Abstract
Background
In some regions, Aboriginal women have higher rates of cervical cancer compared to other Canadian women. However, little data are available regarding the co-factors of HPV infection in the Aboriginal population of Canada. We examined factors associated with high-risk human papillomavirus (HR-HPV) infection in a population of women (both Aboriginal and non-Aboriginal) in the Northwest Territories (NWT).
Methods
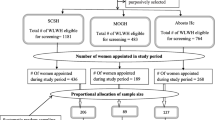
We used a cross-sectional design using a convenience sample of all women aged 14 years or older presenting for Papanicolaou (Pap) testing across all regions of the NWT from March 2009 to March 2010. Women answered a questionnaire on demographic characteristics, sexual behaviour, and gynaecological and obstetrical events. We used multiple regression analysis to explore factors associated with HR-HPV infection according to age and cultural background. HPV typing was done using the Luminex assay.
Results
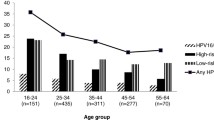
Of the total 1,279 participants, 178 had missing HPV results. We obtained data on 1,101 women and overall HR-HPV prevalence was 14.2%. Younger age, single marital status, Aboriginal background, current smoking, lifetime deliveries, use of hormonal contraceptives, and the numbers of sexual partners in the last year were associated with prevalent HR-HPV.
Discussion
Our findings tend to indicate that Aboriginal women have different predictors of HR-HPV than non-Aboriginal women that may affect HPV progression to cervical cancer. These findings can help to better target public health practices for the women at higher risk of HPV infection and cervical cancer.
Résumé
Contexte
Dans certaines régions, les taux de cancer du col utérin des femmes autochtones sont plus élevés que ceux des autres Canadiennes. Il existe cependant peu de données sur les cofacteurs de l’infection à VPH dans la population autochtone du Canada. Nous avons examiné les facteurs associés à un risque élevé d’infection par le virus du papillome humain à haut risque oncogène (VPH-HR) dans une population de femmes (autochtones et non-autochtones) des Territoires du Nord-Ouest (T.N.-O.).
Méthode
Nous avons mené une étude transversale auprès d’un échantillon de commodité de l’ensemble des femmes de 14 ans et plus s’étant présentées pour un test de Papanicolaou (frottis) dans toutes les régions des T.N.-O. entre mars 2009 et mars 2010. Ces femmes ont répondu à un questionnaire sur leur profil démographique, leur comportement sexuel et leurs événements gynécologiques et obstétriques. Au moyen d’une analyse de régression multiple, nous avons étudié les facteurs associés aux infections à VPH-HR selon l’âge et le milieu culturel. Le typage du VPH a été effectué à l’aide de dosages par Luminex.
Résultats
Sur les 1 279 participantes, 178 n’avaient pas de résultats pour le VPH. Nous avons donc obtenu des données sur 1 101 femmes, chez qui globalement la prévalence du VPH-HR était de 14,2 %. La jeunesse, le fait d’être célibataire, les antécédents autochtones, l’usage actuel du tabac, les accouchements durant la vie, l’utilisation de contraceptifs hormonaux et le nombre de partenaires sexuels au cours de la dernière année étaient associés aux infections à VPH-HR prévalentes.
Discussion
Nos constatations tendent à indiquer que les prédicteurs du VPH-HR chez les femmes autochtones sont différents de ceux des femmes non autochtones, ce qui peut influer sur l’évolution du VPH en cancer du col utérin. Ces constatations pourraient contribuer à mieux cibler les pratiques de santé publique à l’égard des femmes plus vulnérables à l’infection à VPH et au cancer du col utérin.
Similar content being viewed by others
References
Canadian Cancer Society’s Steering Committee on Cancer Statistics. Canadian Cancer Statistics 2011. Toronto, ON: Canadian Cancer Society, 2011.
Bosch FX, Lorincz A, Munoz N, Meijer CJ, Shah KV. The causal relationship between human papillomavirus and cervical cancer. J Clin Pathol 2002;55:244–65.
Marrett LD, Chaudhry M. Cancer incidence and mortality in Ontario First Nations, 1968–1991 (Canada). Cancer Causes Control 2003;14:259–68.
Young TK, Kliewer E, Blanchard J, Mayer T. Monitoring disease burden and preventive behavior with data linkage: Cervical cancer among Aboriginal people in Manitoba, Canada. Am J Public Health 2000;90(9):1466–68.
