Abstract
Introduction
Decompressive craniectomy (DC) is a lifesaving procedure but is associated to several post-operative complications, namely cerebrospinal fluid (CSF) dynamics impairment. The aim of this multicentric study was to evaluate the incidence of such CSF alterations after DC and review their impact on the overall outcome.
Material and methods
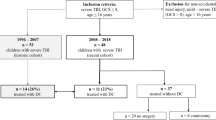
We performed a retrospective multicentric study to analyze the CSF disorders occurring in children aged from 0 to 17 years who had undergone a DC for traumatic brain injury (TBI) in the major Departments of Pediatric Neurosurgery of France between January 2006 and August 2016.
Results
Out of 150 children, ranging in age between 7 months and 17 years, mean 10.75 years, who underwent a DC for TBI in 10 French pediatric neurosurgical centers. Sixteen (6 males, 10 females) (10.67%) developed CSF disorders following the surgical procedure and required an extrathecal CSF shunting. External ventricular drainage increased the risk of further complications, especially cranioplasty infection (p = 0.008).
Conclusion
CSF disorders affect a minority of children after DC for TBI. They may develop early after the DC but they may develop several months after the cranioplasty (8 months), consequently indicating the necessity of clinical and radiological close follow-up after discharge from the neurosurgical unit. External ventricular drainage and permanent CSF shunt placement increase significantly the risk of cranioplasty infection.

Similar content being viewed by others
References
Yang X-J, Hong G-L, Su S-B, Yang S-Y (2003) Complications induced by decompressive craniectomies after traumatic brain injury. Chin J Traumatol Zhonghua Chuang Shang Za Zhi 6(2):99–103
Yang XF, Wen L, Shen F, Li G, Lou R, Liu WG et al (2008) Surgical complications secondary to decompressive craniectomy in patients with a head injury: a series of 108 consecutive cases. Acta Neurochir 150(12):1241–1247 discussion 1248
Gudeman SK, Kishore PR, Becker DP, Lipper MH, Girevendulis AK, Jeffries BF et al (1981) Computed tomography in the evaluation of incidence and significance of post-traumatic hydrocephalus. Radiology 141(2):397–402
Cardoso ER, Galbraith S (1985) Posttraumatic hydrocephalus—a retrospective review. Surg Neurol 23(3):261–264
Hawkins TD, Lloyd AD, Fletcher GI, Hanka R (1976) Ventricular size following head injury: a clinico-radiological study. Clin Radiol 27(3):279–289
LeMay M, Hochberg FH (1979) Ventricular differences between hydrostatic hydrocephalus and hydrocephalus ex vacuo by computed tomography. Neuroradiology 17(4):191–195
Marmarou A, Foda MA, Bandoh K, Yoshihara M, Yamamoto T, Tsuji O et al (1996) Posttraumatic ventriculomegaly: hydrocephalus or atrophy? A new approach for diagnosis using CSF dynamics. J Neurosurg 85(6):1026–1035
Dujovny M, Aviles A, Agner C, Fernandez P, Charbel FT (1997) Cranioplasty: cosmetic or therapeutic? Surg Neurol 47(3):238–241
Segal DH, Oppenheim JS, Murovic JA (1994) Neurological recovery after cranioplasty. Neurosurgery 34(4):729–731 discussion 731
Dujovny M, Agner C, Aviles A (1999) Syndrome of the trephined: theory and facts. Crit Rev Neurosurg 9(5):271–278
Dujovny M, Fernandez P, Alperin N, Betz W, Misra M, Mafee M (1997) Post-cranioplasty cerebrospinal fluid hydrodynamic changes: magnetic resonance imaging quantitative analysis. Neurol Res 19(3):311–316
Fodstad H, Ekstedt J, Fridén H (1979) CSF hydrodynamic studies before and after cranioplasty. Acta Neurochir Suppl (Wien) 28(2):514–518
