Abstract
Background
Chronic obstructive pulmonary disease (COPD) typically includes neutrophilic airway inflammation and eosinophilic inflammation in some cases. Inhaled corticosteroid (ICS) suppresses eosinophilic inflammation of the airway and reduces acute exacerbation (AE). The present study investigated the relationship between ICS and AE in patients with COPD classified by blood eosinophil counts.
Methods
Overall, 244 patients with COPD were retrospectively evaluated between 2014 and 2017 and classified into two groups based on blood eosinophil counts (≥ 300/μL and < 300/μL). These patients were then reclassified into subgroups of those with and without ICS. Differences in the characteristics and incidence of AE and pneumonia with AE in each subgroup were evaluated retrospectively.
Results
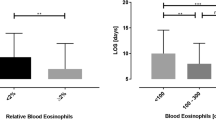
All patients with ICS used 320 μg budesonide twice daily. In the group with blood eosinophil counts ≥ 300/μL, patients with ICS had a significantly lower incidence of AE than those without ICS (P = 0.023). Meanwhile, no significant differences were observed in incidence of AE in the group with blood eosinophil counts < 300/μL. In the group with blood eosinophil counts < 300/μL, patients with ICS had a higher incidence of pneumonia with AE (P = 0.009). Conversely, no significant differences were observed in the group with blood eosinophil counts ≥ 300/μL.
Conclusions
ICS significantly reduced AE in COPD patients with blood eosinophil counts ≥ 300/μL. Meanwhile, ICS significantly increased pneumonia rate in patients with blood eosinophil count < 300/μL. Blood eosinophil count may be a useful indicator to identify the benefits and risks of ICS in COPD.

Similar content being viewed by others
Data Availability
All data used and generated in this study are available from the authors upon reasonable request.
References
Vogelmeier CF, Criner GJ, Martinez FJ et al (2017) Global strategy for the diagnosis, management, and prevention of chronic obstructive lung disease 2017 report: GOLD executive summary. Am J Respir Crit Care Med 195:557–582
Leigh R, Pizzichini MM, Morris MM et al (2006) Stable COPD: predicting benefit from high-dose inhaled corticosteroid treatment. Eur Respir J 27:964–971
Brightling CE, McKenna S, Hargadon B et al (2005) Sputum eosinophilia and the short term response to inhaled mometasone in chronic obstructive pulmonary disease. Thorax 60:193–198
Eltboli O, Bafadhel M, Hollins F et al (2014) COPD exacerbation severity and frequency is associated with impaired macrophage efferocytosis of eosinophils. BMC Pulm Med 14:112
Pizzichini E, Pizzichini MM, Gibson P et al (1998) Sputum eosinophilia predicts benefit from prednisone in smokers with chronic obstructive bronchitis. Am J Respir Crit Care Med 158:1511–1517
Bafadhel M, McKenna S, Terry S et al (2011) Acute exacerbations of chronic obstructive pulmonary disease: identification of biologic clusters and their biomarkers. Am J Respir Crit Care Med 184:662–671
Negewo NA, McDonald VM, Baines KJ et al (2016) Peripheral blood eosinophils: a surrogate marker for airway eosinophilia in stable COPD. Int J Chron Obstruct Pulmon Dis 11:1495–1504
Suissa S, Dell’Aniello S, Ernst P (2019) Comparative effects of LAMA-LABA-ICS vs LAMA-LABA for COPD: Cohort Study in Real-World Clinical Practice. Chest 157:846–855
Schumann DM, Tamm M, Kostikas K et al (2019) Stability of the blood eosinophilic phenotype in stable and exacerbated COPD. Chest 156:456–465
Japanese Respiratory Society (2018) The JRS guidelines for the management of chronic obstructive pulmonary disease. Medical Review
Proboszcz M, Mycroft K, Paplinska-Goryca M et al (2019) Relationship between blood and induced sputum eosinophils, bronchial hyperresponsiveness and reversibility of airway obstruction in mild-to-moderate chronic obstructive pulmonary disease. COPD 16:354–361
Siddiqui SH, Guasconi A, Vestbo J et al (2015) Blood eosinophils: a biomarker of response to extrafine beclomethasone/formoterol in chronic obstructive pulmonary disease. Am J Respir Crit Med 192:523–525
Vedel-Krogh S, Nielsen SF, Lange P et al (2016) Blood eosinophils and exacerbations in chronic obstructive pulmonary disease. The Copenhagen General Population Study. Am J Respir Crit Care Med 193:965–974
Pavord ID, Lettis S, Anzueto A et al (2016) Blood eosinophil count and pneumonia risk in patients with chronic obstructive pulmonary disease: a patient-level meta-analysis. Lancet Respir Med 4:731–741
Vedel-Krogh S, Nordestgaard BG, Lange P et al (2018) Blood eosinophil count and risk of pneumonia hospitalisations in individuals with COPD. Eur Respir J 51:1800120
Pascoe S, Locantore N, Dransfield MT et al (2015) Blood eosinophil counts, exacerbations, and response to the addition of inhaled fluticasone furoate to vilanterol in patients with chronic obstructive pulmonary disease: a secondary analysis of data from two parallel randomised controlled trials. Lancet Respir Med 3:435–442
Wedzicha JA (2016) Eosinophils as biomarkers of chronic obstructive pulmonary disease exacerbation risk. Maybe just for some? Am J Respir Crit Care Med 193:937–938
Roche N, Chapman KR, Vogelmeier CF et al (2017) Blood eosinophils and response to maintenance chronic obstructive pulmonary disease treatment. Data from the FLAME Trial. Am J Respir Crit Care Med 195:1189–1197
Ernst P, Gonzalez AV, Brassard P et al (2010) Inhaled corticosteroid use in chronic obstructive pulmonary disease and the risk of hospitalization for pneumonia. Am J Respir Crit Care Med 176:162–166
Joo MJ, Au DH, Fitzgibbon ML et al (2010) Inhaled corticosteroid and risk of pneumonia in newly diagnosed COPD. Respir Med 104:246–252
Ernst P, Gonzalez AV, Brassard P et al (2007) Inhaled corticosteroid use in chronic obstructive pulmonary disease and the risk of hospitalization for pneumonia. Am J Respir Crit Care Med 176:162–166
Suissa S, Coulombe J, Ernst P (2015) Discontinuation of inhaled corticosteroids in COPD and the risk reduction of pneumonia. Chest 148:1177–1183
Funding
None.
Author information
Authors and Affiliations
Contributions
ZS designed the study and drafted the manuscript. KK made substantial contributions to analysis and interpretation of data. MY, AK, KT, and TH contributed to data collection, analysis, and review of this manuscript. All authors read and approved the final manuscript. We are grateful to all the patients who participated in the current study.
Corresponding author
Ethics declarations
Conflict of interest
No potential conflict of interest exist with any companies/organizations whose products or services may be discussed in this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Saito, Z., Yoshida, M., Kojima, A. et al. Benefits and Risks of Inhaled Corticosteroid Treatment in Patients with Chronic Obstructive Pulmonary Disease Classified by Blood Eosinophil Counts. Lung 198, 925–931 (2020). https://doi.org/10.1007/s00408-020-00397-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-020-00397-4