Abstract
Purpose
Focal nodular hyperplasia (FNH) is commonly found in females of reproductive age. In males, the diagnosis is made more cautiously due to its lower incidence and higher incidence of hepatocellular carcinoma, which can have overlapping imaging features. Follow-up or biopsy is sometimes required. This retrospective study aims to assess management of suspected FNH in male adult patients at our institution over a 10-year period.
Methods
Male adults (≥ 18 years) suspected of having FNH from January 2010—June 2020 were identified using a departmental radiology information system search. Data was collected from radiology reports and patient pathway manager.
Results
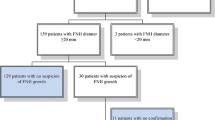
Of 342 patients with suspected FNH, 62 were male (18.1%; F:M of 4.5:1). We only included patients investigated and followed up by MRI, total of 57 patients. Median age was 40 years (range 18–74 years). Background liver disease present in 21/57 (36.8%), majority with hepatic steatosis. Average number of lesions per patient 1.7. 22/57 (38.6%) had at least one MRI follow-up using liver-specific contrast with 7 lesions demonstrating variation in size (range growth: -3.27 mm/year to + 4 mm/year). In 7 cases, MRI was not definitive; 6 required biopsy and 1 resection. Only 2/7 demonstrated malignancy. Of the total 57 patients, 6 have deceased and none due to a misdiagnosed or mismanaged hepatic lesion.
Conclusion
FNH is relatively uncommon in males, however, our data suggests that lesions with typical MRI characteristics do not require follow-up and diagnosis can be made confidently, similar to females. Any atypical features should prompt a biopsy.
Graphical abstract





Similar content being viewed by others
References
Vilgrain V, Uzan F, Brancatelli G et al (2003) Prevalence of hepatic hemangioma in patients with focal nodular hyperplasia: MR imaging analysis. Radiology 229:75–79
Bröker MEE, Klompenhouwer AJ, Gaspersz MP, Alleleyn AME, Dwarkasing RS, Pieters IC, de Man RA, IJzermans JNM. Growth of Focal Nodular Hyperplasia is Not a Reason for Surgical Intervention, but Patients Should be Referred to a Tertiary Referral Centre. World J Surg. 2018 May;42(5):1506-1513.
Craig JR, Peters RL, Edmondson HA. Tumors of the liver and intrahepatic bile ducts. In: Armed Forces Institute of Pathology, editor. Atlas of tumor pathology, second series fascicle. Washington: Armed Forces Institute of Pathology; 1989. p. 26.
Vilgrain V. Focal nodular hyperplasia. Eur J Radiol. 2006 May;58(2):236-45. doi: https://doi.org/10.1016/j.ejrad.2005.11.043. Epub 2006 Jan 18. PMID: 16414229.
Nguyen BN, Fl´ejou JF, Terris B, Belghiti J, Degott C. Focal nodular hyperplasia of the liver: a comprehensive pathologic study of 305 lesions and recognition of new histologic forms. Am J Surg Pathol 1999;23:1441–54.
Rebouissou S, Bioulac-Sage P, Zucman-Rossi J. Molecular pathogenesis of focal nodular hyperplasia and hepatocellular adenoma. J Hepatol. 2008;48:163–170
Vilgrain V (2006) Focal nodular hyperplasia. Eur J Radiol 58:236–245
Luciani A, Kobeiter H, Maison P et al (2002) Focal nodular hyperplasia of the liver in men: is presentation the same in men and women? Gut 50:877–880
Kim MJ, Lim HK, Kim SH, et al. Evaluation of hepatic focal nodular hyperplasia with contrast-enhanced gray scale harmonic sonography: initial experience. J Ultrasound Med 2004;23:297–305.
Dill-Macky MJ, Burns PN, Khalili K, Wilson SR. Focal hepatic masses: enhancement patterns with SH U 508A and pulse inversion US. Radiology 2002;222:95e102.
Bartolotta TV, Taibbi A, Brancatelli G, Matranga D, Tumbarello M, Midiri M, Lagalla R. Imaging findings of hepatic focal nodular hyperplasia in men and women: are they really different? Radiol Med. 2014 Apr;119(4):222-30.
