Abstract
Background
Controlling nutritional status (CONUT) score, calculated from serum albumin and total cholesterol concentrations and total lymphocyte count, is reportedly valuable for nutritional assessment. This study investigated whether CONUT score was predictive of outcomes in colorectal cancer (CRC) patients undergoing surgical resection.
Methods
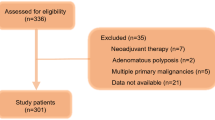
Preoperative CONUT scores were retrospectively evaluated in 417 CRC patients who underwent potentially curative resection at Kumamoto University Hospital from March 2005 to August 2014. Patients were divided into four groups based on preoperative CONUT scores: normal, light, moderate, and severe. The associations of CONUT score with clinicopathological factors, patient survival, and postoperative complications were examined.
Results
CONUT score correlated significantly with age (P < 0.001), body mass index (P = 0.005), carcinoembryonic antigen (P = 0.002), and carbohydrate antigen 19-9 (P = 0.005) concentrations. Overall survival (OS) rate was significantly lower in patients with moderate/severe than light or normal CONUT scores. CONUT score was independently prognostic of OS [moderate/severe vs. normal, hazard ratio = 5.92, 95 % confidence interval (CI) 2.30–14.92; P < 0.001)]. Patients with moderate/severe CONUT scores were at greater risk for complications, especially for severe complications. Multivariate analysis showed that CONUT score was independently predictive of severe complications (moderate/severe vs. normal, odds ratio = 4.51, 95 % CI 1.89–10.74; P < 0.001).
Conclusions
CONUT score may predict survival and postoperative severe complications in CRC patients undergoing potentially curative resection. Management of CRC patients may need consideration of host nutritional status.


Similar content being viewed by others
References
Bistrian BR, Blackburn GL, Vitale J, Cochran D, Naylor J (1976) Prevalence of malnutrition in general medical patients. JAMA 235:1567–1570
Gupta D, Lammersfeld CA, Vashi PG, Burrows J, Lis CG, Grutsch JF (2005) Prognostic significance of subjective global assessment (SGA) in advanced colorectal cancer. Eur J Clin Nutr 59:35–40
Mohri Y, Inoue Y, Tanaka K, Hiro J, Uchida K, Kusunoki M (2013) Prognostic nutritional index predicts postoperative outcome in colorectal cancer. World J Surg 37:2688–2692
Park JH, Watt DG, Roxburgh CS, Horgan PG, McMillan DC (2015) Colorectal cancer, systemic inflammation, and outcome: staging the tumor and staging the host. Ann Surg 263(2):326–336
Ignacio de Ulibarri J, Gonzalez-Madrono A, de Villar NG, Gonzalez P, Gonzalez B, Mancha A, Rodriguez F, Fernandez G (2005) CONUT: a tool for controlling nutritional status. First validation in a hospital population. Nutr Hosp 20:38–45
The Japanese Society for Cancer of the Colon and Rectum. JSCCR Guidelines 2005 for the treatment of colorectal cancer. Tokyo: Kanehara & Co, Ltd.
The Japanese Society for Cancer of the Colon and Rectum. JSCCR Guidelines 2010 for the treatment of colorectal cancer. Tokyo: Kanehara & Co, Ltd
Watanabe T, Itabashi M, Shimada Y, Tanaka S, Ito Y, Ajioka Y, Hamaguchi T, Hyodo I, Igarashi M, Ishida H, Ishiguro M, Kanemitsu Y et al (2012) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2010 for the treatment of colorectal cancer. Int J Clin Oncol 17:1–29
Sobin LH, Gospodarowitz MK, Wittekind CH (2009) TNM classification of malignant tumours. 7th ed. Wiley-Blackwell, New York
Cabre M, Ferreiro C, Arus M, Roca M, Palomera E, Serra-Prat M (2015) Evaluation of CONUT for clinical malnutrition detection and short-term prognostic assessment in hospitalized elderly people. J Nutr Health Aging 19:729–733
Tarantino I, Warschkow R, Worni M, Merati-Kashani K, Koberle D, Schmied BM, Muller SA, Steffen T, Cerny T, Guller U (2012) Elevated preoperative CEA is associated with worse survival in stage I-III rectal cancer patients. Br J Cancer 107:266–274
Stiksma J, Grootendorst DC, van der Linden PW (2014) CA 19-9 as a marker in addition to CEA to monitor colorectal cancer. Clin Colorectal Cancer 13:239–244
Fukushima K, Ueno Y, Kawagishi N, Kondo Y, Inoue J, Kakazu E, Ninomiya M, Wakui Y, Saito N, Satomi S, Shimosegawa T (2014) The nutritional index ‘CONUT’ is useful for predicting long-term prognosis of patients with end-stage liver diseases. Tohoku J Exp Med 224:215–219
Elinav E, Nowarski R, Thaiss CA, Hu B, Jin C, Flavell RA (2013) Inflammation-induced cancer: crosstalk between tumours, immune cells and microorganisms. Nat Rev Cancer 13:759–771
Renfro LA, Loupakis F, Adams RA, Seymour MT, Schmoll HJ, Douillard JY, Hurwitz H, Fuchs CS, Diaz-Rubio E, Porschen R, Tournigand C, Chibaudel B et al (2015) Body mass index is prognostic in metastatic colorectal cancer: pooled analysis of patients from first-line clinical trials in the ARCAD database. J Clin Oncol 34(2):144–150
Moon HG, YT J, Jeong CY, Jung EJ, Lee YJ, Hong SC, Ha WS, Park ST, Choi SK (2008) Visceral obesity may affect oncologic outcome in patients with colorectal cancer. Ann Surg Oncol 15:1918–1922
