Abstract
Background
Treatment pathways for isolated distal radius fractures in children are becoming more tailored to specific fracture types and include different management plans for stable buckle fractures versus potentially unstable distal radius fractures.
Objective
To propose a measurement rule to aid in differentiating stable buckle fractures from other distal radius fractures in children.
Materials and methods
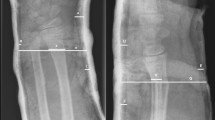
A medical record search identified 203 children with closed distal radius fractures during a 14-month period. A consensus of two senior readers served as a reference standard to distinguish buckle fractures from other distal radius fractures. We measured fracture-to-physis distance on posteroanterior (PA) and lateral radiographs for each of the isolated distal radius fractures. We analyzed diagnostic accuracy, using fracture-to-physis distance as a predictor for buckle fractures, in children ages 3–16 years. We used a receiver operating characteristic (ROC) curve to determine the cut-off values tested.
Results
There were 148 buckle fractures (73%) and 55 isolated potentially unstable distal radius fractures (27%). For children 7–16 years, buckle fracture-to-physis distance was <1 cm in only 1/106 (0.9%) on the PA projection and none on the lateral projection. Diagnostic accuracy for buckle fracture diagnosis was 82% using a cut-off of 14 mm (PA) and 13 mm (lateral). In children 3–6 years old, the buckle fracture-to-physis distance was <1 cm in 1/42 (2.4%) on the PA radiographs and another 1/42 (2.4%) on the lateral radiographs. Diagnostic accuracy was low for younger children for all tested distances.
Conclusion
We propose utilizing a measurement rule to increase diagnostic accuracy for buckle fractures in children ≥7 years old. An isolated distal radius fracture in a child 7 years or older is not likely to be a buckle fracture if the fracture-to-physis distance is <1 cm.




Similar content being viewed by others
References
Bae DS (2008) Pediatric distal radius and forearm fractures. J Hand Surg 33A:1911–1923
Symons S, Rowsell M, Bhowal B, Dias JJ (2001) Hospital versus home management of children with buckle fractures of the distal radius: a prospective, randomised trial. J Bone Joint Surg Br 83:556–560
Van Bosse HJP, Patel RJ, Thacker M, Sala DAS (2005) Minimalistic approach to treating wrist torus fractures. J Pediatr Orthop 25:495–500
West S, Andrews J, Bebbington A et al (2005) Buckle fractures of the distal radius are safely treated in a soft bandage: a randomized prospective trial of bandage versus plaster cast. J Pediatr Orthop 25:322–325
Randsborg PH, Sivertsen EA (2009) Distal radius fractures in children: substantial difference in stability between buckle and greenstick fractures. Acta Orthop 80:585–589
Witney-Lagen C, Smith C, Walsh G (2012) Soft cast versus rigid cast for treatment of distal radius buckle fractures in children. Injury 44:508–513
Koelink E, Schuh S, Howard A et al (2016) Primary care physician follow-up of distal radius buckle fractures. Pediatrics 137:1–9
Bochang C, Katz K, Weigl D et al (2008) Are frequent radiographs necessary in the management of closed forearm fractures in children? J Clin Orthop 2:217–220
Plint AC, Perry JJ, Correll R et al (2006) A randomized, controlled trial of removable splinting versus casting for wrist buckle fractures in children. Pediatrics 117:691–697
Hill CE, Masters JPM, Perry DC (2016) A systemic review of alternative splinting versus complete plaster casts for the management of childhood buckle fractures of the wrist. J Pediatr Orthop B 25:183–190
Williams KG, Smith G, Luhmann SJ et al (2013) A randomized controlled trial of cast versus splint for distal radial buckle fracture: an evaluation of satisfaction, convenience, and preference. Pediatr Emerg Care 29:555–559
Knight KM, Hadley G, Parikh A (2015) Buckle fractures of the distal radius: increased efficiency and cost savings through a new management pathway. Arch Dis Child 100:A229
TerreBlanche B, Eismann EA, Laor T et al (2016) Overdiagnosis of distal radius buckle fracture in children. American Association for Hand Surgery (abstract). http://meeting.handsurgery.org/abstracts/2016/P100.cgi. Accessed 12 Oct 2018
Harris PA, Taylor R, Thielke R et al (2009) Research electronic data capture (REDCap) — a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42:377–381
Hernandez JA, Swischuk LE, Yngve DA, Carmichael JD (2003) The angled buckle fracture in pediatrics: a frequently missed fracture. Emerg Radiol 10:71–75
Joeris A, Lutz N, Blumenthal A (2017) The AO pediatric comprehensive classification of long bone fractures (PCCF). Acta Orthop 88:123–128
Acknowledgments
This work was presented at the annual meeting of the Society for Pediatric Radiology, Nashville, TN, May 15–19, 2018.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Iles, B.W., Samora, J.B., Singh, S. et al. Differentiating stable buckle fractures from other distal radius fractures: the 1-cm rule. Pediatr Radiol 49, 358–364 (2019). https://doi.org/10.1007/s00247-018-4316-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4316-4