Abstract
Purpose
UKA has higher revision risk, particularly for lower volume surgeons. While robotic-arm assisted systems allow for increased accuracy, introduction of new systems has been associated with learning curves. The aim of this study was to determine the learning curve of a UKA robotic-arm assisted system. The hypothesis was that this may affect operative times, patient outcomes, limb alignment, and component placement.
Methods
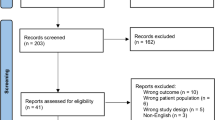
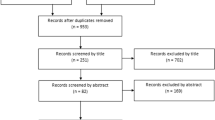
Between 2017 and 2021, five surgeons performed 152 consecutive robotic-arm assisted primary medial UKA, and measurements of interest were recorded. Patient outcomes were measured with Oxford Knee Score, EuroQol-5D, and Forgotten Joint Score at 6 weeks, 1 year, and 2 years. Surgeons were grouped into ‘low’ and ‘high’ usage groups based on total UKA (manual and robotic) performed per year.
Results
A learning curve of 11 cases was found with operative time (p < 0.01), femoral rotation (p = 0.02), and insert sizing (p = 0.03), which highlighted areas that require care during the learning phase. Despite decreased 6-week EQ-5D-5L VAS in the proficiency group (77 cf. 85, p < 0.01), no difference was found with implant survival (98.2%) between phases (p = 0.15), or between ‘high’ and ‘low’ usage surgeons (p = 0.23) at 36 months. This suggested that the learning curve did not lead to early adverse effects in this patient cohort.
Conclusion
Introduction of a UKA robotic-arm assisted system showed learning curves for operative times and insert sizing but not for implant survival at early follow-up. The short learning curve regardless of UKA usage indicated that robotic-arm assisted UKA may be particularly useful for low-usage surgeons.
Level of evidence
Level III, Retrospective cohort study.





Similar content being viewed by others
References
Akagi M, Oh M, Nonaka T, Tsujimoto H, Asano T, Hamanishi C (2004) An Anteroposterior axis of the tibia for total knee arthroplasty. Clin Orthop Relat Res. https://doi.org/10.1097/00003086-200403000-00030
Australian Orthopaedic Association (2019) Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR). Hip, Knee & Shoulder Arthroplasty: 2019 Annual Report. Adelaide, AUS. https://aoanjrr.sahmri.com/. Accessed 7 July 2020
Banger M, Doonan J, Rowe P, Jones B, MacLean A, Blyth MJB (2021) Robotic arm-assisted versus conventional medial unicompartmental knee arthroplasty: five-year clinical outcomes of a randomized controlled trial. Bone Jt J. https://doi.org/10.1302/0301-620X.103B6.BJJ-2020-1355.R2
Batailler C, Bordes M, Lording T, Nigues A, Servien E, Calliess T, Lustig S (2021) Improved sizing with image-based robotic-assisted system compared to image-free and conventional techniques in medial unicompartmental knee arthroplasty. Bone Jt J. https://doi.org/10.1302/0301-620X.103B4.BJJ-2020-1453.R1
Beard DJ, Davies LJ, Cook JA, MacLennan G, Price A, Kent S, Hudson J, Carr A, Leal J, Campbell H, Fitzpatrick R, Arden N, Murray D, Campbell MK, Barker K, Murray G, Simpson H, Dodwell D, Donell S, Warner K (2019) The clinical and cost-effectiveness of total versus partial knee replacement in patients with medial compartment osteoarthritis (TOPKAT): 5-year outcomes of a randomised controlled trial. Lancet 394:746–756
Behrend H, Giesinger K, Giesinger JM, Kuster MS (2012) The ‘forgotten joint’ as the ultimate goal in joint arthroplasty. Validation of a new patient-reported outcome measure. J Arthroplasty 27:430-436.e1
Bell SW, Frcs T, Anthony I, Jones B, Frcs T, Maclean A, Frcs T, Rowe P, Blyth M, Frcs T (2016) Improved accuracy of component positioning. J Bone Jt Surg 98:627–635
Bergeson AG, Berend KR, Lombardi AV, Hurst JM, Morris MJ, Sneller MA (2013) Medial mobile bearing unicompartmental knee arthroplasty. Early survivorship and analysis of failures in 1000 consecutive cases. J Arthroplasty 28:172–175
Bini S, Khatod M, Cafri G, Chen Y, Paxton EW (2013) Surgeon, implant, and patient variables may explain variability in early revision rates reported for unicompartmental arthroplasty. J Bone Jt Surg. https://doi.org/10.2106/JBJS.L.01006
Clement ND, MacDonald D, Simpson AHRW (2014) The minimal clinically important difference in the Oxford knee score and short form 12 score after total knee arthroplasty. Knee Surg Sport Traumatol Arthrosc 22:1933–1939
