Abstract
Summary
Low bone mineral density (BMD) and osteoporosis have become a public health problem. We found that non-Hispanic white, black, and Asian adults with extremely low education and personal income are more likely to have lower BMD. This relationship is gender-specific. These findings are valuable to guide bone health interventions.
Introduction
The evidence is limited regarding the relationship between socioeconomic status (SES) and bone mineral density (BMD) for minority populations in the USA, as well as the relationship between SES and BMD for men. This study explored and examined the relationship between SES and BMD by race/ethnicity and gender.
Methods
Data (n = 6568) from the Louisiana Osteoporosis Study (LOS) was examined, including data for non-Hispanic whites (n = 4153), non-Hispanic blacks (n = 1907), and non-Hispanic Asians (n = 508). General linear models were used to estimate the relationship of SES and BMD (total hip and lumbar spine) stratified by race/ethnicity and gender. Adjustments were made for physiological and behavioral factors.
Results
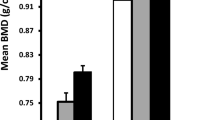
After adjusting for covariates, men with education levels below high school graduate experienced relatively low hip BMD than their counterparts with college or graduate education (p < 0.05). In addition, women reporting a personal annual income under $20,000 had relatively low hip and spine BMD than their counterparts with higher income level(s) (p < 0.05).
Conclusions
Establishing a conclusive positive or negative association between BMD and SES proved to be difficult. However, individuals who are at an extreme SES disadvantage are the most vulnerable to have relatively low BMD in the study population. Efforts to promote bone health may benefit from focusing on men with low education levels and women with low individual income.


Similar content being viewed by others
References
Lee JJY, Aghdassi E, Cheung AM, Morrison S, Cymet A, Peeva V, Neville C, Hewitt S, DaCosta D, Pineau C, Pope J, Fortin PR (2012) Ten-year absolute fracture risk and hip bone strength in Canadian women with systemic lupus Erythematosus. J Rheumatol 39:1378–1384
Nelson HD, Haney EM, Dana T, Bougatsos C, Chou R (2010) Screening for osteoporosis: an update for the U.S. preventive services task force. Ann Intern Med 153(99):W. 43
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A (2007) Incidence and economic burden of osteoporosis-related fractures in the United States, 2005–2025. J Bone Miner Res 22:465–475
Compston J (2010) Osteoporosis: social and economic impact. Radiol Clin N Am 48:477–482
Mariconda M, Costa GG, Cerbasi S, Recano P, Orabona G, Gambacorta M, Misasi M (2016) Factors predicting mobility and the change in activities of daily living after hip fracture: a 1-year prospective cohort study. J Orthop Trauma 30:71–77
Bowman SA (2009) Socioeconomic characteristics, dietary and lifestyle patterns, and health and weight status of older adults in NHANES, 1999–2002: a comparison of Caucasians and African Americans. National Health and Nutrition Examination Survey Journal of Nutrition for the Elderly 28:30–46
Travison T, Chiu G, McKinlay J, Araujo A (2011) Accounting for racial/ethnic variation in bone mineral content and density: the competing influences of socioeconomic factors, body composition, health and lifestyle, and circulating androgens and estrogens. Osteoporosis Int 22:2645–2654
Navarro MC, Saavedra P, Jódar E, Gómez DT, Mirallave A, Sosa M (2013) Osteoporosis and metabolic syndrome according to socio-economic status, contribution of PTH, vitamin D and body weight: the Canarian osteoporosis poverty study (COPS). Clin Endocrinol 78:681–686
Wang S, Lin S, Zhou Y, Wang Z (2008) Social and behavior factors related to aged Chinese women with osteoporosis. Gynecol Endocrinol 24:538–545
