Abstract
Objective
To evaluate effects of lung recruitment maneuvers on gastric mucosal perfusion, systemic circulation, and lung mechanics in patients with acute lung injury.
Design
Prospective observational clinical study.
Setting
General intensive care unit of university hospital.
Patients and participants
Fourteen patients with acute lung injury (ten in the main study group and four in a validation group).
Interventions
Three 2-min-long recruitment maneuvers (RM) with transient increases in mean airway pressure to 35 cmH2O (RM1 and RM2) and 44 cmH2O (RM3).
Measurements and results
Measurements of systemic hemodynamics, gastric mucosal perfusion (laser Doppler flowmetry), and lung mechanics were performed immediately before, at the end of, and 3 min after each RM. Cardiac index decreased during all RMs while mean arterial pressure decreased only during RM3. Gastric mucosal perfusion was not significantly changed during any of the RMs. When comparing values obtained before the first RM with values after the third RM there was a significant decrease in cardiac index (P=0.043) and a non-significant (P=0.051) decrease in gastric mucosal perfusion. There were no significant changes in systemic oxygenation or lung mechanics after three RMs, even though four patients showed marked transient increases in systemic oxygenation during RMs.
Conclusions
In this study of ten patients there were no significant changes in gastric mucosal perfusion during lung recruitment maneuvers. There was, however, a trend towards gradual decreases in gastric mucosal perfusion.
Similar content being viewed by others
Introduction
Acute lung injury is an inflammatory disease with increased pulmonary capillary permeability, leading to atelectasis, venous admixture and hypoxia, often necessitating ventilator treatment [1]. This treatment is supportive, with a main goal to keep the patient adequately oxygenated without causing further lung injury and untoward side effects. Different ventilatory approaches to reach this goal have been described [2]. The open lung concept [3], a ventilatory approach consisting of aggressive opening of the lung with recruitment maneuvers (RMs) and high positive end-expiratory pressures (PEEP), has recently been introduced into clinical practice. Recruitment maneuvers are usually performed by intermittent increases in mean airway pressure, induced by increases in PEEP, plateau airway pressure or both. This is supposed to open up and recruit atelectatic lung regions [4]. It is known that sustained increases in mean airway pressure, by increases in PEEP, may induce negative systemic and regional hemodynamic effects [5, 6], that are related to the concurrent intravascular blood volume [7]. Systemic hemodynamic effects include decreased cardiac output and mean arterial pressure, while central venous pressure and systemic vascular resistance increase [5, 8, 9, 10]. Hepatosplanchnic vasoconstriction is a main characteristic during PEEP ventilation [11, 12, 13, 14] while blood flow is maintained to the kidneys, the brain, and the heart [8, 12].
Recruitment maneuvers have been reported to temporarily increase both PaO2 and pulmonary compliance [15, 16, 17, 18]. Systemic hemodynamic effects of recruitment maneuvers, i.e., transient increases in mean airway pressure, include decreased mean arterial pressure and cardiac output [18]. However, regional hemodynamic effects of RMs in ventilator-treated patients with acute lung injury are less well-described. We therefore designed this study with the primary aim to evaluate the hypothesis that three consecutive recruitment maneuvers induce a decrease in gastric mucosal perfusion. Our second aim was to test the hypothesis that three consecutive recruitment maneuvers do not change systemic oxygenation, respiratory mechanics or systemic circulatory parameters.
Materials and methods
Patients
The study protocol was approved by the institutional ethics committee. We included all eligible patients fulfilling the inclusion criteria that came to our knowledge during the period January 2001 to June 2002. Ten intubated ventilator-treated patients (age 58±5 years, APACHE II at admission 22±3) with acute lung injury (ALI) were included in the study. Patient characteristics are described in Table 1. Informed consent was obtained from the next-of-kin of each patient included in the study. Another three patients were not included in the study due to the closest next of kin denying participation. ALI was defined using the following standard criteria: sudden onset of respiratory failure, bilateral infiltrates on the chest X-ray, arterial oxygen tension/fractional inspired oxygen (PaO2/FiO2) less than 300 mmHg (39.9 kPa) and no signs of left ventricular failure [1]. In all patients, left ventricular failure was excluded by echocardiographic examination by an independent clinical physiologist. Patients with unilateral infiltrates on chest X-ray were also included if they otherwise fulfilled the ALI criteria and had a clinical need for alveolar recruitment. Patients admitted to the ICU due to esophageal bleeding, esophageal surgery, gastric surgery or cerebral edema were excluded. Patients were sedated with continuous infusions of midazolam-fentanyl or propofol-fentanyl. All patients were mechanically ventilated in a pressure-controlled mode with an Evita 4 ventilator (Dräger, Germany). PEEP and peak airway pressure levels were set at the discretion of the attending physician. Patients were fasted at least 6 h before entering the study. During the study period all patients were examined in the supine position and paralyzed with cis-atracurium. Esophageal pressure was measured online during the study. If negative deflections in esophageal pressure indicating spontaneous respiratory effort was detected, additional muscle relaxants were given.