Collier MB, Eickmann TH, Sukezaki F, McAuley JP, Engh GA (2006) Patient, implant, and alignment factors associated with revision of medial compartment unicondylar arthroplasty. J Arthroplasty 21:108–115
Gaudiani MA, Nwachukwu BU, Baviskar JV, Sharma M, Ranawat AS (2017) Optimization of sagittal and coronal planes with robotic-assisted unicompartmental knee arthroplasty. Knee 24:837–843
Gilmour A, MacLean AD, Rowe PJ, Banger MS, Donnelly I, Jones BG, Blyth MJG (2018) Robotic-arm–assisted vs conventional unicompartmental knee arthroplasty. The 2-year clinical outcomes of a randomized controlled trial. J Arthroplasty 33:S109–S115
Goodfellow J, O’Connor J, Pandit H, Dodd C, Murray D (2011) Unicompartmental arthroplasty with the Oxford knee. Goodfellow Publishers Ltd, Woodeaton
Hamilton WG, Ammeen D, Engh CA, Engh GA (2010) Learning curve with minimally invasive unicompartmental knee arthroplasty. J Arthroplasty 25:735–740
Harris IA, Cashman K, Lorimer M, Peng Y, Ackerman I, Heath E, Graves SE (2021) Are responders to patient health surveys representative of those invited to participate? An analysis of the patient-reported outcome measures pilot from the Australian orthopaedic association national joint replacement registry. PLoS ONE 16:1–11
Herdman M, Gudex C, Lloyd A, Janssen M, Kind P, Parkin D, Bonsel G, Badia X (2011) Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Qual Life Res 20:1727–1736
Hernigou P, Deschamps G (2004) Alignment influences wear in the knee after medial unicompartmental arthroplasty. Clin Orthop Relat Res. https://doi.org/10.1097/01.blo.0000128285.90459.12
Inui H, Yamagami R, Kono K, Kawaguchi K, Taketomi S, Tanaka S (2021) Prosthetic alignment and clinical outcomes of navigation-assisted unicompartmental knee arthroplasty by an experienced surgeon compared with inexperienced surgeons. J Arthroplasty 36:2435–2439
Kayani B, Konan S, Huq SS, Tahmassebi J, Haddad FS (2019) Robotic-arm assisted total knee arthroplasty has a learning curve of seven cases for integration into the surgical workflow but no learning curve effect for accuracy of implant positioning. Knee Surg Sport Traumatol Arthrosc 27:1132–1141
Kayani B, Konan S, Pietrzak JRT, Huq SS, Tahmassebi J, Haddad FS (2018) The learning curve associated with robotic-arm assisted unicompartmental knee arthroplasty. Bone Jt J 100B:1033–1042
Kayani B, Konan S, Tahmassebi J, Rowan FE, Haddad FS (2019) An assessment of early functional rehabilitation and hospital discharge in conventional versus robotic-arm assisted unicompartmental knee arthroplasty. Bone Jt J 101B:24–33
Kazarian GS, Barrack TN, Okafor L, Barrack RL, Nunley RM, Lawrie CM (2020) High prevalence of radiographic outliers and revisions with unicompartmental knee arthroplasty. J Bone Jt Surg Am 102:1151–1159
Klasan A, Carter M, Holland S, Young SW (2020) Low femoral component prominence negatively influences early revision rate in robotic unicompartmental knee arthroplasty. Knee Surg Sport Traumatol Arthrosc 28:3906–3911
Klasan A, Parker DA, Lewis PL, Young SW (2021) Low percentage of surgeons meet the minimum recommended unicompartmental knee arthroplasty usage thresholds: analysis of 3037 Surgeons from Three National Joint Registries. Knee Surg Sport Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06437-7 (Advance online publication)
Klasan A, Tay ML, Frampton C, Young SW (2021) High usage of medial unicompartmental knee arthroplasty negatively influences total knee arthroplasty revision rate. Knee Surg Sport Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06650-4 (Advance online publication)
Koh CK, Zeng I, Ravi S, Zhu M, Vince KG, Young SW (2017) Periprosthetic joint infection is the main cause of failure for modern knee arthroplasty: an analysis of 11,134 knees. Clin Orthop Relat Res 475:2194–2201
Kozinn SC, Scott R (1989) Current concepts review: unicondylar knee arthroplasty. J Bone Jt Surg Ser A 71-A:145–150
Liddle AD, Judge A, Pandit H, Murray DW (2014) Adverse outcomes after total and unicompartmental knee replacement in 101330 matched patients: a study of data from the National Joint Registry for England and Wales. Lancet 384:1437–1445
Millar LJ, Banger M, Rowe PJ, Blyth M, Jones B, Maclean A (2018) A five-year follow up of gait in robotic assisted vs conventional unicompartmental knee arthroplasty. Gait Posture 65:31–32
Mittal A, Meshram P, Kim WH, Kim TK (2020) Unicompartmental knee arthroplasty, an enigma, and the ten enigmas of medial UKA. J Orthop Traumatol 21:15–23