Fodstad H, Love JA, Ekstedt J, Fridén H, Liliequist B (1984) Effect of cranioplasty on cerebrospinal fluid hydrodynamics in patients with the syndrome of the trephined. Acta Neurochir 70(1–2):21–30
Gooch MR, Gin GE, Kenning TJ, German JW (2009) Complications of cranioplasty following decompressive craniectomy: analysis of 62 cases. Neurosurg Focus 26(6):E9
Heo J, Park SQ, Cho SJ, Chang JC, Park H-K (2014) Evaluation of simultaneous cranioplasty and ventriculoperitoneal shunt procedures. J Neurosurg 121(2):313–318
Chang V, Hartzfeld P, Langlois M, Mahmood A, Seyfried D (2010) Outcomes of cranial repair after craniectomy. J Neurosurg 112(5):1120–1124
Frassanito P, Massimi L, Caldarelli M, Tamburrini G, Di Rocco C (2012) Complications of delayed cranial repair after decompressive craniectomy in children less than 1 year old. Acta Neurochir 154(5):927–933
Josan VA, Sgouros S, Walsh AR, Dover MS, Nishikawa H, Hockley AD (2005) Cranioplasty in children. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 21(3):200–204
Schuss P, Vatter H, Marquardt G, Imöhl L, Ulrich CT, Seifert V et al (2012) Cranioplasty after decompressive craniectomy: the effect of timing on postoperative complications. J Neurotrauma 29(6):1090–1095
Denes Z, Barsi P, Szel I, Boros E, Fazekas G (2011) Complication during postacute rehabilitation: patients with posttraumatic hydrocephalus. Int J Rehabil Res Int Z Rehabil Rev Int Rech Readapt 34(3):222–226
Poca MA, Sahuquillo J, Mataró M, Benejam B, Arikan F, Báguena M (2005) Ventricular enlargement after moderate or severe head injury: a frequent and neglected problem. J Neurotrauma 22(11):1303–1310
De Bonis P, Pompucci A, Mangiola A, Rigante L, Anile C (2010) Post-traumatic hydrocephalus after decompressive craniectomy: an underestimated risk factor. J Neurotrauma 27(11):1965–1970
Honeybul S, Ho KM (2014) Decompressive craniectomy for severe traumatic brain injury: the relationship between surgical complications and the prediction of an unfavourable outcome. Injury 45(9):1332–1339
Takeuchi S, Nagatani K, Wada K, Nawashiro H, Otani N, Osada H et al (2013) Is decompressive craniectomy a risk factor for ventriculomegaly? Acta Neurochir Suppl 118:281–283
Takeuchi S, Takasato Y, Masaoka H, Hayakawa T, Yatsushige H, Nagatani K et al (2013) Hydrocephalus after decompressive craniectomy for hemispheric cerebral infarction. J Clin Neurosci Off J Neurosurg Soc Australas 20(3):377–382
Jiao Q, Liu Z, Li S, Zhou L, Li S, Tian W et al (2007) Influencing factors for posttraumatic hydrocephalus in patients suffering from severe traumatic brain injuries. Chin J Traumatol Zhonghua Chuang Shang Za Zhi 10(3):159–162
Choi I, Park H-K, Chang J-C, Cho S-J, Choi S-K, Byun B-J (2008) Clinical factors for the development of posttraumatic hydrocephalus after decompressive craniectomy. J Korean Neurosurg Soc 43(5):227–231
Tian H-L, Xu T, Hu J, Cui Y, Chen H, Zhou L-F (2008) Risk factors related to hydrocephalus after traumatic subarachnoid hemorrhage. Surg Neurol 69(3):241–246 discussion 246
Kaen A, Jimenez-Roldan L, Alday R, Gomez PA, Lagares A, Alén JF et al (2010) Interhemispheric hygroma after decompressive craniectomy: does it predict posttraumatic hydrocephalus? J Neurosurg 113(6):1287–1293
Low CYD, Low YYS, Lee KK, Chan SP, Ang BT (2013) Post-traumatic hydrocephalus after ventricular shunt placement in a Singaporean neurosurgical unit. J Clin Neurosci Off J Neurosurg Soc Australas 20(6):867–872
