Abstract
Introduction
Experimental models of osteoporosis in rabbits are useful to investigate anabolic agents because this animal has a fast bone turnover with predominant remodelling over the modelling processes. For that purpose, it is necessary to characterize the densitometric values of each type of bony tissue.
Objective
To determine areal bone mass measurement in the spine and in trabecular, cortical and subchondral bone of the knee in healthy and osteoporotic rabbits.
Design
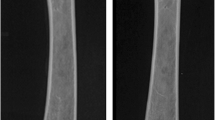
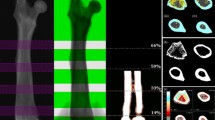
Bone mineral content and bone mineral density were measured in lumbar spine, global knee, and subchondral and cortical bone of the knee with dual energy X-ray absorptiometry using a Hologic QDR-1000/W densitometer in 29 skeletally mature female healthy New Zealand rabbits. Ten rabbits underwent triplicate scans for evaluation of the effect of repositioning. Osteoporosis was experimentally induced in 15 rabbits by bilateral ovariectomy and postoperative corticosteroid treatment for 4 weeks. Identical dual energy X-ray absorptiometry (DXA) studies were performed thereafter.
Results
Mean values of bone mineral content at the lumbar spine, global knee, subchondral bone and cortical tibial metaphysis were: 1934±217 mg, 878±83 mg, 149±14 mg and 29±7.0 mg, respectively. The mean values of bone mineral density at the same regions were: 298±24 mg/cm2, 455±32 mg/cm2, 617±60 mg/cm2 and 678±163 mg/cm2, respectively. Bone mineral content and bone density of healthy rabbits followed a normal distribution at the four skeletal regions studied. Precision after triplicate repositioning yielded a coefficient of variation ranging from 2.6% to 3.8%. The least significant change ranged between 7.3% and 10.7%. Bone mineral density measured at the four different skeletal regions correlated significantly. Bone mineral density in osteoporotic rabbits was significantly lower in the four regions studied than that in controls, rendering a T-score of, respectively, −2.0±1.1 in the lumbar spine, −2.2±2.1 in the global knee, −1.9±0.6 in the subchondral bone, and −5.7±3.1 in the cortical tibia (P<0.05).
Conclusions
DXA is a reliable and precise method to evaluate the bone mass in rabbits. Our results also suggest that subchondral bone is a bone of mixed densitometric characteristics with marked cortical bone predominance.



Similar content being viewed by others
References
Turner AS. Animal models of osteoporosis—necessity and limitations. Eur Cell Mater 2001;1:66–81
Turner RT, Maran A, Lotinun S, et al. Animal models for osteoporosis. Rev Endocr Metab Disord 2001;2:117–27
Bellino FL. Non-primate animal models of menopause: workshop report. Menopause 2000;7:14–24
Kimmel DB. Animal models for in vivo experimentation in osteoporosis research. In: Marcus R, Feldman D, Kelsey J, editors. Osteoporosis, vol 2. San Diego, California: Academic Press; 2001. pp. 29–47
Thompson DD, Simmons HA, Pirie CM, Ke HZ. FDA Guidelines and animal models for osteoporosis. Bone 1995;17 Suppl 4:125S–33S
Wronski TJ, Lowry PL, Walsh CC, Ignaszewski LA. Skeletal alterations in ovariectomized rats. Calcif Tissue Int 1985;37:324–8
Wronski TJ, Walsh CC, Ignaszewski LA. Histologic evidence for osteopenia and increased bone turnover in ovariectomized rats. Bone 1986;7:119–23
Wronski TJ, Yen CF. The ovariectomized rat as an animal model for postmenopausal bone loss. Cell Mater 1992;1 Suppl 1:69–74
Kalu DN. The ovariectomized rat as a model of postmenopausal osteopenia. Bone Miner 1991;15:175–91
Frost HM, Jee WSS. On the rat model of human osteopenia and osteoporoses. Bone Miner 1992;18:227–36
Rodgers JB, Mounier-Faugere MC, Malluche H. Animal models for the study of bone loss after cessation of ovarian functions. Bone 1993;14:369––77
Mosekilde Li. Assessing bone quality—animal models in preclinical osteoporosis research. Bone 1995;17 Suppl 4:343S–52S
Gilsanz V, Roe TF, Gibbens DT, et al. Effect of sex steroids on peak bone density of growing rabbits. Am J Physiol 1988;255:E416–E21
