Abstract
Objective
To evaluate the association of short-term variation (STV) and Doppler parameters with adverse perinatal outcome in low-risk fetuses at term.
Methods
This was a retrospective study of 1008 appropriate–for-gestational age (AGA) term fetuses. Doppler measurements [umbilical artery (UA), middle cerebral artery (MCA), and cerebroplacental ratio (CPR)] and computerized CTG (cCTG) with STV analysis were performed prior to active labor (≤ 4 cm cervical dilatation) within 72 h of delivery. The association between Doppler indices and STV values with adverse perinatal outcome was analyzed using univariate regression analysis.
Results
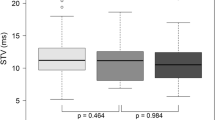
No significant association between Doppler parameters and the need for secondary cesarean delivery (CD) or operative vaginal delivery (OVD) was shown. Regarding fetuses delivered by CD due to fetal distress, regression analyzes revealed significantly higher UA PI MoM. However, the differences in MCA PI MoM and CPR MoM were not statistically significant. Fetuses with the need for emergency CD showed significantly higher UA PI MoM, lower MCA PI MoM and lower CPR MoM. Neonates with a 5-min Apgar score < 7 had significantly lower MCA PI MoM and neonatal acidosis (UA pH ≤ 7.10) showed a significant association with UA PI MoM. None of the assessed outcome parameters were significantly associated to STV.
Conclusion
Doppler indices assessed close to delivery in low-risk fetuses at term show a moderate association with adverse outcome parameters, whereas STV does not appear to predict poor perinatal outcome in this group of fetuses.


Similar content being viewed by others
References
American College of O, Gynecologists (2013) ACOG Practice bulletin no. 134: fetal growth restriction. Obstet Gynecol 121(5):1122–1133. https://doi.org/10.1097/01.AOG.0000429658.85846.f9
Khalil A, Morales-Rosello J, Townsend R, Morlando M, Papageorghiou A, Bhide A, Thilaganathan B (2016) Value of third-trimester cerebroplacental ratio and uterine artery Doppler indices as predictors of stillbirth and perinatal loss. Ultrasound Obstet Gynecol 47(1):74–80. https://doi.org/10.1002/uog.15729
Morales-Rosello J, Khalil A, Morlando M, Papageorghiou A, Bhide A, Thilaganathan B (2014) Changes in fetal Doppler indices as a marker of failure to reach growth potential at term. Ultrasound Obstet Gynecol 43(3):303–310. https://doi.org/10.1002/uog.13319
Morales-Rosello J, Khalil A, Morlando M, Bhide A, Papageorghiou A, Thilaganathan B (2015) Poor neonatal acid-base status in term fetuses with low cerebroplacental ratio. Ultrasound Obstet Gynecol 45(2):156–161. https://doi.org/10.1002/uog.14647
Prior T, Mullins E, Bennett P, Kumar S (2013) Prediction of intrapartum fetal compromise using the cerebroumbilical ratio: a prospective observational study. Am J Obstet Gynecol 208(2):124 e121–124 e126. https://doi.org/10.1016/j.ajog.2012.11.016
Khalil AA, Morales-Rosello J, Morlando M, Hannan H, Bhide A, Papageorghiou A, Thilaganathan B (2015) Is fetal cerebroplacental ratio an independent predictor of intrapartum fetal compromise and neonatal unit admission? Am J Obstet Gynecol 213(1):54 e51–54 e100. https://doi.org/10.1016/j.ajog.2014.10.024
Prior T, Paramasivam G, Bennett P, Kumar S (2015) Are fetuses that fail to achieve their growth potential at increased risk of intrapartum compromise? Ultrasound Obstet Gynecol 46(4):460–464. https://doi.org/10.1002/uog.14758
