Abstract
Introduction: With the resurge of tuberculosis, due to the pandemic of the human immunodeficiency virus and the increase in the number of immunocompromised patients, osteoarticular tuberculosis has increased too. Materials and methods: We report of a 55-year-old patient, with chronic renal failure on haemodialysis, who presented with a painful knee and fever. Culture on Lowënstein–Jensen medium of joint liquid revealed a tuberculous affectation of the proximal tibia. Wide excision was performed, completed with 9 months of tuberculostatic drugs. At 1 year follow-up, the patient was free of symptoms. Conclusion: Tuberculous aetiology should be considered in the differential diagnosis of knee arthritis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tuberculosis cases have increased in the past few years due to acquired immunodeficiency syndrome (AIDS) and immigration of people from endemic zones, affecting one-third of the world’s population. After ganglion and kidney affection, osteoarticular tuberculosis is the third form of extrapulmonary tuberculosis. With the reemergence of tuberculosis, more atypical osteoarticular cases are seen. Staphylococcus aureus is usually responsible for osteomyelitis in patients with chronic renal failure. A high grade of suspicion is necessary to diagnose tuberculosis aetiology in a patient affected with chronic monoarthritis with risk factors that present an insidious evolution.
Case report
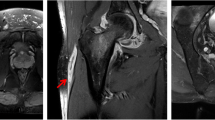
We report the case of a 55-year-old man who presented with a 15-day history of fever (39°C) and a painful and effused knee, without traumatism. The patient had a history of schizophrenia, high blood pressure, diabetes mellitus, and chronic renal failure secondary to diabetic nephropathy. Physical examination showed a heat and effused knee. Blood test revealed 12.1×109 l−1 leukocytes (82.5 neutrophils, 9.5 lymphocytes), erythrocyte sedimentation rate (ESR) of 121 mm/h, and C-reactive protein (CRP) of 11.8 mg/dl. Radiographs of the knee were considered normal (Figs. 1, 2). Knee puncture was performed and joint liquid showed 9,600 cells (95% neutrophils), 44 g/l proteins and 93 mg/dl glucose. Ziehl-Nielsen and Gram stains were negative. We started intravenous antibiotic treatment with vancomycin, but after 15 days of therapy, the patient remained febrile and the inflammatory signs persisted. A bone scan with technetium 99m-labelled leukocytes showed an important uptake by the external tibial plateau area (Fig. 3). A CT scan revealed a cortical lytic lesion on the external margin of the tibial plateau, with an important soft tissue component. MRI was performed and demonstrated an extent soft tissue lesion (5×5 cm2) on the external aspect of the knee, extending and destructing the external tibial plateau (Figs. 4, 5). The differential diagnosis involved a tibial osteomyelitis or a malignant tumoral lesion (chondrosarcoma, bone lymphoma or giant cell tumour). Wide excision and curettage of the bone were performed, by means of a lateral approach, testing the cartilage integrity, and bone defect was filled with cement. Histological examination showed a chronic inflammatory process, with caseous granulomas, microabscesses and Langhans cells. Ziehl-Nielsen and Gram stains were again negative but Löwenstein culture was positive for Mycobacterium tuberculosis. The patient completed treatment with rifampicin, isoniazid, ethambutol and pyrazinamide for 2 months followed by rifampicin and isoniazid for 7 months. One year later, the patient was asymptomatic, and the range of movement of the knee was normal.