Wu DD, Boyd RD, Fix TJ, Burr DB. Regional patterns of bone loss and altered bone remodelling in response to calcium deprivation in laboratory rabbits. Calcif Tissue Int 1990;47:18–23
Newman E, Turner AS, Wark JD. The potential of sheep for the study of osteopenia: current status and comparison with other animal models. Bone 1995;16:277S–84S
Lindgren JU, DeLuca HF, Mazess RB. Effects of 1,25(OH)2D3 on bone tissue in the rabbit: studies on fracture healing, disuse osteoporosis, and prednisone osteoporosis. Calcif Tissue Int 1984;35:591––5
Griffin MG, Kimble R, Hopfer W, Pacifici R. Dual-energy X-ray absorptiometry of the rat: accuracy, precision and measurement of bone loss. J Bone Min Res 1993;8:795–800
Casez JP, Muehlbauer RC, Lippuner K, Kelly T, Fleisch H, Jaeger P. Dual-energy X-ray absorptiometry for measuring total bone mineral content in the rat: study of accuracy and precision. Bone Miner 1994;26:61–8
Yamauchi H, Kushida K, Yamazaki K, Inoue T. Assessment of spine bone mineral density in ovariectomized rats using DXA. J Bone Miner Res 1995;10:1033–9
Petersen MM, Nielsen PK, Lewin E, Olgaard K. Dual energy X-ray absorptiometry in small rats with low bone mineral density. Calcif Tissue Int 2000;67:455–9
Southard TE, Southard KA, Krizan KE, et al. Mandibular bone density and fractal dimension in rabbits with induced osteoporosis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2000;89:244–9
Cao T, Shirota T, Yamazaki M, Ohno K, Michi KI. Bone mineral density in mandibles of ovariectomized rabbits. Clin Oral Implants Res 2001;12:604–8
Mori H, Manabe M, Kurachi Y, Nagumo M. Osteointegration of dental implants in rabbit bone with low mineral density. J Oral Maxillofac Surg 1997;55:351–61
Cao T, Shirota T, Ohno K, Michi KI. Mineralized bone loss in partially edentulous trabeculae of ovariectomized rabbit mandibles. J Periodontal Res 2004;39:37–41
Dequeker J. The relationship between osteoporosis and osteoarthritis. Clin Rheum Dis 1985;11:271–96
Norris SA, Pettifor JM, Gray DA, Biscardi A, Buffenstein R. Validation and application of dual-energy X-ray absorptiometry to measure bone mineral density in rabbit vertebrae. J Clin Densitom 2000;3:49–55
Pogrund H, Rutenberg M, Makin M, Robin GC, Steinberg R, Bloom R. Osteoarthritis of the hand and osteoporosis. Clin Orthop Relat Res 1986;203:239–43
Hart DJ, Mootoosamy I, Doyle DV, Spector TD. The relationship between osteoarthritis and osteoporosis in the general population: the Chingford Study. Ann Rheum Dis 1994;53:158–62
Sambrook P, Naganathan V. What is the relationship between osteoarthritis and osteoporosis? Bailliere’s Clin Rheumatol 1997;11:695–710
Verstraeten A, van Ermen H, Haghebaert G, Nijs J, Geusens P, Dequeker J. Osteoarthrosis retards the development of osteoporosis. Clin Orthop Relat Res 1991;264:169–77
Grynpas MD, Alpert B, Katz I, Lieberman I, Pritzker KP. Subchondral bone in osteoarthritis. Calcif Tissue Int 1991;49:20–6
Benito MJ, Sánchez-Pernaute O, López Armada MJ, et al. Cyclosporin A prevents the histologic damage of antigen arthritis without inducing fibrosis. Arthritis Rheum 2000;43:311–9
Messner K, Fahlgren A, Ross I, Andersson B. Simultaneous changes in bone mineral density and articular cartilage in a rabbit meniscectomy model of knee osteoarthrosis. Osteoarthritis Cartilage 2000;8:197–206
Glueer CC, Blake G, Lu Y, Blunt BA, Jergas M, Genant HK. Accurate assessment of precision errors: how to measure the reproducibility of bone densitometry techniques. Osteoporos Int 1995;5:262–70
Eberhardt AW, Yeager-Jones A, Blair HC. Regional trabecular bone matrix degeneration and osteocyte death in femora of glucocorticoid-treated rabbits. Endocrinology 2001;142:1333–40
Kaplan HM, Timmons EH. The rabbit. A model for the principles of mammalian physiology and surgery. New York: Academic Press; 1979
Dupont WD, Plummer WD. Power and sample size calculations: a review and computer program. Control Clin Trials 1990;11:116–28
Simon MR. The rat as an animal for the study of senile idiopathic osteoporosis. Acta Anat 1984;119:248–50
Grardel B, Sutter B, Flautre B, Viguier E, Lavaste F, Hardouin P. Effects of corticosteroids on skeletal growth in rabbits evaluated by dual-photon absorptiometry, microscopic connectivity and vertebral compressive strength. Osteoporos Int 1994;4:204–10
