Abstract
Purpose
The purpose of this study was to compare the color changes of two different nanocomposites used for two different designs of clear aligner attachments.
Methods
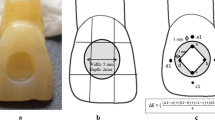
In all, 120 human premolars were embedded in 12 upper dental models with 10 premolars in each model. Models were scanned and attachments were digitally designed. Conventional attachments (CA) were prepared for the first six models and optimized multiplane attachments (OA) were prepared for the other six models with packable composite (PC) on the right quadrant and flowable composite (FC) on the left quadrant of each model. The models were subjected to 2000 thermal cycles at 5 °C/55 °C and then consecutively immersed in the five different staining solutions each for 48 h to simulate external discoloration. Color measurements were taken with a spectrophotometer. Color changes (∆E*ab) of the attachments before and after immersion were compared with the Commission Internationale de l’Éclairage L*a*b* (CIELAB) color space approach.
Results
When ∆E*ab values were examined, no significant difference was observed between the groups according to the attachment type (P > 0.05). After the coloration process, the flowable composite group showed less coloration than the packable composite group for both attachment designs (P < 0.05). Color difference values after the staining procedure were significantly higher in the CA-PC and OA-PC groups compared to the CA-FC and OA-FC groups (P < 0.05).
Conclusion
Color change of the packable nanocomposite was more pronounced than that of the flowable nanocomposite for both attachment designs. Therefore, clear aligner attachments created using flowable nanocomposite can be recommended, especially in the anterior region where esthetics are important for the patient.
Zusammenfassung
Zielsetzung
Ziel dieser Studie war es, die Farbveränderungen zweier verschiedener Nanokomposite zu vergleichen, die für 2 unterschiedliche Designs von Clear-Aligner-Attachments verwendet werden.
Methoden
Insgesamt wurden 120 menschliche Prämolaren in 12 Oberkiefermodelle eingebettet, die jeweils 10 Prämolaren enthielten. Die Modelle wurden gescannt und die Attachments wurden digital entworfen. Für die ersten 6 Modelle wurden konventionelle Attachments (CA) und für die anderen 6 Modelle optimierte Multiplane-Attachments (OA) mit stopfbarem Komposit (PC) auf dem rechten Quadranten und fließfähigem Komposit (FC) auf dem linken Quadranten jedes Modells angefertigt. Die Modelle wurden 2000 thermischen Zyklen bei 5 °C/55 °C unterzogen und dann 48 Stunden lang nacheinander in die 5 verschiedenen Färbelösungen getaucht, um externe Verfärbungen zu simulieren. Die Farbmessungen wurden mit einem Spektralphotometer durchgeführt. Die Farbveränderungen (∆E*ab) der Aufsätze vor und nach dem Eintauchen wurden mit dem Farbraumverfahren der Commission Internationale de lʼÉclairage L*a*b* (CIELAB) verglichen.
Ergebnisse
Bei der Untersuchung der ∆E*ab-Werte wurde kein signifikanter Unterschied zwischen den Gruppen je nach Attachmenttyp festgestellt (p > 0,05). Nach dem Färbeverfahren zeigte die Gruppe mit fließfähigem Komposit bei beiden Geschiebeformen eine geringere Färbung als die Gruppe mit stopfbarem Komposit (p > 0,05). Die Farbdifferenzwerte nach dem Färbeverfahren waren in den Gruppen CA-PC und OA-PC signifikant höher als in den Gruppen CA-FC und OA-FC (p > 0,05).
Schlussfolgerung
Die Farbveränderung des stopfbaren Nanokomposits war bei beiden Attachment-Designs stärker ausgeprägt als die des fließfähigen Nanokomposits. Daher können Clear-Aligner-Attachments, die mit fließfähigem Nanokomposit hergestellt werden, empfohlen werden, insbesondere im Frontzahnbereich, wo die Ästhetik für den Patienten wichtig ist.