Devane D, Lalor JG, Daly S, McGuire W, Cuthbert A, Smith V (2017) Cardiotocography versus intermittent auscultation of fetal heart on admission to labour ward for assessment of fetal wellbeing. Cochrane Database Syst Rev 1:CD005122. https://doi.org/10.1002/14651858.CD005122.pub5
Baschat AA, Galan HL, Bhide A, Berg C, Kush ML, Oepkes D, Thilaganathan B, Gembruch U, Harman CR (2006) Doppler and biophysical assessment in growth restricted fetuses: distribution of test results. Ultrasound Obstet Gynecol 27(1):41–47. https://doi.org/10.1002/uog.2657
Galazios G, Tripsianis G, Tsikouras P, Koutlaki N, Liberis V (2010) Fetal distress evaluation using and analyzing the variables of antepartum computerized cardiotocography. Arch Gynecol Obstet 281(2):229–233. https://doi.org/10.1007/s00404-009-1119-8
Anceschi MM, Piazze JJ, Ruozi-Berretta A, Cosmi E, Cerekja A, Maranghi L, Cosmi EV (2003) Validity of short term variation (STV) in detection of fetal acidemia. J Perinat Med 31(3):231–236. https://doi.org/10.1515/JPM.2003.031
Street P, Dawes GS, Moulden M, Redman CW (1991) Short-term variation in abnormal antenatal fetal heart rate records. Am J Obstet Gynecol 165(3):515–523
Lees CC, Marlow N, van Wassenaer-Leemhuis A, Arabin B, Bilardo CM, Brezinka C, Calvert S, Derks JB, Diemert A, Duvekot JJ, Ferrazzi E, Frusca T, Ganzevoort W, Hecher K, Martinelli P, Ostermayer E, Papageorghiou AT, Schlembach D, Schneider KT, Thilaganathan B, Todros T, Valcamonico A, Visser GH, Wolf H, Group Ts (2015) 2 year neurodevelopmental and intermediate perinatal outcomes in infants with very preterm fetal growth restriction (TRUFFLE): a randomised trial. Lancet 385(9983):2162–2172. https://doi.org/10.1016/S0140-6736(14)62049-3
Schiermeier S, Westhof G, Daumer M, Scholz M, Hatzmann W (2006) Short-time variations of fetal heart rate and the FIGO-CTG-Score—first experience with a combination of these two parameters. Geburtsh Frauenheilk 66:752–755. https://doi.org/10.1055/s-2006-924385
Bahlmann F, Reinhard I, Krummenauer F, Neubert S, Macchiella D, Wellek S (2002) Blood flow velocity waveforms of the fetal middle cerebral artery in a normal population: reference values from 18 weeks to 42 weeks of gestation. J Perinat Med 30(6):490–501. https://doi.org/10.1515/JPM.2002.077
Acharya G, Wilsgaard T, Berntsen GK, Maltau JM, Kiserud T (2005) Reference ranges for serial measurements of umbilical artery Doppler indices in the second half of pregnancy. Am J Obstet Gynecol 192(3):937–944. https://doi.org/10.1016/j.ajog.2004.09.019
Baschat AA, Gembruch U (2003) The cerebroplacental Doppler ratio revisited. Ultrasound Obstet Gynecol 21(2):124–127. https://doi.org/10.1002/uog.20
Yudkin PL, Aboualfa M, Eyre JA, Redman CW, Wilkinson AR (1987) New birthweight and head circumference centiles for gestational ages 24 to 42 weeks. Early Hum Dev 15(1):45–52
Mlynarczyk M, Chauhan SP, Baydoun HA, Wilkes CM, Earhart KR, Zhao Y, Goodier C, Chang E, Lee Plenty NM, Mize EK, Owens M, Babbar S, Maulik D, DeFranco E, McKinney D, Abuhamad AZ (2017) The clinical significance of an estimated fetal weight below the 10th percentile: a comparison of outcomes of < 5th vs 5th-9th percentile. Am J Obstet Gynecol. https://doi.org/10.1016/j.ajog.2017.04.020
National Collaborating Centre for Ws, Children’s H (2014) National Institute for Health and Care Excellence: Clinical Guidelines. In: Intrapartum care: care of healthy women and their babies during childbirth. National Institute for Health and Care Excellence (UK) Copyright (c) 2014 National Collaborating Centre for Women’s and Children’s Health, London
