Abstract
Summary
We evaluated the effect of parathyroid hormone (PTH) on Wnt10b production by immune system cells in humans. We showed that bone anabolic effect of intermittent PTH treatment may be amplified by T cells through increased production of Wnt10b. Chronic increase in PTH as in primary hyperparathyroidism does not increase Wnt10b expression.
Introduction
The aim of this study is to assess the effect of PTH on Wnt10b production by immune system cells in humans. We assessed both the effect of intermittent PTH administration (iPTH) and of chronic PTH hypersecretion in primary hyperparathyroidism (PHP).
Methods
Eighty-two women affected by post-menopausal osteoporosis were randomly assigned to treatment with calcium and vitamin D alone (22) or plus 1-84 PTH (42), or intravenous ibandronate (18). Wnt10b production by unfractioned blood nucleated cells and by T, B cells and monocytes was assessed by real-time RT-PCR and ELISA at baseline, 3, 6, 12 and 18 months of treatment. The effect of chronic elevation of PTH was evaluated in 20 patients affected by PHP at diagnosis and after surgical removal of parathyroid adenoma.
WNT10b from both osteoporotic and PHP patients was compared to healthy subjects matched for age and sex.
Results
iPTH increases Wnt10b production by T cells, whereas PHP does not. After surgical restoration of normal parathyroid function, WNT10b decreases, although it is still comparable with healthy subjects’ level. Thus, chronic elevation of PTH does not significantly increase WNT10b production as respect to control.
Conclusions
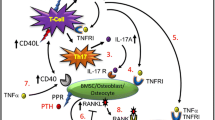
This is the first work showing the effect of both intermittent and chronic PTH increase on Wnt10b production by immune system cells. We suggest that, in humans, T cells amplified the anabolic effect of PTH on bone, by increasing Wnt10b production, which stimulates osteoblast activity.




Similar content being viewed by others
References
Silva BC, Costa AG, Cusano NE, Kousteni S, Bilezikian JP (2011) Catabolic and anabolic actions of parathyroid hormone on the skeleton. J Endocrinol Investig 34:801–810. doi:10.3275/7925
Chen P, Miller PD, Recker R, Resch H, Rana A, Pavo I, Sipos AA (2007) Increases in BMD correlate with improvements in bone microarchitecture with teriparatide treatment in postmenopausal women with osteoporosis. J Bone Miner Res 22:1173–1180
Neer RM, Arnaud CD, Zanchetta JR et al (2001) Effect of parathyroid hormone (1-34) on fractures and bone mineral density in postmenopausal women with osteoporosis. N Engl J Med 344:1434–1441
Greenspan SL, Bone HG, Ettinger MP et al (2007) Effect of recombinant human parathyroid hormone (1-84) on vertebral fracture and bone mineral density in postmenopausal women with osteoporosis: a randomized trial. Ann Intern Med 146:326–339
Thomson M, McCarroll J, Bond J, Gordon-Thomson CD, Williams E, Moore GP (2003) Parathyroid hormone-related peptide modulates signal pathways in skin and hair follicle cells. Exp Dermatol 12:389–395
Gardella TJ, Vilardaga JP (2015) International union of basic and clinical pharmacology. XCIII. The parathyroid hormone receptors-family B G protein-coupled receptors. Pharmacol Rev 67:310–337. doi:10.1124/pr.114.009464
Fiaschi-Taesch N, Sicari BM, Ubriani K, Bigatel T, Takane KK, Cozar-Castellano I, Bisello A, Law B, Stewart AF (2006) Cellular mechanism through which parathyroid hormone-related protein induces proliferation in arterial smooth muscle cells: definition of an arterial smooth muscle PTHrP/p27kip1 pathway. Circ Res 99:933–942
Faucheux C, Horton MA, Price JS (2002) Nuclear localization of type I parathyroid hormone/parathyroid hormone-related protein receptors in deer antler osteoclasts: evidence for parathyroid hormone-related protein and receptor activator of NF-kappaB-dependent effects on osteoclast formation in regenerating mammalian bone. J Bone Miner Res 17:455–464
Saini V, Marengi DA, Barry KJ, Fulzele KS, Heiden E, Liu X, Dedic C, Maeda A, Lotinun S, Baron R, Pajevic PD (2013) Parathyroid hormone (PTH)/PTH-related peptide type 1 receptor (PPR) signaling in osteocytes regulates anabolic and catabolic skeletal responses to PTH. J Biol Chem 288:20122–20134. doi:10.1074/jbc.M112.441360
Leupin O, Kramer I, Collette NM, Loots GG, Natt F, Kneissel M, Keller H (2007) Control of the SOST bone enhancer by PTH using MEF2 transcription factors. J Bone Miner Res 22:1957–1967
