Abstract
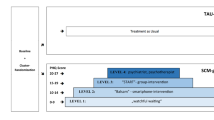
The sudden arrival of culturally diverse asylum seekers and refugees into Germany has created a strong demand for recognizing and appropriately treating those suffering from mental health issues. Due to many systemic, organizational, cultural and socio-linguistic barriers, psychiatric treatment of refugees is posing a major challenge to Germany’s mental health care system. Thus, there is a need for alternative models that allow for increased access to adequate, effective and efficient culturally sensitive mental health care services. Here, we describe the Mental Health in Refugees and Asylum Seekers (MEHIRA) project, a multicentre randomized controlled trial investigating a stepped collaborative care model (SCCM) for providing mental health treatment in this vulnerable population. The proposed SCCM aims to decrease the aforementioned barriers. Adult and adolescent participants will be screened for depressive symptoms and matched to appropriate psychological interventions, including group-level interventions (START intervention, Empowerment/Gender-sensitive/Peer to peer), and other innovative, digital treatment approaches (Smartphone application). The therapeutic effect of the SCCM will be compared to TAU (treatment-as-usual). All interventions have been designed to be culturally sensitive, and offered in two different languages: Arabic and Farsi. The outcome of this study may contribute significantly to future clinical and legal guidelines in developing parallel and efficient new structures of treatment. Collected data will inform primary and secondary mental health care providers with recommendations concerning the design and implementation of effective treatment models and programmes. Guidelines and recommendations may also potentially be adopted by other host countries, developing countries and also in humanitarian aid programmes.



Similar content being viewed by others
References
Ackenheil M, Stotz G, Dietz-Bauer R, Vossen A (1999) Mini international neuropsychiatric interview. German version 5.0.0. Psychiatrische Universitätsklinik München, Munich
Adorjan K, Kluge U, Heinz A, Stamm T, Odenwald M, Dohrmann K et al (2017) Versorgungsmodelle für traumatisierte Flüchtlinge in Deutschland. Der Nervenarzt 88(9):989–994
Asylbewerberleistungsgesetz § 2 (2017) https://www.gesetze-im-internet.de/asylblg/__2.html Accessed 25 Apr 2018.
BAMF (2018) BAMF—Bundesamt für Migration und Flüchtlinge—Asylzahlen. http://www.bamf.de/DE/Infothek/Statistiken/Asylzahlen/asylzahlen-node.html. Accessed 10 Apr 2018
Bajbouj M (2015) Mental health in refugees in Germany. Neuropsychotherapist 21:6–9. http://www.neuropsychotherapist.com/mental-health-in-refugees-in-germany/. Accessed 10 Apr 2018
Bajbouj M, Alabdullah J, Ahmad S, Schidem S, Zellmann H, Schneider F, Heuser I (2018) Psychosoziale Versorgung von Flüchtlingen in Deutschland. Der Nervenarzt 89(1):1–7. https://doi.org/10.1007/s00115-017-0326-y
Bogic M, Njoku A, Priebe S (2015) Long-term mental health of war-refugees: a systematic literature review. BMC Int Health Hum Rights 15(1). https://doi.org/10.1186/s12914-015-0064-9CATS Questionnaire. (2017). Ulmer-onlineklinik.de. https://ulmer-onlineklinik.de/course/view.php?id=1701. Accessed 16 Apr 2018
Bower P, Gilbody S (2005) Stepped care in psychological therapies: access, effectiveness and efficiency: narrative literature review. Br J Psychiatry 186(1):11–17
Campinha-Bacote J (2002) The process of cultural competence in the delivery of healthcare services: a model of care. J Transcult Nurs. 13(3):181–184
Cornelius LJ, Booker NC, Arthur TE, Reeves I, Morgan O (2004) The validity and reliability testing of a consumer base cultural competency inventory. Res Soc Work Pract 14(3):201–209
Dapunt J, Kluge U, Heinz A (2017) Risk of psychosis in refugees: a literature review. Transl Psychiatry 7(6):e1149
Davidson J, Turnbull C, Strickland R, Miller R, Graves K (1986) The Montgomery-Åsberg Depression Scale: reliability and validity. Acta Psychiatr Scand 73(5):544–548. https://doi.org/10.1111/j.1600-0447.1986.tb02723
Devilly G, Borkovec T (2000) Psychometric properties of the credibility/expectancy questionnaire. J Behav Ther Exp Psychiatry 31(2):73–86
Dixius A, Stevens A, Moehler E (2017) A pilot evaluation study of an intercultural treatment program for stabilization and arousal modulation for intensely stressed children and adolescents and minor refugees, called START (Stress-Traumasymptoms-Arousal-Regulation-Treatment. ARC J Psychiatry 2(2):7–14
