Abstract
Introduction
Diagnosing a (low-grade) periprosthetic joint infection (PJI) after hip or knee arthroplasty remains a diagnostic challenge. The aim of this study was to evaluate the utility of using a novel multiplex protein microarray system for synovial biomarkers in determining PJI in patients undergoing revision knee or hip arthroplasty.
Materials and methods
The individual synovial fluid levels of 12 cytokines (IL-1b, IL-2, IL-4, IL-5, IL-6, IL-8, IL-10, IL-12, IL-17, GM-CSF, TNF-α, and INF-γ) were analysed with a novel multiplex protein microarray system in 32 patients undergoing revision hip (n = 22) or knee (n = 10) arthroplasty. Cases were classified into septic and aseptic groups on basis of pre- and interoperative findings: [PJI (n = 14) vs. non-PJI (n = 18)]. Receiver operator characteristic (ROC) curves were calculated to assess the discriminatory strength of the individual parameters. A multiple regression model was used to determine the utility of using a combination of the tested cytokines to determine the infection status.
Results
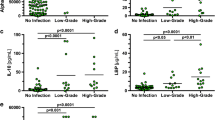
The levels of all of the evaluated cytokines were significantly elevated in the PJI-group. Best sensitivity and specificity were found for IL-6, followed by IL-1b, IL-10, and IL-17. The multiple regression models revealed a combination of IL-2, IL-4, IL-5, IL6, lL-12, and GM-CSF to be associated with the best sensitivity (100%) and specificity (88.9%) for a cut-off value of 0.41, with a likelihood ratio of 9.0.
Conclusion
Analysis of individual synovial fluid cytokine levels showed both high sensitivity and high specificity in diagnosing PJI. A combined model using several cytokines showed even higher sensitivity and specificity in diagnosing PJI and could thus be a useful predictive tool to determine the probability of PJI in patients with a painful prosthesis.
Level of Evidence
Diagnostic IV.



Similar content being viewed by others
References
Wimmer MD, Randau TM, Petersdorf S, Pagenstert GI, Weißkopf M, Wirtz DC, Gravius S (2013) Evaluation of an interdisciplinary therapy algorithm in patients with prosthetic joint infections. Int Orthop 37:2271–2278. https://doi.org/10.1007/s00264-013-1995-1
Deirmengian C, Lonner JH, Booth RE (2005) The Mark Coventry Award: white blood cell gene expression: a new approach toward the study and diagnosis of infection. Clin Orthop 440:38–44
Hischebeth GTR, Randau TM, Molitor E, Wimmer MD, Hoerauf A, Bekeredjian-Ding I, Gravius S (2016) Comparison of bacterial growth in sonication fluid cultures with periprosthetic membranes and with cultures of biopsies for diagnosing periprosthetic joint infection. Diagn Microbiol Infect Dis 84:112–115. https://doi.org/10.1016/j.diagmicrobio.2015.09.007
Alvand A, Rezapoor M, Parvizi J (2017) The role of biomarkers for the diagnosis of implant-related infections in orthopaedics and trauma. In: Drago L (ed) A modern approach to biofilm-related orthopaedic implant infections. Springer, Cham, pp 69–79
Parvizi J, Tan TL, Goswami K, Higuera C, Della Valle C, Chen AF, Shohat N (2018) The 2018 Definition of periprosthetic hip and knee infection: an evidence-based and validated criteria. J Arthroplasty 33:1309–1314.e2. https://doi.org/10.1016/j.arth.2018.02.078
Parvizi J, Gehrke T, Chen AF (2013) Proceedings of the international consensus on periprosthetic joint infection. Bone Jt J 95:1450–1452
Parvizi J, Zmistowski B, Berbari EF, Bauer TW, Springer BD, Della Valle CJ, Garvin KL, Mont MA, Wongworawat MD, Zalavras CG (2011) New definition for periprosthetic joint infection: from the workgroup of the musculoskeletal infection society. Clin Orthop 469:2992–2994. https://doi.org/10.1007/s11999-011-2102-9
Inagaki Y, Uchihara Y, Munemoto M, Scarborough M, Dodd CAF, Gibbons CLMH, Tanaka Y, Athanasou NA (2019) Correlation of histological and microbiological findings in septic and aseptic knee implant failure. Arch Orthop Trauma Surg 139:717–722. https://doi.org/10.1007/s00402-019-03159-x
Balato G, Franceschini V, Ascione T, Lamberti A, Balboni F, Baldini A (2018) Diagnostic accuracy of synovial fluid, blood markers, and microbiological testing in chronic knee prosthetic infections. Arch Orthop Trauma Surg 138:165–171. https://doi.org/10.1007/s00402-017-2832-6
Jämsen E, Huhtala H, Puolakka T, Moilanen T (2009) Risk factors for infection after knee arthroplasty: a register-based analysis of 43,149 cases. J Bone Jt Surg-Am 91:38–47. https://doi.org/10.2106/JBJS.G.01686