Measurements
All pressure transducers (System DPT-6000, PvB, Triplus, Sweden) were calibrated to atmospheric pressure at the level of the right atrium by a saline column. ECG, ventilator gas flow, laser Doppler flowmetry, and all pressures (see below) were continuously recorded using a computer-based multichannel signal acquisition and analysis system (AcqKnowledge III, Biopac systems, USA). The AcqKnowledge software is designed for continuous data collection at 50 Hz, and data for presentation were extracted as mean values established during registration sequences of approximately 30 s.
Systemic hemodynamic parameters
Hemodynamic measurements included registration of heart rate (HR), mean arterial pressure (MAP; through a radial or femoral artery catheter) and central venous pressure (CVP; through an internal jugular or subclavian line). In five patients, monitoring of pulse contour cardiac index via a femoral artery catheter (PICCO system, Pulsion Medical Systems, Germany) was present for clinical reasons. In these five patients, pulse contour cardiac index was recorded at each measuring point according to study protocol. The pulse contour computer continuously computed the arterial pulse contour cardiac index. Calibration of the system was performed according to the manufacturer's instructions by determination of the arterial thermodilution cardiac output, using three to four injections of 15–20 ml room-temperature saline [23].
Gastric mucosal perfusion and abdominal pressure
Gastric mucosal perfusion was continuously measured using laser Doppler flowmetry (LDF) with a specially designed gastric tube fitted with two laser Doppler optical fibers of equal length, terminating at the tip and facing the mucosa perpendicular to the axial line of the gastric tube (probe 415–134, Perimed, Sweden). According to this technique, blood flow is expressed in arbitrary perfusion units (PU), and is described as being equivalent to the number of red blood cells contained in the volume of blood through which the laser light is passing and at the speed at which these cells are moving. Each fiber had a core diameter of 150 μm and a fiber separation of 250 μm. The wavelength of the emitted laser light was 780 nm and the Doppler shift frequency was 20 kHz. The probe was connected to a base unit (PeriFlux 4001 Master, Perimed). Calibration was performed according to the manufacturer's instructions at 0 PU on a plastic disc at optical zero and at 250 PU using a motility standard provided by the manufacturer. The gastric tube was introduced nasally or orally and pushed forward until an adequate signal could be produced. The signal was considered adequate when no visible movement artifacts was observed, when measurements of total backscatter was adequate and when pulse waves and respiratory fluctuations could be identified. The position of the gastric tube was then verified by epigastric auscultation and by X-ray (in two patients). Data are presented from the most consistent optical fiber recording.
Abdominal pressure was measured through the urinary catheter as described by Cheatham [24]. The pressure was recorded after filling the bladder with 50 ml of sterile saline. Respiratory fluctuations and increases in abdominal pressure after compression of the lower abdominal wall confirmed adequate catheter position.
Lung mechanics, ventilation, and oxygenation
Airway pressure was measured by an electronic transducer (System DPT-6000, PvB, Triplus) through an air-filled tube connected to the airway adapter at the proximal end of the orotracheal tube. The gas flow signal was recorded from the analogue port in the Evita 4 Dräger ventilator. Expiratory tidal volume (Vte) of a single breath was determined by integrating the flow signal from end inspiration to end expiration. Esophageal pressure was measured through a saline-filled Salem Sump tube placed in the esophagus as described by Karason [25]. The correct position of this tube was confirmed by observing minimal cardiac fluctuations and by performing the closed airway chest compression test. Blood samples for blood gas analyses, oxygen saturation measurements, and lactate concentration analyses (ABL 625, Radiometer, Denmark) were drawn from the arterial catheter in conjunction with the hemodynamic recordings.