Giacco D, Laxhman N, Priebe S (2017) Prevalence of risk factors for mental disorders in refugees. Semin Cell Dev Biol 77:144–152. https://doi.org/10.1016/j.semcdb.2017.11.030
Goodman R (1997) The Strengths and Difficulties Questionnaire: a research note. J Child Psychol Psychiatry 38(5):581–586. https://doi.org/10.1111/j.1469-7610.1997.tb01545.x
Griner D, Smith T (2006) Culturally adapted mental health intervention: a meta-analytic review. Psychother Theory, Res Pract Train 43:531–548
Hammoud M, White B, Fetters M (2005) Opening cultural doors: providing culturally sensitive healthcare to Arab American and Muslim Patients. Am J Obstet Gynecol 193:1307–1311
Härter M, Watzke B, Daubmann A, Wegscheider K, König H, Brettschneider C, Liebherz S, Heddaeus D, Steinmann M (2018) Guideline-based stepped and collaborative care for patients with depression in a cluster-randomised trial. Sci Rep 8:9389
Ho FY-Y, Yeung W-F, Ng TH-Y, Chan CS (2016) The efficacy and cost-effectiveness of stepped care prevention and treatment for depressive and/or anxiety disorders: a systematic review and meta-analysis. Sci Rep 6:29281. https://doi.org/10.1038/srep29281
Hollifield M, Verbillis-Kolp S, Farmer B, Toolson E, Woldehaimanot T, Yamazaki J et al (2013) The Refugee Health Screener-15 (RHS-15): development and validation of an instrument for anxiety, depression, and PTSD in refugees. Gen Hosp Psychiatry 35(2):202–209. https://doi.org/10.1016/j.genhosppsych.2012.12.002
Jefee-Bahloul H, Bajbouj M, Alabdullah J, Hassan G, Barkil-Oteo A (2016) Mental health in Europe’s Syrian refugee crisis. Lancet Psychiatry 3(4):315–317. https://doi.org/10.1016/s2215-0366(16)00014-6
Johnson J, Harris E, Spitzer R, Williams J (2002) The patient health questionnaire for adolescents: validation of an instrument for the assessment of mental disorders among adolescent primary care patients. J Adolesc Health 30(3):196–204
Kirmayer LJ (2012) Rethinking cultural competence. Transcult Psychiatry 49(2):149–164. https://doi.org/10.1177/1363461512444673
Kirmayer LJ, Narasiah L, Munoz M, Rashid M, Ryder AG, Guzder J, Hassan G, Rousseau C, Pottie K, Canadian Collaboration for Immigrant and Refugee Health (CCIRH) (2011) Common mental health problems in immigrants and refugees: general approach in primary care. CMAJ 183(12):E959–E967. https://doi.org/10.1503/cmaj.090292
Krenawi A, Graham J (2000) Culturally sensitive social work practice with Arab clients in mental health settings. Health Soc Work 25(1):9–22
Kroenke K, Spitzer R, Williams J (2001) The PHQ-9. J General Internal Med 16(9):606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Lawrence P, Rozmus C (2001) Culturally sensitive care of the muslim patient. J Transcult Nurs 12(33):228–233
Laschet A (2016) Zugang zu Gesundheitsleistungen und Gesundheitsversorgung für Flüchtlinge und Asylbewerber: Von der Erstversorgung bis zur psychosozialen Behandlung(Rep.). Robert Bosch Expertenkommission zur Neuausrichtung der Flüchtlingspolitik. website: http://www.bosch-stiftung.de/content/language1/downloads/RBS_Kommissionsbericht_Fluechtlingspolitik_Gesundheit_ES.pdf. Accessed 11 Sep 2017
Lecrubier Y, Sheehan D, Hergueta T, Weiller E (1998) The mini international neuropsychiatric interview. Eur Psychiatry 13:198. https://doi.org/10.1016/S0924-9338(99)80239-9
Lindert J, Carta M, Schäfer I, Mollica R (2016) Refugees mental health—a public mental health challenge. Eur J Public Health 26(3):374–375. https://doi.org/10.1093/eurpub/ckw010
Lovell K, Lamb J, Gask L, Bower P, Waheed W, Chew-Graham C et al (2014) Development and evaluation of culturally sensitive psychosocial interventions for underserved people in primary care. BMC Psychiatry. https://doi.org/10.1186/s12888-014-0217-8
Missmahl I, Kluge U, Bromand Z, Heinz A (2012) Teaching psychiatry and establishing psychosocial services–lessons from Afghanistan. Eur Psychiatry 27:76–80
Mollica R, Caspi-Yavin Y, Bollini P, Truong T, Tor S, Lavelle J (1992) The Harvard Trauma Questionnaire. J Nerv Mental Dis 180(2):111–116. https://doi.org/10.1097/00005053-199202000-00008
Montgomery S, Åsberg M (1979) A new depression scale designed to be sensitive to change. Br J Psychiatry 134(4):382–389. https://doi.org/10.1192/bjp.134.4.382
Muris P, Meesters C, Van den Berg F (2003) The strengths and difficulties questionnaire (SDQ): further evidence for its reliability and validity in a community sample of dutch children and adolescents. Eur Child Adolesc Psychiatry 12(1):1–8. https://doi.org/10.1007/s00787-003-0298-2
