Abstract
Purpose
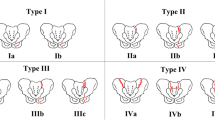
Fragility fractures of the pelvis (FFP) are becoming a commonly encountered disease in aging societies. We aimed to (1) clarify the overall survival rate of FFP, (2) compare survival rates by Rommens and Hofmann classification FFP type, (3) investigate the complications during hospitalization, and (4) investigate walking ability before and after injury depending on the type of fracture in patients with FFP treated conservatively.
Methods
This retrospective, multicenter study included 867 patients with FFP treated conservatively between 2014 and 2018 and excluded patients with insufficient follow-up for two years, lost data, and operative cases. This is a retrospective multicenter study. We established the database, which is named as TRON. We evaluated survival rate by fracture type using the log-rank test. We compared walking ability as defined by a new mobility score and the modified Majeed Pelvic Score among fracture types.
Results
We reviewed 552 cases (98 males and 454 females) with conservative treatment. The overall survival rates of patients with FFP treated conservatively were 0.90 at 1 year and 0.83 at 2 years. Although the survival rate was the lowest in FFP Type III, there was no significant difference in survival rates between fracture types (P = 0.143). The rates of complications during hospitalization were high for both Type III and Type IV fractures. Walking ability post-injury was worse in the patients with Type III fracture.
Conclusions
The survival rate of patients treated by conservative treatment was relatively good. Type III in the Rommens and Hofmann classification was related to lower life expectancy and loss of walking ability.





Similar content being viewed by others
Availability of data and material
The datasets during and/or analyzed during the current study available from the corresponding author on reasonable request.
References
Report of a WHO Study Group. Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. World Health Organ Tech Rep Ser. 1994;843:1–129.
Bonjour J-P, Ammann P, Rizzoli R. Importance of preclinical studies in the development of drugs for treatment of osteoporosis: a review related to the 1998 WHO guidelines. Osteoporos Int. 1999;9(5):379–93.
Papaioannou A, Morin S, Cheung AM, Atkinson S, Brown JP, Feldman S, et al. 2010 clinical practice guidelines for the diagnosis and management of osteoporosis in Canada: summary. CMAJ. 2010;182(17):1864–73.
Hertz K, Santy-Tomlinson J, editors. Fragility fracture nursing: holistic care and management of the orthogeriatric patient. Cham (CH): Springer; 2018.
Kannus P, Palvanen M, Niemi S, Parkkari J, Järvinen M. Epidemiology of osteoporotic pelvic fractures in elderly people in Finland: sharp increase in 1970–1997 and alarming projections for the new millennium. Osteoporos Int. 2000;11(5):443–8.
Miki RA, Oetgen ME, Kirk J, Insogna KL, Lindskog DM. Orthopaedic management improves the rate of early osteoporosis treatment after hip fracture. A randomized clinical trial. J Bone Joint Surg Am. 2008;90(11):2346–53.
Tile M. Pelvic ring fractures: should they be fixed? J Bone Joint Surg Br. 1988;70(1):1–12.
Burgess AR, Eastridge BJ, Young JW, Ellison TS, Ellison PS Jr, Poka A, et al. Pelvic ring disruptions: effective classification system and treatment protocols. J Trauma. 1990;30(7):848–56.
Meinberg E, Agel J, Roberts C, Karam M, Kellam J. Fracture and dislocation classification compendium–2018. J Orthop Trauma. 2018;32(Suppl 1):S1-10.
Tosounidis G, Wirbel R, Culemann U, Pohlemann T. Fehleinschätzung bei vorderer Beckenringfraktur im höheren Lebensalter. Misinterpretation of anterior pelvic ring fractures in the elderly (in German). Unfallchirurg. 2006;109(8):678–80.
Stuby FM, Schäffler A, Haas T, König B, Stöckle U, Freude T. Insufficiency fractures of the pelvic ring (in German). Unfallchirurg. 2013;116(4):351–66. https://doi.org/10.1007/s00113-012-2349-y.
Rommens PM, Hofmann A. Comprehensive classification of fragility fractures of the pelvic ring: recommendations for surgical treatment. Injury. 2013;44(12):1733–44.
Osterhoff G, Noser J, Held U, Werner CML, Pape H-C, Dietrich M. Early operative versus nonoperative treatment of fragility fractures of the pelvis: a propensity-matched multicenter study. J Orthop Trauma. 2019;33(11):e410–5.
Noser J, Dietrich M, Tiziani S, Werner CML, Pape H-C, Osterhoff G. Mid-term follow-up after surgical treatment of fragility fractures of the pelvis. Injury. 2018;49(11):2032–5.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–83.
Parker M, Palmer C. A new mobility score for predicting mortality after hip fracture. J Bone Joint Surg Br. 1993;75(5):797–8.
Yoshida M, Tajima K, Saito Y, Sato K, Uenishi N, Iwata M. Mobility and mortality of 340 patients with fragility fracture of the pelvis. Eur J Trauma Emerg Surg. 2021;47(1):29–36.
Majeed S. Grading the outcome of pelvic fractures. J Bone Joint Surg Br. 1989;71(2):304–6.
Kanda Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant. 2013;48(3):452–8.
Taillandier J, Langue F, Alemanni M, Taillandier-Heriche E. Mortality and functional outcomes of pelvic insufficiency fractures in older patients. Joint Bone Spine. 2003;70(4):287–9.
Leung WY, Ban CM, Lam JJ, Ip FK, Ko PS. Prognosis of acute pelvic fractures in elderly patients: retrospective study. Hong Kong Med J. 2001;7(2):139–45.
Gotis-Graham I, McGuigan L, Diamond T, Portek I, Quinn R, Sturgess A, et al. Sacral insufficiency fractures in the elderly. J Bone Joint Surg Br. 1994;76(6):882–6.
