Abstract
Purpose
To evaluate the outcome of percutaneous lung biopsy (PLB) findings using cone-beam computed tomographic (CT) guidance (CBCT guidance) and compared to conventional biopsy guidance techniques.
Methods
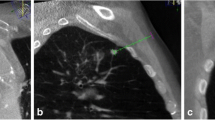
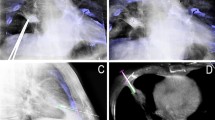
CBCT guidance is a stereotactic technique for needle interventions, combining 3D soft-tissue cone-beam CT, needle planning software, and real-time fluoroscopy. Between March 2007 and August 2010, we performed 84 Tru-Cut PLBs, where bronchoscopy did not provide histopathologic diagnosis. Mean patient age was 64.6 (range 24–85) years; 57 patients were men, and 25 were women. Records were prospectively collected for calculating sensitivity, specificity, positive predictive value, negative predictive value, and accuracy. We also registered fluoroscopy time, room time, interventional time, dose–area product (DAP), and complications. Procedures were divided into subgroups (e.g., location, size, operator).
Results
Mean lesion diameter was 32.5 (range 3.0–93.0) mm, and the mean number of samples per biopsy procedure was 3.2 (range 1–7). Mean fluoroscopy time was 161 (range 104–551) s, room time was 34 (range 15–79) min, mean DAP value was 25.9 (range 3.9–80.5) Gy·cm−2, and interventional time was 18 (range 5–65) min. Of 84 lesions, 70 were malignant (83.3%) and 14 were benign (16.7%). Seven (8.3%) of the biopsy samples were nondiagnostic. All nondiagnostic biopsied lesions proved to be malignant during surgical resection. The outcome for sensitivity, specificity, positive predictive value, negative predictive value, and accuracy was 90% (95% confidence interval [CI] 86–96), 100% (95% CI 82–100), 100% (95% CI 96–100), 66.7% (95% CI 55–83), and 91.7% (95% CI 86–96), respectively. Sixteen patients (19%) had minor and 2 (2.4%) had major complications.
Conclusion
CBCT guidance is an effective method for PLB, with results comparable to CT/CT fluoroscopy guidance.





Similar content being viewed by others
References
Herth FJF, Eberhardt R, Ernst A (2006) The future of bronchoscopy in diagnosing, staging and treatment of lung cancer. Respiratory 73:399–409
Sheth S, Harper UH, Stanley DB et al (1999) US guidance for thoracic biopsy: a valuable alternative to CT. Radiology 210:721–726
Diacon AH, Theron J, Shubert P et al (2007) Ultrasound-assisted transthoracic biopsy: fine needle aspiration or cutting-needle biopsy? Eur Respir J 29:357–362
Heck SL, Blom P, Berstad A (2006) Accuracy and complications in computed tomography fluoroscopy-guided needle biopsies of lung masses. Eur Radiol 16:1387–1392
Hiraki T, Mimura H, Gobara H et al (2009) CT fluoroscopy-guided biopsy of 1, 000 pulmonary lesions performed with 20-gauge coaxial cutting needles: diagnostic yield and risk factors for diagnostic failure. Chest 136:1612–1617
Cham MD, Lane ME, Henschke CI et al (2008) Lung biopsy: special techniques. Semin Respir Crit Care Med 29:335–349
Braak SJ, van Strijen MJL, van Leersum M et al (2010) Real-time 3D fluoroscopy guidance during needle interventions: technique, accuracy, and feasibility. AJR Am J Roentgenol 194:W445–W451
Gupta S, Wallace MJ, Cardella JF et al (2010) Quality improvement guidelines for percutaneous needle biopsy. J Vasc Interv Radiol 21:969–975
Duncan M, Wijesekera N, Padley S (2010) Interventional radiology of the thorax. Respirology 15:401–412
Jin KN, Park CM, Goo JM et al (2010) Initial experience of percutaneous transthoracic needle biopsy of lung nodules using C-arm cone-beam CT systems. Eur Radiol 20:2108–2115
Carlson SK, Felmlee JP, Bender CE et al (2005) CT fluoroscopy-guided biopsy of the lung or upper abdomen with a breath-hold monitoring and feedback system: a prospective randomized controlled clinical trial. Radiology 237:701–708
Schaefer PJ, Schaefer FKW, Heller M et al (2007) CT fluoroscopy-guided biopsy of small pulmonary and upper abdominal lesions: efficacy with a modified breathing technique. J Vasc Interv Radiol 18:1241–1248
Kim GR, Hur J, Lee SM et al (2011) CT fluoroscopy-guided lung biopsy versus conventional CT-guided lung biopsy: a prospective controlled study to assess radiation doses and diagnostic performance. Eur Radiol 21:232–239
Tsukada H, Satou T, Iwashima A et al (2000) Diagnostic accuracy of CT-guided automated needle biopsy of lung nodules. AJR Am J Roentgenol 175:239–243
Betsou S, Efstathopoulos EP, Katritsis D et al (1998) Patiënt radiation doses during cardiac catheterization procedures. Br J Radiol 71:634–639
Yamagami T, Kato T, Hiroto T et al (2006) Usefulness and limitation of manual aspiration immediately after pneumothorax complication interventional radiological procedures with the transthoracic approach. Cardiovasc Intervent Radiol 29:1027–1033
Froelich JJ, Ishaque N, Regn J et al (2002) Guidance of percutaneous pulmonary biopsies with real-time CT. Eur J Radiol 42:74–79
Moore EH (1998) Technical aspects of needle aspiration lung biopsy: a personal perspective. Radiology 208:303–318
Priola AM, Priola SM, Cataldi A et al (2007) Accuracy of CT-guided transthoracic needle biopsy of lung lesions: factors affecting diagnostic yield. Radiol Med 112:1142–1159
Laurent F, Latrabe V, Vergier B et al (2000) Percutaneous CT-guided biopsy of the lung: comparison between aspiration and automatic cutting needles using a coaxial technique. Cardiovasc Intervent Radiol 23:266–272
Moulton JS, Moore PT (1993) Coaxial percutaneous biopsy technique with automated biopsy devices: value in improving accuracy and negative predictive value. Radiology 186:515–522
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Braak, S.J., Herder, G.J.M., van Heesewijk, J.P.M. et al. Pulmonary Masses: Initial Results of Cone-beam CT Guidance with Needle Planning Software for Percutaneous Lung Biopsy. Cardiovasc Intervent Radiol 35, 1414–1421 (2012). https://doi.org/10.1007/s00270-011-0302-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-011-0302-z