Abstract
Purpose
Endourology has undergone fundamental changes over the last 2 decades. Maintaining low intrarenal pressure (IRP) during upper urinary tract procedures is an established concept. However, researchers have not yet studied the concept of reduced intravesical pressures (IVPs) during transurethral (TUR) surgery as thoroughly. Low IVP is supposed to decrease complications as fluid retention, TUR syndrome, and incidence of fever. The study aims to give an overview of the contemporarily existing concepts and specify the term of low IVP to avoid TUR-related complications and optimize TUR-related results.
Methods
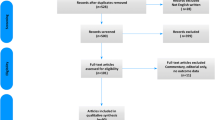
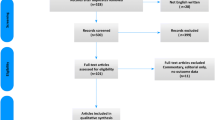
A literature search was performed using PubMed, restricted to original English-written articles, including animal, artificial model, and human studies. Different keywords were transurethral resection, transurethral enucleation, transurethral vaporization, pressure, fluid absorption, and TUR syndrome.
Results
Analyzed mean IVPs during TUR vary between 11 and 35 cmH2O but are mostly kept below 30 cmH2O. Mean maximum IVPs during TUR range from 20 to 55 cmH2O. Maximum IVPs seem to be lower when surgeons utilize continuous flow resection, and irrigation pressures are kept low. The results demonstrate a strong correlation between IVP levels and fluid absorption.
Conclusions
IVP increase remains a neglected predictor of transurethral procedure complications, and endourologists should consider its intraoperative monitoring. Further research is necessary to quantify generated pressures and introduce means of controlling them.

Similar content being viewed by others
References
Gratzke C, Bachmann A, Descazeaud A, Drake MJ, Madersbacher S, Mamoulakis C, Oelke M, Tikkinen KAO, Gravas S (2015) EAU guidelines on the assessment of non-neurogenic male lower urinary tract symptoms including benign prostatic obstruction. Eur Urol 67(6):1099–1109. https://doi.org/10.1016/j.eururo.2014.12.038
Ahyai SA, Gilling P, Kaplan SA, Kuntz RM, Madersbacher S, Montorsi F, Speakman MJ, Stief CG (2010) Meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic enlargement. Eur Urol 58(3):384–397. https://doi.org/10.1016/j.eururo.2010.06.005
Cornu JN, Ahyai S, Bachmann A, de la Rosette J, Gilling P, Gratzke C, McVary K, Novara G, Woo H, Madersbacher S (2015) A systematic review and meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic obstruction: an update. Eur Urol 67(6):1066–1096. https://doi.org/10.1016/j.eururo.2014.06.017
Mordasini L, Abt D, Mullhaupt G, Engeler DS, Luthi A, Schmid HP, Schwab C (2015) Is absorption of irrigation fluid a problem in Thulium laser vaporization of the prostate? A prospective investigation using the expired breath ethanol test. BMC Urol 15:35. https://doi.org/10.1186/s12894-015-0029-2
Tokas T, Herrmann TRW, Skolarikos A, Nagele U (2019) Pressure matters: intrarenal pressures during normal and pathological conditions, and impact of increased values to renal physiology. World J Urol 37(1):125–131. https://doi.org/10.1007/s00345-018-2378-4
Tokas T, Skolarikos A, Herrmann TRW, Nagele U (2019) Pressure matters 2: intrarenal pressure ranges during upper-tract endourological procedures. World J Urol 37(1):133–142. https://doi.org/10.1007/s00345-018-2379-3
Drake MJ, Doumouchtsis SK, Hashim H, Gammie A (2018) Fundamentals of urodynamic practice, based on International Continence Society good urodynamic practices recommendations. Neurourol Urodyn 37(S6):S50–s60. https://doi.org/10.1002/nau.23773
Çetinel B, Önal B, Can G, Talat Z, Erhan B, Gündüz B (2017) Risk factors predicting upper urinary tract deterioration in patients with spinal cord injury: a retrospective study. Neurourol Urodyn 36(3):653–658. https://doi.org/10.1002/nau.22984
Chancellor MB, Rivas DA, Bourgeois IM (1996) Laplace's law and the risks and prevention of bladder rupture after enterocystoplasty and bladder autoaugmentation. Neurourol Urodyn 15(3):223–233. https://doi.org/10.1002/(sici)1520-6777(1996)15:3<223:Aid-nau7>3.0.Co;2-h