Main study group
The main study protocol is illustrated in Fig. 1. After completed catheterization, a five-minute baseline period was allowed to elapse, followed by three consecutive RMs, each separated by a 15-min pause. The RMs were all 2-min-long. The first two RMs were identical and performed with pressure controlled ventilation with a peak airway pressure of 40 cmH2O for 8 s and a PEEP of 20 cmH2O for 2 s. At RM1 and RM2 this 10-s sequence was repeated 12 times during 2 min. The third RM was performed with pressure controlled ventilation at peak airway pressure 50 cmH2O for 4 s and a PEEP of 20 cm H2O for 1 s. At RM3 this 5-s sequence was repeated 24 times during 2 min. Measurements and blood sampling were performed immediately before, at the end of, and 3 min after each RM.
Study protocol reflected as alterations in airway pressure during three 2-min-long recruitment maneuvers (RM1, RM2, and RM3) and interposed 15 min pause periods. The lower line indicates PEEP, middle bold line mean airway pressure, and upper line peak airway pressure. Arrows indicate timing of blood sampling and measurements 2 min before, at the end of, and 3 min after each recruitment maneuver
Validation group
In order to assess effects by the LDF tube on gastric mucosal perfusion, we studied a separate group of four patients. This validation group consisted of patients with acute lung injury and met the same inclusion criteria as patients in the main study group. Gastric mucosal blood flow was measured for 1 h after insertion of the LDF catheter during mechanical ventilation without RMs. Data are presented for values obtained at 0 min, 15 min, 30 min, 45 min, and 60 min.
Calculations
Statistics
Wilcoxon's signed rank test was used to compare values obtained before each RM with values obtained during and after each RM, and data obtained before RM1 compared with data obtained after RM3. Values of P ≤0.05 were considered significant. All values are given as mean±SEM. Statistical analysis was performed with the SPSS software package (version 11.0; SPSS, Chicago, Ill., USA).
A post hoc power analysis based on an alpha value of 0.05, sample size of 10, and using the observed standard deviation of the mean difference of LDF values (before and after the three recruitment maneuvers), reveals a power of 65% to detect an absolute difference of 19% in the LDF measurements. A sample size of 14 would have been required to give a power of 80% to detect the same difference.
Results
Validation group
Four patients with ALI (age 51±14 years, APACHE II 24±5) were included in this group. None of these patients participated in the main study group. There were no significant changes in systemic hemodynamic parameters (data not shown) and gastric mucosal perfusion during the 60-min study period (580±74 PU at 0 min, 541±103 PU at 15 min, 553±108 PU at 30 min, 557±94 PU at 45 min, and 591±118 PU at 60 min).
Main study group
Systemic hemodynamic data
Systemic hemodynamic data are shown in Table 2. Pulse contour cardiac index decreased during all RMs (P=0.043 at RM1, RM2, and RM3), while MAP was decreased only during RM3 (P=0.028). Central venous pressure increased temporarily during all recruitment maneuvers and returned to baseline after each RM (P=0.008 at RM1, and P=0.005 at RM2 and RM3). Calculated systemic vascular resistance index was increased after RM2 and RM3 in comparison with the situation prior to the respective RM (P=0.043 after RM2 and RM3). Comparisons of values obtained before RM1 with values after RM3 demonstrated a decreased pulse contour cardiac index (P=0.043), while systemic vascular resistance index increased (P=0.043).
Gastric mucosal perfusion and abdominal pressure
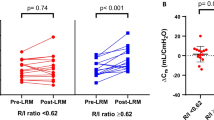
Individual changes in gastric mucosal perfusion are shown in Fig. 2. In one patient we were unable to get consistent gastric mucosal perfusion measurements during the two last recruitment maneuvers, and consequently this patient was excluded from analysis of gastric mucosal perfusion. Gastric mucosal perfusion and calculated gastric mucosal vascular resistance were not significantly changed during any of the RMs. However, when comparing values obtained before RM1 with values obtained after RM3 there was a nearly significant (P=0.051) decrease in gastric mucosal perfusion (Fig. 3) and a corresponding nearly significant (P=0.051) increase in gastric mucosal vascular resistance (data not shown).