Gala-Paniagua J, Díaz Curiel M, De la Piedra Gordo C, Castilla Reparaz C, Torralbo García M. Bone mass assessment in rats by dual energy X-ray absorptiometry. Br J Radiol 1998;71:754–8
Shipp CC, Berger PS, Deehr MS, Dawson-Hughes B. Precision of dual photon absorptiometry. Calcif Tissue Int 1988;42:287–92
Grier SJ, Turner AS, Alvis MR. The use of dual-energy x-ray absorptiometry in animals. Invest Radiol 1996;31:50–62
Sartoris DJ, Resnick D. Current and innovative methods for noninvasive bone densitometry. Radiol Clin North Am 1990;28:257–78
Lang P, Steiger P, Faulkner K, Glueer CC, Genant HK. Osteoporosis. Current techniques and recent developments in quantitative bone densitometry. Radiol Clin North Am 1991;29:49–76
Guglielmi G, Glueer CC, Majumdar S, Blunt BA, Genant HK. Current methods and advances in bone densitometry. Eur Radiol 1995;5:129–39
Hartke JR. Non-primate models of osteoporosis. Lab Anim Sci 1998;48:623–9
Schmidt C, Priemel M, Kohler T, et al. Precision and accuracy of peripheral quantitative computed tomography (pQCT) in the mouse skeleton compared with histology and microcomputed tomography (μCT). J Bone Miner Res 2003;18:1486–96
Veitch SW, Findlay SC, Ingle BM, et al. Accuracy and precision of peripheral quantitative computed tomography measurements at the tibial metaphysis. J Clin Densitom 2004;7:209–17
Rozenberg S, Vandromme J, Neve J, et al. Precision and accuracy of in-vivo bone mineral measurement in rats using dual-energy X-ray absorptiometry. Osteoporos Int 1995;5:47–53
Jayo MJ, Rankin SE, Weaver DS, Carlson CS, Clarkson TB. Accuracy and precision of lumbar bone mineral content by dual-energy X-ray absorptiometry in live female monkeys. Calcif Tissue Int 1991;49:438–40
Turner AS, Mallinckrodt CH, Alvis MR, Bryant HU. Dual-energy X-ray absorptiometry in sheep: experiences with in vivo and ex vivo studies. Bone 1995;17 Suppl 4:381S–7S
Faulkner KG, Glueer CC, Estilo M, Genant HK. Cross-calibration of DXA equipment: upgrading from Hologic QDR 1000/W to QDR 2000. Calcif Tissue Int 1993;52:79–89
Barthe N, Braillon P, Ducassou D, Basse-Cathalinat B. Comparison of two Hologic DXA systems (QDR 1000 and QDR 4500/A). Br J Radiol 1997;70:728–39
Dal Mas I, Biscardi A, Ripamonti U. Comparison of two Hologic DXA systems (QDR 1000 and QDR 4500/A for in vivo bone mass measurement in the baboon (Papio ursinus). J Clin Densitom 2002;5:313–8
Burr DB. Anatomy and physiology of the mineralized tissues: role in the pathogenesis of osteoarthritis. Osteoarthritis Cartilage 2004;12:S20–S30
Sievanen H, Oja P, Vuori I. Precision of dual-energy X-ray absorptiometry in determining bone mineral density and content of various skeletal sites. J Nucl Med 1992;33:1137–42
Casez JP, Troendle A, Lippuner K, Jaeger P. Bone mineral density at the tibia using dual-energy X-ray absorptiometry in normal women and in patients with vertebral osteoporosis or primary hyperparathyroidism. J Bone Miner Res 1994;9:1851–7
Kaartinen E. A histomorphometric study of rabbit tibiofibular bones after rigid intramedullary nailing. Ann Chir Gynaecol 1993;82:189–93
Acknowledgements
The authors wish to thank Dr. C. de la Piedra Gordo, from the Bone Metabolism Research Unit, Dr. O. Sánchez-Pernaute, from the Inflammation Research Unit, and M. Torralbo García, from the Bone Densitometry Unit (Fundación Jiménez Díaz) for their valuable advice and technical assistance in this study. This work was partly funded by grants from the Comunidad Autónoma de Madrid (CAM, 08.7/0007.1/2003), the Spanish Ministerio de Ciencia y Tecnología (SAF 2003/08379) and Fondo de Investigaciones Sanitarias (FIS CP03/0011). M.E.M. is a fellow of the Fundación Conchita Rábago.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Castañeda, S., Largo, R., Calvo, E. et al. Bone mineral measurements of subchondral and trabecular bone in healthy and osteoporotic rabbits. Skeletal Radiol 35, 34–41 (2006). https://doi.org/10.1007/s00256-005-0022-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-005-0022-z