Agri F, Bourgeat M, Becce F, Moerenhout K, Pasquier M, Borens O, et al. Association of pelvic fracture patterns, pelvic binder use and arterial angio-embolization with transfusion requirements and mortality rates; a 7-year retrospective cohort study. BMC Surg. 2017;17(1):104.
Manson T, O’Toole RV, Whitney A, Duggan B, Sciadini M, Nascone J. Young-Burgess classification of pelvic ring fractures: does it predict mortality, transfusion requirements, and non-orthopaedic injuries? J Orthop Trauma. 2010;24(10):603–9.
Hart RA, Badra MI, Madala A, Yoo JU. Use of pelvic incidence as a guide to reduction of H-type spino-pelvic dissociation injuries. J Orthop Trauma. 2007;21(6):369–74.
Lindahl J, Mäkinen TJ, Koskinen SK, Söderlund T. Factors associated with outcome of spinopelvic dissociation treated with lumbopelvic fixation. Injury. 2014;45(12):1914–20.
Lehman RA Jr, Kang DG, Bellabarba C. A new classification for complex lumbosacral injuries. Spine J. 2012;12(7):612–28.
Linstrom NJ, Heiserman JE, Kortman KE, Crawford NR, Baek S, Anderson RL, et al. Anatomical and biomechanical analyses of the unique and consistent locations of sacral insufficiency fractures. Spine. 2009;34(4):309–15.
Rommens PM, Hopf JC, Herteleer M, Devlieger B, Hofmann A, Wagner D. Isolated pubic ramus fractures are serious adverse events for elderly persons: an observational study on 138 patients with fragility fractures of the pelvis type I (FFP type I). J Clin Med Res. 2020;9:2498.
van Dijk WA, Poeze M, van Helden SH, Brink PR, Verbruggen JP. Ten-year mortality among hospitalised patients with fractures of the pubic rami. Injury. 2010;41:411–4.
Maier GS, Kolbow K, Lazovic D, Horas K, Roth KE, Seeger JB, et al. Risk factors for pelvic insufficiency fractures and outcome after conservative therapy. Arch Gerontol Geriatr. 2016;67:80–5.
Brouwers L, Wouter Lansink KW, van Delft-Schreurs K. Differences in the Majeed Pelvic Score between injured and uninjured patients. J Orthop Trauma. 2019;33(5):244–9.
Rommens PM, Boudissa M, Krämer S, Kisilak M, Hofmann A, Wagner D. Operative treatment of fragility fractures of the pelvis is connected with lower mortality. A single institution experience. PLoS ONE. 2021;16: e0253408.
Wagner D, Kisilak M, Porcheron G, Krämer S, Mehling I, Hofmann A, et al. Trans-sacral bar osteosynthesis provides low mortality and high mobility in patients with fragility fractures of the pelvis. Sci Rep. 2021;11:14201.
Saito Y, Tokutake K, Takegami Y, Yoshida M, Omichi T, Imagama S. Does surgical treatment for unstable fragility fracture of the pelvis promote early mobilization and improve survival rate and postoperative clinical function? [published online ahead of print, 2021 Jun 22]. Eur J Trauma Emerg Surg. 2021. https://doi.org/10.1007/s00068-021-01729-6.
Rommens PM, Arand C, Hopf JC, Mehling I, Dietz SO, Wagner D. Progress of instability in fragility fractures of the pelvis: an observational study. Injury. 2019;50(11):1966–73.
Krappinger D, Kaser V, Kammerlander C, Neuerburg C, Merkel A, Lindtner RA. Inter- and intraobserver reliability and critical analysis of the FFP classification of osteoporotic pelvic ring injuries. Injury. 2019;50(2):337–43.
OECD (2021) Medical graduates (indicators). https://doi.org/10.1787/ac5bd5d3-en (Accessed on 16 September 2021)
Acknowledgements
We thank Members of the Trauma research of Nagoya group (shown in alphabetical order of affiliation) as follows: Dr. Takeshi Oguchi (Anjo Kosei Hospital); Dr. Yoshiharu Oka (Chubu Rosai Hospital); Dr. Masahiro Hanabayashi (Ichinomiya Municipal Hospital), Dr. Hiroaki Yoshida (Kamiiida Daiichi General Hospital), Dr. Tokumi Kanemura (Kounan Kosei Hospital), Hidenori Inoue (Nagoya Daiichi Red Cross Hospital), Dr. Koji Maruyama (Nakatsugawa Municipal General Hospital), Dr. Kenichi Yamauchi (Toyohashi Municipal Hospital); Dr. Yasuhide Kanayama (Toyota Kosei Hospital); Dr. Tadahiro Sakai (TOYOTA memorial Hospital), Dr. Nobuhiro Okui (Yokkaichi Municipal Hospital) and Dr. Ryosuke Sugimoto, Dr. Takuya Sugimoto, Dr. Yujiro Kagami, Dr. Hiroshi Takahashi, Dr, Yujiro Katayama (Nagoya university) .
Funding
There is no supporting funding.
Author information
Authors and Affiliations
Contributions
Conceptualization: YT and SI; Methodology: YT, YS; Formal analysis and investigation: TO; Writing—original draft preparation: TO; Writing—review and editing: KT; Resources: OI and TA; Supervision: SI.
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
The approval number in our institute is 2020-0549.
Consent to participate and publication
All patients provided written informed for their data to be used.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Omichi, T., Takegami, Y., Tokutake, K. et al. Mortality and functional outcomes of fragility fractures of the pelvis by fracture type with conservative treatment: a retrospective, multicenter TRON study. Eur J Trauma Emerg Surg 48, 2897–2904 (2022). https://doi.org/10.1007/s00068-021-01839-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-021-01839-1