Abstract
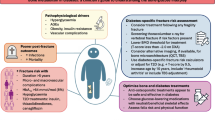
An increased risk of fractures in primary hyperparathyroidism (PHPT) has been reported in a number of relatively small studies. Performing a systematic literature search, we identified available studies and calculated common estimates by pooling results from the individual studies in a meta-analysis. Searching EMBASE and PubMed, we identified published studies reporting the risk of fractures in PHPT compared to a control group. We calculated odds ratio (OR) with 95% confidence interval (CI). A total of 804 studies were identified of which 12 studies were included. Risk of any fracture was increased compared to controls (OR 2.01; 95% CI, 1.61-2.50; I2 46%, 5 studies). Analysis of fracture risk at specific sites showed an increased risk of fracture at the forearm (OR 2.36; 95% CI, 1.64-3.38; I2 0%, 4 studies) and spine (OR 3.00; 95% CI, 1.41, 6.37, I2 88%, 9 studies). Risk estimate for hip fractures was non-significantly increased (OR 1.27; 95% CI, 0.97-1.66; I2 0%, 3 studies). Risk of vertebral fractures (VFx) was also increased if analyses were restricted to only studies with a healthy control group (OR 5.76; 95% CI, 3.86-8.60; I2 29%, 6 studies), studies including patients with mild PHPT (OR 4.22; 95% CI, 2.20-8.12; I2 57%, 4 studies) or studies including postmenopausal women (OR 8.07; 95% CI, 4.79-13.59; I2 0%, 3 studies). PHPT is associated with an increased risk of fractures. Although a number of studies are limited—it seems that the risk is increased across different skeletal sites including patients with mild PHPT and postmenopausal women.





Similar content being viewed by others
References
Fraser WD (2009) Hyperparathyroidism. Lancet 374:145–158. https://doi.org/10.1016/S0140-6736(09)60507-9
Bilezikian JP, Cusano NE, Khan AA et al (2014) Primary hyperparathyroidism. Nat Rev Dis Prim 53:417–424.e5. https://doi.org/10.1016/j.jaac.2013.12.025
Press DM, Siperstein AE, Berber E, Shin JJ, Metzger R, Jin J, Monteiro R, Mino J, Swagel W, Mitchell JC (2013) The prevalence of undiagnosed and unrecognized primary hyperparathyroidism: a population-based analysis from the electronic medical record. Surg (United States) 154:1232–1238. https://doi.org/10.1016/j.surg.2013.06.051
Yu N, Donnan PT, Murphy MJ, Leese GP (2009) Epidemiology of primary hyperparathyroidism in Tayside, Scotland, UK. Clin Endocrinol (Oxf) 71:485–493. https://doi.org/10.1111/j.1365-2265.2008.03520.x
Yeh MW, Ituarte PHG, Zhou HC, Nishimoto S, Amy Liu IL, Harari A, Haigh PI, Adams AL (2013) Incidence and prevalence of primary hyperparathyroidism in a racially mixed population. J Clin Endocrinol Metab 98:1122–1129. https://doi.org/10.1210/jc.2012-4022
Alore EA, Suliburk JW, Ramsey DJ, Massarweh NN, Balentine CJ, Singh H, Awad SS, Makris KI (2019) Diagnosis and management of primary hyperparathyroidism across the Veterans Affairs health care system. JAMA Intern Med 179:1220–1227. https://doi.org/10.1001/jamainternmed.2019.1747
Seib CD, Meng T, Suh I, Cisco RM, Lin DT, Morris AM, Trickey AW, Kebebew E (2020) Undertreatment of primary hyperparathyroidism in a privately insured US population: decreasing utilization of parathyroidectomy despite expanding surgical guidelines. Surgery. 169:87–93. https://doi.org/10.1016/j.surg.2020.04.066
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JPA, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700. https://doi.org/10.1136/bmj.b2700
Kochersberger G, Buckley NJ, Leight GS, Martinez S, Studenski S, Vogler J, Lyles KW (1987) What is the clinical significance of bone loss in primary hyperparathyroidism? Arch Intern Med 147:1951–1953
Wilson RJ (1988) Mild asymptomatic primary hyperparathyroidism is not a risk factor for vertebral fractures. Ann Intern Med 109:959–962. https://doi.org/10.7326/0003-4819-109-12-959
Larsson K, Lindh E, Lind L, Persson I, Ljunghall S (1989) Increased fracture risk in hypercalcemia: bone mineral content measured in hyperparathyroidism. Acta Orthop 60:268–270. https://doi.org/10.3109/17453678909149275
Kenny AM, MacGillivray DC, Pilbeam CC et al (1995) Fracture incidence in postmenopausal women with primary hyperparathyroidism. Surgery 118:109–114
De Geronimo S, Romagnoli E, Diacinti D et al (2006) The risk of fractures in postmenopausal women with primary hyperparathyroidism. Eur J Endocrinol 155:415–420. https://doi.org/10.1530/eje.1.02225
Vignali E, Viccica G, Diacinti D et al (2009) Morphometric vertebral fractures in postmenopausal women with primary hyperparathyroidism. J Clin Endocrinol Metab 94:2306–2312. https://doi.org/10.1210/jc.2008-2006
Kaji H, Yamauchi M, Chihara K, Sugimoto T (2005) The threshold of bone mineral density for vertebral fractures in female patients with primary hyperparathyroidism. Eur J Endocrinol 153:373–378. https://doi.org/10.1530/eje.1.01985