Similar content being viewed by others
References
Maspero C, Farronato D, Giannini L, Farronato G (2010) Orthodontic treatment in elderly patients. Prog Orthod 11(1):62–75. https://doi.org/10.1016/j.pio.2010.04.008
Ghafari JG (2015) Centennial inventory: the changing face of orthodontics. Am J Orthod Dentofacial Orthop 148(5):732–739. https://doi.org/10.1016/j.ajodo.2015.08.011
Malik OH, McMullin A, Waring DT (2013) Invisible orthodontics part 1: invisalign. Dent Update 40(3):203–215. https://doi.org/10.12968/denu.2013.40.3.203
Rosvall MD, Fields HW, Ziuchkovski J, Rosenstiel SF, Johnston WM (2009) Attractiveness, acceptability, and value of orthodontic appliances. Am J Orthod Dentofacial Orthop 5(3):276–277. https://doi.org/10.1016/j.ajodo.2008.09.020
Alansari RA, Faydhi DA, Ashour BS, Alsaggaf DH, Shuman MT, Ghoneim SH et al (2019) Adult perceptions of different orthodontic appliances. Patient Prefer Adherence 13:2119–2128. https://doi.org/10.2147/PPA.S234449
Nucera R, Dolci C, Bellocchio AM, Costa S, Barbera S, Rustico L et al (2022) Effects of composite attachments on orthodontic clear aligners aherapy: a systematic review. Materials (Basel) 15(2):533. https://doi.org/10.3390/ma15020533
Rossini G, Parrini S, Deregibus A, Castroflorio T (2017) Controlling orthodontic tooth movement with clear aligners: an updated systematic review regarding efficacy and efficiency. J Aligner Orthod 1:7–20
Rossini G, Parrini S, Castroflorio T, Deregibus A, Debernardi CL (2015) Efficacy of clear aligners in controlling orthodontic tooth movement: a systematic review. Angle Orthod 85(5):881–889. https://doi.org/10.2319/061614-436.1
Papadimitriou A, Mousoulea S, Gkantidis N, Kloukos D (2018) Clinical effectiveness of Invisalign® orthodontic treatment: a systematic review. Prog Orthod 19(1):37. https://doi.org/10.1186/s40510-018-0235-z
Simon M, Keilig L, Schwarze J, Jung BA, Bourauel C (2014) Forces and moments generated by removable thermoplastic aligners: incisor torque, premolar derotation, and molar distalization. Am J Orthod Dentofacial Orthop 145(6):728–736. https://doi.org/10.1016/j.ajodo.2014.03.015
Comba B, Parrini S, Rossini G, Castroflorio T, Deregibus A (2017) A three dimensional finite element analysis of upper-canine distalization with clear aligners, composite attachments, and class II elastics. J Clin Orthod 51:24–28
Gomez JP, Peña FM, Martínez V, Giraldo DC, Cardona CI (2015) Initial force systems during bodily tooth movement with plastic aligners and composite attachments: a three-dimensional finite element analysis. Angle Orthod 85(3):454. https://doi.org/10.2319/050714-330.1
Gazzani F, Bellisario D, Quadrini F, Parrinello F, Pavoni C, Cozza P, Lione R (2022) Comparison between different composite resins used for clear aligner attachments: an in-vitro study. Front Mater 8:789143. https://doi.org/10.3389/fmats.2021.789143
Ferracane JL (2011) Resin composite-state of the Art. Dent Mater 27(1):29–38. https://doi.org/10.1016/j.dental.2010.10.020
Mantovani E, Castroflorio E, Rossini G, Garino F, Cugliari G, Deregibus A et al (2019) Scanning electron microscopy analysis of aligner fitting on anchorage attachments. J Orofac Orthop 80(2):79–87. https://doi.org/10.1007/s00056-018-00167-1
Bayne SC, Thompson JY, Swift EJ Jr, Stamatiades P, Wilkerson M (1998) A characterization of first-generation flowable composites. J Am Dent Assoc 129(5):567–577. https://doi.org/10.14219/jada.archive.1998.0274
