Abstract
Objective
The objective of this study was to analyze and compare the effects of different urate-lowering agents on testicular functions in men with gout in a clinical setting.
Methods
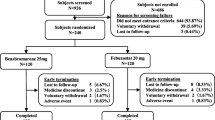
In this prospective cohort study (Clinical Trial Registration Number: NCT04213534), a total of 49 male patients aged 18–45 years with gout were enrolled. They were divided into three groups and received treatment with either allopurinol, febuxostat or benzbromarone for a duration of 3 months. Semen parameters, reproductive hormones and biochemical assessments were evaluated at baseline, month 1, and month 3.
Results
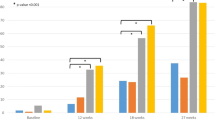
Overall, 40 individuals (81.6%) completed the follow-up visits. In allopurinol group, there were no significant differences in semen parameters from baseline to month 3. Most of sperm parameters in febuxostat group did not show notable changes, except for a decrease in sperm motility at month 3(33.6%, [22.9–54.3] vs 48.4%, [27.4–67.6], p = 0.033). However, the total motile sperm count did not differ significantly after febuxostat treatment. Surprisingly, administration of benzbromarone resulted in improved sperm concentration (37.19 M/mL, [29.6–69.92] vs 58.5 M/mL, [49.8–116.6], p = 0.001). There were no significant changes observed in sperm DNA integrity and reproductive hormones in the three groups from baseline to month 3. The incidence of adverse events did not differ significantly among the three groups as well.
Conclusion
This study is the first to demonstrate that urate-lowering agents, allopurinol and febuxostat, do not have clinically relevant negative effects on sperm quality and reproductive hormones in men with gout, and benzbromarone presents improving sperm concentration. Results provide important preliminary guidance for the development of reproductive health management guidelines for patients RCID with gout.


Similar content being viewed by others
Data availability
All data are available from the corresponding author on reasonable request.
References
Zhang J, Jin C, Ma B, Sun H, Chen Y, Zhong Y, Han C, Liu T, Li Y (2023) Global, regional and national burdens of gout in the young population from 1990 to 2019: a population-based study. RMD Open. https://doi.org/10.1136/rmdopen-2023-003025
Kim Y, Kang J, Kim GT (2018) Prevalence of hyperuricemia and its associated factors in the general Korean population: an analysis of a population-based nationally representative sample. Clin Rheumatol 37(9):2529–2538. https://doi.org/10.1007/s10067-018-4130-2
Wang X, Li X, Wang H, Chen M, Wen C, Huang L, Zhou M (2023) All-cause and specific mortality in patients with gout: a systematic review and meta-analysis. Semin Arthritis Rheum 63:152273. https://doi.org/10.1016/j.semarthrit.2023.152273
Perez-Garcia LF, Dolhain R, Vorstenbosch S, Bramer W, van Puijenbroek E, Hazes JMW, Te Winkel B (2020) The effect of paternal exposure to immunosuppressive drugs on sexual function, reproductive hormones, fertility, pregnancy and offspring outcomes: a systematic review. Hum Reprod Update 26(6):961–1001. https://doi.org/10.1093/humupd/dmaa022
Perez-Garcia LF, Röder E, Krijthe BP, Kranenburg-van Koppen LJ, van Adrichem R, Zirkzee E, Griffioen PH, Peeters K, Lin M, Struys EA, Jansen G, van Doorn MB, de Jonge R, Dohle GR, Dolhain RJ (2023) Is methotrexate safe for men with an immune-mediated inflammatory disease and an active desire to become a father? Results of a prospective cohort study (iFAME-MTX). Ann Rheum Dis 82(8):1068–1075. https://doi.org/10.1136/ard-2023-224032
Reinisch W, Hellstrom W, Dolhain R, Sikka S, Westhovens R, Mehta R, Ritter T, Seidler U, Golovchenko O, Simanenkov V, Garmish O, Jeka S, Moravcová R, Rajendran V, Le Brun FO, Arterburn S, Watkins TR, Besuyen R, Vanderschueren D (2023) Effects of filgotinib on semen parameters and sex hormones in male patients with inflammatory diseases: results from the phase 2, randomised, double-blind, placebo-controlled MANTA and MANTA-RAy studies. Ann Rheum Dis 82(8):1049–1058. https://doi.org/10.1136/ard-2023-224017