Kumar A, Mittal S, Orito S, Ishitani K, Ohta H (2010) Impact of dietary intake, education, and physical activity on bone mineral density among north Indian women. J Bone Miner Metab 28:192–201
Shin CS, Choi HJ, Kim MJ, Kim JT, Yu SH, Koo BK, Cho HY, Cho SW, Kim SW, Park YJ, Jang HC, Kim SY, Cho NH (2010) Prevalence and risk factors of osteoporosis in Korea: a community-based cohort study with lumbar spine and hip bone mineral density. Bone 47:378–387
Hsieh C-H, Wang C-Y, McCubbin M, Zhang S, Inouye J (2008) Factors influencing osteoporosis preventive behaviours: testing a path model. J Adv Nurs 62:336–345
Brennan SL, Pasco JA, Urquhart DM, Oldenburg B, Wang Y, Wluka AE (2011) Association between socioeconomic status and bone mineral density in adults: a systematic review. Osteoporosis Int 22:517–527
Myong J, Kim H, Choi SE, Koo J (2012) The effect of socioeconomic position on bone health among Koreans by gender and menopausal status. Calcif Tissue Int 90:488–495
Brennan S, Winzenberg T, Pasco J, Wluka A, Dobbins A, Jones G (2013) Social disadvantage, bone mineral density and vertebral wedge deformities in the Tasmanian older adult cohort. Osteoporosis Int 24:1909–1916
Brennan SL, Henry MJ, Wluka AE, Nicholson GC, Kotowicz MA, Williams JW, Pasco JA (2009) BMD in population-based adult women is associated with socioeconomic status. J Bone Miner Res 24:809–815
Elliot JR, Gilchrist NL, Wells JE (1996) The effect of socioeconomic status on bone density in a male Caucasian population (English). Bone 18:371–373
Brennan SL, Henry MJ, Wluka AE, Nicholson GC, Kotowicz MA, Pasco JA (2010) Socioeconomic status and bone mineral density in a population-based sample of men. Bone 46:993–999
Crandall CJ, Merkin SS, Seeman TE, Greendale GA, Binkley N, Karlamangla AS (2012) Socioeconomic status over the life-course and adult bone mineral density: the midlife in the U.S. study. Bone 51:107–113
Wang M, Dixon L (2006) Socioeconomic influences on bone health in postmenopausal women: findings from NHANES III, 1988–1994. Osteoporosis Int 17:91–98
He H, Liu Y, Tian Q, Papasian CJ, Hu T, Deng H (2016) Relationship of sarcopenia and body composition with osteoporosis. Osteoporos Int 27:473–8222
Deng HW, Stegman MR, Davies KM, Conway T, Recker RR (1999) Genetic determination of variation and covariation of peak bone mass at the hip and spine. J Clin Densitom 2:251–263
Carey G (2013) Chapter 9 The General Linear Model (GLM): A gentle introduction. In: Quantitative Methods In Neuroscience. http://psych.colorado.edu/~carey/qmin/QMIN_2013_03_17.pdf. Accessed 12 January 2017
Liu H, Guo G (2015) Lifetime socioeconomic status, historical context, and genetic inheritance in shaping body mass in middle and late adulthood. Am Sociol Rev 80:705–737
Zhu K, Hunter M, James A, Lim EM, Walsh JP (2015) Associations between body mass index, lean and fat body mass and bone mineral density in middle-aged Australians: the Busselton healthy ageing study. Bone 74:146–152
Mielck A, Vogelmann M, Leidl R (2014) Health-related quality of life and socioeconomic status: inequalities among adults with a chronic disease. Health & Quality of Life Outcomes 12:1–17
Luepker RV, Rosamond WD, Murphy R, Sprafka JM, Folsom AR, McGovern PG, Blackburn H (1993) Socioeconomic status and coronary heart disease risk factor trends. The Minnesota Heart Survey Circulation 88:2172–2179
Farber CR (2012) Systems genetics: a novel approach to dissect the genetic basis of osteoporosis. Curr Osteoporos Rep 10:228–235
Megyesi MS, Hunt LM, Brody H (2011) A critical review of racial/ethnic variables in osteoporosis and bone density research. Osteoporosis Int 22:1669–1679
Melton LJ (1990) Epidemiology of osteoporosis: predicting who is at risk. Ann N Y Acad Sci 592:295–306
