Abstract
Introduction and hypothesis
The aim of present study was to compare pelvic floor morphology and function in women with and without major defects of the pubovisceral muscle.
Methods
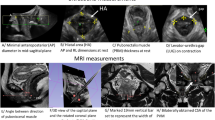
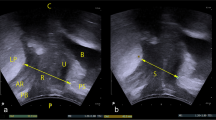
One hundred fifty-seven women with pelvic organ prolapse participated in this cross-sectional study. Participants answered a symptom questionnaire and underwent clinical and three- and four-dimensional transperineal ultrasound examination. Pelvic floor muscle maximum voluntary contraction (MVC), endurance, and resting vaginal pressure were registered with a vaginal balloon catheter. Offline analyses were performed for the presence of major pubovisceral muscle defects (PVMD) and hiatal dimensions.
Results
The levator hiatus dimensions at rest and contraction were significantly larger in women with than without major PVMD. Mean differences in levator hiatus area between women with and without major PVMD were: rest 1.9 cm2 95% confidence intervals (CI) 0.21–3.7, P = 0.028 and contraction 2.75 cm2 95% CI 1.0–4.5, P =0.002; and Valsalva maneuver mean difference was 0.82 cm2 95% CI 2.18–3.83, P = 0.543. Women with major PVMD had lower MVC and endurance measurements as compared with women without major PVMD, but the differences were not statistically significant.
Conclusions
Women with major pubovisceral muscle defects have larger hiatal dimensions at rest and at contraction than women without PVMD. We were unable to prove the corresponding relationship for hiatal dimensions on Valsalva.


Similar content being viewed by others
References
Nygaard I, Barber MD, Burgio KL, Kenton K, Meikle S, Schaffer J et al (2008) Prevalence of symptomatic pelvic floor disorders in US women. JAMA 300:1311–1316
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89:501–506
Dietz HP, Shek C, Clarke B (2005) Biometry of the pubovisceral muscle and levator hiatus by three-dimensional pelvic floor ultrasound. Ultrasound Obstet Gynecol 25:580–585
Kearney R, Miller JM, DeLancey JOL (2006) Interrater reliability and physical examination of the pubovisceral portion of the levator ani muscle, validity comparisons using MR imaging. Neurourol Urodyn 25:50–54
Delancey JO (1994) The anatomy of the pelvic floor. Curr Opin Obstet Gynecol 6:313–316
DeLancey JOL, Kearney R, Chou Q, Speights S, Binno S (2003) The appearance of levator ani muscle abnormalities in magnetic resonance images after vaginal delivery. Obstet Gynecol 101:46–53
Dietz HP, Simpson JM (2008) Levator trauma is associated with pelvic organ prolapse. BJOG 115:979–984
Knuttgen HG, Kraemer WJ (1987) Terminology and measurement in exercise performance. J Appl Sport Sci Res 1:1–10
Bo K, Sherburn M (2005) Evaluation of female pelvic-floor muscle function and strength. Phys Ther 85:269–282
Braekken IH, Majida M, Engh ME, Bo K (2010) Pelvic floor muscle strength, endurance and vaginal resting pressure are positively associated with muscle thickness, size of levator hiatus and position of the bladder in women with prolapse stage I, Ii and Iii. A 3D/4D ultrasound study. Neurourol Urodyn 29:1167–1168
Majida M, Braekken I, Bo K, Benth J, Engh M (2011) Anterior but not posterior compartment prolapse is associated with levator hiatus area: a three- and four-dimensional transperineal ultrasound study. BJOG 118:329–337
Braekken IH, Majida M, Ellstrom EM, Holme IM, Bo K (2009) Pelvic floor function is independently associated with pelvic organ prolapse. BJOG 116:1706–1714
Braekken IH, Majida M, Engh ME, Bo K (2010) Can pelvic floor muscle training reverse pelvic organ prolapse and reduce prolapse symptoms? An assessor-blinded, randomized, controlled trial. Am J Obstet Gynecol 203(2):170.e1–170.e7
Orno AK, Dietz HP (2007) Levator co-activation is a significant confounder of pelvic organ descent on Valsalva maneuver. Ultrasound Obstet Gynecol 30:346–350
Dietz HP, Bernardo MJ, Kirby A, Shek KL (2010) Minimal criteria for the diagnosis of avulsion of the puborectalis muscle by tomographic ultrasound. Int Urogynecol J Pelvic Floor Dysfunct 22(6):699–704
Dietz HP, Abbu A, Shek KL (2008) The levator-urethra gap measurement: a more objective means of determining levator avulsion? Ultrasound Obstet Gynecol 32:941–945
Majida M, Braekken IH, Umek W, Bo K, Saltyte BJ, Ellstrom EM (2009) Interobserver repeatability of three- and four-dimensional transperineal ultrasound assessment of pelvic floor muscle anatomy and function. Ultrasound Obstet Gynecol 33:567–573
Mouritsen L, Larsen JP (2003) Symptoms, bother and POPQ in women referred with pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 14:122–127
Bump RC, Mattiasson A, Bo K, Brubaker LP, DeLancey JOL, Klarskov P et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Abdool Z, Shek KL, Dietz HP (2009) The effect of levator avulsion on hiatal dimension and function. Am J Obstet Gynecol 201:89.e1–5
Steensma AB, Konstantinovic ML, Burger CW, de RD, Timmerman D, Deprest J (2010) Prevalence of major levator abnormalities in symptomatic patients with an underactive pelvic floor contraction. Int Urogynecol J Pelvic Floor Dysfunct 21:861–867
Barber EL, Lundsberg LS, Belanger K, Pettker CM, Funai EF, Illuzzi JL (2011) Indications contributing to the increasing cesarean delivery rate. Obstet Gynecol 118:29–38
Kolas TF, Hofoss DF, Daltveit AK, Nilsen ST, Henriksen TF, Hager RF, et al. Indications for cesarean deliveries in Norway. Am J Obstet Gynecol 188(4):864–870
Delancey JO, Morgan DM, Fenner DE, Kearney R, Guire K, Miller JM et al (2007) Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obstet Gynecol 109:295–302
Kruger JA, Heap SW, Murphy BA, Dietz HP (2010) How best to measure the levator hiatus: evidence for the non-Euclidean nature of the ‘plane of minimal dimensions’. Ultrasound Obstet Gynecol 36:755–758
Dietz HP, Shek C (2008) Levator avulsion and grading of pelvic floor muscle strength. Int Urogynecol J Pelvic Floor Dysfunct 19:633–636
Weinstein MM, Jung SA, Pretorius DH, Nager CW, den Boer DJ, Mittal RK (2007) The reliability of puborectalis muscle measurements with 3-dimensional ultrasound imaging. Am J Obstet Gynecol 197:68–6
Acknowledgments
The study was funded by South-Eastern Norwegian Regional Health Authority and strategic research funds from Akershus University Hospital.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Majida, M., Brækken, I.H., Bø, K. et al. Levator hiatus dimensions and pelvic floor function in women with and without major defects of the pubovisceral muscle. Int Urogynecol J 23, 707–714 (2012). https://doi.org/10.1007/s00192-011-1652-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-011-1652-4