Abstract
Purpose
This study aimed to test the hypothesis that identifying the exact location of the most superior portion of the subscapularis tendon using magnetic resonance imaging (MRI) provides high diagnostic accuracy in detecting subscapularis tendon tears.
Methods
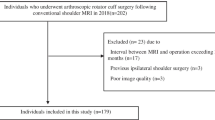
This study included 157 patients who underwent primary arthroscopic rotator cuff repair between 2014 and 2017. All patients underwent conventional 1.5-T MRI in our hospital, within 3 months before surgery. We retrospectively compared the diagnosis of subscapularis tendon tears using MRI based on an anatomical concept focusing on the superior-most insertion point of the subscapularis tendon with intraoperative arthroscopic findings.
Results
Subscapularis tendon tears were detected in 80 (51.0%) of the 157 patients during arthroscopic evaluation. The overall sensitivity, specificity, positive predictive value, negative predictive value, and accuracy of the MRI examination were 90, 83, 85, 89, and 87%, respectively. With a kappa score of 0.83, the concordance rate between the two raters was almost perfect (95% confidence interval, 0.75–0.92). The sensitivities of the oblique-sagittal and axial sequences were 84 and 79%, respectively.
Conclusions
Preoperative MRI evaluation focusing on the most superior portion of the subscapularis tendon demonstrated high diagnostic accuracy in detecting subscapularis tendon tears. To find the most superior portion of the subscapularis tendon tears, it was essential to check the slice at the level of the lesser tubercle tip and its adjacent slice. In addition, the combined observation of oblique-sagittal and axial sequences helped to detect subscapularis tendon tears with higher sensitivity.




Similar content being viewed by others
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Adams CR, Brady PC, Koo SS, Narbona P, Arrigoni P, Karnes GJ et al (2012) A systematic approach for diagnosing subscapularis tendon tears with preoperative magnetic resonance imaging scans. Arthroscopy 28:1592–1600. https://doi.org/10.1016/j.arthro.2012.04.142
Arai R, Sugaya H, Mochizuki T, Nimura A, Moriishi J, Akita K (2008) Subscapularis tendon tear: an anatomic and clinical investigation. Arthroscopy 24:997–1004. https://doi.org/10.1016/j.arthro.2008.04.076
Burkhart SS, Brady PC (2006) Arthroscopic subscapularis repair: surgical tips and pearls A to Z. Arthroscopy 22:1014–1027. https://doi.org/10.1016/j.arthro.2006.07.020
Deutsch A, Altchek DW, Veltri DM, Potter HG, Warren RF (1997) Traumatic tears of the subscapularis tendon: clinical diagnosis, magnetic resonance imaging findings, and operative treatment. Am J Sports Med 25:13–22. https://doi.org/10.1177/036354659702500104
Foad A, Wijdicks CA (2012) The accuracy of magnetic resonance imaging and magnetic resonance arthrogram versus arthroscopy in the diagnosis of subscapularis tendon injury. Arthroscopy 28:636–641. https://doi.org/10.1016/j.arthro.2011.10.006
Furukawa R, Morihara T, Arai Y, Ito H, Kida Y, Sukenari T et al (2014) Diagnostic accuracy of magnetic resonance imaging for subscapularis tendon tears using radial-slice magnetic resonance images. J Shoulder Elbow Surg 23:e283-290. https://doi.org/10.1016/j.jse.2014.03.011
Garavaglia G, Ufenast H, Taverna E (2011) The frequency of subscapularis tears in arthroscopic rotator cuff repairs: a retrospective study comparing magnetic resonance imaging and arthroscopic findings. Int J Shoulder Surg 5:90–94. https://doi.org/10.4103/0973-6042.91000
Hsu HC, Wu JJ, Jim YF, Chang CY, Lo WH, Yang DJ (1994) Calcific tendinitis and rotator cuff tearing: a clinical and radiographic study. J Shoulder Elbow Surg 3:159–164. https://doi.org/10.1016/S1058-2746(09)80095-5