Kramer I, Baertschi S, Halleux C, Keller H, Kneissel M (2012) Mef2c deletion in osteocytes results in increased bone mass. J Bone Miner Res 27:360–373. doi:10.1002/jbmr.1492
Genetos DC, Toupadakis CA, Raheja LF, Wong A, Papanicolaou SE, Fyhrie DP, Loots GG, Yellowley CE (2010) Hypoxia decreases sclerostin expression and increases Wnt signaling in osteoblasts. J Cell Biochem 110:457–467. doi:10.1002/jcb.22559
Collette NM, Genetos DC, Economides AN, Xie L, Shahnazari M, Yao W, Lane NE, Harland RM, Loots GG (2012) Targeted deletion of Sost distal enhancer increases bone formation and bone mass. Proc Natl Acad Sci U S A 109:14092–14097. doi:10.1073/pnas.1207188109
Drake MT, Srinivasan B, Mödder UI, Peterson JM, McCready LK, Riggs BL, Dwyer D, Stolina M, Kostenuik P, Khosla S (2010) Effects of parathyroid hormone treatment on circulating sclerostin levels in postmenopausal women. J Clin Endocrinol Metab 95:5056–5062. doi:10.1210/jc.2010-072
Piemonte S, Romagnoli E, Bratengeier C, Woloszczuk W, Tancredi A, Pepe J, Cipriani C, Minisola S (2012) Serum sclerostin levels decline in post-menopausal women with osteoporosis following treatment with intermittent parathyroid hormone. J Endocrinol Investig 35:866–868. doi:10.3275/8522
Manolagas SC (2014) Wnt signaling and osteoporosis. Maturitas 78:233–237. doi:10.1016/j.maturitas.2014.04.013
Bedi B, Li JY, Tawfeek H, Baek KH, Adams J, Vangara SS, Chang MK, Kneissel M, Weitzmann MN, Pacifici R (2012) Silencing of parathyroid hormone (PTH) receptor 1 in T cells blunts the bone anabolic activity of PTH. Proc Natl Acad Sci U S A 109:E725–E733. doi:10.1073/pnas.1120735109
Terauchi M, Li JY, Bedi B, Baek KH, Tawfeek H, Galley S, Gilbert L, Nanes MS, Zayzafoon M, Guldberg R, Lamar DL, Singer MA, Lane TF, Kronenberg HM, Weitzmann MN, Pacifici R (2009) T lymphocytes amplify the anabolic activity of parathyroid hormone through Wnt10b signaling. Cell Metab 10:229–240. doi:10.1016/j.cmet.2009.07.010
Li JY, Walker LD, Tyagi AM, Adams J, Weitzmann MN, Pacifici R (2014) The sclerostin-independent bone anabolic activity of intermittent PTH treatment is mediated by T-cell-produced Wnt10b. J Bone Miner Res 29:43–54. doi:10.1002/jbmr.2044
Viapiana O, Fracassi E, Troplini S, Idolazzi L, Rossini M, Adami S, Gatti D (2013) Sclerostin and DKK1 in primary hyperparathyroidism. Calcif Tissue Int 92:324–329. doi:10.1007/s00223-012-9665-7
Ardawi MS, Al-Sibiany AM, Bakhsh TM, Rouzi AA, Qari MH (2012) Decreased serum sclerostin levels in patients with primary hyperparathyroidism: a cross-sectional and a longitudinal study. Osteoporos Int 23:1789–1797. doi:10.1007/s00198-011-1806-8
Bellido T, Ali AA, Gubrij I, Plotkin LI, Fu Q, O’Brien CA, Manolagas SC, Jilka R (2005) Chronic elevation of parathyroid hormone in mice reduces expression of sclerostin by osteocytes: a novel mechanism for hormonal control of osteoblastogenesis. Endocrinology 146:4577–4583
Parisien M, Mellish RW, Silverberg SJ, Shane E, Lindsay R, Bilezikian JP, Dempster DW (1992) Maintenance of cancellous bone connectivity in primary hyperparathyroidism: trabecular strut analysis. J Bone Miner Res 7:913–919
Parisien M, Silverberg SJ, Shane E, de la Cruz L, Lindsay R, Bilezikian JP, Dempster DW (1990) The histomorphometry of bone in primary hyperparathyroidism: preservation of cancellous bone structure. J Clin Endocrinol Metab 70:930–938
Parisien M, Cosman F, Mellish RW et al (1995) Bone structure in postmenopausal hyperparathyroid, osteoporotic, and normal women. J Bone Miner Res 10:1393–1399
Uchiyama T, Tanizawa T, Ito A, Endo N, Takahashi HE (1999) Microstructure of the trabecula and cortex of iliac bone in primary hyperparathyroidism patients determined using histomorphometry and node-strut analysis. J Bone Miner Metab 17:283–288
Acknowledgments
This work was supported by an unconditioned grant from Nycomed SpA (ISAG02AP13) which also provides the PTH 1-84 and calcium and vitamin D supplements. IR was supported by a grant from Italian Ministry of Health: Ricerca Sanitaria Finalizzata e Giovani Ricercatori 2009 (GR 2009-1584485). We are grateful to Prof. G. Gasparri (University of Turin, Italy) for recruiting PHP patients.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
D’Amelio, P., Sassi, F., Buondonno, I. et al. Treatment with intermittent PTH increases Wnt10b production by T cells in osteoporotic patients. Osteoporos Int 26, 2785–2791 (2015). https://doi.org/10.1007/s00198-015-3189-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-015-3189-8