Abstract
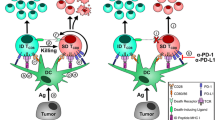
Identification of immunogenic tumor antigens, their corresponding T cell epitopes and the selection of effective adjuvants are prerequisites for developing effective cancer immunotherapies such as therapeutic vaccines. Murine double minute 2 (MDM2) is an E3 ubiquitin-protein ligase that negatively regulates tumor suppressor p53. Because MDM2 overexpression serves as a poor prognosis factor in various types of tumors, it would be beneficial to develop MDM2-targeted cancer vaccines. In this report, we identified an MDM2-derived peptide epitope (MDM232-46) that elicited antigen-specific and tumor-reactive CD4+ T cell responses. These CD4+ T cells directly killed tumor cells via granzyme B. MDM2 is expressed in head and neck cancer patients with poor prognosis, and the T cells that recognize this MDM2 peptide were present in these patients. Notably, Nutlin-3 (MDM2-p53 blocker), inhibited tumor cell proliferation, was shown to augment antitumor T cell responses by increasing MDM2 expression, HLA-class I and HLA-DR through class II transactivator (CIITA). These results suggest that the use of this MDM2 peptide as a therapeutic vaccine combined with MDM2 inhibitors could represent an effective immunologic strategy to treat cancer.







Similar content being viewed by others
Abbreviations
- APC:
-
Antigen-presenting cell
- CIITA:
-
Class II transactivator
- CTL:
-
CD8+ cytotoxic T lymphocyte
- DC:
-
Dendritic cell
- E:
-
T: Effector: Target
- FFPE:
-
Formalin fixed, paraffin embedded
- HNSCC:
-
Head and neck squamous cell carcinoma
- HTL:
-
CD4+ helper T lymphocyte
- ICI:
-
Immune checkpoint inhibitor
- mAb:
-
Monoclonal antibody
- MDM2:
-
Murine double minute 2
- MFI:
-
Mean fluorescence intensity
- PBMC:
-
Peripheral blood mononuclear cell
- TAA:
-
Tumor-associated antigen
References
Kumai T, Kobayashi H, Harabuchi Y, Celis E (2017) Peptide vaccines in cancer-old concept revisited. Curr Opin Immunol 45:1–7. https://doi.org/10.1016/j.coi.2016.11.001
Ott PA, Hu-Lieskovan S, Chmielowski B et al (2020) A phase Ib trial of personalized neoantigen therapy plus anti-PD-1 in patients with advanced melanoma, non-small cell lung cancer, or bladder cancer. Cell 183(347–62):e24. https://doi.org/10.1016/j.cell.2020.08.053
Dupont Jensen J, Laenkholm AV, Knoop A, Ewertz M, Bandaru R, Liu W, Hackl W, Barrett JC, Gardner H (2011) PIK3CA mutations may be discordant between primary and corresponding metastatic disease in breast cancer. Clin Cancer Res 17:667–677. https://doi.org/10.1158/1078-0432.CCR-10-1133
Ishibashi K, Kumai T, Ohkuri T et al (2016) Epigenetic modification augments the immunogenicity of human leukocyte antigen G serving as a tumor antigen for T cell-based immunotherapy. Oncoimmunology 5:e1169356. https://doi.org/10.1080/2162402X.2016.1169356
Kumai T, Lee S, Cho HI, Sultan H, Kobayashi H, Harabuchi Y, Celis E (2017) Optimization of peptide vaccines to induce robust antitumor CD4 T-cell responses. Cancer Immunol Res 5:72–83. https://doi.org/10.1158/2326-6066.CIR-16-0194
Nagato T, Celis E (2014) A novel combinatorial cancer immunotherapy: poly-IC and blockade of the PD-1/PD-L1 pathway. Oncoimmunology 3:e28440. https://doi.org/10.4161/onci.28440
Sultan H, Fesenkova VI, Addis D, Fan AE, Kumai T, Wu J, Salazar AM, Celis E (2017) Designing therapeutic cancer vaccines by mimicking viral infections. Cancer Immunol Immunother 66:203–213. https://doi.org/10.1007/s00262-016-1834-5
Sultan H, Kumai T, Nagato T, Wu J, Salazar AM, Celis E (2019) The route of administration dictates the immunogenicity of peptide-based cancer vaccines in mice. Cancer Immunol Immunother 68:455–466. https://doi.org/10.1007/s00262-018-02294-5