Data from five patients showed that abdominal pressure increased significantly from 11.1±2.0 to 12.3±2.0 mmHg during RM2 (P=0.028) and from 10.1±2.0 to 12.7±2.1 mmHg during RM3 (P=0.050).
Lung mechanics, ventilation, and systemic oxygenation
Respiratory data are presented in Table 3. Peak airway pressure, mean airway pressure and PEEP increased (P<0.050) during all RMs. Intrinsic PEEP was unaltered during RM1 and RM2, but increased from 1.9±0.5 to 6.2±0.4 cmH2O (P=0.008) during RM3 (n=8). PaO2 increased during RM2 (P=0.008) but was otherwise not significantly influenced by the RMs. Three of the patients exhibited marked increases in oxygenation during all RMs, while another patient increased PaO2 only during the last recruitment maneuvers. In these four patients, PaO2 declined to pre-recruitment levels within 3 min following the recruitment maneuvers (Fig. 4). Dynamic compliance of the lung and of the respiratory system decreased (P=0.028) during RM3. Blood gas analyses demonstrated decreased pH and increased PaCO2 during RM1 (P=0.017 and 0.041, respectively) and RM2 (P=0.017 and 0.025, respectively), while pH increased and PaCO2 decreased during RM3 (P=0.011 and 0.013, respectively). No significant differences in respiratory pressures, dynamic compliance, PaO2, PaCO2 or pH were observed when comparing values obtained before RM1 with corresponding values after RM3.
Discussion
The present study demonstrates that gastric mucosal perfusion and calculated gastric mucosal vascular resistance were not significantly changed during any of the RMs in spite of a concomitant decrease in cardiac index. However, when comparing data prior to RM1 with corresponding data after RM3, we found a 9% decrease in cardiac index and a 19% decrease in absolute values of gastric mucosal perfusion, although the decrease in gastric mucosal perfusion did not reach statistical significance. This finding indicates that even brief increases in mean airway pressure, as induced by recruitment maneuvers, might induce alterations in systemic as well as regional perfusion. These observations are clinically important when considering that gastrointestinal ischemia and subsequent reperfusion can prime inflammatory cells and augment systemic inflammation, thereby causing multiple organ failure [22].
Assessment of gastrointestinal circulation is difficult in the clinical setting. Laser Doppler flowmetry using a surface-mounted probe is an established method for measurements of gastrointestinal blood flow [32, 33]. One advantage of this method, in comparison with other commonly used methods such as gastric tonometry or indocyanine green clearance, is that it allows a continuous measurement of perfusion, which makes it suitable for assessment of dynamic changes in perfusion. These properties were useful in the present study, demonstrating that laser Doppler flowmetry was able to monitor rapid alterations in gastric mucosal perfusion as induced by RMs.
As regards the laser Doppler flowmetry method, there has been a debate concerning the measuring depth of the laser light when measuring gastrointestinal blood flow. This measuring depth is influenced by tissue properties including the degree of light absorption and diffusion in the tissue. In addition, measuring depth is also dependent on light source, wave length, and probe configuration. The probe used in this study was specifically designed to measure mucosal blood flow, and not total gastric blood flow. Similar endoluminal probes have been used to study intestinal mucosal perfusion during brief hemodynamic challenges in man [34].
The relevance of gastric mucosal perfusion as an indicator of intestinal perfusion might be questioned. Obviously, vascular supply of the ventricle differs from that of the small intestine. The ventricle is supplied from truncus coeliacus, while the main supply of the small intestine is from the superior mesenteric artery. However, despite these differences in vascular supply, changes in gastric mucosal perfusion paralleled those of ileal perfusion in a model of porcine endotoxemic shock [30]. Similar data, presented by Hiltebrand and coworkers, indicate that gastric mucosal perfusion decreased in parallel with changes in hepatic, pancreatic, and colonic perfusion in a porcine model of septic shock [31]. We chose to measure mucosal blood flow, since the major part of gastrointestinal perfusion is distributed to the mucosa [35, 36], and hypoperfusion of the mucosa probably denotes significant gastric hypoperfusion.
Another methodological aspect is that mechanical stimulation of the feline intestinal mucosa has been shown to transiently increase intestinal blood flow [37]. To evaluate the impact of this mechanism on our present observations, we included a separate validation group comprising four patients. In this group, we were unable to demonstrate any significant changes in gastric mucosal perfusion induced by mechanical stimulation of the LDF probe.