Miyamoto Y, Baba Y, Sakamoto Y, Ohuchi M, Tokunaga R, Kurashige J, Hiyoshi Y, Iwagami S, Yoshida N, Watanabe M, Baba H (2015) Negative impact of skeletal muscle loss after systemic chemotherapy in patients with unresectable colorectal cancer. PLoS One 10 e0129742
Toyokawa TKN, Shibutani M, Sakurai K, Nagahara H, Tanaka H, Muguruma K, Ohtani H, Yashiro M, Maeda K, Ohira M, Hirakawa K (2015) The pretreatment controlling nutritional status (CONUT) score as an independent prognostic factor in patients with clinical stage I-III esophageal squamous cell carcinoma. Ann Oncol 26(Supplement 4):iv1–iv100
Iseki Y, Shibutani M, Maeda K, Nagahara H, Ohtani H, Sugano K, Ikeya T, Muguruma K, Tanaka H, Toyokawa T, Sakurai K, Hirakawa K (2015) Impact of the preoperative controlling nutritional status (CONUT) score on the survival after curative surgery for colorectal cancer. PLoS One 10 e0132488
Cengiz O, Kocer B, Surmeli S, Santicky MJ, Soran A (2006) Are pretreatment serum albumin and cholesterol levels prognostic tools in patients with colorectal carcinoma? Med Sci Monit 12:CR240–CR247
Peters SJ, Vanhaecke T, Papeleu P, Rogiers V, Haagsman HP, van Norren K (2010) Co-culture of primary rat hepatocytes with rat liver epithelial cells enhances interleukin-6-induced acute-phase protein response. Cell Tissue Res 340:451–457
Honda H, Qureshi AR, Heimburger O, Barany P, Wang K, Pecoits-Filho R, Stenvinkel P, Lindholm B (2006) Serum albumin, C-reactive protein, interleukin 6, and fetuin a as predictors of malnutrition, cardiovascular disease, and mortality in patients with ESRD. Am J Kidney Dis 47:139–148
Sonoda A, Ohnishi S, Nakao S, Iwashita Y, Hashimoto N, Ishida K, Kondo Y, Ishitsuka Y, Irie T (2015) Factors affecting serum albumin in the perioperative period of colorectal surgery: a retrospective study. BMC Res Notes 8:638
Domenicali M, Baldassarre M, Giannone FA, Naldi M, Mastroroberto M, Biselli M, Laggetta M, Patrono D, Bertucci C, Bernardi M, Caraceni P (2014) Posttranscriptional changes of serum albumin: clinical and prognostic significance in hospitalized patients with cirrhosis. Hepatology 60:1851–1860
Okuyama H, Ichikawa Y, Sun Y, Hamazaki T, Lands WE (2007) Cancer and all-cause mortalities are lower in the higher total cholesterol groups among general populations. World Rev Nutr Diet 96:37–54
Kreger BE, Anderson KM, Schatzkin A, Splansky GL (1992) Serum cholesterol level, body mass index, and the risk of colon cancer. The Framingham study. Cancer 70:1038–1043
de Martino M, Leitner CV, Seemann C, Hofbauer SL, Lucca I, Haitel A, Shariat SF, Klatte T (2015) Preoperative serum cholesterol is an independent prognostic factor for patients with renal cell carcinoma (RCC). BJU Int 115:397–404
Niendorf A, Nagele H, Gerding D, Meyer-Pannwitt U, Gebhardt A (1995) Increased LDL receptor mRNA expression in colon cancer is correlated with a rise in plasma cholesterol levels after curative surgery. Int J Cancer 61:461–464
Cardwell CR, Hicks BM, Hughes C, Murray LJ (2014) Statin use after colorectal cancer diagnosis and survival: a population-based cohort study. J Clin Oncol 32:3177–3183
Nielsen SF, Nordestgaard BG, Bojesen SE (2012) Statin use and reduced cancer-related mortality. N Engl J Med 367:1792–1802
Liang L, Zhu J, Jia H, Huang L, Li D, Li Q, Li X (2016) Predictive value of pretreatment lymphocyte count in stage II colorectal cancer and in high-risk patients treated with adjuvant chemotherapy. Oncotarget 7(1):1014–1028
Network CGA (2012) Comprehensive molecular characterization of human colon and rectal cancer. Nature 487:330–337
Moyes LH, Leitch EF, McKee RF, Anderson JH, Horgan PG, McMillan DC (2009) Preoperative systemic inflammation predicts postoperative infectious complications in patients undergoing curative resection for colorectal cancer. Br J Cancer 100:1236–1239
Andreyev HJ, Norman AR, Oates J, Cunningham D (1998) Why do patients with weight loss have a worse outcome when undergoing chemotherapy for gastrointestinal malignancies? Eur J Cancer 34:503–509
Fearon KC, Voss AC, Hustead DS (2006) Definition of cancer cachexia: effect of weight loss, reduced food intake, and systemic inflammation on functional status and prognosis. Am J Clin Nutr 83:1345–1350
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Use of the clinical data was approved by the human ethics review committee of the graduate school of medicine, Kumamoto University.
Conflict of interest
The authors declare that they have no conflict of interest.
Source of funding
No financial support was received for this study.
Additional information
Presentation
We have not presented this study anywhere.
Electronic supplementary material
Supplementary Figure 1
(PPTX 2719 kb)
Supplementary Table 1
(DOCX 24 kb)
Supplementary Table 2
(DOCX 21 kb)
Rights and permissions
About this article
Cite this article
Tokunaga, R., Sakamoto, Y., Nakagawa, S. et al. CONUT: a novel independent predictive score for colorectal cancer patients undergoing potentially curative resection. Int J Colorectal Dis 32, 99–106 (2017). https://doi.org/10.1007/s00384-016-2668-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-016-2668-5