Weisshaar S, Litschauer B, Reichardt B, Gruber F, Leitner S, Sibinovic S, Kossmeier M, Wolzt M (2022) Cardiovascular risk and mortality in patients with hyperuricemia treated with febuxostat or allopurinol: a retrospective nation-wide cohort study in Austria 2014–2017. Rheumatol Int 42(9):1597–1603. https://doi.org/10.1007/s00296-022-05139-8
FitzGerald JD, Dalbeth N, Mikuls T, Brignardello-Petersen R, Guyatt G, Abeles AM, Gelber AC, Harrold LR, Khanna D, King C, Levy G, Libbey C, Mount D, Pillinger MH, Rosenthal A, Singh JA, Sims JE, Smith BJ, Wenger NS, Bae SS, Danve A, Khanna PP, Kim SC, Lenert A, Poon S, Qasim A, Sehra ST, Sharma TSK, Toprover M, Turgunbaev M, Zeng L, Zhang MA, Turner AS, Neogi T (2020) 2020 American college of rheumatology guideline for the management of Gout. Arthritis Care Res 72(6):744–760. https://doi.org/10.1002/acr.24180
Richette P, Doherty M, Pascual E, Barskova V, Becce F (2017) 2016 updated EULAR evidence-based recommendations for the management of gout. Ann Rheum Dis 76(1):29–42. https://doi.org/10.1136/annrheumdis-2016-209707
Perez-Ruiz F (2009) Treating to target: a strategy to cure gout. Rheumatology (Oxford, England) 48(Suppl 2):ii9–ii4. https://doi.org/10.1093/rheumatology/kep087
Sammaritano LR, Bermas BL, Chakravarty EE, Chambers C, Clowse MEB (2020) 2020 American college of rheumatology guideline for the management of reproductive health in rheumatic and musculoskeletal diseases. Arthritis Rheumatol 72(4):529–556. https://doi.org/10.1002/art.41191
Castrejon I, Toledano E, Rosario MP, Loza E, Pérez-Ruiz F, Carmona L (2015) Safety of allopurinol compared with other urate-lowering drugs in patients with gout: a systematic review and meta-analysis. Rheumatol Int 35(7):1127–1137. https://doi.org/10.1007/s00296-014-3189-6
Frampton JE (2015) Febuxostat: a review of its use in the treatment of hyperuricaemia in patients with gout. Drugs 75(4):427–438. https://doi.org/10.1007/s40265-015-0360-7
Kozenko M, Grynspan D, Oluyomi-Obi T, Sitar D, Elliott AM, Chodirker BN (2011) Potential teratogenic effects of allopurinol: a case report. Am J Med Genet Part A 155(9):2247–2252. https://doi.org/10.1002/ajmg.a.34139
Hoeltzenbein M, Stieler K, Panse M, Wacker E, Schaefer C (2013) Allopurinol use during pregnancy - outcome of 31 prospectively ascertained cases and a phenotype possibly indicative for teratogenicity. PLoS One 8(6):e66637. https://doi.org/10.1371/journal.pone.0066637
Nudell DM, Monoski MM, Lipshultz LI (2002) Common medications and drugs: how they affect male fertility. Urol Clinics N Am 29(4):965–973. https://doi.org/10.1016/s0094-0143(02)00079-4
Neogi T, Jansen TL, Dalbeth N, Fransen J, Schumacher HR, Berendsen D, Brown M, Choi H, Edwards NL, Janssens HJ, Lioté F, Naden RP, Nuki G, Ogdie A, Perez-Ruiz F, Saag K, Singh JA, Sundy JS, Tausche AK, Vaquez-Mellado J, Yarows SA, Taylor WJ (2015) 2015 Gout classification criteria: an American college of rheumatology/european league against rheumatism collaborative initiative. Ann Rheum Dis 74(10):1789–1798. https://doi.org/10.1136/annrheumdis-2015-208237
Cooper TG, Noonan E, von Eckardstein S, Auger J, Baker HW, Behre HM, Haugen TB, Kruger T, Wang C, Mbizvo MT, Vogelsong KM (2010) World Health Organization reference values for human semen characteristics. Hum Reprod Update 16(3):231–245. https://doi.org/10.1093/humupd/dmp048
Yü T (1982) The efficacy of colchicine prophylaxis in articular gout–a reappraisal after 20 years. Semin Arthritis Rheum 12(2):256–264. https://doi.org/10.1016/0049-0172(82)90065-8
Schreiber K, Frishman M, Russell MD, Dey M, Flint J, Allen A, Crossley A, Gayed M, Hodson K, Khamashta M, Moore L, Panchal S, Piper M, Reid C, Saxby K, Senvar N, Tosounidou S, van de Venne M, Warburton L, Williams D, Yee CS, Gordon C, Giles I (2023) Executive summary: british society for Rheumatology guideline on prescribing drugs in pregnancy and breastfeeding: comorbidity medications used in rheumatology practice. Rheumatology (Oxford) 62(4):1388–1397. https://doi.org/10.1093/rheumatology/keac559
Baskaran S, Finelli R, Agarwal A, Henkel R (2021) Diagnostic value of routine semen analysis in clinical andrology. Andrologia 53(2):e13614. https://doi.org/10.1111/and.13614
Benn CL, Dua P, Gurrell R, Loudon P, Pike A, Storer RI, Vangjeli C (2018) Physiology of hyperuricemia and urate-lowering treatments. Front Med 5:160. https://doi.org/10.3389/fmed.2018.00160