Benetti AR, Havndrup-Pedersen C, Honoré D, Pedersen MK, Pallesen U (2015) Bulk-fill resin composites: polymerization contraction, depth of cure, and gap formation. Oper Dent 40(2):190–200. https://doi.org/10.2341/13-324-L
Clelland NL, Pagnotto MP, Kerby RE, Seghi RR (2005) Relative wear of flowable and highly filled composite. J Prosthet Dent 93(2):153–157. https://doi.org/10.1016/j.prosdent.2004.11.006
Badr C, Spagnuolo G, Amenta F, Khairallah C, Mahdi SS, Daher E et al (2021) A two-year comparative evaluation of clinical performance of a nanohybrid composite resin to a flowable composite resin. J Funct Biomater 12(3):51. https://doi.org/10.3390/jfb12030051
Guler AU, Yilmaz F, Kulunk T, Guler E, Kurt S (2005) Effects of different drinks on stainability of resin composite provisional restorative materials. J Prosthet Dent 94(2):118–124. https://doi.org/10.1016/j.prosdent.2005.05.004
Özdaş DÖ, Kazak M, Çilingir A, Subaşı MG, Tiryaki M, Günal Ş (2016) Color stability of composites after short-term oral simulation: an in vitro study. Open Dent J 10(1):431–437. https://doi.org/10.2174/1874210601610010431
Harorlı OT, Barutcigil Ç (2014) Color recovery effect of commercial mouth rinses on a discolored composite. J Esthet Restor Dent 26(4):256–263. https://doi.org/10.1111/jerd.12107
Sarafianou A, Iosifidou S, Papadopoulos T, Eliades G (2007) Color stability and degree of cure of direct composite restoratives after accelerated aging. Oper Dent 32(4):406–411. https://doi.org/10.2341/06-127
Vichi A, Ferrari M, Davidson CL (2004) Color and opacity variations in three different resin-based composite products after water aging. Dent Mater 20(6):530–534. https://doi.org/10.1016/j.dental.2002.11.001
Al Kheraif AA, Bin Qasim SS, Ramakrishnaiah R, Rehman I (2013) Effect of different beverages on the color stability and degree of conversion of nano and microhybrid composites. Dent Mater J 32(2):326–331. https://doi.org/10.4012/dmj.2011-267
Bagheri R, Burrow MF, Tyas M (2005) Influence of food-simulating solutions and surface finish on susceptibility to staining of aesthetic restorative materials. J Dent 33(5):389–398. https://doi.org/10.1016/j.jdent.2004.10.018
Elembaby AES (2014) The effects of mouth rinses on the color stability of resin-based restorative materials. J Esthet Restor Dent 26(4):264–271. https://doi.org/10.1111/jerd.12061
Shalish M, Cooper-Kazaz R, Ivgi I, Canetti L, Tsur B, Bachar E et al (2012) Adult patients’ adjustability to orthodontic appliances. Part I: a comparison between labial, lingual, and InvisalignTM. Eur J Orthod 34(6):724–730. https://doi.org/10.1093/ejo/cjr086
Paravina RD, Ghinea R, Herrera LJ, Bona AD, Igiel C, Linninger M et al (2015) Color difference thresholds in dentistry. J Esthet Restor Dent 27:1–9. https://doi.org/10.1111/jerd.12149
Bureau Central de la Commision Internationale de l’Eclairage (CIE) (1978) Recommendations on uniform color-spaces, color difference equations, psychometric color terms. CIE, Paris, pp 9–12 (Supplement No. 2 to CIE Publication No. 15)
International Standardization Organization (1985) DIN EN 27491. Dentistry: dental materials: determination of color stability of dental polymeric materials. Beuth, Belgium
Schulze KA, Marshall SJ, Gansky SA, Marshall GW (2003) Color stability and hardness in dental composites after accelerated aging. Dent Mater 19(7):612–619. https://doi.org/10.1016/s0109-5641(03)00003-4
