Summary
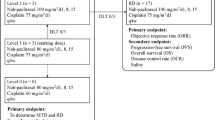
Survival in patients with locally advanced (stage III Mo) and metastatic (M1) non-small-cell lung cancer (NSCLC) is short. Phase II studies have reported objective responses ranging from 20% to 60% using cisplatin-based chemotherapeutic regimens, yet few have shown improvement in median survival. In our phase II pilot studies with cisplatin (CDDP) and etoposide (VP-16), we observed a 26% response rate; with CDDP, VP-16, and mitomycin-C, a 38% response rate was obtained in advanced NSCLC patients. A total of 156 consecutive patients with locally advanced and metastatic NSCLC were randomized to one of three treatment arms to determine whether the chemotherapy protocols had any effect on response rate and median survival in a large, randomized study. Arm 1 consisted of CDDP (120 mg/m2 × 3 weeks); arm 2, of CDDP (120 mg/m2) and VP-16 (100 mg/m2 given i.v. on days 1–3), repeated every 3 weeks; and arm 3, of CDDP (120 mg/m2) and VP-16 (100 mg/m2 on days 1–3) given every 3 weeks, plus mitomycin C (10 mg/m2 on days 1, 21, and 42, then every 6 weeks, for a maximal dose of 100 mg). After 71 patients had been enrolled in the study, we stopped accrual in the CDDP arm due to a lack of response [1 complete response (CR) in 24 patients; 4%] and continued enrollment in the two combination-chemotherapy arms. In the CDDP/VP-16 arm a 30% response rate [1 CR, 18 partial responses (PRs)] was obtained, and in the CDDP/VP-16 mitomycin C arm a 26% response rate (4 CRs, 11 PRs) was seen among a total of 150 evaluable patients. Responses were observed in 31% of patients with favorable performance status (PS) (ECOG 0–1) vs 14% in patients with a poor PS (ECOG 2–3). Of patients with locally advanced disease (III Mo), 17 (33%) obtained an objective response, compared with 20 patients (20%) with metastatic disease. Median survival was 18 weeks in the CDDP arm, 35 weeks in the CDDP/VP-16 arm, and 37 weeks in the CDDP/VP-16/mitomycin C arm. The median survival in the multimodal chemotherapy arms was significantly greater than that obtained with CDDP alone. Toxicity was predominantly myelosuppression in the mitomycin C-containing arm (27%, wtto grade 3–4). Our study shows that combination chemotherapy using CDDP/VP-16 is active and safe in the treatment of advanced NSCLC patients with a good performance status. The addition of mitomycin C did not improve the therapeutic response.
Similar content being viewed by others
References
Bonomi P (1986) Brief overview of combination chemotherapy in non-small cell lung cancer. Semin Oncol 8: 89–91
Cartei G (1988) Evaluation of synergy with cisplatin in non-small lung cancer: interim report from a multicenter study. Proc Am Soc Clin Oncol 7: 198
Davis S, Tonato M, Crinò L, Colozza M, Lubansky K, Grignani F (1986) Cisplatin, etoposide and mitomycin in the treatment of non-small cell lung cancer. Cancer 58: 1018–1021
Eagan RT, Fleming TR, Shoonover V (1979) Evaluation of response criteria in advanced lung cancer. Cancer 44: 1125–1128
Einhorn LH, Loeher PJ, Williams DS, Meyers S, Gabrys T, Nattan SR, Woodburn R, Drasga R, Songer J, Fisher W, Stephens D, Hui S (1986) Random prospective study of vindesine vs vindesine plus high-dose cisplatin vs vindesine plus cisplatin plus mitomycin C in advanced non-small cell lung cancer. J Clin Oncol 4: 1037–1043
Elliot JA, Ahmedzai S, Hole D, Dorward AJ, Stevenson RD, Kage SB, Banham SW, Stack BHR, Calman KC (1984) Vindesine and cisplatin combination chemotherapy compared with vindesine as a single agent in the management of non-small cell lung cancer. A randomized study. Eur J Cancer Clin Oncol 20: 1025–1032
Finkelstein DM, Ettinger DS, Ruckdeschel JC (1986) Long term survivors in metastatic non-small cell lung cancer: an ECOG study. J Clin Oncol 4: 702–709
Gralla RJ, Casper ES, Kelsen DP, Braun DW, Dukeman ME, Martini N, Young CW, Golbey RB (1981) Cisplatin and vindesine combination chemotherapy for advanced carcinoma of the lung: a randomized trial investigating two dosage schedules. Ann Intern Med 95: 414–420
Hansen HH (1987) Advanced non-small cell lung cancer: to treat or not to treat? J Clin Oncol 5: 1711–1712
Hayniuk W, Bush H (1984) The importance of dose intensity in chemotherapy of metastatic breast cancer. J Clin Oncol 2: 1281–1288
Lanzotti VJ, Thomas DR, Boyle LE, Smith LT, Gehan EA, Samuels ML (1977) Survival with inoperable lung cancer. An integration of prognostic variables based on simple clinical criteria. Cancer 39: 303–313
Mountain CF (1986) A new international staging system for lung cancer. Chest 89 (suppl 4): 225–233
Mountain CF, Carr DT, Anderson WAS (1979) Staging of lung cancer 1979. American Joint Committee for Cancer, Staging and End Results Reporting. Task Force on Lung Cancer, Chicago
Mulshine JL, Gatstein E, Ruckdeschel JC (1986) Treatment of non-small cell lung cancer. J Clin Oncol 4: 1704–1715
Rapp E, Pater JL, Wilan A, Cormier Y, Murray N, Evans KW, Hodson ID, Clark DA, Feld R, Arnold AM, Ajoub JI, Wilson KS, Latreille J, Wierzbicki RF, Hill DP (1988) Chemotherapy can prolong survival in patients with advanced non-small cell lung cancer. Report of a Canadian multicenter trial. J Clin Oncol 6: 633–641
Ruckdeschel JC, Finkelstein DM, Ettinger DS, Creech RH, Mason BA, Joss RA, Vogl S (1986) A randomized trial of the four most active regimens for metastatic non-small cell lung cancer. J Clin Oncol 4: 14–22
Williams CJ, Woods R, Levi J, Page J (1988) Chemotherapy for non-small cell lung cancer: a randomized trial of cisplatin/vindesine vs no chemotherapy. Seminars in Oncology 15 (suppl 7): 58–61
Author information
Authors and Affiliations
Additional information
Published in part in Seminars in Oncology, suppl., Dec. 88 in the proceedings of the Perugia International Cancer Conference I
Professore’ A. Contratto, Université di Perugia
Rights and permissions
About this article
Cite this article
Crino, L., Tonato, M., Darwish, S. et al. A randomized trial of three cisplatin-containing regimens in advanced non-small-cell lung cancer (NSCLC): a study of the Umbrian Lung Cancer Group. Cancer Chemother Pharmacol 26, 52–56 (1990). https://doi.org/10.1007/BF02940294
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02940294