Roemer VM, Heger-Römermann G (1993) Der Notfall-Kaiserschnitt—Basisdaten. In: Krebs D, Berg D (eds) Gynäkologie und Geburtshilfe 1992. Springer, Berlin, pp 1545–1547. 10.1007/978-3-642-77857-5_630
Berg D, Ratzel R (2013) Stellungnahme zur Frage der erlaubten Zeit zwischen Indikationsstellung und Sectio (EE-Zeit) bei einer Notlage. Der Gynäkologe 46(2):84–87. https://doi.org/10.1007/s00129-012-3003-z
DGGG (2013) S1-Leitlinie: anwendung des CTG während Schwangerschaft und Geburt. http://www.awmf.org/leitlinien/detail/ll/015-036.html. Accessed 30 June 2017
Genuttis N, Bolz M, Briese V (2017) Can the rate of C-sections performed in a level I perinatal center be reduced?—an analysis of the university gynecology clinic Rostock, 2008–2014. Geburtshilfe und Frauenheilkunde 77(7):771–779. https://doi.org/10.1055/s-0043-112863
Anceschi MM, Ruozi-Berretta A, Piazze JJ, Cosmi E, Cerekja A, Meloni P, Cosmi EV (2004) Computerized cardiotocography in the management of intrauterine growth restriction associated with Doppler velocimetry alterations. Int J Gynaecol Obstet 86(3):365–370. https://doi.org/10.1016/j.ijgo.2004.05.012
Ropacka-Lesiak M, Korbelak T, Swider-Musielak J, Breborowicz G (2015) Cerebroplacental ratio in prediction of adverse perinatal outcome and fetal heart rate disturbances in uncomplicated pregnancy at 40 weeks and beyond. Arch Med Sci 11(1):142–148. https://doi.org/10.5114/aoms.2015.49204
Garcia-Simon R, Figueras F, Savchev S, Fabre E, Gratacos E, Oros D (2015) Cervical condition and fetal cerebral Doppler as determinants of adverse perinatal outcome after labor induction for late-onset small-for-gestational-age fetuses. Ultrasound Obstet Gynecol 46(6):713–717. https://doi.org/10.1002/uog.14807
Cruz-Martinez R, Figueras F, Hernandez-Andrade E, Oros D, Gratacos E (2011) Fetal brain Doppler to predict cesarean delivery for nonreassuring fetal status in term small-for-gestational-age fetuses. Obstet Gynecol 117(3):618–626. https://doi.org/10.1097/AOG.0b013e31820b0884
Flood K, Unterscheider J, Daly S, Geary MP, Kennelly MM, McAuliffe FM, O’Donoghue K, Hunter A, Morrison JJ, Burke G, Dicker P, Tully EC, Malone FD (2014) The role of brain sparing in the prediction of adverse outcomes in intrauterine growth restriction: results of the multicenter PORTO Study. Am J Obstet Gynecol 211(3):288 e281–288 e285. https://doi.org/10.1016/j.ajog.2014.05.008
Makhseed M, Jirous J, Ahmed MA, Viswanathan DL (2000) Middle cerebral artery to umbilical artery resistance index ratio in the prediction of neonatal outcome. Int J Gynaecol Obstet 71(2):119–125
Triunfo S, Crispi F, Gratacos E, Figueras F (2016) Prediction of delivery of small for gestational age neonates and adverse perinatal outcomes by feto-placental Doppler at 37 weeks’ gestation. Ultrasound Obstet Gynecol. https://doi.org/10.1002/uog.15979
Lees C, Marlow N, Arabin B, Bilardo CM, Brezinka C, Derks JB, Duvekot J, Frusca T, Diemert A, Ferrazzi E, Ganzevoort W, Hecher K, Martinelli P, Ostermayer E, Papageorghiou AT, Schlembach D, Schneider KT, Thilaganathan B, Todros T, van Wassenaer-Leemhuis A, Valcamonico A, Visser GH, Wolf H, Group T (2013) Perinatal morbidity and mortality in early-onset fetal growth restriction: cohort outcomes of the trial of randomized umbilical and fetal flow in Europe (TRUFFLE). Ultrasound Obstet Gynecol 42(4):400–408. https://doi.org/10.1002/uog.13190