Hamada K, Saitoh S, Nishino N, Fukushima D, Techigawara K, Koyanagi R, Horikawa Y, Shiwa Y, Sakuma H, Kondo F. An elderly man with progressive focal nodular hyperplasia. Clin J Gastroenterol. 2020 Jun;13(3):413-420.
Fujita N, Nishie A, Asayama Y, Ishigami K, Ushijima Y, Kakihara D, Nakayama T, Morita K, Ishimatsu K, Honda H. Hyperintense Liver Masses at Hepatobiliary Phase Gadoxetic Acid-enhanced MRI: Imaging Appearances and Clinical Importance. Radiographics. 2020 Jan-Feb;40(1):72-94.
Quaglia A, Tibballs J, Grasso A et al. Focal nodular hyperplasia-like areas in cirrhosis. Histopathology 2003; 42(1):14–21.
Ronot M, Bahrami S, Calderaro J, et al. Hepatocellular adenomas: accuracy of magnetic resonance imaging and liver biopsy in subtype classification. Hepatology 2011; 53: 1182–91.
Park MJ, Kim YK, Lee MW, Lee WJ, Kim YS, Kim SH, Choi D, Rhim H. Small hepatocellular carcinomas: improved sensitivity by combining gadoxetic acid-enhanced and diffusion-weighted MR imaging patterns. Radiology. 2012 Sep;264(3):761-70.
Grazioli L, Bondioni MP, Haradome H, et al. Hepatocellular adenoma and focal nodular hyperplasia: value of gadoxetic acid-enhanced MR imaging in differential diagnosis. Radiology 2012; 262: 520–9.
Kierans AS, Kang SK, Rosenkrantz AB. The Diagnostic Performance of Dynamic Contrast-enhanced MR Imaging for Detection of Small Hepatocellular Carcinoma Measuring Up to 2 cm: A Meta-Analysis. Radiology. 2016 Jan;278(1):82-94.
Kogita S, Imai Y, Okada M, et al. Gd-EOB-DTPAenhanced magnetic resonance images of hepatocellular carcinoma: correlation with histological grading and portal blood flow. Eur Radiol 2010; 10:2405–2413
Lee MH, Kim SH, Park MJ, Park CK, Rhim H. Gadoxetic acid-enhanced hepatobiliary phase MRI and high-b-value diffusion-weighted imaging to distinguish well-differentiated hepatocellular carcinomas from benign nodules in patients with chronic liver disease. AJR Am J Roentgenol. 2011 Nov;197(5):W868-75.
Ueno A, Masugi Y, Yamazaki K, Komuta M, Effendi K, Tanami Y, et al. OATP1B3 expression is strongly associated with Wnt/β-catenin signalling and represents the transporter of gadoxetic acid in hepatocellular carcinoma. J Hepatol. 2014;61:1080–1087.
Ba-Ssalamah A, Antunes C, Feier D, Bastati N, Hodge JC, Stift J, Cipriano MA, Wrba F, Trauner M, Herold CJ, Caseiro-Alves F. Morphologic and Molecular Features of Hepatocellular Adenoma with Gadoxetic Acid-enhanced MR Imaging. Radiology. 2015 Oct;277(1):104-13. doi: https://doi.org/10.1148/radiol.2015142366. Epub 2015 May 18. PMID: 25985059.
Zech CJ, Grazioli L, Breuer J, Reiser MF, Schoenberg SO. Diagnostic performance and description of morphological features of focal nodular hyperplasia in Gd-EOB-DTPAenhanced liver magnetic resonance imaging: results of a multicenter trial. Invest Radiol 2008; 43: 504–11.
Kim YY, Park MS, Aljoqiman KS, Choi JY, Kim MJ. Gadoxetic acid-enhanced magnetic resonance imaging: Hepatocellular carcinoma and mimickers. Clin Mol Hepatol. 2019;25(3):223-233.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to disclose.
Ethical approval
Institutional Review Board approval was not required due to the retrospective nature of this study.
Informed consent
Written informed consent was not required due to the retrospective nature of this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Corallo, C., Bell, J., Laverty, A. et al. Suspected focal nodular hyperplasia in male adults: 10-year experience from a large liver centre. Abdom Radiol 48, 2292–2301 (2023). https://doi.org/10.1007/s00261-023-03896-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-023-03896-z