Abstract
Introduction and hypothesis
Our objective was to evaluate the effectiveness of pelvic floor muscle training (PFMT) in reducing overactive bladder (OAB) symptoms in women.
Methods
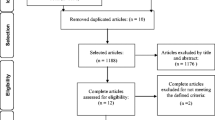
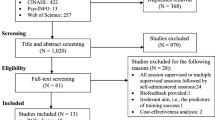
Searches were performed at MEDLINE, PubMed, Physiotherapy Evidence Database (PEDro), Scielo, and Central Cochrane Library PubMed until January 2017. Controlled trials were researched by two independent reviewers. Eligible studies were restricted to random and controlled clinical trials that investigated the effectiveness of PFMT in decreasing OAB symptoms. Qualitative methodology was evaluated using the PEDro scale. Data was analyzed and interpreted qualitatively.
Results
The final search retrieved eight studies (n = 1161 women with urgency symptoms), which were published between 2002 and 2016. The methodological scores varied between 4 and 7 in the PEDro scale. PFMT, with the objective of controlling urgent micturition, demonstrated improvements in quality of life in women with OAB. Most data in this revision came from small- to moderate-sized trials, with different and inconsistent outcome measures, which could have impacted the end results.
Conclusions
The literature regarding the effectiveness of PFMT in OAB remains heterogeneous and inconclusive.

Similar content being viewed by others
Abbreviations
- BFB:
-
Biofeedback
- BT:
-
Bladder training
- CPFR:
-
PFMT + BT: pelvic floor muscle training and combined pelvic floor rehabilitation
- DeCS:
-
Descritores em Ciências da Saúde, Health Science descriptors
- DO:
-
Detrusor overactivity
- DT:
-
Drug therapy
- FES:
-
Functional electrical stimulation
- ICF:
-
International classification of functioning, disability and health
- ICS:
-
International Continence Society
- I-QOL:
-
Incontinence Quality of Life Questionnaire
- ISI:
-
Incontinence Severity Index
- KHQ:
-
King’s Health Questionnaire
- MeSH:
-
Medical Subject Headings of the National Library of Medicine
- MUI:
-
Mixed urinary incontinence
- OAB:
-
Overactive bladder
- PFM:
-
Pelvic floor muscle(s)
- PFMT:
-
Pelvic floor muscle training
- PEDro:
-
Physiotherapy Evidence Database
- PPIU-S:
-
Patient’s Perception of Intensity of Urgency Scale
- RCTs:
-
Randomized controlled trials
- SF-36:
-
Short-Form Health Survey
- SUI:
-
Stress urinary incontinence
- UI:
-
Urinary incontinence
- UUI:
-
Urgency urinary incontinence
- VC:
-
Vaginal cone
References
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, et al. The standardization of terminology of lower urinary tract function: report from the standardization sub-committee of the international continence society. Neurourol Urodyn. 2002;21(2):167–78.
Irwin DE, Kopp ZS, Agatep B, Milsom I, Abrams P. Worldwide prevalence estimates of lower urinary tract symptoms, overactive bladder, urinary incontinence and bladder outlet obstruction. BJU Int. 2011;108(7):1132–8. https://doi.org/10.1111/j.1464-410X.2010.09993.x.
Stewart WF, Van Rooyen JB, Cundiff GW, Abrams P, Herzog AR, Corey R, et al. Prevalence and burden of overactive bladder in the United States. World J Urol. 2003;20:327–36. https://doi.org/10.1007/s00345-002-0301-4.
Staski D, Kelleher C, Avery K, Bosch R, Cotterill N, Coyne K, et al. Initial assessment of urinary and faecal incontinence in adult male and female patients. In: Abrams P, Cardozo L, Khoury S, Wein A, editors. Incontinence. 4th International Consultation on Incontinence (2008), International Continence Society. 4th ed. Paris: Health Publications Ltd; 2009. p. 331–412.
Lapitan MC, Chye PL. The epidemiology of overactive bladder among females in Asia: a questionnaire survey. Int Urogynecol J Pelvic Floor Dysfunct. 2001;12(4):226–31.
Milson Md, Altman D, Cartwright R, Lapitan MC, Nelson R, Sillén U, et al. Epidemiology of Urinary Incontinence (UI) and other Lower Urinary Tract Symptoms (LUTS), Pelvic Organ Prolapse (POP) and Anal Incontinence (AI). In: Abrams P, et al. editors. (2012) Incontinence. 5th International Consultation on Incontinence, International Continence Society, 2013. J et al (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. 5th ed. Paris: Health Publications Ltd; 2012. p. 15–108.
Gormley EA, Lightner DJ, Burgio KL, Chai TC, Quentin Clemens J, Culkin DJ. Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. Am Urol Assoc Educ Res. 2012;188:2455–63. https://doi.org/10.1016/j.juro.2012.09.079.
Dumoulin C, Hay-Smith J, Habée-Séguin GM, Mercier J. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women: a short version Cochrane systematic review with meta-analysis. Neurourol Urodyn. 2014;34(4):300–8. https://doi.org/10.1002/nau.22700.
Burgio KL, Whitehead WE, Engel BT. Urinary incontinence in the elderly. Bladder-sphincter biofeedback and toileting skills training. Ann Intern Med. 1985;103(4):507–15.
Shafik A, Shafik IA. Overactive bladder inhibition in response to pelvic floor muscle exercises. World J Urol. 2003;20(6):374–7.
Groat WC. A neurologic basis for the overactive bladder. Urology. 1997;50(6A Suppl):36–52. discussion 53-6.
Dumoulin C, Hay-Smith J. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. Cochrane Database Syst Rev. CD005654. 2010. https://doi.org/10.1002/14651858.CD005654.pub2.
