Abstract
Purpose
To evaluate the role of preoperative multiparametric magnetic resonance imaging (MRI) as predictor of post-prostatectomy incontinence (PPI).
Methods
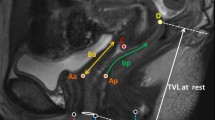
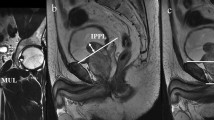
We analyzed patients who underwent robot-assisted radical prostatectomy for localized prostate cancer at our institution between July 2015 and April 2017. In these patients, we measured the perfusion quality of the pelvic floor with contrast media kinetics in the preoperative MRI of the prostate and compared the levator ani muscle (region of interest) to the surrounding pelvic muscle structures (reference). Prospectively collected questionnaires regarding urinary incontinence were then evaluated 1 year postoperatively. Outcomes were dichotomized into “continent” (ICIQ-Score = 0–5) and “incontinent” (ICIQ-Score ≥ 6). In each patient, we determined the perfusion ratio of the levator ani muscle divided by the surrounding pelvic muscle structures and compared them among the groups.
Results
Forty-two patients were included in the study (n = 22 in “continent”, n = 20 in “incontinent” group). The median perfusion ratio from the continent group was significantly higher compared to the incontinent group (1.61 vs. 1.15; 95% CI 0.09–0.81, p = 0.015). The median perfusion ratio in “excellent” (ICIQ-Score = 0) was significantly higher than in “poor” (ICIQ-Score ≥ 11) outcomes (1.48 vs. 0.94; 95% CI 0.04–1.03, p = 0.036). Further, a higher perfusion ratio was negatively correlated with ICIQ-Score (r = − 0.33; 95% CI − 0.58 to 0.03; p = 0.031).
Conclusions
Our data demonstrate a promising new strategy to predict PPI through the perfusion quality of pelvic muscle structures with contrast media kinetics. This may facilitate preoperative patient consulting and decision-making.



Similar content being viewed by others
References
Ficarra V, Borghesi M, Suardi N, De Naeyer G, Novara G, Schatteman P, De Groote R, Carpentier P, Mottrie A (2013) Long-term evaluation of survival, continence and potency (SCP) outcomes after robot-assisted radical prostatectomy (RARP). BJU Int 112(3):338–345. https://doi.org/10.1111/bju.12001
Punnen S, Cowan JE, Chan JM, Carroll PR, Cooperberg MR (2015) Long-term health-related quality of life after primary treatment for localized prostate cancer: results from the CaPSURE registry. Eur Urol 68(4):600–608. https://doi.org/10.1016/j.eururo.2014.08.074
Sciarra A, Gentilucci A, Salciccia S, Von Heland M, Ricciuti GP, Marzio V, Pierella F, Musio D, Tombolini V, Frantellizzi V, Pasquini M, Maraone A, Guandalini A, Maggi M (2018) Psychological and functional effect of different primary treatments for prostate cancer: a comparative prospective analysis. Urol Oncol 36(7):340.e7–340.e21. https://doi.org/10.1016/j.urolonc.2018.03.022
Liss MA, Osann K, Canvasser N, Chu W, Chang A, Gan J, Li R, Santos R, Skarecky D, Finley DS, Ahlering TE (2010) Continence definition after radical prostatectomy using urinary quality of life: evaluation of patient reported validated questionnaires. J Urol 183(4):1464–1468. https://doi.org/10.1016/j.juro.2009.12.009
Sanda MG, Dunn RL, Michalski J, Sandler HM, Northouse L, Hembroff L, Lin X, Greenfield TK, Litwin MS, Saigal CS, Mahadevan A, Klein E, Kibel A, Pisters LL, Kuban D, Kaplan I, Wood D, Ciezki J, Shah N, Wei JT (2008) Quality of life and satisfaction with outcome among prostate-cancer survivors. N Engl J Med 358(12):1250–1261. https://doi.org/10.1056/NEJMoa074311
Ficarra V, Novara G, Rosen RC, Artibani W, Carroll PR, Costello A, Menon M, Montorsi F, Patel VR, Stolzenburg JU, Van der Poel H, Wilson TG, Zattoni F, Mottrie A (2012) Systematic review and meta-analysis of studies reporting urinary continence recovery after robot-assisted radical prostatectomy. Eur Urol 62(3):405–417. https://doi.org/10.1016/j.eururo.2012.05.045
