Abstract
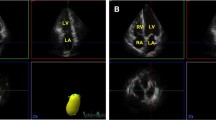
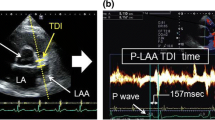
P-wave signal-averaged electrocardiography (P-SAECG) can detect imperceptible conduction abnormalities, and volume analysis using two-dimensional speckle-tracking echocardiography (2-DSTE) allows us to easily measure the phasic function of the left atrium (LA). Both conduction abnormalities and functional deformation of the LA may be linked to the clinical outcome; however, the exact relationship is unclear. The aim of this study was to investigate the relationship between the phasic function of the LA and electrical conduction using P-SAECG and 2-DSTE. The subjects were 112 male volunteers (age 46.9 ± 13.2 years) with normal cardiac function who underwent P-SAECG and 2-DSTE. The filtered p-wave duration (FPD) and the root-mean-square voltage for the last 20 ms (RMS20) on P-SAECG wave were measured in ms and μV, respectively. Total emptying function (EF) (reservoir function), passive EF (conduit function), and active EF (booster pump function) of the LA were calculated as percentages to evaluate phasic LA function using 2DSTE. The mean FPD was 134.3 ± 11.7 ms and the mean RMS20 was 4.59 ± 2.39 μV. The mean total EF was 60.5 ± 13.1%, mean passive EF was 39.4 ± 13.9%, and mean active EF was 35.1 ± 13.9%. FPD had a negative correlation with passive EF (r = − 0.20, p = 0.039). FPD showed no significant relationship with total EF (r = − 0.03, p = 0.78) or active EF (r = 0.13, p = 0.18). There was a significant association between RMS20 and passive EF (r = 0.19, p = 0.048); however, no there was no correlation between RMS20 and total EF (r = 0.12, p = 0.23), or between RMS20 and passive EF (r = − 0.02, p = 0.86). In multivariate regression analysis, passive EF was an independent factor that influenced FPD duration. This study indicated that FPD was associated with conduit function, which includes phasic LA function. Therefore, electrical conduction of the LA and left ventricular diastolic function are closely related. In the clinical setting, when conduction abnormalities are detected, lifestyle measures or interventions can be applied to reduce cardiovascular risk.




Similar content being viewed by others
References
Yamada T, Fukunami M, Shimonagata T, Kumagai K, Ogita H, Asano Y, Hirata A, Masatsugu H, Hoki N (2000) Prediction of paroxysmal atrial fibrillation in patients with congestive heart failure: a prospective study. J Am Coll Cardiol 35:405–413
Yamada T, Fukunami M, Shimonagata T, Kumagai K, Sanada S, Ogita H, Asano Y, Hori M, Hoki N (1999) Dispersion of signal-averaged P wave duration on precordial body surface in patients with paroxysmal atrial fibrillation. Eur Heart J 20:211–220
Tanaka S, Noda T, Kubota T, Segawa T, Iwama M, Kawasaki M, Nishigaki T, Watanabe S, Minagawa T, Minatoguchi S (2015) Evaluation of circadian rhythm of atrial late potentials continuously measured by digital Holter monitor. Ther Res 36:799–807
Yodogawa K, Seino Y, Ohara T, Hayashi M, Miyauchi Y, Katoh T, Mizuno K (2013) Prediction of atrial fibrillation after ischemic stroke using P-wave signal averaged electrocardiography. J Cardiol 61(49):52
Shimada K, Tomita T, Kamijo Y, Higuchi M, Ito K, Koizumi Y, Yamamoto K, Aizawa K, Koshikawa M, Kasai H, Izawa A, Miyashita Y, Kumazaki S, Koyama J, Ikeda U (2012) Hemodialysis-induced P-wave signal-averaged electrocardiogram alterations are indicative of vulnerability to atrial arrhythmias. Circ J 76:612–617
Maeno K, Kasagi S, Ueda A, Kawana F, Ishiwata S, Ohno M, Yamaguchi T, Narui K, Kasai T (2013) Effects of obstructive sleep apnea and its treatment on signal-averaged P-wave duration in men. Circ Arrhythm Electrophysiol 6:287–293
Girasis C, Vassilikos V, Efthimiadis GK, Papadopoulou SL, Dakos G, Dalamaga EG, Chouvarda I, Giannakoulas G, Kamperidis V, Paraskevaidis S, Maglaveras N, Karvounis HI, Parcharidis GE, Styliadis IH (2013) Patients with hypertrophic cardiomyopathy at risk for paroxysmal atrial fibrillation: advanced echocardiographic evaluation of the left atrium combined with non-invasive P-wave analysis. Eur Heart J Cardiovasc Imaging 14:425–434
Ogawa K, Hozumi T, Sugioka K, Iwata S, Otsuka R, Takagi Y, Yoshitani H, Yoshiyama M, Yoshikawa J (2009) Automated assessment of left atrial function from time-left atrial volume curves using a novel speckle tracking imaging method. J Am Soc Echocardiogr 22:63–69
Nagaya M, Kawasaki M, Tanaka R, Onishi N, Sato N, Ono K, Watanabe T, Minatoguchi S, Miwa H, Goto Y, Hirose T, Arai M, Noda T, Watanabe S, Minatoguchi S (2013) Quantitative validation of left atrial structure and function by two-dimensional and three-dimensional speckle tracking echocardiography: a comparative study with three-dimensional computed tomography. J Cardiol 62:188–194
