Abstract
Background
The relationship between surgical management of adhesive small bowel obstruction (ASBO) and hospital teaching status is not well known. We sought to elucidate the association between hospital teaching status and clinical metrics for ASBO.
Methods
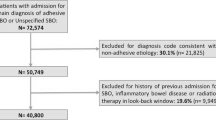
Using the 2007–2017 California Office of Statewide Health Planning and Development database, we identified adult ASBO patients hospitalized for surgical intervention. Hospital teaching status was categorized as major teaching (MajT), minor teaching (MinT), and non-teaching (NT). Cox proportional hazards modeling was used to evaluate risk of death and other adverse outcomes.
Results
Of 25,047 admissions, 15.4% were at MajT, 32.0% at MinT, and 52.6% at NT; 2.9% died. Patients at MajT had longer overall hospital stays (HLOS) than those at MinT or NT (median days 9 vs. 8 vs. 8; p = 0.005), longer post-ASBO procedure HLOS (median days 7 vs. 6 vs. 6; p = 0.0001) and higher rates of small bowel resection (27.1% vs. 21.7% vs. 21.7%; p < 0.0001). Mean time to first surgery at MajT was 3.3 days compared with 2.6 days (p = 0.004) at MinT and NT. Compared with patients at NT, those at MajT were significantly less likely to die (HR 0.62, p < 0.0001), develop pneumonia (HR 0.57, p = 0.001), or experience adverse discharge disposition (HR 0.79, p < 0.0001).
Conclusion
Mortality and morbidity of ASBO surgery were reduced at MajT; however, time to surgery, HLOS, and rate of small bowel resection were greater. These findings may guide improvements in the management of ASBO patients.
Similar content being viewed by others
Availability of data and material
Data are published by the California Office of Statewide Health Planning and Development.
Code availability
Stata statistical software analysis code available upon request.
References
Menzies D, Ellis H. Intestinal obstruction from adhesions–how big is the problem? Ann R Coll Surg Engl. 1990;72(1):60–3.
ten Broek RP, et al. Burden of adhesions in abdominal and pelvic surgery: systematic review and meta-analysis. BMJ. 2013;347: f5588. https://doi.org/10.1136/bmj.f5588.
Irvin TT. Abdominal pain: a surgical audit of 1190 emergency admissions. Br J Surg. 1989;76(11):1121–5. https://doi.org/10.1002/bjs.1800761105.
Ogola GO, Shafi S. Cost of specific emergency general surgery diseases and factors associated with high-cost patients. J Trauma Acute Care Surg. 2016;80(2):265–71. https://doi.org/10.1097/ta.0000000000000911.
Wessels LE, et al. Outcomes in adhesive small bowel obstruction from a large statewide database: What to expect after nonoperative management. J Trauma Acute Care Surg. 2019;86(4):651–7. https://doi.org/10.1097/ta.0000000000002196.
Schraufnagel D, Rajaee S, Millham FH. How many sunsets? Timing of surgery in adhesive small bowel obstruction: a study of the Nationwide Inpatient Sample. J Trauma Acute Care Surg. 2013;74(1):181–7. https://doi.org/10.1097/ta.0b013e31827891a1.
Foster NM, et al. Small bowel obstruction: a population-based appraisal. J Am Coll Surg. 2006;203(2):170–6. https://doi.org/10.1016/j.jamcollsurg.2006.04.020.
Azagury D, et al. Small bowel obstruction: a practical step-by-step evidence-based approach to evaluation, decision making, and management. J Trauma Acute Care Surg. 2015;79(4):661–8. https://doi.org/10.1097/ta.0000000000000824.
Fung BSC, et al. Longer trials of non-operative management for adhesive small bowel obstruction are associated with increased complications. J Gastrointest Surg. 2020;24(4):890–8. https://doi.org/10.1007/s11605-019-04156-6.
Shah A, et al. Variation in timely surgery for hip fracture by day and time of presentation: a nationwide prospective cohort study from the National Hip Fracture Database for England, Wales and Northern Ireland. BMJ Qual Saf. 2020. https://doi.org/10.1136/bmjqs-2020-011196.
Daniel VT, et al. Association between operating room access and mortality for life-threatening general surgery emergencies. J Trauma Acute Care Surg. 2019;87(1):35–42. https://doi.org/10.1097/ta.0000000000002267.
Glance LG, et al. Outcomes are worse in us patients undergoing surgery on weekends compared with weekdays. Med Care. 2016;54(6):608–15. https://doi.org/10.1097/mlr.0000000000000532.
Sundararajan V, et al. New ICD-10 version of the Charlson comorbidity index predicted in-hospital mortality. J Clin Epidemiol. 2004;57(12):1288–94. https://doi.org/10.1016/j.jclinepi.2004.03.012.
