Abstract
Background
Symptomatic isolated carotid artery occlusions (ICAO) can lead to disability, recurrent stroke, and mortality, but natural history and best therapeutic management remain poorly known. The objective of this study was to describe our cohort of ICAO patients with an initial medical management.
Methods
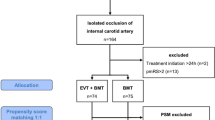
We conducted a retrospective study including consecutive patients admitted to our Comprehensive Stroke Center for ICAO within 24 h after stroke onset between January 2016 and September 2018. Patients with immediate endovascular therapy (EVT) were excluded. Medical treatment was based on anticoagulation (delayed by 24 h if intravenous thrombolysis was performed). ‘Rescue’ EVT was considered if first-week neurological deterioration (FWND) occurred.
Results
Fifty-six patients were included, with a median National Institutes of Health Stroke Scale (NIHSS) of 3. Eleven patients (20%) had FWND during the first week, four benefited from rescue EVT. A mismatch volume > 40 cc on initial perfusion imaging and FLAIR vascular hyperintensities were associated with FWND (p = 0.007 and p = 0.009, respectively). Thirty-eight patients (69%) had a good outcome (modified Rankin Scale mRS 0–2) at 3 months, 36 (69%) had an excellent outcome (mRS 0–1). Seventeen patients (38%) had carotid patency on 3-month control imaging. Recurrences occurred in six (13%) of the survivors (mean follow-up: 13.6 months).
Conclusion
Our results suggest that the prognosis of patients with acute ICAO was favorable with a medical strategy, albeit a substantial rate of FWND and recurrence. FWND was well predicted by a core-perfusion mismatch volume > 40 cc. Randomized controlled trials are necessary to assess the benefit of EVT in ICAO.


Similar content being viewed by others
References
Powers WJ (2003) Atherosclerotic carotid artery occlusion. Curr Treat Options Cardiovasc Med 5:501–509. https://doi.org/10.1007/s11936-003-0039-3
Flaherty ML, Flemming KD, McClelland R et al (2004) Population-based study of symptomatic internal carotid artery occlusion: incidence and long-term follow-up. Stroke 35:e349–e352. https://doi.org/10.1161/01.STR.0000135024.54608.3f
Paciaroni M, Caso V, Venti M et al (2005) Outcome in patients with stroke associated with internal carotid artery occlusion. Cerebrovasc Dis 20:108–113. https://doi.org/10.1159/000086800
Paciaroni M, Agnelli G, Caso V et al (2012) Intravenous thrombolysis for acute ischemic stroke associated to extracranial internal carotid artery occlusion: the ICARO-2 study. Cerebrovasc Dis 34:430–435. https://doi.org/10.1159/000345081
Hankey GJ, Warlow CP (1991) Prognosis of symptomatic carotid artery occlusion. Cerebrovasc Dis 1:245–256. https://doi.org/10.1159/000108851
Klijn CJ, Kappelle LJ, Tulleken CA, van Gijn J (1997) Symptomatic carotid artery occlusion. A reappraisal of hemodynamic factors. Stroke 28:2084–2093. https://doi.org/10.1161/01.str.28.10.2084
Klijn CJM, van Buren PA, Kappelle LJ et al (2000) Outcome in patients with symptomatic occlusion of the internal carotid artery. Eur J Vasc Endovasc Surg 19:579–586. https://doi.org/10.1053/ejvs.2000.1129
Grubb RL, Derdeyn CP, Fritsch SM et al (1998) Importance of hemodynamic factors in the prognosis of symptomatic carotid occlusion. JAMA 280:6. https://doi.org/10.1001/jama.280.12.1055
Lanari A, Silvestrelli G (2012) Acute and chronic carotid occlusion syndromes. In: Paciaroni M, Agnelli G, Caso V, Bogousslavsky J (eds) Frontiers of neurology and neuroscience. Karger, Basel, pp 185–190
Bhatia R, Hill MD, Shobha N et al (2010) Low rates of acute recanalization with intravenous recombinant tissue plasminogen activator in ischemic stroke: real-world experience and a call for action. Stroke 41:2254–2258. https://doi.org/10.1161/STROKEAHA.110.592535
Paciaroni M, Balucani C, Agnelli G et al (2012) Systemic thrombolysis in patients with acute ischemic stroke and internal carotid artery occlusion: the ICARO study. Stroke 43:125–130. https://doi.org/10.1161/STROKEAHA.111.630624
Yeo LLL, Kong WY, Paliwal P et al (2016) Intravenous thrombolysis for acute ischemic stroke due to cervical internal carotid artery occlusion. J Stroke Cerebrovasc Dis 25:2423–2429. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.06.014
Goyal M, Menon BK, van Zwam WH et al (2016) Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomised trials. Lancet Lond Engl 387:1723–1731. https://doi.org/10.1016/S0140-6736(16)00163-X
Mokin M, Kass-Hout T, Kass-Hout O et al (2012) Intravenous thrombolysis and endovascular therapy for acute ischemic stroke with internal carotid artery occlusion: a systematic review of clinical outcomes. Stroke 43:2362–2368. https://doi.org/10.1161/STROKEAHA.112.655621
Paciaroni M, Inzitari D, Agnelli G et al (2015) Intravenous thrombolysis or endovascular therapy for acute ischemic stroke associated with cervical internal carotid artery occlusion: the ICARO-3 study. J Neurol 262:459–468. https://doi.org/10.1007/s00415-014-7550-1