Ruyter IE, Nilner K, Moller B (1987) Color stability of dental composite resin materials for crown and bridge veneers. Dent Mater 3(5):246–251. https://doi.org/10.1016/S0109-5641(87)80081-7
Giddon DB (1995) Orthodontic applications of pschological and perceptual studies of facial esthetics. Semin Orthod 1(2):82–93. https://doi.org/10.1016/S1073-8746(95)80095-6
Pabari S, Moles DR, Cunningham SJ (2015) Assessment of motivation and psychological characteristics of adult orthodontic patients. Am J Orthod Dentofacial Orthop 140(6):263–272. https://doi.org/10.1016/j.ajodo.2011.06.022
Jeremiah HG, Bister D, Newton JT (2011) Social perceptions of adults wearing orthodontic appliances: a cross-sectional study. Eur J Orthod 33(5):476–482. https://doi.org/10.1093/ejo/cjq069
Nanda R, Garino F, Ojima K, Castroflorio T, Parrini S (2021) The hybrid approach in class II malocclusions treatment, 1st edn. Principles and biomechanics of aligner treatment. Amsterdam, The Netherlands, pp 149–160
Labella R, Lambrechts P, Van Meerbeek B, Vanherle G (1999) Polymerization shrinkage and elasticity of flowable composites and filled adhesives. Dent Mater 15(2):128–137. https://doi.org/10.1016/s0109-5641(99)00022-6
Bueno RP, Salomone P, Villetti MA, Pozzobon RT (2013) Effect of bleaching agents on the fluorescence of composite resins. Eur J Esthet Dent 8(4):582–591
Tsiliagkou A, Diamantopoulou S, Papazoglou E, Kakaboura A (2016) Evaluation of reliability and validity of three dental color-matching devices. Int J Esthet Dent 11(1):110–124
Mehl A, Bosch G, Fischer C, Ender A (2017) In vivo tooth-color measurement with a new 3D intraoral scanning system in comparison to conventional digital and visual color determination methods. Int J Comput Dent 20(4):343–361. https://doi.org/10.5167/UZH-144972
Montes‑G GM, Draughn RA (1986) In vitro surface degradation of composites by water and thermal cycling. Dent Mater 2(5):193–197. https://doi.org/10.1016/S0109-5641(86)80012-4
Paolone G, Formiga S, De Palma F, Abbruzzese L, Chirico L, Scolavino S et al (2022) Color stability of resin-based composites: staining procedures with liquids—a narrative review. J Esthet Restor Dent. https://doi.org/10.1111/jerd.12912
Gupta G, Gupta T (2011) Evaluation of the effect of various beverages and food material on the color stability of provisional materials—an in vitro study. J Conserv Dent 14(3):287–292. https://doi.org/10.4103/0972-0707.85818
Chittem J, Sajjan GS, Kanumuri MV (2017) Spectrophotometric evaluation of color stability of nano hybrid composite resin in commonly used food colorants in asian countries. J Clin Diagn Res 11(1):61–65. https://doi.org/10.7860/JCDR/2017/22919.9193
Stober T, Gilde H, Lenz P (2001) Color stability of highly filled composite resin materials for facings. Dent Mater 17(1):87–94. https://doi.org/10.1016/s0109-5641(00)00065-8
Chami VO, Gebert F, Assaf DC, Centeno ACT, Ferrazzo VA, Durand LB, Marquezan M (2022) Color stability of resin composites for orthodontic attachments: an in vitro study. Dental Press J Orthod. https://doi.org/10.1590/2177-6709.27.1.e2220432.oar
Ertaş E, Güler AU, Yücel AÇ, Köprülü H, Güler E (2006) Color stability of resin composites after immersion in different drinks. Dent Mater J 25(2):371–376
Inokoshi S, Burrow MF, Kataumi M et al (1996) Opacity and color changes of tooth-colored restorative materials. Oper Dent 21(2):73–80