Gaines JM, Marx KA (2011) Older men’s knowledge about osteoporosis and educational interventions to increase osteoporosis knowledge in older men: a systematic review. Maturitas 68:5–12
Nyakato VN (2014) Intra-household Social Determinants of Demand for Maternal Health Services in Mbarara District, Uganda. Thesis
Cunningham K, Ploubidis GB, Menon P, Ruel M, Kadiyala S, Uauy R, Ferguson E (2015) Women’s empowerment in agriculture and child nutritional status in rural Nepal. Public Health Nutr 18:3134–3145
Dito BB (2015) Women’s Intrahousehold decision-making power and their health status: evidence from rural Ethiopia. Fem Econ 21:168–190
Brenzel LE (1996) Female Decision-Making Power & the Intrahousehold Allocation of Food & Child Medical Care Resources in Ghana. In: NLM Catalog. https://www.ncbi.nlm.nih.gov/nlmcatalog/101069014. Accessed 15 January 2017
Doss C (2013) Intrahousehold bargaining and resource allocation in developing countries. World Bank Res Obs 28:52–78
Fridberg L, Webb A (2006) Determinants and Consequences of Bargaining Power in Households. In: The national bureau of economic research. http://www.nber.org/papers/w12367. Accessed 6 Jun 2016
Du Y, Xu Q (2016) Health disparities and delayed health care among older adults in California: a perspective from race, ethnicity, and immigration. Public Health Nurs 33:383–394
Cooper C, Westlake S, Harvey N, Javaid K, Dennison E, Hanson M (2006) Review: developmental origins of osteoporotic fracture. Osteoporosis Int 17:337
Marwaha RK, Tandon N, Reddy DHK, Mani K, Puri S, Aggarwal N, Grewal K, Singh S (2007) Peripheral bone mineral density and its predictors in healthy school girls from two different socioeconomic groups in Delhi. Osteoporos Int 18:375–383
Arabi A, Nabulsi M, Maalouf J, Choucair M, Khalifé H, Vieth R, El-Hajj Fuleihan G (2004) Bone mineral density by age, gender, pubertal stages, and socioeconomic status in healthy Lebanese children and adolescents. Bone 35:1169–1179
Brennan-Olsena SL, Williamsa LJ, Hollowaya KL, Hoskinga SM, Stuarta AL, Dobbinsa AG, Pascoa JA (2015) Small area-level socioeconomic status and all-cause mortality within 10 years in a population-based cohort of women: data from the Geelong osteoporosis study. Preventive Medicine Reports 2:505–511
Melton LJ (2001) The prevalence of osteoporosis: gender and racial comparison. Calcif Tissue Int 69:179–181
Moss NE (2002) Gender equity and socioeconomic inequality: a framework for the patterning of women’s health. Soc Sci Med 54:649–661
Hyndman JO (2009) Women and power in schools: Kentucky today through an historic lens. American Educational History Journal 36:105–120
Williams DR, Mohammed SA, Leavell J, Collins C (2010) Race, socioeconomic status and health: complexities, ongoing challenges and research opportunities. Ann N Y Acad Sci 1186:69–101
Centers for Disease Control and Prevention (2016) Excessive drinking. In: Alcohol and Public Health. http://www.cdc.gov/alcohol/data-stats.htm. Accessed 6 Nov 2016
Kang H (2013) The prevention and handling of the missing data. Korean Journal of Anesthesiology 64:402–406
Acknowledgments
We thank all the Louisiana Osteoporosis Study participants for volunteering to participate in this study. We would like to thank all staff who provided clinical expertise and/or collected and managed data. The Louisiana Osteoporosis Study was supported by Tulane University. Grants from the National Institutes of Health (Grant Nos. R01 AR059781, R01 MH104680), Edward G. Schlieder Endowment, and startup funds from Tulane University partially supported this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Du, Y., Zhao, LJ., Xu, Q. et al. Socioeconomic status and bone mineral density in adults by race/ethnicity and gender: the Louisiana osteoporosis study. Osteoporos Int 28, 1699–1709 (2017). https://doi.org/10.1007/s00198-017-3951-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-017-3951-1