Guzman ER, Vintzileos AM, Martins M, Benito C, Houlihan C, Hanley M (1996) The efficacy of individual computer heart rate indices in detecting acidemia at birth in growth-restricted fetuses. Obstet Gynecol 87(6):969–974
Dawes GS, Moulden M, Redman CW (1992) Short-term fetal heart rate variation, decelerations, and umbilical flow velocity waveforms before labor. Obstet Gynecol 80(4):673–678
Garcia GS, Mariani Neto C, Araujo Junior E, Garcia RL, Nardozza LM, Moron AF (2008) Fetal acidemia prediction through short-term variation assessed by antepartum computerized cardiotocography in pregnant women with hypertension syndrome. Arch Gynecol Obstet 278(2):125–128. https://doi.org/10.1007/s00404-007-0537-8
Turan S, Turan OM, Berg C, Moyano D, Bhide A, Bower S, Thilaganathan B, Gembruch U, Nicolaides K, Harman C, Baschat AA (2007) Computerized fetal heart rate analysis, Doppler ultrasound and biophysical profile score in the prediction of acid-base status of growth-restricted fetuses. Ultrasound Obstet Gynecol 30(5):750–756. https://doi.org/10.1002/uog.4101
Serra V, Moulden M, Bellver J, Redman CW (2008) The value of the short-term fetal heart rate variation for timing the delivery of growth-retarded fetuses. BJOG 115(9):1101–1107. https://doi.org/10.1111/j.1471-0528.2008.01774.x
Annunziata ML, Tagliaferri S, Esposito FG, Giuliano N, Mereghini F, Di Lieto A, Campanile M (2016) Computerized analysis of fetal heart rate variability signal during the stages of labor. J Obstet Gynaecol Res 42(3):258–265. https://doi.org/10.1111/jog.12908
Schiermeier S, Reinhard J, Hatzmann H, Zimmermann RC, Westhof G (2009) Fetal short time variation during labor: a non-invasive alternative to fetal scalp pH measurements? J Perinat Med 37(5):529–533. https://doi.org/10.1515/JPM.2009.089
Agrawal SK, Doucette F, Gratton R, Richardson B, Gagnon R (2003) Intrapartum computerized fetal heart rate parameters and metabolic acidosis at birth. Obstet Gynecol 102(4):731–738
Amorim-Costa C, Costa-Santos C, Ayres-de-Campos D, Bernardes J (2016) Longitudinal evaluation of computerized cardiotocographic parameters throughout pregnancy in normal fetuses: a prospective cohort study. Acta Obstetricia et Gynecologica Scandinavica 95(10):1143–1152. https://doi.org/10.1111/aogs.12932
Khalil AA, Morales-Rosello J, Elsaddig M, Khan N, Papageorghiou A, Bhide A, Thilaganathan B (2015) The association between fetal Doppler and admission to neonatal unit at term. Am J Obstet Gynecol 213(1):57 e51–57 e57. https://doi.org/10.1016/j.ajog.2014.10.013
Author information
Authors and Affiliations
Contributions
FMS conceptualization, project administration, data collection, and writing original draft. SK conceptualization, writing, review and editing. JP data collection. FB data collection. CMB data collection. ES data collection. MO Schneider: data collection. AM formal analysis. RLS supervision. MS formal analysis. MWB supervision. FF conceptualization, supervision, data collection, writing, review and editing.
Corresponding author
Ethics declarations
Conflict of interest
We have no conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
Stumpfe, F.M., Kehl, S., Pretscher, J. et al. Correlation of short-term variation and Doppler parameters with adverse perinatal outcome in low-risk fetuses at term. Arch Gynecol Obstet 299, 411–420 (2019). https://doi.org/10.1007/s00404-018-4978-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-018-4978-z