Abstract
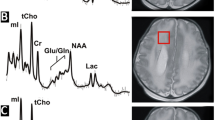
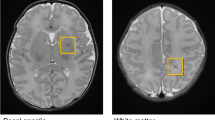
Patients with congenital heart disease (CHD) are at high risk for adverse neurodevelopmental outcomes. The aim of this work was to assess brain maturity and brain injury in newborns with cyanotic CHD using proton magnetic resonance spectroscopy (MRS). The study included 38 newborns with cyanotic CHD (study group) and 20 healthy full-term newborns (control group) matched together regarding gestational age and sex. Three-dimensional MRS showed that the mean ratio of N-acetylaspartate to choline (Ch) was significantly lower in newborns with cyanotic CHD (0.55 ± 0.08) compared with controls (0.67 ± 0.11) (p < 0.001). However, the mean ratio of lactate to Ch metabolite was significantly higher in the studied cases (0.14 ± 0.04) compared with controls (0.09 ± 0.04) (p < 0.001). The mean value for average diffusivity was 1.41 ± 0.06 in newborns with cyanotic CHD compared with 1.27 ± 0.07 in control newborns (p < 0.001), and the mean value for white-matter fractional anisotropy was 0.19 ± 0.03 in cyanotic newborns and 0.25 ± 0.08 in controls (p < 0.001). Newborns with cyanotic CHD are at increased risk of cerebral white matter injury as well as poor brain maturity. MRS provides a surrogate marker for early detection of such brain abnormalities.


Similar content being viewed by others
References
Ballard J, Khory J, Wedig K, Wang L, Eilers-Walsman B, Lipp R (1991) New Ballard score: expanded to include extremely premature infants. J Pediatr 119:417–420
Barkovich AJ, Westmark KD, Bedi HS, Partridge JC, Ferriero DM, Vigneron DB (2001) Proton spectroscopy and diffusion imaging on the first day of life after perinatal asphyxia: preliminary report. Am J Neuroradiol 22:1786–1794
Barkovich AJ, Miller SP, Bartha A, Newton N, Hamrick SE, Mukherjee P et al (2006) MR imaging, MR spectroscopy, and diffusion tensor imaging of sequential studies in neonates with encephalopathy. Am J Neuroradiol 27:533–547
Bland JM, Altman DG (1996) Statistics notes: logarithms. Br Med J 4:312–319
Deipolyi AR, Mukherjee P, Gill K, Henry R, Partridge SC, Veeraghavan S et al (2005) Comparing microstructural and macrostructural development of the cerebral cortex in premature newborns: diffusion tensor imaging versus cortical gyration. Neuroimage 27:579–586
Drobyshevsky A, Song SK, Gamkrelidze G, Wyrwicz AM, Derrick M, Meng F et al (2005) Developmental changes in diffusion anisotropy coincide with immature oligodendrocyte progression and maturation of compound action potential. J Neurosci 25:5988–5997
Freed DH, Robertson CMT, Sauve RS, Joffe AR, Rebeyka IM, Ross IM et al (2006) Intermediate-term outcomes of the arterial switch operation for transposition of great arteries in neonates: alive but well? J Thorac Cardiovasc Surg 132:845–852
Gaynor JW, Jarvik GP, Bernbaum J, Gerdes M, Wernovsky G, Burnham NB et al (2006) The relationship of post-operative electrographic seizures to neurodevelopmental outcome at 1 year of age after neonatal and infant cardiac surgery. J Thorac Cardiovasc Surg 131:181–189
Kandil ME, Elwan A, Hussein Y, Kandeel W, Rasheed M (2009) Ghrelin levels in children with congenital heart disease. J Trop Pediatr 55:307–312
Limperopoulos C, Majnemer A, Shevell MI, Rosenblatt B, Rohlicek C, Tchervenkov C (1999) Neurologic status of newborns with congenital heart defects before open heart surgery. Pediatrics 103:402–408
Mahle WT, Tavani F, Zimmerman RA, Nicolson SC, Galli KK, Gaynor JW et al (2002) An MRI study of neurological injury before and after congenital heart surgery. Circulation 106:I109–I114
McQuillen PS, Hamrick SE, Perez MJ, Barkovich AJ, Glidden DV, Karl TR et al (2006) Balloon atrial septostomy is associated with preoperative stroke in neonates with transposition of the great arteries. Circulation 113:280–285
Michael JH, Scallan FRCA (2010) Brain injury in children with congenital heart disease. Pediatr Anaesth 13:284–293
Miller G, Tesman JR, Ramer JC, Baylen BG, Myers JL (1996) Outcome after open-heart surgery in infants and children. J Child Neurol 11:49–53
Miller SP, Newton N, Ferriero D, Partridge JC, Glidder DV (2002) MRS predictors of 30-month outcome following perinatal depression. Role of socio-economic factors. Pediatr Res 52:71–77
Miller SP, McQuillen PS, Hamrick S, Xu DV, Charlton N, Karl TA et al (2007) Abnormal brain development in newborns with congenital heart disease. N Engl J Med 357:1928–1938
Mukherjee P, Miller JH, Shimony JS, Philip JV, Nehra D, Snyder AZ et al (2002) Diffusion-tensor MR imaging of gray and white matter development during normal human brain maturation. Am J Neuroradiol 23:1445–1456
Newburger JW, Jonas RA, Wernovsky G, Wipij D, Hickey PR, Kuban KC et al (1993) A comparison of the perioperative neurologic effects of hypothermic circulatory arrest versus low-flow cardiopulmonary bypass in infant heart surgery. N Engl J Med 329:1057–1064
Novotny E, Ashwal S, Shevell M (1998) Proton magnetic resonance spectroscopy: an emerging technology in pediatric neurology research. Pediatr Res 44:1–10
Oates RK, Simpson JM, Turnbull JA, Cartmill TB (1995) The relationship between intelligence and duration of circulatory arrest with deep hypothermia. J Thorac Cardiovasc Surg 110:786–792
Ransom J, Srivastava D (2007) The genetics of cardiac birth defects. Semin Cell Dev Biol 18:132–139
Scherlock RL, McQuillen PS, Miller SP (2009) Preventing brain injury in newborns with congenital heart disease. Brain imaging and innovative trial designs. Stroke 40:327–334
Snider AR, Serwer GA, Ritter SP (1997) Echocardiography in pediatric heart disease, 2nd edn. Mosby, St. Louis, MO, pp 195–223
Vigneron DB, Barkovich AJ, Noworolski SM, Busschea MD, Henrya RG, Lua Y et al (2001) Three-dimensional proton MR spectroscopic imaging of premature and term neonates. Am J Neuroradiol 22:1424–1433
Zeger SL, Liang KY, Albert PS (1998) Models for longitudinal data: a generalized estimating equation approach. Biometrics 44:1049–1060
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shedeed, S.A., Elfaytouri, E. Brain Maturity and Brain Injury in Newborns With Cyanotic Congenital Heart Disease. Pediatr Cardiol 32, 47–54 (2011). https://doi.org/10.1007/s00246-010-9813-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-010-9813-7