Turssi CP, de Magalhães CS, Serra MC, Rodrigues Júnior AL (2001) Surface roughness assessment of resin-based materials during brushing preceded by pH-cycling simulations. Oper Dent 26(6):576–584
Karadaş M, Demirbuğa S (2017) Evaluation of color stability and surface roughness of bulk-fill resin composites and nanocomposites. Meandros Med Dent J 18(3):199–205. https://doi.org/10.4274/meandros.36855
Chen MH (2010) Critical reviews in oral biology & medicine: update on dental nanocomposites. J Dent Res 89(6):549–560. https://doi.org/10.1177/0022034510363765
Shaalan O, Abou-Auf E, El Zoghby A (2017) Clinical evaluation of flowable resin composite versus conventional resin composite in carious and noncarious lesions: systematic review and meta-analysis. J Conserv Dent 20(6):380–385. https://doi.org/10.4103/JCD.JCD_226_17
Sumino N, Tsubota K, Takamizawa T, Shiratsuchi K, Miyazaki M, Latta MA (2013) Comparison of the wear and flexural characteristics of flowable resin composites for posterior lesions. Acta Odontol Scand 71(3):820–827. https://doi.org/10.3109/00016357.2012.734405
Hirata-Tsuchiya S, Yoshii S, Ichimaru-Suematsu M, Washio A, Saito N, Urata M et al (2017) Two-year clinical comparison of a flowable-type nano-hybrid composite and a paste-type composite in posterior restoration. J Investig Clin Dent. https://doi.org/10.1111/jicd.12227
Barakah HM, Taher NM (2014) Effect of polishing systems on stain susceptibility and surface roughness of nanocomposite resin material. J Prosthet Dent 112(3):625–631. https://doi.org/10.1016/j.prosdent.2013.12.007
Duc O, Di Bella E, Krejci I, Betrisey E, Abdelaziz M, Ardu S (2019) Susceptibility of resin composite materials. Am J Dent 32(1):39–42
Tavangar M, Bagheri R, Kwon T‑Y, Mese A, Manton DJ (2018) Influence of beverages and surface roughness on the color change of resin composites. J Investig Clin Dent. https://doi.org/10.1111/jicd.12333
Abzal MS, Rathakrishnan M, Prakash V, Vivekanandhan P, Subbiya A, Sukumaran VG (2016) Evaluation of surface roughness of three different composite resins with three different polishing systems. J Conserv Dent 19(2):171–174. https://doi.org/10.4103/0972-0707.178703
Acknowledgements
The authors thank Prof. Neslihan Arhun for her unwavering support at every stage of this study. The authors would also like to thank Orthero® Aligner Company and assistance from Aydın Dinkkulak in this study.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study design and conception. Sample preparation, data collection, and analysis were performed by S. Özsoy, H. Pamukçu, and E.M. Ateş. The first draft was written by S. Özsoy, H. Pamukçu, and Ö. Polat-Özsoy and all authors commented on previous versions of manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
S. Özsoy, H. Pamukçu, Ö. Polat-Özsoy and E.M. Ateş declare that they have no competing interests.
Ethical standards
This study was approved by Baskent University Institutional Review Board (project no: D‑KA 22/02) and supported by Baskent University Research Fund. Written informed consent from the patients who donated their teeth was collected at the beginning of the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Özsoy, S., Pamukçu, H., Polat-Özsoy, Ö. et al. Color changes of nanocomposites used for clear aligner attachments: an in vitro study. J Orofac Orthop 84 (Suppl 3), 266–275 (2023). https://doi.org/10.1007/s00056-023-00461-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00056-023-00461-7