Rivas DA, Chancellor MB, Huang B, Epple A, Figueroa TE (1996) Comparison of bladder rupture pressure after intestinal bladder augmentation (ileocystoplasty) and myomyotomy (autoaugmentation). Urology 48(1):40–46. https://doi.org/10.1016/s0090-4295(96)00096-9
Ran L, He W, Zhu X, Zhou Q, Gou X (2013) Comparison of fluid absorption between transurethral enucleation and transurethral resection for benign prostate hyperplasia. Urol Int 91(1):26–30. https://doi.org/10.1159/000348793
Hermanns T, Grossmann NC, Wettstein MS, Fankhauser CD, Capol JC, Poyet C, Hefermehl LJ, Zimmermann M, Sulser T, Muller A (2015) Absorption of irrigation fluid occurs frequently during high power 532 nm laser vaporization of the prostate. J Urol 193(1):211–216. https://doi.org/10.1016/j.juro.2014.07.117
Falagas ME, Pitsouni EI, Malietzis GA, Pappas G (2008) Comparison of PubMed, Scopus, Web of Science, and Google Scholar: strengths and weaknesses. FASEB J 22(2):338–342. https://doi.org/10.1096/fj.07-9492LSF
Madsen PO, Naber KG (1973) The importance of the pressure in the prostatic fossa and absorption of irrigating fluid during transurethral resection of the prostate. J Urol 109(3):446–452
Hansen RI, Iversen HG, Christiansen B (1978) Intravesical pressure during transurethral resection using Iglesias resectoscope with continuous irrigation and suction. Scand J Urol Nephrol 12(3):223–225
Rabe HB, de Kock ML (1982) Transurethral prostatectomy—studies with different intravesical pressures. S Afr Med J 61(21):778–780
Bretan PN Jr, Carroll PR, McClure RD, Williams RD (1985) Improved continuous flow transurethral prostatectomy. J Urol 134(1):77–80
Hahn R, Berlin T, Johansson H, Lewenhaupt A (1988) Changes in intravesical pressure during irrigating fluid absorption in transurethral prostatic surgery. Urol Res 16(4):281–285
Ekengren J, Hahn RG (1994) Continuous versus intermittent flow irrigation in transurethral resection of the prostate. Urology 43(3):328–332
Zhang W, Ekengren J, Hahn RG (1996) Large-sized bladders reduce intravesical pressure and fluid absorption during TURP using the suprapubic trocar. Urol Int 56(1):28–32
Hahn RG (2000) Intravesical pressure during irrigating fluid absorption in transurethral resection of the prostate. Scand J Urol Nephrol 34(2):102–108
Gray RA, Lynch C, Hehir M, Worsley M (2001) Intravesical pressure and the TUR syndrome. Anaesthesia 56(5):461–465
El-Abbady AA, Shoukry MS, Hanno AG, Younis LK, Abdel-Rahman M (2002) Repeated transurethral resection of recurrent superficial bladder tumors—does it affect the spread and stage of the tumor? Scand J Urol Nephrol 36(1):60–64
Gray RA, Moores AH, Hehir M, Worsley M (2003) Transurethral vaporisation of the prostate and irrigating fluid absorption. Anaesthesia 58(8):787–791
Hahn RG (1990) Fluid and electrolyte dynamics during development of the TURP syndrome. Br J Urol 66(1):79–84
Maluf NS, Boren JS, Brandes GE (1956) Absorption of irrigating solution and associated changes upon transurethral electroresection of prostate. J Urol 75(5):824–836
Oester A, Madsen PO (1969) Determination of absorption of irrigating fluid during transurethral resection of the prostate by means of radioisotopes. J Urol 102(6):714–719
Hulten JO (2002) How to master absorption during transurethral resection of the prostate: basic measures guided by the ethanol method. BJU Int 90(3):244–247
Hulten JO, Hahn RG (1989) Monitoring irrigating fluid absorption during transurethral resection of the prostate (TURP); a comparison between 1 and 2% ethanol as a tracer. Scand J Urol Nephrol 23(2):103–108
Stalberg HP, Hahn RG, Jones AW (1992) Ethanol monitoring of transurethral prostatic resection during inhaled anesthesia. Anesth Analg 75(6):983–988
Hulten J, Bengtsson M, Engberg A, Hjertberg H, Svedberg J (1984) The pressure in the prostatic fossa and fluid absorption. Scand J Urol Nephrol (Suppl) 82:33–43
Hahn RG (2000) The volumetric fluid balance as a measure of fluid absorption during transurethral resection of the prostate. Eur J Anaesthesiol 17(9):559–565