Randau TM, Friedrich MJ, Wimmer MD, Reichert B, Kuberra D, Stoffel-Wagner B, Limmer A, Wirtz DC, Gravius S (2014) Interleukin-6 in serum and in synovial fluid enhances the differentiation between periprosthetic joint infection and aseptic loosening. PLoS ONE 9:e89045. https://doi.org/10.1371/journal.pone.0089045
Fröschen FS, Randau TM, Hischebeth GTR, Gravius N, Gravius S, Walter SG (2019) Mid-term results after revision total hip arthroplasty with custom-made acetabular implants in patients with Paprosky III acetabular bone loss. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-019-03318-0
Bingham J, Clarke H, Spangehl M, Schwartz A, Beauchamp C, Goldberg B (2014) The alpha defensin-1 biomarker assay can be used to evaluate the potentially infected total joint arthroplasty. Clin Orthop Relat Res 472:4006–4009. https://doi.org/10.1007/s11999-014-3900-7
Friedrich MJ, Wimmer MD, Schmolders J, Strauss AC, Ploger MM, Kohlhof H, Wirtz DC, Gravius S, Randau TM (2017) RANK-ligand and osteoprotegerin as biomarkers in the differentiation between periprosthetic joint infection and aseptic prosthesis loosening. World J Orthop 8:342. https://doi.org/10.5312/wjo.v8.i4.342
Patel R, Alijanipour P, Parvizi J (2016) Advancements in diagnosing periprosthetic joint infections after total hip and knee arthroplasty. Open Orthop J 10:654–661. https://doi.org/10.2174/1874325001610010654
Shahi A, Parvizi J (2016) The role of biomarkers in the diagnosis of periprosthetic joint infection. EFORT Open Rev 1:275–278. https://doi.org/10.1302/2058-5241.1.160019
Deirmengian C, Kardos K, Kilmartin P, Cameron A, Schiller K, Parvizi J (2014) Diagnosing periprosthetic joint infection: has the era of the biomarker arrived? Clin Orthop Relat Res 472:3254–3262. https://doi.org/10.1007/s11999-014-3543-8
Frangiamore SJ, Saleh A, Grosso MJ, Farias Kovac M, Zhang X, Daly TM, Bauer TW, Derwin KA, Iannotti JP, Ricchetti ET (2017) Neer award 2015: analysis of cytokine profiles in the diagnosis of periprosthetic joint infections of the shoulder. J Shoulder Elbow Surg 26:186–196. https://doi.org/10.1016/j.jse.2016.07.017
Balato G, de Matteo V, Ascione T, Di Donato SL, De Franco C, Smeraglia F, Baldini A, Mariconda M (2019) Laboratory-based versus qualitative assessment of α-defensin in periprosthetic hip and knee infections: a systematic review and meta-analysis. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-019-03232-5
Matsen Ko L, Parvizi J (2016) Diagnosis of periprosthetic infection. Orthop Clin North Am 47:1–9. https://doi.org/10.1016/j.ocl.2015.08.003
Lee YS, Koo K-H, Kim HJ, Tian S, Kim T-Y, Maltenfort MG, Chen AF (2017) Synovial fluid biomarkers for the diagnosis of periprosthetic joint infection: a systematic review and meta-analysis. J Bone Jt Surg 99:2077–2084. https://doi.org/10.2106/JBJS.17.00123
Liu JZ, Saleh A, Klika AK, Barsoum WK, Higuera CA (2014) Serum inflammatory markers for periprosthetic knee infection in obese versus non-obese patients. J Arthroplasty 29:1880–1883. https://doi.org/10.1016/j.arth.2014.07.005
Bottner F, Wegner A, Winkelmann W, Becker K, Erren M, Gotze C (2007) Interleukin-6, procalcitonin and TNF : markers of peri-prosthetic infection following total joint replacement. J Bone Jt Surg 89:94–99. https://doi.org/10.1302/0301-620X.89B1.17485
Ettinger M, Calliess T, Kielstein JT, Sibai J, Brückner T, Lichtinghagen R, Windhagen H, Lukasz A (2015) Circulating biomarkers for discrimination between aseptic joint failure, low-grade infection, and high-grade septic failure. Clin Infect Dis 61:332–341. https://doi.org/10.1093/cid/civ286
Diamond G, Beckloff N, Weinberg A, Kisich K (2009) The roles of antimicrobial peptides in innate host defense. Curr Pharm Des 15:2377–2392. https://doi.org/10.2174/138161209788682325
Renz N, Yermak K, Perka C, Trampuz A (2018) Alpha defensin lateral flow test for diagnosis of periprosthetic joint infection: not a screening but a confirmatory test. J Bone Jt Surg 100:742–750. https://doi.org/10.2106/JBJS.17.01005
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest. No benefits have been or will be received from a commercial party related directly or indirectly to the subject matter of this article.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. For this type of study formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fröschen, F.S., Schell, S., Schildberg, F.A. et al. Analysis of synovial biomarkers with a multiplex protein microarray in patients with PJI undergoing revision arthroplasty of the hip or knee joint. Arch Orthop Trauma Surg 140, 1883–1890 (2020). https://doi.org/10.1007/s00402-020-03388-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03388-5