Abstract
Summary
A cohort of 183 postmenopausal women, who had either discontinued or continued bisphosphonates (BPs) after first-line therapy, was used to investigate the relationships between “drug holiday” and clinical fracture. The risk of new clinical fractures was found to be 40% higher in women who had taken a BP “drug holiday.”
Introduction
BPs are the most widely used treatment for postmenopausal osteoporosis. The optimal treatment duration, however, remains unclear. The purpose of this study was to evaluate the fracture risk in postmenopausal women with osteoporosis after discontinuing BP treatment (BP “drug holiday”).
Methods
A retrospective analysis was performed at Lille University Hospital (LUH) on postmenopausal women with osteoporosis who had taken a “drug holiday” or continued treatment after first-line BP therapy (3 to 5 years). The occurrence of new clinical fractures during follow-up was also explored. Cox proportional hazards models were used to investigate the relationships between BP “drug holiday” and the occurrence of clinical fractures, while controlling for confounding factors. Survival without new clinical fractures was analyzed using Kaplan-Meier curves and log-rank tests.
Results
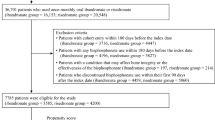
One hundred eighty-three women (mean age: 61.8 years; SD: 8.7) who had previously undergone BP treatment for 3 to 5 years were enrolled in our study. The patients had received alendronate (n = 81), risedronate (n = 73), zoledronic acid (n = 20), and ibandronate (n = 9). In 166 patients (“drug holiday” group: n = 31; continuous-treatment group: n = 135), follow-up ranged from 6 to 36 months (mean duration: 31.8 months; SD: 8.2). The incidences of new clinical fractures during follow-up were 16.1% (5/31) and 11.9% (16/135). After full adjustment, the hazard ratio of new clinical fractures among “drug holiday” patients was 1.40 (95% CI: 1.12–1.60; p = 0.0095).
Conclusions
After first-line BP therapy in postmenopausal women with osteoporosis, the risk of new clinical fractures was 40% higher in subjects who took a bisphosphonate drug holiday.




Similar content being viewed by others
References
Black DM, Cummings SR, Karpf DB et al (1996) Randomised trial of effect of alendronate on risk of fracture in women with existing vertebral fractures. Fracture Intervention Trial Research Group Lancet 348:1535–1541
Cummings SR, Black DM, Thompson DE et al (1998) Effect of alendronate on risk of fracture in women with low bone density but without vertebral fractures: results from the Fracture Intervention Trial. JAMA 280:2077–2082
Black DM, Delmas PD, Eastell R et al (2007) HORIZON Pivotal Fracture Trial. Once yearly zoledronic acid for treatment of postmenopausal osteoporosis. N Engl J Med 356:1809–1822
Lyles KW, Colón-Emeric CS, Magaziner JS et al (2007) HORIZON Recurrent Fracture Trial. Zoledronic acid and clinical fractures and mortality after hip fracture. N Engl J Med 357:1799–1809
Gedmintas L, Solomon DH, Kim SC (2013) Bisphosphonates and risk of subtrochanteric, femoral shaft, and atypical femur fracture: a systematic review and meta-analysis. J Bone Miner Res 28:1729–1737
Khan AA, Morrison A, Hanley DA et al (2015) Diagnosis and management of osteonecrosis of the jaw: a systematic review and international consensus. J Bone Miner Res 30:3–23
Black DM, Schwartz AV, Ensrud KE et al (2006) Effects of continuing or stopping alendronate after 5 years of treatment: the Fracture Intervention Trial Long-term Extension (FLEX): a randomized trial. JAMA 24:2927–2938
Black DM, Reid IR, Boonen S et al (2012) The effect of 3 versus 6 years of zoledronic acid treatment of osteoporosis: a randomized extension to the HORIZON-Pivotal Fracture Trial (PFT). J Bone Miner Res 27:243–254
Paccou J (2016) Management after first-line antiresorptive treatment for postmenopausal osteoporosis. Joint Bone Spine 83:373–375
Curtis JR, Westfall AO, Cheng H, Delzell E, Saag KG (2008) Risk of hip fracture after bisphosphonate discontinuation: implications for a drug holiday. Osteoporos Int 19:1613–1620
Adams AL, Adams JL, Raebel MA, et al. Bisphosphonate drug holiday and fracture risk. Abstract 1045. Presented at: American Society for Bone and Mineral Research 2014 Sept 12–15, 2014; Houston, Texas
Briot K, Cortet B, Thomas T et al (2012) 2012 Update of French guidelines for the pharmacological treatment of postmenopausal osteoporosis. Joint Bone Spine 79:304–313
Adler RA, El-Hajj Fuleihan G, Bauer DC, Camacho PM, Clarke BL et al (2016) Managing osteoporosis in patients on long-term bisphosphonate treatment: report of a Task Force of the American Society for Bone and Mineral Research. J Bone Miner Res 31:16–35
Silverman SL, Adachi JD, Dennison E, International Osteoporosis Foundation Epidemiology/Quality of Life Working Group (2016) Bisphosphonate drug holidays: we reap what we sow. Osteoporos Int 27:849–852
Cosman F, Cauley JA, Eastell R, Boonen S, Palermo L, Reid IR, Cummings SR, Black DM (2014) Reassessment of fracture risk in women after 3 years of treatment with xoledronic acid: when is it reasonable to discontinue treatment? J Clin Endocrinol Metab 99:4546–4554
Bauer DC, Schwartz A, Palermo L et al (2014) Fracture prediction after discontinuation of 4 to 5 years of alendronate therapy. JAMA Intern Med 174:1126–1134
Chiha M, Myers LE, Ball CA, Sinacore JM, Camacho PM (2013) Long-term follow-up of patients on drug holiday from bisphosphonates: real-world setting. Endocr Pract 19:989–994
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Julien Paccou has received honoraria from Amgen, MSD, Eli Lilly, and Pfizer. Bernard Cortet has received honoraria from Amgen, Eli Lilly, Expanscience, Ferring, Medtronic, Novartis, and Roche Diagnostics. For the remaining authors, none were declared.
Rights and permissions
About this article
Cite this article
Mignot, M.A., Taisne, N., Legroux, I. et al. Bisphosphonate drug holidays in postmenopausal osteoporosis: effect on clinical fracture risk. Osteoporos Int 28, 3431–3438 (2017). https://doi.org/10.1007/s00198-017-4215-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-017-4215-9