Sachser C, Berliner L, Holt T, Jensen T, Jungbluth N, Risch E et al (2017) International development and psychometric properties of the Child and Adolescent Trauma Screen (CATS). J Affect Disord 210:189–195. https://doi.org/10.1016/j.jad.2016.12.040
Schneider C, Joos S, Bozorgmehr K (2015) Disparities in health and access to healthcare between asylum seekers and residents in Germany: a population-based cross-sectional feasibility study. BMJ 5(11):e008784
Schneider F, Bajbouj M, Heinz A (2017) Psychische Versorgung von Fluchtlingen in Deutschland. Modell fur ein gestuftes Vorgehen. Der Nervenarzt 88(1):10–17. https://doi.org/10.1007/s00115-016-0243-5
Schwarzer R, Jerusalem M (1995) Generalized Self-Efficacy scale. In: Weinman J, Wright S, Johnston M (eds) Measures in health psychology: a user’s portfolio. Causal and control beliefs. NFER-NELSON, Windsor, pp 35–37
Sheehan DV, Lecrubier Y, Sheehan KH, Amorim P, Janavs J, Weiller E, Hergueta T, Baker R, Dunbar GC (1998) The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry 59(20):22–33
Shoeb M, Weinstein H, Mollica R (2007) The harvard trauma questionnaire: adapting a cross-Cultural instrument for measuring torture, trauma and posttraumatic stress disorder in iraqi refugees. Int J Soc Psychiatry 53(5):447–463. https://doi.org/10.1177/0020764007078362
Sijbrandij M, Acarturk C, Bird M, Bryant RA, Burchert S, Carswell K, Cuijpers P (2017) Strengthening mental health care systems for Syrian refugees in Europe and the Middle East: integrating scalable psychological interventions in eight countries. Eur J Psychotraumatol 8(2):1388102
Silove D, Ventevogel P, Rees S (2017) The contemporary research crisis: an overview of mental health challenges. World Psychiatry 16:130–139. https://doi.org/10.1002/wps.20438
Skevington SM, Lotfy M, O’Connell KA, WHOQOL Group (2004) The World Health Organization’s WHOQOL-BREF quality of life assessment: psychometric properties and results of the international field trial. A report from the WHOQOL group. Qual Life Res 13(2):299–310
Smith B, Dalen J, Wiggins K, Tooley E, Christopher P, Bernard J (2008) The brief resilience scale: assessing the ability to bounce back. Int J Behav Med 15(3):194–200. https://doi.org/10.1080/10705500802222972
Stemler S (2004) A comparison of consensus, consistency, and measurement approaches to estimating interrater reliability. Pract Assess Res Evalu 9:1–19
TreatChildTrauma (2016) CATS—Child and Adolescent Trauma Screening. http://treatchildtrauma.de/cats-child-and-adolescent-trauma-screening-free-download/
Ullmann E, Barthel A, Taché S, Bornstein A, Licinio J, Bornstein S (2015) Emotional and psychological trauma in refugees arriving in Germany in 2015. Mol Psychiatry 20(12):1483–1484. https://doi.org/10.1038/mp.2015.164
Watzke B, Heddaeus D, Steinmann M, König HH, Wegscheider K, Schulz H, Härter M (2014) Effectiveness and cost-effectiveness of a guideline-based stepped care model for patients with depression: study protocol of a cluster-randomized controlled trial in routine care. BMC Psychiatry 14:230. https://doi.org/10.1186/s12888-014-0230-y
World Health Organization (2004) Prevention of Mental Disorders: Effective Interventions and Policy Options. Summary Report
World Health Organization (1998) Development of the World Health Organization WHOQOL-BREF quality of life assessment. Psychol Med 28(3):551–558. https://doi.org/10.1017/s0033291798006667
Williams N (2014) PHQ-9. Occup Med 64(2):139–140. https://doi.org/10.1093/occmed/kqt154
Witt A, Rassenhofer M, Fegert J, Plener P (2015) Hilfebedarf und Hilfsangebote in der Versorgung von unbegleiteten minderjährigen Flüchtlingen. Kindheit Entwicklung 24(4):209–224. https://doi.org/10.1026/0942-5403/a000177
Acknowledgements
The authors declared no potential conflicts of interest with respect to the research, authorship or publication of this article.
Funding
The MEHIRA study is funded by the Innovationsfond, Ministry of Health (01VSF16061).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Böge, K., Karnouk, C., Hahn, E. et al. Mental health in refugees and asylum seekers (MEHIRA): study design and methodology of a prospective multicentre randomized controlled trail investigating the effects of a stepped and collaborative care model. Eur Arch Psychiatry Clin Neurosci 270, 95–106 (2020). https://doi.org/10.1007/s00406-019-00991-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00406-019-00991-5