Abstract
Introduction and hypothesis
Urinary Incontinence (UI) in women is a condition that becomes more common with age. Pelvic floor muscle training (PFMT) is recommended as a first option of treatment for women with symptoms of stress urinary incontinence (SUI), mixed urinary incontinence (MUI), and for some with symptoms of urge urinary incontinence (UUI). PFMT can be performed in groups, individually, and at home, and there is no consensus as to which of the approaches is more efficient for the conservative treatment of UI. The objective was to perform a systematic review comparing the effects of group PFMT vs individual or home training in the treatment of women with UI.
Methods
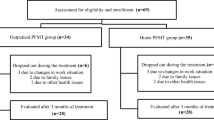
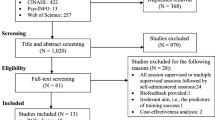
Cochrane’s recommendations for systematic reviews were followed. The inclusion criteria were that the studies had been carried out in adult women who suffered from UI and who underwent PFMT in a group.
Results
Ten studies that fit the criteria previously mentioned were included in this systematic review. The meta-analysis showed that there was no difference when comparing PFMT in groups vs individual PFMT. However, when comparing PFMT in groups vs PFMT at home, the group intervention was more efficient in the treatment of UI.
Conclusion
PFMT is an efficient technique for the improvement of the symptoms of female UI. When PFMT was supervised by a physiotherapist, no significant difference was noted when comparing group with individual approaches.




Similar content being viewed by others
References
Haylen B, Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, et al. An international urogynecological association (IUGA)/international continence society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21(1):5–26.
Irwin DE, Koop ZS, Agatep B, Milsom I, Abrams P. Worldwide prevalence estimates of lower urinary tract symptoms, overactive bladder, urinary incontinence and bladder outlet obstruction. BJU Int. 2011;108(7):1132–9.
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, et al. The standardization of terminology of lower urinary tract function: report from the Standardization Sub-committee of the International Continence Society. Am J Obstet Gynecol. 2002;187(1):116–26.
Lukacz ES, Whitcomb E, Lawrence JM, Nager CW, Contreras R, Luber KM. Are sexual activity and satisfaction affected by pelvic floor disorders? analysis of a community based survey. Am J Obstet Gynecol. 2007;197(1):88.e1–6.
Dedicação AC, Haddad M, Saldanha MÊS, Driusso P. Comparação da qualidade de vida nos diferentes tipos de incontinência urinária feminina. Rev Bras Fis. 2009;13(2):116–22.
Dumoulin C, Hay-Smith EJC, Mac Habée-Séguin G (2014) Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. Cochrane Database Syst Rev 5:CD005654
Ferreira M, Santos P. Pelvic floor muscle training programmes: a systematic review. Acta Med Port. 2011;24(2):309–18.
Luginbuehl H, Baeyens JP, Taeymans J, Maeder IM, Kuhn A, Lorenz R. Pelvic floor muscle activation and strength components influencing female urinary continence and stress incontinence: a systematic review. Neurourol Urodyn. 2015;34(6):498–506.
Hay-Smith J, Herderschee R, Dumoulin C, Herbison GP. Comparisons of approaches to pelvic floor muscle training for urinary incontinence in women: an abridged Cochrane systematic review. Eur J Phys Rehabil Med. 2012;48(4):689–705.
Moroni RM, Magnani PS, Haddad JM, Castro RA, Brito LGO. Conservative treatment of stress urinary incontinence: a systematic review with meta-analysis of randomized controlled trials. Rev Bras Ginecol Obstet. 2016;38(97):97–111.
Higgins J, Green S. Cochrane handbook for systematic reviews of interventions 5.0. The Cochrane Collaboration, 2011. Available from www.handbook.cochrane.org
Demain S, Smith JF, Hiller L, Dziedzic K. Comparison of group and individual physiotherapy for female urinary incontinence in primary care: pilot study. Physiotherapy. 2001;87(5):235–42.
Janssen CCM, Lagro-Janssen ALM, Felling AJA. The effects of physiotherapy for female urinary incontinence: individual compared with group treatment. BJU Int. 2001;87(3):201–6.
Konstantinidou E, Apostolidis A, Kondelidis N, Tsimtsiou Z, Hatzichristou D, Ioannides E. Short-term efficacy of group pelvic floor training under intensive supervision versus unsupervised home training for female stress urinary incontinence: a randomized pilot study. Neurourol Urodyn. 2007;26(4):486–91.
