Abstract
Objectives
Intravertebral cleft (IVC) is a common but not unique imaging manifestation in Kümmell’s disease. To date, great controversy exists regarding the specific mechanisms of IVC. In this study, we aimed to investigate the characteristics of microarchitecture and metabolism in patients with IVC and to analyse the correlations between degree of vertebral collapse and risk factors.
Methods
A total of 79 elderly men were included in this study. We divided all patients into two groups: the IVC group (30 patients) and the non-IVC group (49 patients). We compared the differences in microarchitecture and bone turnover marker (BTM) serum concentrations between the groups and analysed risk factors affecting vertebral collapse by using the Mann–Whitney U test and Spearman’s correlation test.
Results
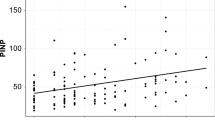
Quantitative analysis of the microarchitecture showed higher content of necrotic bone (p < 0.001) and lower content of lamellar bone (p < 0.001) in the IVC group. Analysis of BTMs identified lower concentration of N-terminal propeptide of type I collagen (PINP, p = 0.002) and higher concentration of β-isomerized C-terminal telopeptide (β-CTX, p < 0.001) in the IVC group. The correlation analysis showed that lamellar bone content (p < 0.001) and spine T-score (p = 0.011) were significantly correlated with the degree of vertebral collapse.
Conclusions
IVC is a radiological feature of excessive bone resorption by higher activities of osteoclasts and decreased bone remodelling ability by lower activities of osteoblasts. Histomorphological feature in patients with IVC is delayed callus mineralisation, which may increase the risk of vertebral collapse.
Key Points
• A key histomorphological feature in patients with IVC is delayed callus mineralisation, which may aggravate the degree of vertebral collapse.
• We investigated bone metabolism in patients with IVC to evaluate the activities of osteoclasts and osteoblasts directly.
• We propose a novel hypothesis for the pathogenesis of IVC: bone resorption by higher activity of osteoclasts and decreased callus mineralisation ability by lower activity of osteoblasts are the main mechanisms leading to IVC.






Similar content being viewed by others
Abbreviations
- ALP:
-
Alkaline phosphatase
- BTMs:
-
Bone turnover markers
- BV/TV:
-
Cancellous bone volume/tissue volume
- EBV/TV:
-
Endochondral bone volume/tissue volume
- FV/TV:
-
Fibrous tissue volume/tissue volume
- IVC:
-
Intravertebral cleft
- LBV/TV:
-
Lamellar bone volume/tissue volume
- NBV/TV:
-
Necrotic bone volume/tissue volume
- OST:
-
Osteocalcin
- PINP:
-
N-terminal propeptide of type I collagen
- PKP:
-
Percutaneous kyphoplasty
- PMHC:
-
Percentage of middle height compression
- WBV/TV:
-
Woven bone volume/tissue volume
- β-CTX:
-
β-Isomerized C-terminal telopeptide
References
Kümmell H (1895) Ueber die traumatischen Erkrankungen der Wirbelsäule1). Dtsch Med Wochenschr 21:180–181
Matzaroglou C, Georgiou CS, Panagopoulos A et al (2014) Kümmell’s disease: clarifying the mechanisms and patients’ inclusion criteria. Open Orthop J 8:288–297
Young WF, Brown D, Kendler A, Clements D (2002) Delayed post-traumatic osteonecrosis of a vertebral body (Kummell’s disease). Acta Orthop Belg 68:13
Stell HH (1951) Kümmell’s disease. Am J Surg 81:161–7
Malghem J, Maldague B, Labaisse MA et al (1993) Intravertebral vacuum cleft: changes in content after supine positioning. Radiology 187:483–487
Sarli M, Pérez Manghi FC, Gallo R, Zanchetta JR (2005) The vacuum cleft sign: an uncommon radiological sign. Osteoporos Int 16:1210–1214
Kumpan W, Salomonowitz E, Seidl G, Wittich GR (1986) The intravertebral vacuum phenomenon. Skeletal Radiol 15:444–447
Mirovsky Y, Anekstein Y, Shalmon E, Peer A (2005) Vacuum clefts of the vertebral bodies. AJNR Am J Neuroradiol 26:1634–1640
Sasaki Y, Aoki Y, Nakajima A et al (2013) Delayed neurologic deficit due to foraminal stenosis following osteoporotic late collapse of a lumbar spine vertebral body. Case Rep Orthop 2013:682075
He D, Yu W, Chen Z, Li L, Zhu K, Fan S (2016) Pathogenesis of the intravertebral vacuum of Kümmell’s disease (review). Exp Ther Med 12:879–882
Heo DH, Chin DK, Yoon YS, Kuh SU (2009) Recollapse of previous vertebral compression fracture after percutaneous vertebroplasty. Osteoporos Int 20:473–480
Fang X, Yu F, Fu S, Song H (2015) Intravertebral clefts in osteoporotic compression fractures of the spine: incidence, characteristics, and therapeutic efficacy. Int J Clin Exp Med 8:16960–16968
Niu J, Zhou H, Meng Q, Shi J, Meng B, Yang H (2015) Factors affecting recompression of augmented vertebrae after successful percutaneous balloon kyphoplasty: a retrospective analysis. Acta Radiol 56:1380–1387
Theodorou DJ (2001) The intravertebral vacuum cleft sign. Radiology 221:787–788
Ito Y, Hasegawa Y, Toda K, Nakahara S (2002) Pathogenesis and diagnosis of delayed vertebral collapse resulting from osteoporotic spinal fracture. Spine J 2(2):101–106
Maldague BE, Noel HM, Malghem JJ (1978) The intravertebral vacuum cleft: a sign of ischemic vertebral collapse 1. Radiology 129:23–29
Ratcliffe JF (1980) The arterial anatomy of the adult human lumbar vertebral body: a microarteriographic study. J Anat 131:57–79
Van Eenenaam DP, el-Khoury GY (1993) Delayed post-traumatic vertebral collapse (Kummell’s disease): case report with serial radiographs, computed tomographic scans, and bone scans. Spine (Phila Pa 1976) 18: 1236–41.