Regarding effects of lung recruitment maneuvers on systemic oxygenation and respiratory mechanics, we found no lasting effects of such maneuvers, except for a minor increase in PaO2 after RM2. As shown in Fig. 4, two different response patterns were observed during RMs. Four patients exhibited marked increases in PaO2 at the end of the recruitment maneuver (three patients during all RMs, one patient during RM3 only), while the remaining patients showed no alteration in PaO2. The reason for this discrepancy is not easily explained since the four patients that increased their PaO2 shared no common properties regarding pre-recruitment intraabdominal pressure, systemic hemodynamic parameters, systemic oxygenation or lung mechanics. Further, there was no observable common pattern in their response to recruitment maneuvers regarding cardiovascular response or lung mechanics.
The peak airway pressure chosen for the recruitment maneuvers 1 and 2 was based on the findings by Rothen and colleagues [38]. According to their study, an otherwise healthy but atelectatic lung needs at least a pressure of 40 cmH2O to open fully. The inspiratory time needed to achieve recruitment at this pressure has been found to be about 8 s [39]. The time to expiratory collapse is probably rather short. Recent studies in patients with ARDS indicate that the time to expiratory collapse is less than 1 s [40]. It is therefore possible that the chosen expiratory time of 2 s used in recruitment maneuvers 1 and 2 was to long to prevent alveolar collapse, even though the lung was only allowed to collapse to a pressure of 20 cmH2O.
The third recruitment maneuver was different, and performed with a peak airway pressure of 50 cmH2O. The rationale for this increase in inspiratory recruitment pressure was that some of our patients were ventilated with peak airway pressures close to the inspiratory recruitment pressures used in RMs 1 and 2. Further, there is evidence for the need of higher distending pressures to achieve full lung opening in some patients with ARDS [17]. In order to minimize any circulatory instability that may arise during this higher peak airway pressure level, we shortened the inspiratory time to 4 s. To reduce alveolar collapse we also adjusted the expiratory time to 1 s.
There are at least two possible explanations regarding why we did not observe any beneficial effects of these recruitment maneuvers on systemic oxygenation. First, the peak airway pressure and the inspiratory time used in these recruitment maneuvers may not have been sufficient to achieve full lung opening. However, obtained peak and mean airway pressures during the recruitment maneuvers were rather high. We also observed a decline in dynamic compliance during RM3, indicative of overdistension of the lung. It is more likely that at least partial lung opening was achieved, but lung collapse occurred soon after termination of the recruitment maneuver.
The degree of lung opening during RMs cannot be described since we did not examine the patients with computed chest tomography. However, in at least four patients dramatic improvement in systemic oxygenation occurred during RMs, giving evidence of full lung opening in these patients. A second explanation about why we did not observe any persistent beneficial effects of recruitment maneuvers on systemic oxygenation is that we chose not to alter the PEEP setting after RMs.
Many clinicians decrease PEEP gradually from a high PEEP level following RMs to optimize PEEP. We chose not to alter PEEP levels following RMs since our primary aim was to study the effects of transient increases in intrathoracic pressure on gastric mucosal perfusion. This regimen probably promoted alveolar collapse.
We have previously demonstrated that effects of increased intrathoracic pressures, as induced by PEEP, on intestinal circulatory parameters are crucially dependent on intestinal perfusion pressure levels [41]. In the present study, we have investigated whether shorter periods of increased intrathoracic pressures also influence gastric mucosal perfusion. This question is clinically relevant, since modern concepts in ventilatory treatment include the use of high PEEP levels and frequent recruitment maneuvers. To conclude, this study on ten patients demonstrated no significant changes in gastric mucosal perfusion during lung recruitment maneuvers. There was, however, a trend towards gradual decreases in gastric mucosal perfusion. Further, we found that repeated RMs, as used in this study, did not induce any beneficial effects on arterial oxygenation or dynamic lung compliance.
