Abstract
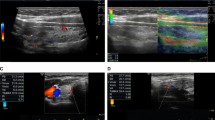
Amiodarone-induced thyrotoxicosis (AIT) is a life-threatening condition, the appropriate management of which is achieved by identifying its different subtypes. Type 1 AIT develops in patients with underlying thyroid abnormalities and is believed to be due to increased thyroid hormone synthesis and release; Type 2 AIT occurs in patients with a normal thyroid gland and is an amiodarone-induced destructive process of the thyroid. Management differs in the two forms of AIT, since Type 1 usually responds to combined thionamides and potassium perchlorate therapy, while Type 2 is generally responsive to glucocorticoids. Mixed forms, characterized by coexistence of excess thyroid hormone synthesis and destructive phenomena, may require a combination of the two therapeutic regimens. In this cross-sectional prospective study, 55 consecutive untreated patients, whose AIT was subtyped according to clinical and biochemical criteria, were evaluated to assess the specificity of color flow doppler sonography (CFDS) and thyroidal radioiodine uptake (RAIU) in the differential diagnosis of AIT. Sixteen patients (6 men, 10 women, age 66±13 yr), who had diffuse or nodular goiter with or without circulating thyroid autoantibodies, were classified as Type 1 AIT; 39 patients (27 men, 12 women, age 65±13 yr) with apparently normal thyroids were classified as Type 2 AIT. All Type 1 patients had normal or increased thyroidal vascularity on CFDS, while Type 2 AIT patients had absent vascularity (p<0.0001). Thirteen Type 1 AIT patients had inappropriately normal or elevated thyroidal 3-h and 24-h RAIU values (range 6–37% and 10–58%, respectively), in spite of elevated values of urinary iodine excretion; the remaining 3 patients (two with nodular goiter, one with a thyroid adenoma) had low 3-h and 24-h RAIU values (range 1.1–3.0% and 0.9–4.0%, respectively). The latter patients, who were unresponsive to the combination of methimazole and potassium perchlorate, became euthyroid after the addition of glucocorticoids. Thirty-eight Type 2 AIT patients had low 3-h and 24-h RAIU values (range 0.4–3.7% and 0.2–3.0%, respectively), but one had inappropriately normal 3-h and 24-h RAIU values (6% and 13%, respectively).
In conclusion, CFDS can accurately distinguish between Type 1 and Type 2 AIT, and in general the CFDS pattern is concordant with the thyroid RAIU. However, in 4 out of 55 patients (7%) the thyroid RAIU was discrepant, probably reflecting the coexistence of Type 1 and Type 2 AIT. Thus, assessment of both CFDS and RAIU may provide a more accurate subtyping of AIT and help in selecting the appropriate therapy. Finally, in long standing iodine sufficient areas, such as the United States, where the thyroid RAIU is consistently low irrespective of the etiology of the AIT, CFDS offers a rapid and available method to differentiate between Type 1 and Type 2 AIT.
Similar content being viewed by others
References
Martino E, Bartalena L, Bogazzi F, Braverman LE. Amiodarone and the thyroid. Endocr Rev 2001, 22: 240–54.
Bartalena L, Bogazzi F, Braverman LE, Martino E. Effects of amiodarone administration during pregnancy of neonatal thyroid function and subsequent neurodevelopment. J Endocrinol Invest 2001, 4: 116–30.
Wiersinga WM. Amiodarone and the thyroid. In: Weetman AP, Grossman A eds. Pharmacotherapeutics of the thyroid gland. Berlin: Springer-Verlag 1997, 225–87.
Iudica-Souza C, Burch HB. Amiodarone-induced thyroid dysfunction. The Endocrinologist 1999, 9: 216–27.
Thorne SA, Barnes I, Cullinan P, Somerville J. Amiodaroneinduced thyroid dysfunction. Risk factors in adults with congenital heart disease. Circulation 1999, 100: 149–54.
Bartalena L, Brogioni S, Grasso L, Bogazzi F, Burelli A, Martino E. Treatment of amiodarone-induced thyrotoxicosis, a difficult challenge: results from a prospective study. J Clin Endocrinol Metab 1996, 81: 2930–3.
Bartalena L, Bogazzi F, Martino E. Amiodarone-induced thyrotoxicosis: a difficult diagnostic and therapeutic challenge. Clin Endocrinol (Oxf) 2002, 56: 23–4.
Farwell AP, Abend SL, Huang SK, Patwardhan NA, Braverman LE. Thyroidectomy for amiodarone-induced thyrotoxicosis. JAMA 1990, 263: 1526–8.
Bogazzi F, Aghini-Lombardi F, Cosci C, et al. Iopanoic acid rapidly controls Type 1 amiodarone-induced thyrotoxicosis prior to thyrodectomy. J Endocrinol Invest 2002, 25: 176–80.