Naul LG, Peet GL, Maupin WB (1989) Avascular necrosis of the vertebral body: MR imaging. Radiology 172:219
Qi H, Xue J, Gao J, Zhang Y, Sun J, Wang G (2020) Changes of bone turnover markers and bone tissue content after severe osteoporotic vertebral compression fracture. Med Sci Monit 26:e923713
Qi H, Qi J, Gao J, Sun J, Wang G (2021) The impact of bone mineral density on bone metabolism and the fracture healing process in elderly Chinese patients with osteoporotic vertebral compression fractures. J Clin Densitom 24:135–145
Diamond TH, Clark WA, Kumar SV (2007) Histomorphometric analysis of fracture healing cascade in acute osteoporotic vertebral body fractures. Bone 40:775–780
Vernon-Roberts B, Pirie CJ (1973) Healing trabecular microfractures in the bodies of lumbar vertebrae. Ann Rheum Dis 32:406–412
Jelinek JS, Kransdorf MJ, Gray R, Aboulafia AJ, Malawer MM (1996) Percutaneous transpedicular biopsy of vertebral body lesions. Spine (Phila Pa 1976) 21: 2035–2040.
Chaudhary RK, Acharya S, Chahal RS, Kalra KL (2019) Fluoroscopy guided percutaneous transpedicular biopsy of vertebral body lesion. J Nepal Health Res Counc 17:163–167
Baur A, Stäbler A, Arbogast S, Duerr HR, Bartl R, Reiser M (2002) Acute osteoporotic and neoplastic vertebral compression fractures: fluid sign at MR imaging. Radiology 225:730
Peh WC, Gelbart MS, Gilula LA, Peck DD (2003) Percutaneous vertebroplasty: treatment of painful vertebral compression fractures with intraosseous vacuum phenomena. AJR Am J Roentgenol 180:1411–1417
Hiwatashi A, Ohgiya Y, Kakimoto N, Westesson PL (2007) Cement leakage during vertebroplasty can be predicted on preoperative MRI. AJR Am J Roentgenol 188:1089–1093
Tanigawa N, Kariya S, Komemushi A et al (2009) Cement leakage in percutaneous vertebroplasty for osteoporotic compression fractures with or without intravertebral clefts. AJR Am J Roentgenol 193:W442–W445
Klazen CA, Lohle PN, De Vries J et al (2010) Vertebroplasty versus conservative treatment in acute osteoporotic vertebral compression fractures (Vertos II): an open-label randomised trial. Lancet 376:1085–1092
Yu CW, Hsu CY, Shih TT, Chen BB, Fu CJ (2007) Vertebral osteonecrosis: MR imaging findings and related changes on adjacent levels. AJNR Am J Neuroradiol 28:42–47
Lane JI, Maus TP, Wald JT, Thielen KR, Bobra S, Luetmer PH (2002) Intravertebral clefts opacified during vertebroplasty: pathogenesis, technical implications, and prognostic significance. AJNR Am J Neuroradiol 23:1642–1646
Tsoumakido G, Too CW, Koch G et al (2017) CIRSE guidelines on percutaneous vertebral augmentation. Cardiovasc Intervent Radiol 40:331–342
Einhorn TA (2005) The science of fracture healing. J Orthop Trauma 19:S4-6
Hsu WE, Su KC, Chen KH, Pan CC, Lu WH, Lee CH (2019) The evaluation of different radiological measurement parameters of the degree of collapse of the vertebral body in vertebral compression fractures. Appl Bionics Biomech 2019:1–5
Sousa CP, Dias IR, Lopez-Peña M et al (2015) Bone turnover markers for early detection of fracture healing disturbances: a review of the scientific literature. An Acad Bras Cienc 87:1049–1061
Leeming DJ, Alexandersen P, Karsdal MA, Qvist P, Schaller S, Tankó LB (2006) An update on biomarkers of bone turnover and their utility in biomedical research and clinical practice. Eur J Clin Pharmacol 62:781–792
Veitch SW, Findlay SC, Hamer AJ, Blumsohn A, Eastell R, Ingle BM (2006) Changes in bone mass and bone turnover following tibial shaft fracture. Osteoporos Int 17:364–372
Whitmarsh T, Humbert L, Del Río Barquero LM, Di Gregorio S, Frangi AF (2013) 3D reconstruction of the lumbar vertebrae from anteroposterior and lateral dual-energy X-ray absorptiometry. Med Image Anal 17:475–487