References
Bernard GR, Artigas A, Brigham KL, Carlet J, Falke K, Hudson L, Lamy M, LeGall JR, Morris A, Spragg R (1994) The American-European Consensus Conference on ARDS. Definitions, mechanisms, relevant outcomes, and clinical trial coordination. Am J Respir Crit Care Med 149:818–824
Sjostrand UH, Lichtwarck-Aschoff M, Nielsen JB, Markstrom A, Larsson A, Svensson BA, Wegenius GA, Nordgren KA (1995) Different ventilatory approaches to keep the lung open. Intensive Care Med 21:310–318
Lachmann B (1992) Open up the lung and keep the lung open. Intensive Care Med 18:319–321
Rothen HU, Sporre B, Engberg G, Wegenius G, Hedenstierna G (1993) Re-expansion of atelectasis during general anaesthesia: a computed tomography study. Br J Anaesth 71:788–795
Winso O, Biber B, Gustavsson B, Holm C, Milsom I, Niemand D (1986) Portal blood flow in man during graded positive end-expiratory pressure ventilation. Intensive Care Med 12:80–85
Lehtipalo S, Biber B, Frojse R, Arnerlov C, Johansson G, Winso O (2001) Effects of positive end-expiratory pressure on intestinal circulation during graded mesenteric artery occlusion. Acta Anaesthesiol Scand 45:875–884
De Backer D (2000) The effects of positive end-expiratory pressure on the splanchnic circulation. Intensive Care Med 26:361–363
Dorinsky PM, Whitcomb ME (1983) The effect of PEEP on cardiac output. Chest 84:210–216
Robotham JL, Cherry D, Mitzner W, Rabson JL, Lixfeld W, Bromberger-Barnea B (1983) A re-evaluation of the hemodynamic consequences of intermittent positive pressure ventilation. Crit Care Med 11:783–793
Tanaka S, Sagawa S, Miki K, Claybaugh JR, Shiraki K (1994) Changes in muscle sympathetic nerve activity and renal function during positive-pressure breathing in humans. Am J Physiol 266:R1220–1228
Aneman A, Ponten J, Fandriks L, Eisenhofer G, Friberg P, Biber B (1997) Hemodynamic, sympathetic and angiotensin II responses to PEEP ventilation before and during administration of isoflurane. Acta Anaesthesiol Scand 41:41–48
Bersten AD, Gnidec AA, Rutledge FS, Sibbald WJ (1990) Hyperdynamic sepsis modifies a PEEP-mediated redistribution in organ blood flows. Am Rev Respir Dis 141:1198–1208
Aneman A, Eisenhofer G, Fandriks L, Olbe L, Dalenback J, Nitescu P, Friberg P (1999) Splanchnic circulation and regional sympathetic outflow during peroperative PEEP ventilation in humans. Br J Anaesth 82:838–842
Fujita Y (1993) Effects of PEEP on splanchnic hemodynamics and blood volume. Acta Anaesthesiol Scand 37:427–431
Rimensberger PC, Cox PN, Frndova H, Bryan AC (1999) The open lung during small tidal volume ventilation: concepts of recruitment and "optimal" positive end-expiratory pressure. Crit Care Med 27:1946–1952
Pelosi P, Cadringher P, Bottino N, Panigada M, Carrieri F, Riva E, Lissoni A, Gattinoni L (1999) Sigh in acute respiratory distress syndrome. Am J Respir Crit Care Med 159:872–880
Medoff BD, Harris RS, Kesselman H, Venegas J, Amato MB, Hess D (2000) Use of recruitment maneuvers and high-positive end-expiratory pressure in a patient with acute respiratory distress syndrome. Crit Care Med 28:1210–1216
Lapinsky SE, Aubin M, Mehta S, Boiteau P, Slutsky AS (1999) Safety and efficacy of a sustained inflation for alveolar recruitment in adults with respiratory failure. Intensive Care Med 25:1297–1301
Lundgren O, Svanvik J (1973) Mucosal hemodynamics in the small intestine of the cat during reduced perfusion pressure. Acta Physiol Scand 88:551–553
Papa M, Halperin Z, Rubinstein E, Orenstein A, Gafin S, Adar R (1983) The effect of ischemia of the dog's colon on transmural migration of bacteria and endotoxin. J Surg Res 35:264-269
Landow L, Andersen LW (1994) Splanchnic ischaemia and its role in multiple organ failure. Acta Anaesthesiol Scand 38:626–639
Biffl WL, Moore EE (1996) Splanchnic ischaemia/reperfusion and multiple organ failure. Br J Anaesth 77:59–70