Sand PK, Goldberg RP, Dmochowski RR, McIlwain M, Dahl NV. The impact of the overactive bladder syndrome on sexual function: a preliminary report from the multicenter assessment of transdermal therapy in overactive bladder with oxybutynin trial. Am J Obstet Gynecol. 2006;195(6):1730–5. https://doi.org/10.1016/j.ajog.2006.08.013.
Berghmans B, Waalwijk V, Van Doorn E, Nieman F, De Bie R, Van den Brandt P, et al. Efficacy of physical therapeutic modalities in women with proven bladder overactivity. Eur Urol. 2002;41(6):581–7.
Greer JA, Smith AL, Arya LA. Pelvic floor muscle training for urgency urinary incontinence in women: a systematic review. Int Urogynecol J. 2012;23:687–97. https://doi.org/10.1007/s00192-011-1651-5.
Burgio KL, Goode PS, Locher JL, Umlauf MG, Roth DL, Richter HE, et al. Behavioral training with and without biofeedback in the treatment of urge incontinence in older women: a randomized controlled trial. JAMA. 2002;288(18):2293–9.
Millard RJ. Clinical efficacy of tolterodine with or without a simplified pelvic floor exercise regimen. Neurourol Urodyn. 2004;23(1):48–53. https://doi.org/10.1002/nau.10167.
Kafri R, Langer R, Dvir Z, Katz-Leurer M. Rehabilitation vs drug therapy for urge urinary incontinence: short-term outcome. Int Urogynecol J. 2007;18(4):407–11. https://doi.org/10.1007/s00192-006-0163-1.
Arruda MR, Castro RA, Sousa GC, Sartori MG, Baracat EC, Girão MJ. Prospective randomized comparison of oxybutynin, functional electrostimulation, and pelvic floor training for treatment of detrusor overactivity in women. Int Urogynecol J. 2008;19(8):1055–61. https://doi.org/10.1007/s00192-008-0586-y.
Kafri R, Deutscher D, Shames J, Golombp J, Melzer I. Randomized trial of a comparison of rehabilitation or drug therapy for urgency urinary incontinence: 1-year follow-up. Int Urogynecol J. 2013;24(7):1181–9. https://doi.org/10.1007/s00192-012-1992-8.
Yuce T, Dökmeci F, Çetinkaya SE. A prospective randomized trial comparing the use of tolterodine or weighted vaginal cones in women with overactive bladder syndrome. Eur J Obstet Gynecol Reprod Biol. 2016;197:91–7. https://doi.org/10.1016/j.ejogrb.2015.11.034.
Voorham CJ, Wachter SD, Van de Bos TWL, Putter H, Nijeholt GAL, Voorham PJ. The effect of EMG biofeedback assisted pelvic floor muscle therapy on symptoms of the overactive bladder syndrome in women: a randomized controlled trial. Neurourol Urodyn. 2016;36(7):1796–803. https://doi.org/10.1002/nau.23180.
Moseley AM, Herbert RD, Sherrington C, Maher CG. Evidence for physiotherapy practice: a survey of the physiotherapy evidence database (PEDro). Aust J Physiother. 2002;48(1):43–9.
Van Tulder M, Furlan A, Bombardier C, Bouter L, the Editorial Board of the Cochrane Collaboration Back Review Group. Updated method guidelines for systematic reviews in the Cochrane collaboration back review group. Spine. 2003;28(12):1290–9. https://doi.org/10.1097/01.BRS.0000065484.95996.AF.
Wang AC, Wang YY, Chen MC. Single-blind, randomized trial of pelvic floor muscle training, biofeedback-assisted pelvic floor muscle training, and electrical stimulation in the management of overactive bladder. Urology. 2004;63(1):61–6. https://doi.org/10.1016/j.urology.2003.08.047.
Lai HH, Rawal A, Shen B, Vetter J. The relationship between anxiety and overactive bladder or urinary incontinence symptoms in the clinical population. Urol J. 2016;98:50–7. https://doi.org/10.1016/j.urology.2016.07.013.
World Health Organization / PAHO. CIF international classification of functioning, disability and health. 1st ed. São Paulo: EdUSP; 2003. p. 37–8.
Hay Smith J, Berghmans B, Burgio K, Dumoulin C, Hagen S, Moore K, et al. Adult conservative management. In: Abrams P, Cardozo L, Khoury S, Wein A, editors. Incontinence, 4th international consultation on incontinence. 4th ed. Paris: Health Publications Ltd; 2009. p. 1027–120.
Bø K, Berghmans B, Morkved S, Van Kampen M. Evidence-based physical therapy for the pelvic floor: bridging science and clinical practice. 2nd ed. Edinburgh: Churchill Livingstone; 2015. p. 111–30.
American College of Sports Medicine. Position stand progression models in resistance training for healthy adults. Med Sci Sports Exerc. 2009;41(3):687–708. https://doi.org/10.1249/MSS.0b013e3181915670.
Salvatore S, Delancey J, Igawa Y, Koelbl H, Laterza RM, Serati M, et al. Pathophysiology of urinary incontinence, fecal incontinence and pelvic organ prolapse. In: Abrams P, Cardozo L, Wagg A, Wein A, editors. Incontinence. 6th International Consultation on Incontinence (2016), International Continence Society, 6th ed. Paris: Health Publications Ltd; 2017. p. 365–66.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Electronic supplementary material
ESM 1
(DOCX 16 kb)
Rights and permissions
About this article
Cite this article
Monteiro, S., Riccetto, C., Araújo, A. et al. Efficacy of pelvic floor muscle training in women with overactive bladder syndrome: a systematic review. Int Urogynecol J 29, 1565–1573 (2018). https://doi.org/10.1007/s00192-018-3602-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-018-3602-x