Waziri A, Fusco D, Mayer SA, McKhann GM, Connolly ES (2007) Postoperative hydrocephalus in patients undergoing decompressive hemicraniectomy for ischemic or hemorrhagic stroke. Neurosurgery 61(3):489–493 discussion 493-494
Anile C, De Bonis P, Di Chirico A, Ficola A, Mangiola A, Petrella G (2009) Cerebral blood flow autoregulation during intracranial hypertension: a simple, purely hydraulic mechanism? Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 25(3):325–335 discussion 337-340
Lee M-H, Yang J-T, Weng H-H, Cheng Y-K, Lin MH-C, Su C-H et al (2012) Hydrocephalus following decompressive craniectomy for malignant middle cerebral artery infarction. Clin Neurol Neurosurg 114(6):555–559
Hakim S, Adams RD (1965) The special clinical problem of symptomatic hydrocephalus with normal cerebrospinal fluid pressure. Observations on cerebrospinal fluid hydrodynamics. J Neurol Sci 2(4):307–327
Malcolm JG, Rindler RS, Chu JK, Grossberg JA, Pradilla G, Ahmad FU (2016) Complications following cranioplasty and relationship to timing: a systematic review and meta-analysis. J Clin Neurosci Off J Neurosurg Soc Australas 33:39–51
Adamo MA, Drazin D, Waldman JB (2009) Decompressive craniectomy and postoperative complication management in infants and toddlers with severe traumatic brain injuries. J Neurosurg Pediatr 3(4):334–339
Brommeland T, Rydning PN, Pripp AH, Helseth E (2015) Cranioplasty complications and risk factors associated with bone flap resorption. Scand J Trauma Resusc Emerg Med 23:75
Archavlis E, Carvi Y, Nievas M (2012) The impact of timing of cranioplasty in patients with large cranial defects after decompressive hemicraniectomy. Acta Neurochir 154(6):1055–1062
Klinger DR, Madden C, Beshay J, White J, Gambrell K, Rickert K (2014) Autologous and acrylic cranioplasty: a review of 10 years and 258 cases. World Neurosurg 82(3–4):e525–e530
Moreira-Gonzalez A, Jackson IT, Miyawaki T, Barakat K, DiNick V (2003) Clinical outcome in cranioplasty: critical review in long-term follow-up. J Craniofac Surg 14(2):144–153
Schoekler B, Trummer M (2014) Prediction parameters of bone flap resorption following cranioplasty with autologous bone. Clin Neurol Neurosurg 120:64–67
Rocque BG, Amancherla K, Lew SM, Lam S (2013) Outcomes of cranioplasty following decompressive craniectomy in the pediatric population. J Neurosurg Pediatr 12(2):120–125
Grant GA, Jolley M, Ellenbogen RG, Roberts TS, Gruss JR, Loeser JD (2004) Failure of autologous bone-assisted cranioplasty following decompressive craniectomy in children and adolescents. J Neurosurg 100(2 Suppl Pediatrics):163–168
Mustroph CM, Malcolm JG, Rindler RS, Chu JK, Grossberg JA, Pradilla G et al. (2017) Cranioplasty infection and resorption are associated with presence of a ventriculoperitoneal shunt: a systematic review and meta-analysis. World Neurosurg 18
Acknowledgments
The overall series is based on the data obtained from French Pediatric Neurosurgery Departments of Bordeaux, Grenoble, Lille, Lyon, Marseille, Montpellier, Nancy, Nice, Paris, and Toulouse. We thank Dr. Guesmi for her “radiological” support and all the secretaries of the several centers for their help in retrieving the files.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Rights and permissions
About this article
Cite this article
Manfiotto, M., Mottolese, C., Szathmari, A. et al. Decompressive craniectomy and CSF disorders in children. Childs Nerv Syst 33, 1751–1757 (2017). https://doi.org/10.1007/s00381-017-3542-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-017-3542-7