Abstract
Purpose
We hypothesized that the individual bone geometry is the most important variable to achieve acceptable soft tissue balancing during total knee arthroplasty.
Methods
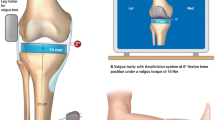
Long-standing 3-foot films and computer navigation data from 90 patients with varus (n = 45) or valgus deformity (n = 45) were utilized who underwent navigated total knee arthroplasty. Mean age was 65 ± 8 years with 50 women and 40 men. Hip-knee-ankle angle (HKA) was measured and ranged from 23° varus to 21.5° of valgus. Three additional measurements were made: lateral distal femoral angle (DFA), the intraarticular angle (IAA), and the medial proximal tibial angle (PTA). Intra-operative computer navigation data were obtained. Knees were then stressed with both a maximum varus/valgus moment in 10° flexion. Values were compared with the angle measurements of 3-foot films. Maximum varus/valgus measurements were correlated with HKA for both varus and valgus knees.
Results
Varus knees: Mean HKA measured 9° ± 5°, and the maximum varus stress measured intraoperatively was 12° ± 4°. The mean DFA, PTA, and IAA were 88° ± 2.5°, 84° ± 3.4°, and 4.5° ± 2.5°, respectively. If the HKA was <10°, the deformity was correctable in (16/26) 61 % of cases. Positive correlation exists between the HKA, and maximal varus stress obtained intraoperatively (r = 0.75, p < 0.0001). IAA correlated with increasing HKA (r = 0.80, p < 0.0001). Mean IAA was significantly greater in the varus than valgus group (4.5 ± 2.6 vs 3.2 ± 2.4, respectively, p = 0.01). Valgus knees: Mean HKA measured was 9.4° ± 4°. The mean DFA, PTA, and IAA were 83° ± 2°, 89.5° ± 2°, and 3.2° ± 2.4°, respectively. If the HKA was more than 10°, maximal varus stress of the knee was able to correct the valgus deformity (15/22) 68 % of the time. If the HKA was <10°, the deformity was correctable in (21/23) 91 % of cases. Positive correlation exists between the HKA and maximal valgus stress examination (r = 0.74, p < 0.0001). There was a positive correlation of IAA with increasing HKA (r = 0.61, p < 0.0001). Mean flexion contracture for varus knees was 6.3° ± 6.9° compared with 0.8° ± 7.6° in the valgus group (p = 0.0004).
Conclusion
These data suggest that soft tissues play more of a role in the varus knee deformity than they do in the valgus knee and that the bony contribution may be the main contributing factor to the overall deformity of the valgus knee.
Level of evidence
IV.




Similar content being viewed by others
References
Bellemans J, Vandenneucker H, Vanlauwe J, Victor J (2010) The influence of coronal plane deformity on mediolateral ligament status: an observational study in varus knees. Knee Surg Sports Traumatol Arthrosc 18(2):152–156
Fehring TK, Odum S, Griffin WL, Mason JB, Nadaud M (2001) Early failures in total knee arthroplasty. Clin Orthop Relat Res 392:315–318
Fishkin Z, Miller D, Ritter C, Ziv I (2002) Changes in human knee ligament stiffness secondary to osteoarthritis. J Orthop Res 20(2):204–207
Ishii Y, Noguchi H, Matsuda Y, Kiga H, Takeda M, Toyabe S (2009) Preoperative laxity in osteoarthritis patients undergoing total knee arthroplasty. Int Orthop 33(1):105–109
Kuster MS, Jeffcote BO, Schirm AC, Jacob H, Nicholls RL (2009) Assessment of isometricity before and after total knee arthroplasty: a cadaver study. Knee 16(5):352–357
Matsuda S, Miura H, Nagamine R, Mawatari T, Tokunaga M, Nabeyama R, Iwamoto Y (2004) Anatomical analysis of the femoral condyle in normal and osteoarthritic knees. J Orthop Res 22(1):104–109
Matziolis G, Matziolis D, Perka C (2012) Pre-operative frontal plane malalignment predicts the extension gap asymmetry in knee osteoarthritis. Int Orthop 36(1):79–82
Mulhall KJ, Ghomrawi HM, Scully S, Callaghan JJ, Saleh KJ (2006) Current etiologies and modes of failure in total knee arthroplasty revision. Clin Orthop Relat Res 446:45–50
Okamoto S, Okazaki K, Mitsuyasu H, Matsuda S, Iwamoto Y (2013) Lateral soft tissue laxity increases but medial laxity does not contract with varus deformity in total knee arthroplasty. Clin Orthop Relat Res 471(4):1334–1342
Thienpont E, Paternostre F, Pietsch M, Hafez M, Howell S (2013) Total knee arthroplasty with patient-specific instruments improves function and restores limb alignment in patients with extra-articular deformity. Knee 20(6):407–411
Victor J, Wong P, Witvrouw E, Sloten JV, Bellemans J (2009) How isometric are the medial patellofemoral, superficial medial collateral, and lateral collateral ligaments of the knee? Am J Sports Med 37(10):2028–2036
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
This study has been approved by the appropriate ethics committees and has therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hohman, D.W., Nodzo, S.R., Phillips, M. et al. The implications of mechanical alignment on soft tissue balancing in total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 23, 3632–3636 (2015). https://doi.org/10.1007/s00167-014-3262-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-014-3262-4