Charlson M, et al. Validation of a combined comorbidity index. J Clin Epidemiol. 1994;47(11):1245–51. https://doi.org/10.1016/0895-4356(94)90129-5.
Shahian DM, et al. Contemporary performance of U.S. teaching and nonteaching hospitals. Acad Med. 2012;87(6):701–8. https://doi.org/10.1097/acm.0b013e318253676a.
Khuri SF, et al. Comparison of surgical outcomes between teaching and nonteaching hospitals in the Department of Veterans Affairs. Ann Surg. 2001;234(3):370–82. https://doi.org/10.1097/00000658-200109000-00011.
Vartak S, Ward MM, Vaughn TE. Do postoperative complications vary by hospital teaching status? Med Care. 2008;46(1):25–32. https://doi.org/10.1097/mlr.0b013e3181484927.
Boyd-Carson H, et al. Trainee-led emergency laparotomy operating. Br J Surg. 2020;107(10):1289–98. https://doi.org/10.1002/bjs.11611.
Zeitoun JD, Reboul-Marty J, Lefevre JH. Impact of resident and fellow changeovers on patient outcomes: a nationwide cross-sectional study. Eur J Public Health. 2017;27(6):960–5. https://doi.org/10.1093/eurpub/ckx072.
Thornlow DK, Stukenborg GJ. The association between hospital characteristics and rates of preventable complications and adverse events. Med Care. 2006;44(3):265–9. https://doi.org/10.1097/01.mlr.0000199668.42261.a3.
Papanikolaou PN, Christidi GD, Ioannidis JP. Patient outcomes with teaching versus nonteaching healthcare: a systematic review. PLoS Med. 2006;3(9): e341. https://doi.org/10.1371/journal.pmed.0030341.
Iezzoni LI. Major teaching hospitals defying Darwin. JAMA. 1997;278(6):520.
Fonarow GC, et al. Adherence to heart failure quality-of-care indicators in US hospitals: analysis of the ADHERE Registry. Arch Intern Med. 2005;165(13):1469–77. https://doi.org/10.1001/archinte.165.13.1469.
Burke LG, et al. Association between teaching status and mortality in US hospitals. JAMA. 2017;317(20):2105–13. https://doi.org/10.1001/jama.2017.5702.
Di Saverio S, et al. Bologna guidelines for diagnosis and management of adhesive small bowel obstruction (ASBO): 2013 update of the evidence-based guidelines from the world society of emergency surgery ASBO working group. World J Emerg Surg. 2013;8(1):42. https://doi.org/10.1186/1749-7922-8-42.
Loftus T, et al. A protocol for the management of adhesive small bowel obstruction. J Trauma Acute Care Surg. 2015;78(1):13–9. https://doi.org/10.1097/ta.0000000000000491.
Hyder O, et al. Impact of hospital teaching status on length of stay and mortality among patients undergoing complex hepatopancreaticobiliary surgery in the USA. J Gastrointest Surg. 2013;17(12):2114–22. https://doi.org/10.1007/s11605-013-2349-4.
Silber JH, et al. Comparing outcomes and costs of medical patients treated at major teaching and non-teaching hospitals: a national matched analysis. J Gen Intern Med. 2020;35(3):743–52. https://doi.org/10.1007/s11606-019-05449-x.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
MJC conducted the literature search. MJC, JB, DAB, JAD, RYC, CBS, MJM, and VB participated in the conception or design of the work. MJC, JB, and RYC acquired, analyzed, or interpreted the data for the work. MJC, JB, DAB, JAD, RYC, CBS, MJM, and VB participated in drafting the work or revising it for important intellectual content. All authors approved the final version of the work to be published.
Corresponding author
Ethics declarations
Conflicts of interest
The authors report no proprietary or commercial interest in any product mentioned or concept discussed in this article. The authors report no conflict of interest.
Ethics approval
This study was approved by the California Health and Human Services Agency Committee for the Protection of Human Subjects and the local Institutional Review Board.
Consent to participate
Requirement of informed consent was waived for this study by the institutions listed in the Ethics Approval section.
Additional information
Meeting Presentation: This work was presented as a poster presentation at the 79th Annual Meeting of the American Association for the Surgery of Trauma and Clinical Congress of Acute Care Surgery, September 8–18, 2020. Virtual Meeting.
Rights and permissions
About this article
Cite this article
Carr, M.J., Badiee, J., Benham, D.A. et al. Surgical management and outcomes of adhesive small bowel obstruction: teaching versus non-teaching hospitals. Eur J Trauma Emerg Surg 48, 107–112 (2022). https://doi.org/10.1007/s00068-021-01812-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-021-01812-y