Louchini R, Beaupré M. Cancer incidence and mortality among Aboriginal people living on reserves and Northern villages in Québec, 1988–2004. Int J Circumpolar Health 2008;67:445–51.
Circumpolar Inuit Cancer Review Working Group, Kelly J, Lanier A, Santos M, Healey S, Louchini R, et al. Cancer among the Circumpolar Inuit, 1989-2003: Patterns and trends. Int J Circumpolar Health 2008;67(5):408–20.
Canadian Partnership Against Cancer. 2010 System Performance Report. Canadian Partnership Against Cancer, November 2010.
Annual Population Estimates by Community & Other Characteristics of the Northwest Territories. NWT Bureau of Statistics, 2009. Available at: https://doi.org/www.stats.gov.nt.ca/Statinfo/Demographics/population/popest.htlm (Accessed November 14, 2011).
Jiang Y, Brassard P, Severini A, Goleski V, Santos M, Leamon A, et al. Type-specific prevalence of human papillomavirus infection among women in the Northwest Territories, Canada. J Infect Public Health 2011;4(5-6):219–27.
Franco EL, Duarte-Franco E, Ferenczy A. Cervical cancer: Epidemiology, prevention and the role of human papillomavirus infection. CMAJ 2001;164:1017–25.
Hamlin-Douglas LK, Coutlee F, Roger M, Hanley J, Franco EL, Brassard P. Determinants of human papillomavirus infection among Inuit women of Northern Quebec, Canada. Sex Transm Dis 2001;37(6):377–81.
Bosch XF, Qiao Y, Castellsagué X. The epidemiology of human papillomavirus infection and its association with cervical cancer. Int J Gynaecol Obstet 2006;94:8–21.
Special Report: Policy. The Lancet 2009;10(4):321–22. Available at: https://doi.org/www.the-lancet.com/oncology (Accessed November 14, 2011).
Luminex xMAP Technology. Luminex Corporation, 2010. Available at: https://doi.org/www.luminexcorp.com/(Accessed November 14, 2011).
Zubach V, Smart G, Ratnam S, Severini A. Novel microsphere-based method for detection and typing of 46 mucosal human papillomavirus types. J Clin Microbiol 2012;50(2):460. DOI: 10.1128/JCM.06090-11.
Rebbapragada A, Perusini S, Di Prima A, Salit I, Goleski V, Ratnam S, et al. Evaluation of test performance characteristics and operational parameters of 5 hpv genotyping assays. 26th International Papillomavirus Conference, Montreal, QC, July 3–8, 2010.
Statistics Canada, 2006 Census. Population by Age and Gender Northwest Territories & Canada. 2006. Available at: https://doi.org/www.stats.gov.nt.ca/census/2006/Age%20and%20Sex_2006.pdf (Accessed November 14, 2011).
Molano M, Posso H, Weiderpass E, van den Brule AJ, Ronderos M, Franceschi S, et al. Prevalence and determinants of HPV infection among Colombian women with normal cytology. Br J Cancer 2002;87(3):324–33.
Kasap B, Yetimalar H, Keklik A, Yildiz A, Cukurova K, Soylu F. Prevalence and risk factors for human papillomavirus DNA in cervical cytology. Eur J Obstet Gynecol Reprod Biol 2011;159(1):168–71.
Hildesheim A, Gravitt P, Schiffman MH, Kurman RJ, Barnes W, Jones S, et al. Determinants of genital human papillomavirus infection in low-income women in Washington, D.C. Sex Transm Dis 1993;20(5):279–85.
Demers AA, Kliewer EV, Remes O, Onysko J, Dinner K, Wong T, Jayaraman GC. Cervical cancer among Aboriginal women in Canada. CMAJ 2012;184(7):743–44.
Elias B, Kliewer EV, Hall M, Demers AA, Turner D, Martens P, et al. The burden of cancer risk in Canada’s indigenous population: A comparative study of known risks in a Canadian region. Int J Gen Med 2011;4:699–709.
Author information
Authors and Affiliations
Corresponding author
Additional information
Acknowledgements: This study was financially supported by the Government of Canada International Polar Year Program and the Public Health Agency of Canada. P. Brassard was supported by a clinician scientist career award from the Fonds de la Recherche en Santé du Quebec (FRSQ).
Conflict of Interest: None to declare.
Rights and permissions
About this article
Cite this article
Brassard, P., Jiang, Y., Severini, A. et al. Factors Associated With Human Papillomavirus Infection Among Women in the Northwest Territories. Can J Public Health 103, e282–e287 (2012). https://doi.org/10.1007/BF03404236
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03404236