Finkelstein JS, Cleary RL, Butler JP et al (1994) A comparison of lateral versus anterior-posterior spine dual energy x-ray absorptiometry for the diagnosis of osteopenia. J Clin Endocrinol Metab 78:724–730
Larnach TA, Boyd SJ, Smart RC, Butler SP, Rohl PG, Diamond TH (1992) Reproducibility of lateral spine scans using dual energy X-ray absorptiometry. Calcif Tissue Int 51:255
Franck H, Munz M, Scherrer M, v Lilienfeld-Toal H, (1995) Lateral spine dual-energy X-ray absorptiometry bone mineral measurement with fan-beam design: effect of osteophytic calcifications on lateral and anteroposterior spine BMD. Rheumatol Int 15:151–154
Hart DJ, Mootoosamy I, Doyle DV, Spector TD (1994) The relationship between osteoarthritis and osteoporosis in the general population: the Chingford Study. Ann Rheum Dis 53:158–162
Orwoll ES, Oviatt SK, Mann T (1990) The impact of osteophytic and vascular calcifications on vertebral mineral density measurements in men. J Clin Endocrinol Metab 70:1202–1207
Pocock NA, Eberl S, Eisman JA et al (1987) Dual-photon bone densitometry in normal Australian women: a cross-sectional study. Med J Aust 146:293–297
Reid IR, Evans MC, Stapleton J (1992) Lateral spine densitometry is a more sensitive indicator of glucocorticoid-induced bone loss. J Bone Miner Res 7:1221–1225
Jergas M, Breitenseher M, Glüer CC et al (1995) Which vertebrae should be assessed using lateral dual-energy X-ray absorptiometry of the lumbar spine. Osteoporos Int 5:196–204
Nakamae T, Fujimoto Y, Yamada K et al (2017) Relationship between clinical symptoms of osteoporotic vertebral fracture with intravertebral cleft and radiographic findings. J Orthop Sci 22:201
Stäbler A, Schneider P, Link TM et al (1999) Intravertebral vacuum phenomenon following fractures: CT study on frequency and etiology. J Comput Assist Tomogr 23:976–980
Freedman BA, Heller JG (2009) Kummel disease: a not-so-rare complication of osteoporotic vertebral compression fractures. J Am Board Fam Med 22:75–78
Lafforgue P (2006) Pathophysiology and natural history of avascular necrosis of bone. Joint Bone Spine 73:500–507
Kim DY, Lee SH, Jang JS, Chung SK, Lee HY (2004) Intravertebral vacuum phenomenon in osteoporotic compression fracture: report of 67 cases with quantitative evaluation of intravertebral instability. J Neurosurg 100:24–31
Liu SH, Yang RS, al-Shaikh R, Lane JM (1995) Collagen in tendon, ligament, and bone healing. A current review. Clin Orthop Relat Res 1995:265–78
Kurdy NM (2000) Serology of abnormal fracture healing: the role of PIIINP, PICP, and BsALP. J Orthop Trauma 14:48
Lu C, Miclau T, Hu D et al (2005) Cellular basis for age-related changes in fracture repair. J Orthop Res 23:1300–1307
Acknowledgements
Techniques of specimen preparation and measurement were supported by the Pathology Laboratory of Shandong Provincial Hospital and Jinan Infectious Diseases Hospital.
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Dr. Jianmin Sun
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article
Statistics and biometry
No complex statistical methods were necessary for this paper
Informed consent
Written informed consent was obtained from all subjects (patients) in this study
Ethical approval
Institutional Review Board approval was obtained
Methodology
• retrospective
• randomised controlled trial
• performed at one institution
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Qi, H., Qi, J., Sun, Y. et al. Bone microarchitecture and metabolism in elderly male patients with signs of intravertebral cleft on MRI. Eur Radiol 32, 3931–3943 (2022). https://doi.org/10.1007/s00330-021-08458-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-021-08458-9