Abstract
Introduction
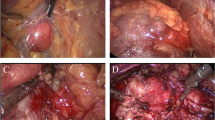
Adherent perirenal fat (APF) can be defined as inflammatory fat sticking to renal parenchyma, whose dissection is difficult and makes it troublesome to expose the tumour. Our objective was to evaluate the impact of APF on the technical difficulty of robot-assisted partial nephrectomy (RPN).
Patients and methods
We analysed data of 202 patients who underwent RPN for a small renal tumour. Patients were divided into two groups according to the presence of APF. Peri-operative data were compared between the two groups. Predictors of APF were evaluated by univariate and multivariate analysis. The validity of the MAP score (radiological scoring system) was also assessed.
Results
APF was observed in 80 patients (39.6 %). Tumour complexity and surgeon’s experience were similar between both groups. Operative time was 40 min longer in the APF group (188.5 vs. 147.9 min, p < 0.0001). Blood loss was twice higher, and transfusions were more common in the APF group (694 vs. 330 ml, p < 0.0001 and 19 vs. 5.8 %, p = 0.003, respectively). APF was associated with an increased risk of conversion to open surgery (11.2 vs. 0 %, p = 0.0002) or radical nephrectomy (6.2 vs. 0.8 %, p = 0.03). In multivariate analysis, male gender (OR 13.2, p < 0.0001), obesity (OR 1.2, p = 0.007), hypertension (OR 3.7, p = 0.02), and MAP score (OR 3.3; p < 0.0001) were significant predictors of APF.
Conclusion
During RPN, APF is associated with increased bleeding and a higher risk of conversion to open surgery and to radical nephrectomy. Male gender, hypertension, obesity, and MAP score are predictors of APF.

Similar content being viewed by others
References
Ljungberg B, Bensalah K, BexA et al. Guidelines on renal cell carcinoma. Uroweb 2013. Available at: http://www.uroweb.org/gls/pdf/10_Renal_Cell_Carcinoma_LRV2.pdf
Gill IS, Kavoussi LR, Lane BR et al (2007) Comparison of 1,800 laparoscopic and open partial nephrectomies for single renal tumors. J Urol 178:41–46
Ficarra V, Rossanese M, Gnech M, Novara G, Mottrie A (2014) Outcomes and limitations of robotic and laparoscopic partial nephrectomy. Curr Opin Urol 24(5):441–447
Van Poppel H, DaPozzo L, Albrecht W et al (2007) A prospective randomized EORTC intergroup phase 3 study comparing the complications of elective nephron-sparing surgery and radical nephrectomy for low-stage renal carcinoma. Eur Urol 51:1606–1615
Stephenson AJ, Hakimi AA, Snyder ME et al (2004) Complications of radical and partial nephrectomy in a large contemporary cohort. J Urol 171:130–134
Poon SA, Silberstein JL, Chen LY et al (2013) Trends in partial and radical nephrectomy: an analysis of case logs from certifying urologists. J Urol 190(2):464–469
Kutikov A, Uzzo RG (2009) The R.E.N.A.L. Nephrometry score: a comprehensive standardized system for quantitating renal tumor size, location and depth. J Urol 182:844–853
Ficarra V, Novara G, Secco S et al (2009) Preoperative aspects and dimension used for an anatomical (PADUA) classification of renal tumours in patients who are candidates for nephron-sparing surgery. Eur Urol 56(5):786–793
Zhang ZY, Tang Q, Li XS et al (2014) Clinical analysis of the PADUA and the RENAL scoring systems for renal neoplasms: a retrospective study of 245 patients undergoing laparoscopic partial nephrectomy. Int J Urol 21(1):40–44
Kruck S, Anastasiadis AG, Walcher U, Stenzl A, Hermann TR, Nagele U (2012) Laparoscopic partial nephrectomy: risk stratification according to patient and tumor characteristics. World J Urol 30(5):639–646
Long JA, Arnoux V, Fiard G et al (2013) External validation of the RENAL nephrometry score in renal tumours treated by partial nephrectomy. BJU Int 111(2):233–239
Macleod LC, His RS, Gore JL, Wright JL, Harper JD (2014) Perinephric fat thickness is an independent predictor of operative complexity during robot-assisted partial nephrectomy. J Endourol 28(5):587–591
Bylund JR, Qiong H, Crispen PL, Venkatesh R, Strup SE (2013) Association of clinical and radiographic features with perinephric “sticky” fat. J Endourol 27(3):370–373
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 240(2):205–213
Eisner BH, Zargooshi J, Berger AD et al (2010) Gender differences in subcutaneous and perirenal fat distribution. Surg Radiol Anat 32(9):879–882. doi:10.1007/s00276-010-0692-7
Kim S, Choi S, Lee SM et al (2013) Predictive vale of preoperative unenhanced computed tomography during ureteroscopic lithotripsy: a single institute’s experience. Korean J Urol 54:772–777
Davidiuk AJ, Parker AS, Thomas CS et al (2014) Mayo adhesive probability score; an accurate image-based scoring system to predict adherent perinephric fat in partial nephrectomy. Eur Urol 66(6):1165–1171. doi:10.1016/j.eururo.2014.08.054
Wang AJ, Bhayani SB (2009) Robotic partial nephrectomy versus laparoscopic partial nephrectomy for renal cell carcinoma: single- surgeon analysis of >00 consecutive procedures. Urology 73:306–310
Hew MN, Baseskioglu B, Barwari K et al (2011) Critical appraisal of the PADUA classification and assessment of the R.E.N.A.L. nephrometry score in patients undergoing partial nephrectomy. J Urol 186(1):42–46
Long JA, Arnoux V, Fiard G et al (2013) External validation of the RENAL nephrometry score in renal tumours treated by partial nephrectomy. BJU Int 111(2):233–239
Zheng Y, Espiritu P, Hakky T et al (2013) Predicting ease of perinephric fat dissection at time of partial nephrectomy using preoperative fat density characteristics. BJU Int 114(6):872–880. doi:10.1111/bju.12579
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
Local ethics committee approval.
Author information
Authors and Affiliations
Corresponding author
Additional information
Zine-Eddine Khene and Benoit Peyronnet have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Khene, ZE., Peyronnet, B., Mathieu, R. et al. Analysis of the impact of adherent perirenal fat on peri-operative outcomes of robotic partial nephrectomy. World J Urol 33, 1801–1806 (2015). https://doi.org/10.1007/s00345-015-1500-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-015-1500-0