Bogazzi, F, Bartalena, L, Brogioni, S, et al. Color flow doppler sonography rapidly differentiates Type 1 and Type 2 amiodarone-induced thyrotoxicosis. Thyroid 1997, 7: 541–5.
Eaton SEM, Euinton HA, Newman CM, Weetman AP, Bennet WM. Clinical experience of amiodarone-induced thyrotoxicosis over a 3 yr period: role of colour-flow doppler sonography. Clin Endocrinol (Oxf) 2002, 56: 33–8.
Rago T, Vitti P, Chiovato L, et al. Role of conventional ultrasonography and color flow-doppler sonography in predicting malignancy in ‘cold’ thyroid nodules. Eur J Endocrinol 1998, 138: 41–6.
Vitti P, Rago T, Mazzeo S, et al. Thyroid blood flow evaluation by color-flow doppler sonography distinguishes Graves’ disease from Hashimoto’s thyroiditis. J Endocrinol Invest 1995, 18: 857–61.
Bogazzi F, Bartalena L, Vitti P, Rago T, Brogioni S, Martino E. Color flow doppler sonography in thyrotoxicosis factitia. J Endocrinol Invest 1996, 19: 603–6.
Bogazzi F, Bartalena L, Brogioni S, et al. Thyroid vascularity and blood flow are not dependent on serum thyroid hormone levels: studies in vivo by color flow doppler sonography. Eur J Endocrinol 1999, 140: 452–6.
Rago T, Chiovato L, Aghini-Lombardi F, Grasso L, Pinchera A, Vitti P. Non-palpable thyroid nodules in a borderline iodine sufficient area: detection by ultrasonography and follow-up. J Endocrinol Invest 2001, 24: 770–6.
Trip MD, Wiersinga WM. Incidence, predictability, and pathogenesis of amiodarone-induced thyrotoxicosis and hypothyroidism. Am J Med 1991, 91: 603–6.
Martino E, Aghini-Lombardi F, Bartalena L, et al. Enhanced susceptibility to amiodarone-induced hypothyroidism in patients with thyroid autoimmune disease. Arch Intern Med 1994, 154: 2722–6.
Leger AF, Massin JP, Laurent MF. Iodine-induced thyrotoxicosis: analysis of eighty-five consecutive cases. Eur J Clin Invest 1984, 14: 449–57.
Wimpfheimer C, Staubli M, Schadelin J, Studer H. Prednisone in amiodarone-induced thyrotoxicosis. BMJ 1982, 284: 1835–6.
Broussolle C, Ducottet X, Martin C, et al. Rapid effectiveness of prednisone and thionamides combined therapy in severe amiodarone iodine-induced thyrotoxicosis. Comparison of two groups of patients with apparently normal thyroid glands. J Endocrinol Invest 1989, 12: 37–42.
Bonnyns M, Sterling I, Renard M. Dexamethasone treatment of amiodarone-induced thyrotoxicosis (AIT) with or without persistent administration of the drug. Acta Cardiol 1989, 44: 235–43.
Martino E, Aghini-Lombardi F, Mariotti S, et al. Treatment of amiodarone associated thyrotoxicosis by simultaneous administration of potassium perchlorate and methimazole. J Endocrinol Invest 1986, 9: 201–7.
Roti E, Minelli R, Gardini E, Bianconi L, Braverman LE. Thyrotoxicosis followed by hypothyroidism in patients treated with amiodarone. Arch Intern Med 1993, 153: 886–92.
Williams M, Lo Gerfo P. Thyrodectomy using local anesthesia in critically ill patients with amiodarone-induced thyrotoxicosis: a review and description of the technique. Thyroid 2002, 12: 523–5.
Schwartz AE, Clark OH, Ituarte P, Lo Gerfo P. Therapeutic controversy: thyroid surgery —the choice. J Clin Endocrinol Metab 1988, 83: 1097–105.
Osman F, Franklyn JA, Sheppard MC, Gammage MD. Succesfull treatment of amiodarone-induced thyrotoxicosis. Circulation 2002, 105: 1275–7.
Martino E, Safran M, Aghini-Lombardi F, et al. Enviromental iodine intake and thyroid dysfunction during chronic amiodarone therapy. Ann Intern Med 1984, 101: 28–34.
Daniels GH. Amiodarone-induced thyrotoxicosis. J Clin Endocrinol Metab 2001, 86: 3–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bogazzi, F., Martino, E., Dell’Unto, E. et al. Thyroid color flow doppler sonography and radioiodine uptake in 55 consecutive patients with amiodarone-induced thyrotoxicosis. J Endocrinol Invest 26, 635–640 (2003). https://doi.org/10.1007/BF03347021
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03347021