Sakka SG, Reinhart K, Meier-Hellman A (1999) Comparison of pulmonary artery and arterial thermodilution cardiac output in critically ill patients. Intensive Care Med 25:843–846
Cheatham ML, Safcsak K (1998) Intraabdominal pressure: a revised method for measurement. J Am Coll Surg 186:594–595
Karason S, Karlsen KL, Lundin S, Stenqvist O (1999) A simplified method for separate measurements of lung and chest wall mechanics in ventilator-treated patients. Acta Anaesthesiol Scand 43:308–315
Edouard AR, Degremont AC, Duranteu J, Pussard E, Berdeaux A, Samii K (1994) Heterogeneous regional vascular responses to simulated transient hypovolemia in man. Intensive Care Med 20:403–404
Ruokonen E, Uusaro A, Alhava E, Takala J (1997) The effect of dobutamine infusion on splanchnic blood flow and oxygen transport in patients with acute pancreatitis. Intensive Care Med 23:732–737
Vogt J, Reinelt H, Radermacher P (1997) Dobutamine and the oxygen uptake/supply relationship: from global to regional-nothing is simple and easy. Intensive Care Med 23:715–717
Kiefer P, Nunes S, Kosonen P, Takala J (2000) Effect of positive end-expiratory pressure on splanchnic perfusion in acute lung injury. Intensive Care Med 26:376–383
Neviere R, Chagnon J, Vallet B, Lebleu N, Marechal X, Mathieu D, Wattel F, Dupuis B (1997) Dobutamin improves gastrointestinal blood flow in a porcine model of endotoxic shock. Crit Care Med 25:1371–1377
Hiltebrand LB, Krejci V, Banic A, Erni D, Wheatley AM, Sigurdsson GH (2000) Dynamic study of the distribution of microcirculatory blood flow in multiple splanchnic organs in septic shock. Crit Care Med 28:3233–3241
Ahn H, Lindhagen J, Nilsson G, Salerud E, Jodal M, Lundgren O (1985) Evaluation of laser Doppler flowmetry in the assessment of intestinal blood flow in cat. Gastroenterology 88:951–957
Kvietys PR, Shepherd AP, Granger DN (1985) Laser-Doppler, H2 clearance, and microsphere estimates of mucosal blood flow. Am J Physiol 249:G221–227
Thoren A, Ricksten SE, Lundin S, Gazelius B, Elam M (1998) Baroreceptor-mediated reduction of jejunal mucosal perfusion, evaluated with endoluminal laser Doppler flowmetry in conscious humans. J Auton Nerv Syst 68:157–163
Hulten L, Jodal M, Lindhagen J, Lundgren O (1976) Blood flow in the small intestine of cat and man as analyzed by an inert gas washout technique. Gastroenterology 70:45–51
Granger DN, Richardson PD, Kvietys PR, Mortillaro NA (1980) Intestinal blood flow. Gastroenterology 78:837–863
Biber B, Lundgren O, Svanvik J (1971) Studies on the intestinal vasodilatation observed after mechanical stimulation of the mucosa of the gut. Acta Physiol Scand 82:177–190
Rothen HU, Sporre B, Engberg G, Wegenius G, Hedenstierna G (1993) Re-expansion of atelectasis during general anaesthesia: a computed tomography study. Br J Anaesth 71:788–795
Rothen HU, Neumann P, Berglund JE, Valtysson J, Magnusson A, Hedenstierna G (1999) Dynamics of re-expansion of atelectasis during general anaesthesia. Br J Anaesth 82:551–556
Markstaller K, Eberle B, Kauczor HU, Scholz A, Bink A, Thelen M, Heinrichs W, Weiler N (2001) Temporal dynamics of lung aeration determined by dynamic CT in a porcine model of ARDS. Br J Anaesth 87:459–468
Lehtipalo S, Biber B, Frojse R, Arnerlov C, Johansson G, Winso O (2003) Effects of dopexamine and PEEP on intestinal blood flow and oxygenation: The perfusion pressure perspective. Chest (in press)
Acknowledgements
This work was supported by grants from the Tore Nilsson foundation and the Medical Faculty, Umeå University.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Claesson, J., Lehtipalo, S. & Winsö, O. Do lung recruitment maneuvers decrease gastric mucosal perfusion?. Intensive Care Med 29, 1314–1321 (2003). https://doi.org/10.1007/s00134-003-1830-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-003-1830-z