Jung J-Y, Jee W-H, Chun C-W, Kim Y-S (2017) Diagnostic performance of MR arthrography with anterior trans-subscapularis versus posterior injection approach for subscapularis tendon tears at 3.0T. Eur Radiol 27:1303–1311. https://doi.org/10.1007/s00330-016-4467-3
Lafosse L, Jost B, Reiland Y, Audebert S, Toussaint B, Gobezie R (2007) Structural integrity and clinical outcomes after arthroscopic repair of isolated subscapularis tears. J Bone Joint Surg Am 89:1184–1193. https://doi.org/10.2106/JBJS.F.00007
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Lee JH, Yoon YC, Jung JY, Yoo JC (2015) Rotator cuff tears noncontrast MRI compared to MR arthrography. Skeletal Radiol 44:1745–1754. https://doi.org/10.1007/s00256-015-2228-z
Lin L, Yan H, Xiao J, He Z, Luo H, Cheng X et al (2016) The diagnostic value of magnetic resonance imaging for different types of subscapularis lesions. Knee Surg Sports Traumatol Arthrosc 24:2252–2258. https://doi.org/10.1007/s00167-014-3335-4
Malavolta EA, Assunção JH, Guglielmetti CLB, de Souza FF, Gracitelli MEC, Bordalo-Rodrigues M et al (2016) Accuracy of preoperative MRI in the diagnosis of subscapularis tears. Arch Orthop Trauma Surg 136:1425–1430. https://doi.org/10.1007/s00402-016-2507-8
Martetschläger F, Zampeli F, Tauber M, Habermeyer P, Leibe M (2021) A classification for partial subscapularis tendon tears. Knee Surg Sports Traumatol Arthrosc 29:275–283. https://doi.org/10.1007/s00167-020-05989-4
Peh WCG, Chan JHM (1998) The magic angle phenomenon in tendons: effect of varying the MR echo time. Br J Radiol 71:31–36. https://doi.org/10.1259/bjr.71.841.9534696
Ryu HY, Song SY, Yoo JC, Yun JY, Yoon YC (2016) Accuracy of sagittal oblique view in preoperative indirect magnetic resonance arthrography for diagnosis of tears involving the upper third of the subscapularis tendon. J Shoulder Elbow Surg 25:1944–1953. https://doi.org/10.1016/j.jse.2016.02.038
Sakurai G, Ozaki J, Tomita Y, Kondo T, Tamai S (1998) Incomplete tears of the subscapularis tendon associated with tears of the supraspinatus tendon: cadaveric and clinical studies. J Shoulder Elbow Surg 7:510–515. https://doi.org/10.1016/s1058-2746(98)90204-x
Tung GA, Yoo DC, Levine SM, Brody JM, Green A (2001) Subscapularis tendon tear: primary and associated signs on MRI. J Comput Assist Tomogr 25:417–424. https://doi.org/10.1097/00004728-200105000-00015
Acknowledgements
We thank Satoshi Takagi for his help in the initial preparation of data.
Funding
No funds, grants, or other support was received.
Author information
Authors and Affiliations
Contributions
SH: data extraction and analysis, and manuscript drafting. HY: Project planning, management of data analysis, and manuscript review. TM: manuscript review and editing. RA: Project planning and manuscript review. KA: Statistical analysis and manuscript review. AN: Management of data analysis, manuscript editing and review.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
Ethical approval for this study was granted following review by the Kawaguchi Kogyo General Hospital Institutional Review Board (#105321).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
Informed consent regarding publishing their data and photographs was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hasegawa, S., Yoshimura, H., Mochizuki, T. et al. High diagnostic accuracy of magnetic resonance imaging in detecting subscapularis tendon tears by focusing on the most superior portion of the subscapularis tendon. Surg Radiol Anat 45, 17–24 (2023). https://doi.org/10.1007/s00276-022-03059-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-022-03059-7