Summary
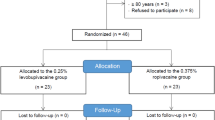
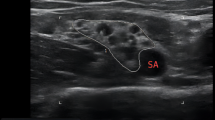
In this study, the pharmacokinetics, tolerability and efficacy of 40 ml of ropivacaine 7.5 mg/ml (300 mg) for axillary brachial plexus block were investigated. With institutional review board approval, 10 patients presenting for surgery of the upper limb were enrolled in this open study. The axillary plexus was identified with a nerve stimulator and the study drug was injected into the neurovascular sheath. Fifteen venous blood samples were obtained from each patient for pharmacokinetic measurements over a 24-h period. All blocks were sufficient for surgery after 45 min without any need for supplemental analgesia or general anesthesia. The mean (SD) peak plasma concentration was 2.3 (0.8) mg/l at median tmax 54 min (range 16–92 min). The mean (SD) maximum free plasma concentration was calculated to be 0.12 (0.06) mg/l (range 0.07–0.29 mg/l). The t1/2 was about 6 h. There were no clinical signs or symptoms of central nervous system and/or cardiac toxicity in any patient. Ropivacaine 7.5 mg/ml, used in a dose of 300 mg, was effective and well tolerated for axillary brachial plexus block.
Similar content being viewed by others
References
Åkerman B, Hellberg IB, Trossvik C. (1988) Primary evaluation of the local anaesthetic properties of the amino amide agent ropivacaine (LEA 103). Acta Anaesthesiol Scand; 32: 571–578.
Arthur GR, Feldman HS, Covino BG. (1988) Comparative pharmacokinetics of bupivacaine and ropivacaine, a new amide local anesthetic. Anesth Analg; 67: 1053–1058.
Scott DB, Lee A, Fagan D, Bowler GM, Bloomfield P, Lundh R. (1989) Acute toxivity of ropivacaine compared with that of bupivacaine. Anesth Analg; 69: 563–569.
Knudsen K, Beckman Suurküla M, Blomberg S, Sjövall J, Edvardsson N. (1997) Central nervous and cardiovascular effects of i.v. infusions of ropivacaine, bupivacaine and placebo in volunteers. Brit J Anaesth; 78: 507–514.
Hickey R, Candido KD, Ramamurthy S, Winnie AP, Blanchard J, Raza SM, Hoffman J, Durrani Z, Masters RW. (1990) Brachial plexus block with a new local anesthetic: 0.5 per cent ropivacaine. Can J Anaesth; 37:732–738.
Hickey R, Hoffman J, Ramamurthy S. (1991) A comparison of ropivacaine 0.5% and bupivacaine 0.5% for brachial plexus block. Anesthesiology; 74:639–642.
Hickey R, Rowley CL, Candido KD, Hoffman J, Ramamurthy S, Winnie AP. (1992) A comparative study of 0.25% ropivacaine and 0.25% bupivacaine for brachial plexus block. Anesth Analg; 75: 602–606.
Tryba M, Zenz M, Thole H, Pern U (1997) Ropivacaine 0.5% vs Ropivacaine 0.25% for axillary brachial plexus anesthesia-a double blind study. Anesthesiology; 77: Suppl A891.
Vainionpää VA, Haavisto ET., Huha TM, Korpi KJ, Nuutinen LS, Hollmén AI, Jozwiak HM, Magnusson Å (1995). A clinical and pharmacokinetic comparison of ropivacaine and bupivacaine in axillary plexus block. Anesth Analg; 81: 534–538.
Raeder JC, Drösdahl S, Klaastad Ö, Kvalsvik O, Isaksen B, Strömskag KE, Mowinckel P, Bergheim R, Selander D. (1999) Axillary branchial plexus block with ropivacaine 7.5 mg/ml. A comparative study with bupivacaine 5 mg/ml. Acta Anaesthesiol Scand; 43: 794–798.
Björk M, Pettersson KJ, Österlöf G. (1990) Capillary gas chromatographic method for the simultaneous determination of local anaesthetics in plasma samples. J Chromatogr; 533: 229–234.
Arvidsson T, Eklund E. (1995) Determination of free concentration of ropivacaine and bupivacaine in blood plasma by ultrafiltration and coupled-column liquid chromatography. J Chromatogr B Biomed Appl; 668: 91–98.
Mancini G, Carbonara AO, Heremans JF. (1965) Immunochemical quantitation of antigens by single radial immunodiffusion. Immunochemistry; 2: 235–254.
Lee A, Fagan D, Lamont M, Tucker GT, Halldin M, Scott DB. (1989) Disposition kinetics of ropivacaine in humans. Anesth Analg; 69: 736–738.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Wank, W., Büttner, J., Maier, K.R. et al. Pharmacokinetics and efficacy of 40 ml ropivacaine 7.5 mg/ml (300 mg), for axillary brachial plexus block — an open pilot study. Eur. J. Drug Metab. Pharmacokinet. 27, 53–59 (2002). https://doi.org/10.1007/BF03190406
Received:
Issue Date:
DOI: https://doi.org/10.1007/BF03190406