Kumai T, Ishibashi K, Oikawa K et al (2014) Induction of tumor-reactive T helper responses by a posttranslational modified epitope from tumor protein p53. Cancer Immunol Immunother 63:469–478. https://doi.org/10.1007/s00262-014-1533-z
Ohara K, Ohkuri T, Kumai T et al (2018) Targeting phosphorylated p53 to elicit tumor-reactive T helper responses against head and neck squamous cell carcinoma. Oncoimmunology 7:e1466771. https://doi.org/10.1080/2162402X.2018.1466771
Momand J, Zambetti GP, Olson DC, George D, Levine AJ (1992) The mdm-2 oncogene product forms a complex with the p53 protein and inhibits p53-mediated transactivation. Cell 69:1237–1245. https://doi.org/10.1016/0092-8674(92)90644-r
Haitel A, Wiener HG, Baethge U, Marberger M, Susani M (2000) mdm2 expression as a prognostic indicator in clear cell renal cell carcinoma: comparison with p53 overexpression and clinicopathological parameters. Clin Cancer Res 6:1840–1844
Park HS, Park JM, Park S, Cho J, Kim SI, Park BW (2014) Subcellular localization of Mdm2 expression and prognosis of breast cancer. Int J Clin Oncol 19:842–851. https://doi.org/10.1007/s10147-013-0639-1
Konopleva M, Martinelli G, Daver N, Papayannidis C, Wei A, Higgins B, Ott M, Mascarenhas J, Andreeff M (2020) MDM2 inhibition: an important step forward in cancer therapy. Leukemia 34:2858–2874. https://doi.org/10.1038/s41375-020-0949-z
Wang B, Niu D, Lai L, Ren EC (2013) p53 increases MHC class I expression by upregulating the endoplasmic reticulum aminopeptidase ERAP1. Nat Commun 4:2359. https://doi.org/10.1038/ncomms3359
Rammensee H, Bachmann J, Emmerich NP, Bachor OA, Stevanovic S (1999) SYFPEITHI: database for MHC ligands and peptide motifs. Immunogenetics 50:213–219. https://doi.org/10.1007/s002510050595
Vita R, Mahajan S, Overton JA, Dhanda SK, Martini S, Cantrell JR, Wheeler DK, Sette A, Peters B (2019) The Immune epitope database (IEDB): 2018 update. Nucleic Acids Res 47:D339–D343. https://doi.org/10.1093/nar/gky1006
Kobayashi H, Wood M, Song Y, Appella E, Celis E (2000) Defining promiscuous MHC class II helper T-cell epitopes for the HER2/neu tumor antigen. Cancer Res 60:5228–5236
Hirata-Nozaki Y, Ohkuri T, Ohara K et al (2019) PD-L1-specific helper T-cells exhibit effective antitumor responses: new strategy of cancer immunotherapy targeting PD-L1 in head and neck squamous cell carcinoma. J Transl Med 17:207. https://doi.org/10.1186/s12967-019-1957-5
Kumai T, Matsuda Y, Oikawa K, Aoki N, Kimura S, Harabuchi Y, Celis E, Kobayashi H (2013) EGFR inhibitors augment antitumour helper T-cell responses of HER family-specific immunotherapy. Br J Cancer 109:2155–2166. https://doi.org/10.1038/bjc.2013.577
Kumai T, Ohkuri T, Nagato T et al (2015) Targeting HER-3 to elicit antitumor helper T cells against head and neck squamous cell carcinoma. Sci Rep 5:16280. https://doi.org/10.1038/srep16280
Chrysovergis A, Papanikolaou V, Tsiambas E, Stavraka C, Ragos V, Peschos D, Psyrri A, Mastronikolis N, Kyrodimos E (2019) P53/MDM2 Co-expression in laryngeal squamous cell carcinoma based on digital image analysis. Anticancer Res 39:4137–4142. https://doi.org/10.21873/anticanres.13572
Digre A, Lindskog C (2021) The human protein atlas-spatial localization of the human proteome in health and disease. Protein Sci 30:218–233. https://doi.org/10.1002/pro.3987
Quezada SA, Simpson TR, Peggs KS et al (2010) Tumor-reactive CD4(+) T cells develop cytotoxic activity and eradicate large established melanoma after transfer into lymphopenic hosts. J Exp Med 207:637–650. https://doi.org/10.1084/jem.20091918
Ramirez F, Ghani Y, Stauss H (2004) Incomplete tolerance to the tumour-associated antigen MDM2. Int Immunol 16:327–334. https://doi.org/10.1093/intimm/dxh040