Discussion
An increased incidence of patients with osteoarticular tuberculosis has been observed due to human immunodeficiency virus infection, immigration from endemic areas, alcoholism, chronic kidney disorders, immunosuppressive therapy, drug addiction, intraarticular steroid injection and systemic illness [11, 16]. Extrapulmonary tuberculosis represents at least 10% of all infections by M. tuberculosis, spinal tuberculosis being the most common form of osteoarticular tuberculosis, followed by hip and knee [7, 12]. Osteoarticular tuberculosis is caused by haematogenous, lymphatic or direct local spread of tubercle bacilli from other lesions from a quiescent pulmonary primary or other extraosseous focus, although direct inoculation has been already reported [2, 14]. Tuberculosis is usually a monoarticular disease, being most of the cases of monoarticular arthritis tuberculous [4, 9, 13]. There are few cases of tuberculous osteitis without joint damage [1, 3, 5, 15]. Knee tuberculosis presents usually as a chronic pain, local tenderness and progressive loss of function that could be intermittent and may delay the diagnosis [8, 10]. In approximately 50% of the patients, no radiographic evidence of pulmonary involvement can be identified and a negative tuberculin skin test does not exclude the diagnosis, as in immunocompromised patients (i.e. patients with chronic renal failure) who had a high rate of anergy. In the early stages, radiological findings are nonspecific. The typical radiographic findings are periarticular osteoporosis, peripherally located osseous erosions and gradual narrowing of the cartilage space, and they appear later on. In order to evaluate soft tissue affection, MRI is the best complementary method. Bone scans with technetium 99m are useful in identifying osteomyelitis foci. To achieve a definitive diagnosis, it is essential to identify M. tuberculosis; however, bone and joint tuberculosis are paucibacillar and many a time Ziehl-Nielsen stain is negative and it becomes necessary to wait for Löwenstein culture. Examination of a biopsy specimen is an important and useful diagnostic method, and a biopsy should be performed in every case of osteoarthritis, in order to know which pathogen is responsible. Probably, amplifying DNA of M. tuberculosis from synovial fluid or bone by polymerase chain reaction could be a useful tool for the early diagnosis of tuberculosis. In conclusion, tuberculosis should be considered in immunosupressed patients with osteoarthritis, particularly if they do not respond to antibiotics. The 9 months of treatment was associated with a good clinical and functional result.
Conflict of interest
No benefits in any form have been received or will be received from any commercial party related directly or indirectly to the subject of this article.
References
Aalto K, Osterman K, Peltola H, Rasanen J (1984) Changes in erythrocyte sedimentation rate and C-reactive protein after total hip arthoplasty. Clin Orthop 184:118–120
Chen WS, Wang CJ, Eng HL (1997) Tuberculous arthritis of the elbow. Int Orthop 21:367–370
Combalía A, Sastre S, Esteban P (2004) Tuberculous osteomyelitis of the knee. Arch Orthop Trauma Surg 124:708–710
Domingo A, Nomdedeu M, Tomás X, García S (2005) Elbow tuberculosis: an unusual location and diagnostic problem. Arch Orthop Trauma Surg 125:56–58
Galois L, Chary-Valckenaere I, Mainard D, Pourel J, Delagoutte JP (2003) Tuberculosis of the patella. Arch Orthop Trauma Surg 123:192–194
García S, Segur JM, Combalía A (1994) Tuberculosis of the ischium. Acta Orthop Belg 60:238–240
García S, Combalía A, Serra A, Segur JM, Ramón R (1997) Unusual locations of osteoarticular tuberculosis. Arch Orthop Trauma Surg 116:321–323
Hoffman EB, Allin J, Campbell JA, Leisegang FM (2002) Tuberculosis of the knee. Clin Orthop 398:100–106
Hunfeld KP, Rittmeister M, Wichelhaus TA, Brade V, Enzensberger R (1998) Two cases of chronic arthritis of the forearm due to Mycobacterium tuberculosis. Eur J Microbiol Infect Dis 17:344–348
Kerri O, Martini M (1985) Tuberculosis of the knee. Int Orthop 9:153–157
Khan K, Muenning P, Bheta M, Zivin JG (2002) Global drug-resistance patterns and management of latent tuberculosis infection in immigrants to the United States. N Engl J Med 347:1850–1859
Martini M (1988) Tuberculosis of the knee. In: Martini M (ed) Tuberculosis of the bones and joints, 2nd edn. Springer, Berlin Heidelberg New York, pp 125–138
Martini M, Ouahes M (1988) Bone and joint tuberculosis: a review of 652 cases. Orthopedics 11:861–866
Muraladi D, Gold WL, Vellend H, Becker E (1993) Multifactorial osteoarticular tuberculosis: report of four cases and review of management. Clin Infect Dis 17:204–209
Sastre S, García S, Soriano A (2003) Reactivation of ancient trochanteric tuberculosis sixty years after surgical drainage. Rheumatology 42:1263–1264
Vallés X, Sánchez F, Pañella H, García de Olalla P, Jansá JM, Caylà JA (2002) Tuberculosis importada: una enfermedad emergente en países industrializados. Med Clín (Barc) 118:376–378
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Esteban, P.L., Soriano, A., Tomás, X. et al. Tuberculous osteomyelitis of the knee: a case report. Arch Orthop Trauma Surg 126, 631–633 (2006). https://doi.org/10.1007/s00402-005-0087-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-005-0087-0