Eller-Vainicher C, Filopanti M, Palmieri S, Ulivieri FM, Morelli V, Zhukouskaya VV, Cairoli E, Pino R, Naccarato A, Verga U, Scillitani A, Beck-Peccoz P, Chiodini I (2013) Bone quality, as measured by trabecular bone score, in patients with primary hyperparathyroidism. Eur J Endocrinol 169:155–162. https://doi.org/10.1530/EJE-13-0305
Larsson K, LJUNGHALL S, KRUSEMO UB et al (1993) The risk of hip fractures in patients with primary hyperparathyroidism: a population-based cohort study with a follow-up of 19 years. J Intern Med 234:585–593. https://doi.org/10.1111/j.1365-2796.1993.tb01017.x
Khosla S, Melton LJ, Wermers RA et al (1999) Primary hyperparathyroidism and the risk of fracture: a population-based study. J Bone Miner Res 14:1700–1707. https://doi.org/10.1359/jbmr.1999.14.10.1700
Vestergaard P, Mollerup CL, Frøkjaer VG et al (2000) Cohort study of fracture risk before and after surgery of primary hyperparathyroidism. BMJ Clin Res ed 163:4875–4878
Yu N, Donnan PT, Leese GP (2011) A record linkage study of outcomes in patients with mild primary hyperparathyroidism: the Parathyroid Epidemiology and Audit Research Study (PEARS). Clin Endocrinol (Oxf) 75:169–176. https://doi.org/10.1111/j.1365-2265.2010.03958.x
Lewiecki EM, Miller PD (2013) Skeletal effects of primary hyperparathyroidism: bone mineral density and fracture risk. J Clin Densitom 16:28–32. https://doi.org/10.1016/j.jocd.2012.11.013
Silverberg SJ, Shane E, De La Cruz L et al (1989) Skeletal disease in primary hyperparathyroidism. J Bone Miner Res 4:283–291
Hansen S, Jensen JEB, Rasmussen L et al (2010) Effects on bone geometry, density, and microarchitecture in the distal radius but not the tibia in women with primary hyperparathyroidism: a case-control study using HR-pQCT. J Bone Miner Res 25:1941–1947. https://doi.org/10.1002/jbmr.98
Wang W, Nie M, Jiang Y, Li M, Meng X, Xing X, Wang O, Xia W (2020) Impaired geometry, volumetric density, and microstructure of cortical and trabecular bone assessed by HR-pQCT in both sporadic and MEN1-related primary hyperparathyroidism. Osteoporos Int 31:165–173. https://doi.org/10.1007/s00198-019-05186-1
Cusano NE, Rubin MR, Silva BC, Tay YKD, Williams JM, Agarwal S, Omeragic B, Guo XE, Bilezikian JP (2018) Skeletal microstructure and estimated bone strength improve following parathyroidectomy in primary hyperparathyroidism. J Clin Endocrinol Metab 103:196–205. https://doi.org/10.1210/jc.2017-01932
Hansen S, Hauge EM, Rasmussen L, Jensen JEB, Brixen K (2012) Parathyroidectomy improves bone geometry and microarchitecture in female patients with primary hyperparathyroidism: a one-year prospective controlled study using high-resolution peripheral quantitative computed tomography. J Bone Miner Res 27:1150–1158. https://doi.org/10.1002/jbmr.1540
Silva BC, Boutroy S, Zhang C, McMahon DJ, Zhou B, Wang J, Udesky J, Cremers S, Sarquis M, Guo XDE, Hans D, Bilezikian JP (2013) Trabecular bone score (TBS)-a novel method to evaluate bone microarchitectural texture in patients with primary hyperparathyroidism. J Clin Endocrinol Metab 98:1963–1970. https://doi.org/10.1210/jc.2012-4255
Bilezikian JP, Brandi ML, Eastell R, Silverberg SJ, Udelsman R, Marcocci C, Potts JT Jr (2014) Guidelines for the management of asymptomatic primary hyperparathyroidism: summary statement from the fourth international workshop. J Clin Endocrinol Metab 99:3561–3569. https://doi.org/10.1210/jc.2014-1413
Lundstam K, Heck A, Mollerup C, Godang K, Baranowski M, Pernow Y, Varhaug JE, Hessman O, Rosén T, Nordenström J, Jansson S, Hellström M, Bollerslev J, SIPH Study Group (2015) Effects of parathyroidectomy versus observation on the development of vertebral fractures in mild primary hyperparathyroidism. J Clin Endocrinol Metab 100:1359–1367. https://doi.org/10.1210/jc.2014-3441
Ejlsmark-Svensson H, Bislev LS, Lajlev S, Harsløf T, Rolighed L, Sikjaer T, Rejnmark L (2018) Prevalence and risk of vertebral fractures in primary hyperparathyroidism: a nested case-control study. J Bone Miner Res 33:1657–1664. https://doi.org/10.1002/jbmr.3461
Bilezikian JP (2018) Primary hyperparathyroidism. J Clin Endocrinol Metab 103:3993–4004
Rao DS, Phillips ER, Divine GW, Talpos GB (2004) Randomized controlled clinical trial of surgery versus no surgery in patients with mild asymptomatic primary hyperparathyroidism. J Clin Endocrinol Metab 89:5415–5422. https://doi.org/10.1210/jc.2004-0028
Ambrogini E, Cetani F, Cianferotti L, Vignali E, Banti C, Viccica G, Oppo A, Miccoli P, Berti P, Bilezikian JP, Pinchera A, Marcocci C (2007) Surgery or surveillance for mild asymptomatic primary hyperparathyroidism: a prospective, randomized clinical trial. J Clin Endocrinol Metab 92:3114–3121. https://doi.org/10.1210/jc.2007-0219
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ejlsmark-Svensson, H., Rolighed, L., Harsløf, T. et al. Risk of fractures in primary hyperparathyroidism: a systematic review and meta-analysis. Osteoporos Int 32, 1053–1060 (2021). https://doi.org/10.1007/s00198-021-05822-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-021-05822-9