Zanetti MR, Castro RA, Rotta AL, Santos PD, Santori M, Girão MJB. Impact of supervised physiotherapeutic pelvic floor exercises for treating female stress urinary incontinence. Sao Paulo Med J. 2007;125(5):265–9.
Lamb SE, Pepper J, Lall R, Jørstad-Stein EC, Clark MD, Hill L, et al. Group treatments for sensitive health care problems: a randomized controlled trial of group versus individual physiotherapy sessions for female urinary incontinence. BMC Womens Health. 2009;9(1):26.
Camargo FO, Rodrigues AM, Arruda RM, Sartori MGF, Girão MJB, Castro RA. Pelvic floor muscle training in female stress urinary incontinence: comparison between group training and individual treatment using PERFECT assessment scheme. Int Urogynecol J. 2009;20:1455–62.
Felicíssimo MF, Carneiro MM, Saleme CS, Pinto RZ, Fonseca AMRM, Silva-Filho AL. Intensive supervised versus unsupervised pelvic floor muscle training for the treatment of stress urinary incontinence: a randomized comparative trial. Int Urogynecol J. 2010;21:835–40.
Pereira VS, Correia GN, Driusso P. Individual and group pelvic floor muscle training versus no treatment in female stress urinary incontinence: a randomized controlled pilot study. Eur J Obstet Gynecol Reprod Biol. 2011;159:465–71.
Nascimento-Correia G, Santos-Pereira V, Tahara N, Driusso P. Effects of pelvic floor muscle training on quality of life of a group of women with urinary incontinence: randomized controlled trial. Actas Urol Esp. 2012;36(4):216–21.
Soni K, Soni H, Desai D, Shah C, Patel H. Randomized controlled trial of group versus individual physiotherapy sessions for genuine stress incontinence in women. Indian J Physiother Occup Ther. 2013;7(1):110–5.
Figueiredo EM, Cruz MC. Avaliação funcional do assoalho pélvico feminino. In: Baracho E, editor. Fisioterapia aplicada à saúde da mulher. 5th ed. Rio de Janeiro: Guanabara Koogan; 2012. p. 231–41.
Bø K, Sherburn M. Evaluation of female pelvic-floor muscle function and strength. Phys Ther. 2005;85:269–82.
Dumoulin C, Hay-Smith J, Seguin GMH, Mercier J. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women: a short version Cochrane systematic review with meta-analysis. Neurourol Urodyn. 2015;34:300–8.
Ferreira M, Santos P. Princípios da fisiologia do exercício no treino dos músculos do pavimento pélvico. Acta Urol. 2009;26(3):31–8.
Abrams P, Andersson KE, Birder L, Brubaker L, Cardozo L, Chapple C, et al. Fourth international consultation on incontinence recommendations of the international scientific committee: evaluation and treatment of urinary incontinence, pelvic organ prolapse, and fecal incontinence. Neurourol Urodyn. 2010;29(1):213–40.
Bø K, Talseth T, Holme I. Single blind, randomised controlled trial of pelvic floor exercises, electrical stimulation, vaginal cones, and no treatment in management of genuine stress incontinence in women. BMJ. 1999;318:487–93.
Garber CE, Blissmer B, Deschenes MR, Franklin BA, Lamonte MJ, Lee IM, et al. American college of sports medicine position stand. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: guidance for prescribing exercise. Med Sci Sports Exerc. 2011;43(7):1334–59.
Hay-Smith J, Herderschee R, Dumoulin C, Herbison GP. Comparisons of approaches to pelvic floor muscle training for urinary incontinence in women. Cochrane Database Syst Rev. 2011;12:CD009508.
Berzuk K, Shay B. Effect of increasing awareness of pelvic floor muscle function on pelvic floor dysfunction: a randomized controlled trial. Int Urogynecol J. 2015;26(6):837–44.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Paiva, L.L., Ferla, L., Darski, C. et al. Pelvic floor muscle training in groups versus individual or home treatment of women with urinary incontinence: systematic review and meta-analysis. Int Urogynecol J 28, 351–359 (2017). https://doi.org/10.1007/s00192-016-3133-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-016-3133-2