Hulten JO, Sundstrom GS (1990) Extravascular absorption of irrigating fluid during TURP. The role of transmural bladder pressure as the driving pressure gradient. Br J Urol 65(1):39–42
Hulten JO, Jorfeldt LS, Wictorsson YM (1986) Monitoring fluid absorption during TURP by marking the irrigating solution with ethanol. Scand J Urol Nephrol 20(4):245–251
Hjertberg H, Pettersson B (1992) The use of a bladder pressure warning device during transurethral prostatic resection decreases absorption of irrigation fluid. Br J Urol 69(1):56–60
Hulten J, Sarma VJ, Hjertberg H, Palmquist B (1991) Monitoring of irrigating fluid absorption during transurethral prostatectomy. A study in anaesthetised patients using a 1% ethanol tag solution. Anaesthesia 46(5):349–353
Konrad C, Gerber HR, Schuepfer G, Schmucki O (1998) Transurethral resection syndrome: effect of the introduction into clinical practice of a new method for monitoring fluid absorption. J Clin Anesth 10(5):360–365
Mommsen S, Genster HG, Moller J (1977) Changes in the serum concentrations of sodium, potassium, and free haemoglobin during transurethral resection of the prostate—parts of the TUR-syndrome? Urol Res 5(4):201–205
Norlen H, Allgen LG (1993) A comparison between intermittent and continuous transurethral resection of the prostate. Scand J Urol Nephrol 27(1):21–25
Madsen PO, Frimodt-Moller PC (1984) Transurethral prostatic resection with suprapubic trocar technique. J Urol 132(2):277–279
Rao PN, Lister B, Livesey JL, Barnard RJ (1983) Are we using the right irrigation system? Br J Urol 55(3):287–293
Reuter HJ, Jones LW (1974) Physiologic low pressure irrigation for transurethral resection: suprapubic trocar drainage. J Urol 111(2):210–212
Heidler H (1999) Frequency and causes of fluid absorption: a comparison of three techniques for resection of the prostate under continuous pressure monitoring. BJU Int 83(6):619–622
Mebust WK, Holtgrewe HL, Cockett AT, Peters PC (2002) Transurethral prostatectomy: immediate and postoperative complications. Cooperative study of 13 participating institutions evaluating 3,885 patients. J Urol 167(1):5–9. https://doi.org/10.1016/s0022-5347(05)65370-0 (J Urol, 141: 243-247, 1989)
Porsch M, Mittelstadt P, Wendler JJ, Baumunk D, Fichtler K, Janitzky A, Lux A, Liehr UB, Schostak M (2016) Measurement of procedure-specific irrigation-fluid absorption in transurethral therapy of lower urinary tract syndrome, using ethanolic saline and breath alcometry. Urol Int 97(3):299–309. https://doi.org/10.1159/000445694
Akcayoz M, Kaygisiz O, Akdemir O, Aki FT, Adsan O, Cetinkaya M (2006) Comparison of transurethral resection and plasmakinetic transurethral resection applications with regard to fluid absorption amounts in benign prostate hyperplasia. Urol Int 77(2):143–147. https://doi.org/10.1159/000093909
Hubert J, Cormier L, Gerbaud PF, Guillemin F, Pertek JP, Mangin P (1996) Computer-controlled monitoring of bladder pressure in the prevention of 'TUR syndrome': a randomized study of 53 cases. Br J Urol 78(2):228–233
Doizi S, Letendre J, Cloutier J, Ploumidis A, Traxer O (2020) Continuous monitoring of intrapelvic pressure during flexible ureteroscopy using a sensor wire: a pilot study. World J Urol. https://doi.org/10.1007/s00345-020-03216-w
Author information
Authors and Affiliations
Consortia
Contributions
TT: data management, data analysis, and manuscript writing. GO: data management and data analysis. TRWH: interpreting data and manuscript revision. UN: protocol/project development, interpreting data, and manuscript revision.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights
This review does not involve human participants and/or animals.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tokas, T., Ortner, G., Herrmann, T.R.W. et al. Relevance of intravesical pressures during transurethral procedures. World J Urol 39, 1747–1756 (2021). https://doi.org/10.1007/s00345-020-03401-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-020-03401-x