Mofidi A, Plate JF, Lu B, Conditt MA, Lang JE, Poehling GG, Jinnah RH (2014) Assessment of accuracy of robotically assisted unicompartmental arthroplasty. Knee Surg Sport Traumatol Arthrosc 22:1918–1925
Murray DW, Fitzpatrick R, Rogers K, Pandit H, Beard DJ, Carr AJ, Dawson J (2007) The use of the Oxford hip and knee scores. J Bone Jt Surg Ser B 89:1010–1014
National Joint Registry (2019) National joint registry for England, wales, northern Ireland and the isle of man: 16th annual report 2019. Hemel Hempstead
New Zealand Orthopaedic Association (2019) The New Zealand Joint Registry Twenty-one Year Report January 1999 to December 2019. https://nzoa.org.nz/nzoa-joint-registry. Accessed 22 Apr 2020
Noticewala MS, Geller JA, Lee JH, Macaulay W (2012) Unicompartmental knee arthroplasty relieves pain and improves function more than total knee arthroplasty. J Arthroplasty 27:99–105
Pearle AD, van der List JP, Lee L, Coon TM, Borus TA, Roche MW (2017) Survivorship and patient satisfaction of robotic-assisted medial unicompartmental knee arthroplasty at a minimum two-year follow-up. Knee 24:419–428
Tay ML, McGlashan SR, Monk AP, Young SW (2021) Revision indications for medial unicompartmental knee arthroplasty: a systematic review. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-021-03827-x (Advance online publication)
Vermue H, Lambrechts J, Tampere T, Arnout N, Auvinet E, Victor J (2020) How should we evaluate robotics in the operating theatre? Bone Jt J. https://doi.org/10.1302/0301-620X.102B4.BJJ-2019-1210.R1
Vermue H, Luyckx T, Winnock de Grave P, Ryckaert A, Cools AS, Himpe N, Victor J (2020) Robot-assisted total knee arthroplasty is associated with a learning curve for surgical time but not for component alignment, limb alignment and gap balancing. Knee Surg Sport Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06341-6 (Advance online publication)
Whittaker JP, Dwyer KA, Howard J, Huey V, Lesko J, Nunley RM, Verdonk P (2018) Learning curve with a new primary total knee arthroplasty implant: a multicenter perspective with more than 2000 patients. Arthroplast Today 4:348–353
Willis-Owen CA, Brust K, Alsop H, Miraldo M, Cobb JP (2009) Unicondylar knee arthroplasty in the UK National Health Service: an analysis of candidacy, outcome and cost efficacy. Knee 16:473–478
Wilson HA, Middleton R, Abram SGF, Smith S, Alvand A, Jackson WF, Bottomley N, Hopewell S, Price AJ (2019) Patient relevant outcomes of unicompartmental versus total knee replacement: systematic review and meta-analysis. BMJ 364:1–17
Zhang Q, Zhang Q, Guo W, Liu Z, Cheng L, Yue D, Zhang N (2014) The learning curve for minimally invasive Oxford phase 3 unicompartmental knee arthroplasty: cumulative summation test for learning curve (LC-CUSUM). J Orthop Surg Res 9:1–9
Acknowledgements
The authors would like to thank Dr. Sherina Holland for assistance with data collection and Mr. Greg Gamble for statistical advice for this study. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
MLT, SWY, and MC conceived this research and participated in concept and study methodology design. MLT, MC, and NZ performed data collection and data validation. MLT performed data analysis. MLT, SMB, and SWY participated in interpretation of the data. MLT wrote the original draft and all authors reviewed manuscript and participated in revisions. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
SWY receives research support and is a paid consultant for Stryker Orthopaedics NZ. MC is a senior product specialist at Stryker Orthopaedics. These affiliations did not influence study design or data collection, analysis, or interpretation of data. Stryker Orthopaedics did not influence any decisions for manuscript preparation or publication. MLT, SMB, and NZ declare no conflict of interest.
Ethical approval
This study received ethics approval from the national New Zealand Health and Disability Ethics Committees (17/NTB/174) and the local institution.
Informed consent
Participants included in this study were informed of, and provided consent for, the collection and use of their data for the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tay, M.L., Carter, M., Bolam, S.M. et al. Robotic-arm assisted unicompartmental knee arthroplasty system has a learning curve of 11 cases and increased operating time. Knee Surg Sports Traumatol Arthrosc 31, 793–802 (2023). https://doi.org/10.1007/s00167-021-06814-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06814-2