Hirose T, Kawasaki M, Tanaka R, Ono K, Watanabe T, Iwama M, Noda T, Watanabe S, Takemura G, Minatoguchi S (2012) Left atrial function assessed by speckle tracking echocardiography as a predictor of new-onset non-valvular atrial fibrillation: results from a prospective study in 580 adults. Eur Heart J Cardiovasc Imaging 13:243–250
Kojima T, Kawasaki M, Tanaka R, Ono K, Hirose T, Iwama M, Watanabe T, Noda T, Watanabe S, Takemura G, Minatoguchi S (2011) Left atrial global and regional function in patients with paroxysmal atrial fibrillation has already been impaired before enlargement of left atrium: velocity vector imaging echocardiography study. Eur Heart J Cardiovasc Imaging 13:227–234
Farzaneh-Far A, Ariyarajah V, Shenoy C, Dorval JF, Kaminski M, Curillova Z, Wu H, Brown KB, Kwong RY (2011) Left atrial passive emptying function during dobutamine stress MR imaging is a predictor of cardiac events in patients with suspected myocardial ischemia. JACC Cardiovasc Imaging 4:378–388
Dodson JA, Neilan TG, Shah RV, Farhad H, Blankstein R, Steigner M, Michaud GF, John R, Abbasi SA, Jerosch-Herold M, Kwong RY (2014) Left atrial passive emptying function determined by cardiac magnetic resonance predicts atrial fibrillation recurrence after pulmonary vein isolation. Circ Cardiovasc Imaging 7:586–592
Scherr J, Jung P, Schuster T, Pollmer L, Eisele G, Goss F, Schneider J, Halle M (2016) Left ventricular diastolic function is strongly correlated with active emptying of the left atrium: a novel analysis using three-dimensional echocardiography. Cardiovasc Ultrasound 14:43–52
Fujimoto Y, Yodogawa K, Takahashi K, Tsuboi I, Hayashi H, Uetake S, Iwasaki YK, Hayashi M, Miyauchi Y, Shimizu W (2017) Noninvasive evaluation of reverse atrial remodeling after catheter ablation of atrial fibrillation by P wave dispersion. Heart Vessels 32:1375–1381
Doi A, Takagi M, Katayama H, Yoshiyama T, Hayashi Y, Tatsumi H, Yoshiyama M (2018) Diagnostic value of electrocardiographic P-wave characteristics in atrial fibrillation recurrence and tachycardia-induced cardiomyopathy after catheter ablation. Heart Vessels 32:1381-1389
Tsujimoto S, Miyasaka Y, Suwa Y, Taniguchi N, Kittaka S, Yamamoto K, Shiojima I (2018) Diastolic wall strain as a predictor of age-related cardiovascular events in patients with preserved left ventricular ejection fraction. Heart Vessels. https://doi.org/10.1007/s00380-018-1311-5
Allessie M, Ausma J, Schotten U (2002) Electrical, contractile and structural remodeling during atrial fibrillation. Cardiovasc Res. 54:230–246
Vatan MB, Yılmaz S, Ağaç MT, Çakar MA, Erkan H, Aksoy M, Demirtas S, Varım C, Akdemir R, Gündüz H (2015) Relationship between CHA2DS2-VASc score and atrial electromechanical function in patients with paroxysmal atrial fibrillation: A pilot study. J Cardiol 66:382–387
Fukunami M (2001) P and Ta waves on signal-averaged electrocardiogram. JPN J ELECTROCARDIOLOGY 21:384–391
Kawamura M, Munetsugu Y, Kawasaki S, Onishi K, Onuma Y, Kikuchi M, Tanno K, Kobayashi Y (2012) Type III procollagen-N-peptide as a predictor of persistent atrial fibrillation recurrence after cardioversion. Europace 14:1719–1725
Kubota T, Kawasaki M, Takasugi N, Takeyama U, Ishihara Y, Okubo M, Yamaki T, Ojio S, Aoyama T, Arai M, Nishigaki K, Takemura G, Fujiwara H, Minatoguchi S (2009) Evaluation of left atrial degeneration for the prediction of atrial fibrillation: usefulness of integrated backscatter transesophageal echocardiography. JACC Cardiovasc Imaging 2:1039–1047
Kubota T, Kawasaki M, Takasugi N, Imai H, Ishihara Y, Okubo M, Takahashi S, Sato H, Nishigaki K, Takemura G, Minatoguchi S (2012) Left atrial pathological degeneration assessed by integrated backscatter transesophageal echocardiography as a predictor of progression to persistent atrial fibrillation: results from a prospective study of three-years follow-up. Cardiovasc Ultrasound 10:28–34
JCS Joint Working Group (2012) Guidelines for risks and prevention of sudden cardiac death (JCS 2010)—digest version. Circ J 76:489–507
Acknowledgements
We are very grateful to Nakamura M, MSc for supervising the P-SAECG procedures and acquiring data in our electrocardiography laboratory. We would also like to thank Sato N, MSc, Aoki M, MSc, Miyazaki M, MSc, Nagaya M, MSc, Nakamura J, MSc, Onishi, MSc Otsuka, M MSc, Saeki M, MSc, Shouji T, MSc, and Yamamoto I, MSc for providing the experimental equipment. We would like to thank Ms. Nakanishi T for assisting in the preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tanaka, S., Noda, T., Kawasaki, M. et al. Relationship between electrical conduction and phasic left atrial function: P-wave signal-averaged electrocardiography and time-left atrial volume curve assessments using two-dimensional speckle-tracking echocardiography. Heart Vessels 34, 1212–1220 (2019). https://doi.org/10.1007/s00380-019-01351-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-019-01351-y