Becker A, Tennstedt P, Hansen J, Trinh QD, Kluth L, Atassi N, Schlomm T, Salomon G, Haese A, Budaeus L, Michl U, Heinzer H, Huland H, Graefen M, Steuber T (2014) Functional and oncological outcomes of patients aged < 50 years treated with radical prostatectomy for localised prostate cancer in a European population. BJU Int 114(1):38–45. https://doi.org/10.1111/bju.12407
Wei Y, Wu YP, Lin MY, Chen SH, Lin YZ, Li XD, Zheng QS, Xue XY, Xu N (2018) Impact of obesity on long-term urinary incontinence after radical prostatectomy: a meta-analysis. Biomed Res Int 2018:8279523. https://doi.org/10.1155/2018/8279523
Rajih E, Meskawi M, Alenizi AM, Zorn KC, Alnazari M, Zanaty M, Alhathal N, El-Hakim A (2018) Perioperative predictors for post-prostatectomy urinary incontinence in prostate cancer patients following robotic-assisted radical prostatectomy: long-term results of a Canadian prospective cohort. Can Urol Assoc J. https://doi.org/10.5489/cuaj.5356
Konety BR, Sadetsky N, Carroll PR, Ca PI (2007) Recovery of urinary continence following radical prostatectomy: the impact of prostate volume–analysis of data from the CaPSURE Database. J Urol 177(4):1423–1425. https://doi.org/10.1016/j.juro.2006.11.089(discussion 1425–1426)
Kunz I, Musch M, Roggenbuck U, Klevecka V, Kroepfl D (2013) Tumour characteristics, oncological and functional outcomes in patients aged ≥ 70 years undergoing radical prostatectomy. BJU Int 111(3 Pt B):E24–E29. https://doi.org/10.1111/j.1464-410x.2012.11368.x
Steineck G, Bjartell A, Hugosson J, Axen E, Carlsson S, Stranne J, Wallerstedt A, Persson J, Wilderang U, Thorsteinsdottir T, Gustafsson O, Lagerkvist M, Jiborn T, Haglind E, Wiklund P, LS Committee (2015) Degree of preservation of the neurovascular bundles during radical prostatectomy and urinary continence 1 year after surgery. Eur Urol 67(3):559–568. https://doi.org/10.1016/j.eururo.2014.10.011
Nyarangi-Dix JN, Radtke JP, Hadaschik B, Pahernik S, Hohenfellner M (2013) Impact of complete bladder neck preservation on urinary continence, quality of life and surgical margins after radical prostatectomy: a randomized, controlled, single blind trial. J Urol 189(3):891–898. https://doi.org/10.1016/j.juro.2012.09.082
Shao IH, Chou CY, Huang CC, Lin CF, Chang YH, Tseng HJ, Wu CT (2015) A specific cystography pattern can predict postprostatectomy incontinence. Ann Surg Oncol 22(Suppl 3):S1580–S1586. https://doi.org/10.1245/s10434-015-4847-y
Gandaglia G, Suardi N, Gallina A, Capitanio U, Abdollah F, Salonia A, Nava L, Colombo R, Guazzoni G, Rigatti P, Montorsi F, Briganti A (2012) Preoperative erectile function represents a significant predictor of postoperative urinary continence recovery in patients treated with bilateral nerve sparing radical prostatectomy. J Urol 187(2):569–574. https://doi.org/10.1016/j.juro.2011.10.034
Murphy G, Haddock P, Doak H, Jackson M, Dorin R, Meraney A, Kesler S, Staff I, Wagner JR (2015) Urinary bother as a predictor of postsurgical changes in urinary function after robotic radical prostatectomy. Urology 86(4):817–823. https://doi.org/10.1016/j.urology.2015.04.041
Tienza A, Robles JE, Hevia M, Algarra R, Diez-Caballero F, Pascual JI (2018) Prevalence analysis of urinary incontinence after radical prostatectomy and influential preoperative factors in a single institution. Aging Male 21(1):24–30. https://doi.org/10.1080/13685538.2017.1369944
Heesakkers J, Farag F, Bauer RM, Sandhu J, De Ridder D, Stenzl A (2017) Pathophysiology and contributing factors in postprostatectomy incontinence: a review. Eur Urol 71(6):936–944. https://doi.org/10.1016/j.eururo.2016.09.031
Donovan JL, Peters TJ, Abrams P, Brookes ST, de aa Rosette JJ, Schafer W (2000) Scoring the short form ICSmaleSF questionnaire. International Continence Society. J Urol 164(6):1948–1955
Abrams P, Avery K, Gardener N, Donovan J, Board IA (2006) The International Consultation on Incontinence Modular Questionnaire: http://www.iciq.net. J Urol 175(3 Pt 1):1063–1066. https://doi.org/10.1016/s0022-5347(05)00348-4(discussion 1066)