Kumagai A, Kodama H, Kumagai J, Fukuda J, Kawamura K, Tanikawa H, Sato N, Tanaka T (2002) Xanthine oxidase inhibitors suppress testicular germ cell apoptosis induced by experimental cryptorchidism. Mol Hum Reprod 8(2):118–123. https://doi.org/10.1093/molehr/8.2.118
Bozlu M (2005) Allopurinol provides long-term protection for experimentally induced testicular torsion in a rabbit model. BJU Int 96(4):686–687. https://doi.org/10.1111/j.1464-410X.2005.05788_4.x
Kadowaki D, Sakaguchi S, Miyamoto Y, Taguchi K, Muraya N, Narita Y, Sato K, Chuang VT, Maruyama T, Otagiri M, Hirata S (2015) Direct radical scavenging activity of benzbromarone provides beneficial antioxidant properties for hyperuricemia treatment. Biol Pharm Bull 38(3):487–492. https://doi.org/10.1248/bpb.b14-00514
Muraya N, Kadowaki D, Miyamura S, Kitamura K, Uchimura K, Narita Y, Miyamoto Y, Chuang VTG, Taguchi K, Maruyama T, Otagiri M, Hirata S (2018) Benzbromarone attenuates oxidative stress in angiotensin ii- and salt-induced hypertensive model rats. Oxid Med Cell Longev 2018:7635274. https://doi.org/10.1155/2018/7635274
Caliskan Z, Kucukgergin C, Aktan G, Kadioglu A, Ozdemirler G (2022) Evaluation of sperm DNA fragmentation in male infertility. Andrologia 54(11):e14587. https://doi.org/10.1111/and.14587
Malić Vončina S, Stenqvist A, Bungum M, Schyman T, Giwercman A (2021) Sperm DNA fragmentation index and cumulative live birth rate in a cohort of 2713 couples undergoing assisted reproduction treatment. Fertil Steril 116(6):1483–1490. https://doi.org/10.1016/j.fertnstert.2021.06.049
Yifu P, Lei Y, Shaoming L, Yujin G, Xingwang Z (2020) Sperm DNA fragmentation index with unexplained recurrent spontaneous abortion: a systematic review and meta-analysis. J Gynecol obstet Hum Reprod. https://doi.org/10.1016/j.jogoh.2020.101740
Speyer BE, Pizzey AR, Ranieri M, Joshi R, Delhanty JD, Serhal P (2010) Fall in implantation rates following ICSI with sperm with high DNA fragmentation. Hum Reprod (Oxford, England) 25(7):1609–1618. https://doi.org/10.1093/humrep/deq116
Misra DP, Agarwal V (2019) Real-world evidence in rheumatic diseases: relevance and lessons learnt. Rheumatol Int 39(3):403–416. https://doi.org/10.1007/s00296-019-04248-1
Landewé RBM (2021) The unsustainable bubble of disease-modifying antirheumatic drugs in rheumatology. Lancet Rheumatol 3(4):e306–e312. https://doi.org/10.1016/s2665-9913(21)00013-8
Ben-Chetrit E, Levy M (2003) Reproductive system in familial Mediterranean fever: an overview. Ann Rheum Dis 62(10):916–919. https://doi.org/10.1136/ard.62.10.916
Both T, van Laar JA, Bonte-Mineur F, van Hagen PM, van Daele PL (2012) Colchicine has no negative effect on fertility and pregnancy. Ned Tijdschr Geneeskd 156(12):A4196
Funding
This study was supported by the National Key Research & Developmental Program of China (2022YFC2702600), National Nature Science Foundation of China (No.82270066, No.82271634), Beijing Municipal Natural Science Foundation (No.7222264).
Author information
Authors and Affiliations
Contributions
CL, YW, and RM contributed equally to this work. All authors met the authorship criteria, they had a substantial contribution to the concept and design of the work (CL, ZZ, RM, HJ) or the acquisition (CL, ZZ, JZ, ZY, JZ, YJ, RL, DL, KH), analysis (YW, ZZ, CL.) or interpretation of data for the work (all authors) and were involved in revising a draft of this work, gave final approval of this version to be published. CL and ZZ had full access to all of the data in the study. All authors take responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding authors
Ethics declarations
Conflict of interest
The author declares that have no conflict of interest.
Ethical approval
Ethical approval was obtained from the Peking University Third Hospital Medical Science Research Ethics Committee (Protocol No: LM2019273, dated 9th April 2019). All participants provided written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, C., Wang, Y., Mu, R. et al. Urate-lowering agents do not have clinically relevant negative effects on sperm quality and reproductive hormones in men with gout: a prospective open-label cohort study. Rheumatol Int (2024). https://doi.org/10.1007/s00296-024-05572-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00296-024-05572-x