pea AS, Brittingham A (2005) Murine macrophages produce endothelin-1 after microbial stimulation. Exp Biol Med (Maywood) 230:652–658
Wang XD, Soltesz V, Andersson R, Bengmark S (1993) Bacterial translocation in acute liver failure induced by 90 % hepatectomy in the rat. Br J Surg 80:66–71
Xu CP, Liu J, Liu JC, Han DW, Zhang Y, Zhao YC (2007) Dynamic changes and mechanism of intestinal endotoxemia in partially hepatectomized rats. World J Gastroenterol 13:3592–3597
Yuan Q, Liu YY, Sun K, Chen CH, Zhou CM, Wang CS, Li A, Zhang SW, Ye ZL, Fan JY, Han JY (2009) Improving effect of pretreatment with yiqifumai on LPS-induced microcirculatory disturbance in rat mesentery. Shock 32:310–316
Acknowledgments
This study was supported by the German Federal Ministry for Education and Research (BMBF) Virtual Liver Network (VLN, C6), the National Natural Science Fund of China (NSFC) (81300343), and the Anhui Provincial Natural Science Foundation (1408085QH170). We thank Stephanie Lange for her excellent animal care.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liu, A., Fang, H., Wei, W. et al. G-CSF pretreatment aggravates LPS-associated microcirculatory dysfunction and acute liver injury after partial hepatectomy in rats. Histochem Cell Biol 142, 667–676 (2014). https://doi.org/10.1007/s00418-014-1242-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-014-1242-x