Jadhav A, Panczykowski D, Jumaa M et al (2018) Angioplasty and stenting for symptomatic extracranial non-tandem internal carotid artery occlusion. J NeuroInterv Surg 10:1155–1160. https://doi.org/10.1136/neurintsurg-2018-013810
Adams HP, Bendixen BH, Leira E et al (1999) Antithrombotic treatment of ischemic stroke among patients with occlusion or severe stenosis of the internal carotid artery: a report of the Trial of Org 10172 in Acute Stroke Treatment (TOAST). Neurology 53:122–125. https://doi.org/10.1212/wnl.53.1.122
Damania D, Kung NT-M, Jain M et al (2016) Factors associated with recurrent stroke and recanalization in patients presenting with isolated symptomatic carotid occlusion. Eur J Neurol 23:127–132. https://doi.org/10.1111/ene.12819
EC/IC Bypass Study Group (1985) Failure of extracranial-intracranial arterial bypass to reduce the risk of ischemic stroke. N Engl J Med 313:1191–1200. https://doi.org/10.1056/NEJM198511073131904
Powers WJ, Clarke WR, Grubb RL et al (2011) Extracranial-intracranial bypass surgery for stroke prevention in hemodynamic cerebral ischemia: the carotid occlusion surgery study randomized trial. JAMA 306:1983–1992. https://doi.org/10.1001/jama.2011.1610
Seners P, Turc G, Tisserand M et al (2014) Unexplained early neurological deterioration after intravenous thrombolysis: incidence, predictors, and associated factors. Stroke 45:2004–2009. https://doi.org/10.1161/STROKEAHA.114.005426
Kernan WN, Ovbiagele B, Black HR et al (2014) Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 45:2160–2236. https://doi.org/10.1161/STR.0000000000000024
Rebello LC, Bouslama M, Haussen DC et al (2017) Endovascular treatment for patients with acute stroke who have a large ischemic core and large mismatch imaging profile. JAMA Neurol 74:34. https://doi.org/10.1001/jamaneurol.2016.3954
Hacke W (1995) Intravenous thrombolysis with recombinant tissue plasminogen activator for acute hemispheric stroke. The European Cooperative Acute Stroke Study (ECASS). JAMA J Am Med Assoc 274:1017–1025. https://doi.org/10.1001/jama.274.13.1017
Adams HP, Bendixen BH, Kappelle LJ et al (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24:35–41. https://doi.org/10.1161/01.STR.24.1.35
Hause S, Oldag A, Breja A et al (2019) Acute symptomatic extracranial internal carotid occlusion—natural course and clinical impact. Vasa. https://doi.org/10.1024/0301-1526/a000826
Albers GW, Marks MP, Kemp S et al (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med 378:708–718. https://doi.org/10.1056/NEJMoa1713973
Mazya MV, Cooray C, Lees KR et al (2018) Minor stroke due to large artery occlusion. When is intravenous thrombolysis not enough? Results from the SITS International Stroke Thrombolysis Register. Eur Stroke J 3:29–38. https://doi.org/10.1177/2396987317746003
Xu B, Li C, Guo Y et al (2017) Current understanding of chronic total occlusion of the internal carotid artery (review). Biomed Rep. https://doi.org/10.3892/br.2017.1033
Legrand L, Tisserand M, Turc G et al (2015) Do FLAIR vascular hyperintensities beyond the DWI lesion represent the ischemic penumbra? Am J Neuroradiol 36:269–274. https://doi.org/10.3174/ajnr.A4088
Saver JL, Goyal M, Bonafe A et al (2015) Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. N Engl J Med 372:2285–2295. https://doi.org/10.1056/NEJMoa1415061
Campbell BCV, Mitchell PJ, Kleinig TJ et al (2015) Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med 372:1009–1018. https://doi.org/10.1056/NEJMoa1414792
Dargazanli C, Arquizan C, Gory B et al (2017) Mechanical thrombectomy for minor and mild stroke patients harboring large vessel occlusion in the anterior circulation: a multicenter cohort study. Stroke 48:3274–3281. https://doi.org/10.1161/STROKEAHA.117.018113
Cagnazzo F, Dargazanli C, Lefevre P-H et al (2019) Chronic occlusion of the internal carotid artery: endovascular revascularization technique of long occlusive lesions. J Neuroradiol. https://doi.org/10.1016/j.neurad.2019.05.005
Acknowledgements
Authors would like to thank Mrs Hattinguais Jessica for assistance in data collection.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
CA and AS planned the study data collection, identified the patient cohort, gathered the data, and drafted the manuscript; CD and AS did the statistical analysis. All authors contributed to data collection, made suggestions on analysis, and approved the final manuscript. Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethics approval
This study has been approved by local institutional review board (IRB 202000337) of Montpellier University Hospital, waiving need for informed consent due to the observational design.
Consent for publication
Informed consent has been waving by local IRB due to the study observational design.
Availability of data and material
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ter Schiphorst, A., Gaillard, N., Dargazanli, C. et al. Symptomatic isolated internal carotid artery occlusion with initial medical management: a monocentric cohort. J Neurol 268, 346–355 (2021). https://doi.org/10.1007/s00415-020-10118-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-020-10118-9