Weinreb JC, Barentsz JO, Choyke PL, Cornud F, Haider MA, Macura KJ, Margolis D, Schnall MD, Shtern F, Tempany CM, Thoeny HC, Verma S (2016) PI-RADS prostate imaging—reporting and data system: 2015, version 2. Eur Urol 69(1):16–40. https://doi.org/10.1016/j.eururo.2015.08.052
R Core Team (2017) R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna. https://www.R-project.org/
Hatiboglu G, Teber D, Hohenfellner M (2012) Robot-assisted prostatectomy: the new standard of care. Langenbecks Arch Surg 397(3):343–352. https://doi.org/10.1007/s00423-011-0743-5
Paparel P, Akin O, Sandhu JS, Otero JR, Serio AM, Scardino PT, Hricak H, Guillonneau B (2009) Recovery of urinary continence after radical prostatectomy: association with urethral length and urethral fibrosis measured by preoperative and postoperative endorectal magnetic resonance imaging. Eur Urol 55(3):629–637. https://doi.org/10.1016/j.eururo.2008.08.057
Avulova S, Zhao Z, Lee D, Huang LC, Koyama T, Hoffman KE, Conwill RM, Wu XC, Chen V, Cooperberg MR, Goodman M, Greenfield S, Hamilton AS, Hashibe M, Paddock LE, Stroup A, Resnick MJ, Penson DF, Barocas DA (2018) The effect of nerve sparing status on sexual and urinary function: 3-year results from the CEASAR study. J Urol 199(5):1202–1209. https://doi.org/10.1016/j.juro.2017.12.037
Mungovan SF, Sandhu JS, Akin O, Smart NA, Graham PL, Patel MI (2017) Preoperative membranous urethral length measurement and continence recovery following radical prostatectomy: a systematic review and meta-analysis. Eur Urol 71(3):368–378. https://doi.org/10.1016/j.eururo.2016.06.023
Coakley FV, Eberhardt S, Kattan MW, Wei DC, Scardino PT, Hricak H (2002) Urinary continence after radical retropubic prostatectomy: relationship with membranous urethral length on preoperative endorectal magnetic resonance imaging. J Urol 168(3):1032–1035. https://doi.org/10.1097/01.ju.0000025881.75827.a5
Kim LHC, Patel A, Kinsella N, Sharabiani MTA, Ap Dafydd D, Cahill D (2019) Association between preoperative magnetic resonance imaging-based urethral parameters and continence recovery following robot-assisted radical prostatectomy. Eur Urol Focus. https://doi.org/10.1016/j.euf.2019.01.011
von Bodman C, Matsushita K, Savage C, Matikainen MP, Eastham JA, Scardino PT, Rabbani F, Akin O, Sandhu JS (2012) Recovery of urinary function after radical prostatectomy: predictors of urinary function on preoperative prostate magnetic resonance imaging. J Urol 187(3):945–950. https://doi.org/10.1016/j.juro.2011.10.143
Nguyen L, Jhaveri J, Tewari A (2008) Surgical technique to overcome anatomical shortcoming: balancing post-prostatectomy continence outcomes of urethral sphincter lengths on preoperative magnetic resonance imaging. J Urol 179(5):1907–1911. https://doi.org/10.1016/j.juro.2008.01.036
Schlomm T, Heinzer H, Steuber T, Salomon G, Engel O, Michl U, Haese A, Graefen M, Huland H (2011) Full functional-length urethral sphincter preservation during radical prostatectomy. Eur Urol 60(2):320–329. https://doi.org/10.1016/j.eururo.2011.02.040
Author information
Authors and Affiliations
Contributions
FAS: protocol/project development, data collection and management, data analysis, manuscript writing. MSW: data collection and management, data analysis, manuscript editing. TMK: protocol/project development, manuscript editing. TH: project development, manuscript editing. AB: protocol/project development, data collection and management, manuscript editing. AMH: data analysis, manuscript editing. DE: protocol/project development, manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (local ethical review board “Kantonale Ethikkomission Zürich”, study approval: KEK-StV-Nr. 06/08) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Schmid, F.A., Wettstein, M.S., Kessler, T.M. et al. Contrast media kinetics in multiparametric magnetic resonance imaging before radical prostatectomy predicts the probability of postoperative incontinence. World J Urol 38, 1741–1748 (2020). https://doi.org/10.1007/s00345-019-02952-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-019-02952-y