Mayr C, Bund D, Schlee M, Bamberger M, Kofler DM, Hallek M, Wendtner CM (2006) MDM2 is recognized as a tumor-associated antigen in chronic lymphocytic leukemia by CD8+ autologous T lymphocytes. Exp Hematol 34:44–53. https://doi.org/10.1016/j.exphem.2005.09.016
Janssen EM, Droin NM, Lemmens EE, Pinkoski MJ, Bensinger SJ, Ehst BD, Griffith TS, Green DR, Schoenberger SP (2005) CD4+ T-cell help controls CD8+ T-cell memory via TRAIL-mediated activation-induced cell death. Nature 434:88–93. https://doi.org/10.1038/nature03337
Alspach E, Lussier DM, Miceli AP et al (2019) MHC-II neoantigens shape tumour immunity and response to immunotherapy. Nature 574:696–701. https://doi.org/10.1038/s41586-019-1671-8
Inderberg EM, Walchli S (2020) Long-term surviving cancer patients as a source of therapeutic TCR. Cancer Immunol Immunother 69:859–865. https://doi.org/10.1007/s00262-019-02468-9
Kumai T, Fan A, Harabuchi Y, Celis E (2017) Cancer immunotherapy: moving forward with peptide T cell vaccines. Curr Opin Immunol 47:57–63. https://doi.org/10.1016/j.coi.2017.07.003
Lukashchuk N, Vousden KH (2007) Ubiquitination and degradation of mutant p53. Mol Cell Biol 27:8284–8295. https://doi.org/10.1128/MCB.00050-07
Moll UM, Petrenko O (2003) The MDM2-p53 interaction. Mol Cancer Res 1:1001–1008
Cordon-Cardo C, Latres E, Drobnjak M et al (1994) Molecular abnormalities of mdm2 and p53 genes in adult soft tissue sarcomas. Cancer Res 54:794–799
Jeay S, Ferretti S, Holzer P et al (2018) Dose and schedule determine distinct molecular mechanisms underlying the efficacy of the p53-MDM2 inhibitor HDM201. Cancer Res 78:6257–6267. https://doi.org/10.1158/0008-5472.CAN-18-0338
Zhao Y, Aguilar A, Bernard D, Wang S (2015) Small-molecule inhibitors of the MDM2-p53 protein-protein interaction (MDM2 Inhibitors) in clinical trials for cancer treatment. J Med Chem 58:1038–1052. https://doi.org/10.1021/jm501092z
Schuler PJ, Harasymczuk M, Visus C et al (2014) Phase I dendritic cell p53 peptide vaccine for head and neck cancer. Clin Cancer Res 20:2433–2444. https://doi.org/10.1158/1078-0432.CCR-13-2617
Jeay S, Gaulis S, Ferretti S et al (2015) A distinct p53 target gene set predicts for response to the selective p53-HDM2 inhibitor NVP-CGM097. Elife. https://doi.org/10.7554/eLife.06498
Guo G, Yu M, Xiao W, Celis E, Cui Y (2017) Local activation of p53 in the tumor microenvironment overcomes immune suppression and enhances antitumor immunity. Cancer Res 77:2292–2305. https://doi.org/10.1158/0008-5472.CAN-16-2832
Pollack BP, Sapkota B, Cartee TV (2011) Epidermal growth factor receptor inhibition augments the expression of MHC class I and II genes. Clin Cancer Res 17:4400–4413. https://doi.org/10.1158/1078-0432.CCR-10-3283
Luo N, Formisano L, Gonzalez-Ericsson PI et al (2018) Melanoma response to anti-PD-L1 immunotherapy requires JAK1 signaling, but not JAK2. Oncoimmunology 7:e1438106. https://doi.org/10.1080/2162402X.2018.1438106
Kato S, Goodman A, Walavalkar V, Barkauskas DA, Sharabi A, Kurzrock R (2017) Hyperprogressors after immunotherapy: analysis of genomic alterations associated with accelerated growth rate. Clin Cancer Res 23:4242–4250. https://doi.org/10.1158/1078-0432.CCR-16-3133
Fang W, Zhou H, Shen J, Li J, Zhang Y, Hong S, Zhang L (2020) MDM2/4 amplification predicts poor response to immune checkpoint inhibitors: a pan-cancer analysis. ESMO Open. https://doi.org/10.1136/esmoopen-2019-000614
Sahin I, Zhang S, Navaraj A, Zhou L, Dizon D, Safran H, El-Deiry WS (2020) AMG-232 sensitizes high MDM2-expressing tumor cells to T-cell-mediated killing. Cell Death Discov 6:57. https://doi.org/10.1038/s41420-020-0292-1
Fang DD, Tang Q, Kong Y et al (2019) MDM2 inhibitor APG-115 synergizes with PD-1 blockade through enhancing antitumor immunity in the tumor microenvironment. J Immunother Cancer 7:327. https://doi.org/10.1186/s40425-019-0750-6
Veneziani I, Infante P, Ferretti E et al (2020) Nutlin-3a enhances natural killer cell-mediated killing of neuroblastoma by restoring p53-dependent expression of ligands for NKG2D and DNAM-1 receptors. Cancer Immunol Res. https://doi.org/10.1158/2326-6066.CIR-20-0313
Acknowledgements
The authors also thank Dr. Hajime Kamada (Hokuto Social Medical Corporation) for his excellent suggestions for the manuscript
Funding
This work was supported by JSPS KAKENHI Grant Number 20K209724.
Author information
Authors and Affiliations
Contributions
MK, TK, RH, HY, HK, RW, TN and KO took part in acquisition, analysis and interpretation of data. KK, MT and AKa involved in statistical analysis of data. TO, AKo, HK participated in material support. TK, TH and YH involved in development of methodology. TK took part in conception, design and supervision of the study. MK and TK involved in writing of the paper. TK, YH and EC participated in review of the paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no potential conflicts of interest
Availability of data and material
All data relevant to the study are included in the article or uploaded as supplementary information
Ethics approval, consent to participate and consent for publication
All experiments were approved by the institutional ethics committee on the Asahikawa Medical University (#16217). The study was conducted ethically in accordance with the World Medical Association Declaration of Helsinki. The patients have given their written informed consent to participate and publish their case.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
262_2021_2940_MOESM1_ESM.pptx
Supplementary Table S1: Correlations between MDM2 expression and clinical characteristics in HNSCC patients. The data were analyzed using Fisher’s exact test.
Supplementary Figure S1:MDM2 inhibitor reduced the proliferation of HNSCC cells in a dose-dependent manner. Error bars indicate standard deviations of triplicates.
Supplementary Figure S2: MDM2 inhibitor (Nutlin-3, 10μM) upregulated MDM2 expression in HNSCC cell lines.
Supplementary Figure S3: Expression levels of EGFR in HNSCC cell lines co-cultured with Nultin-3 were evaluated by flow cytometry. Left panels show representative data of flow cytometry. Black: isotype control, blue: EGFR on untreated tumor cell lines, red: EGFR on tumor cell lines treated with Nutlin-3 (10µM). Right panels show averages values of mean fluorescence intensity (MFI). (***<0.001, Student’s t test).
Supplementary Figure S4: Kaplan–Meier curves show the relationship between MDM2 expression and overall survival in HNSCC patients. Statistical difference was calculated using log-rank test. Kaplan–Meier analysis was performed with GraphPad Prism 8.
Supplementary Figure S5: Expression levels of PD-L1 in HNSCC cell lines co-cultured with Nultin-3 were evaluated by flow cytometry. Left panels show representative data of flow cytometry. Black: isotype control, blue: PD-L1 on untreated tumor cell lines, red: PD-L1 on tumor cell lines treated with Nutlin-3 (10µM). Right panels show averages values of mean fluorescence intensity (MFI). (***<0.001, Student’s t test).
Supplementary file1 (PPTX 842 kb)
Rights and permissions
About this article
Cite this article
Kono, M., Kumai, T., Hayashi, R. et al. Interruption of MDM2 signaling augments MDM2-targeted T cell-based antitumor immunotherapy through antigen-presenting machinery. Cancer Immunol Immunother 70, 3421–3434 (2021). https://doi.org/10.1007/s00262-021-02940-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-021-02940-5