Abstract
Purpose
Omentin-1 plays an important role in regulating insulin sensitivity outside pregnancy. As an adipokine derived from human placental and adipose tissue, it may be an important contributor in the biological pathway of gestational diabetes.
Methods
Omentin-1 was measured in a sub-cohort of 50 participants in the Omega study.
We aimed to evaluate whether circulating maternal omentin-1 concentrations are associated with fasting serum glucose, insulin, HOMA-IR and maternal obesity as measured by body mass index (BMI) and subcutaneous and intra-abdominal fat thickness measurements in normoglycemic pregnant participants. We performed a subgroup analysis by BMI category.
Results
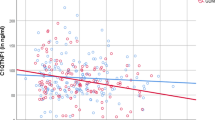
Omentin-1 was negatively correlated with HOMA-IR and insulin and inversely associated with serum glucose concentration in the fully adjusted model (− 47%; slope per tertile increase in concentration − 0.19; P-trend 0.01). This association was significant in non-overweight/obese (< 25 kg/m2) but not among overweight/obese (≥ 25 kg/ m2) participants. The association with serum insulin was not significant in the fully adjusted model.
Conclusion
Circulating omentin-1 concentrations are inversely associated with serum glucose concentrations. Although the relevance of these findings remains to be elucidated, they may indicate a mechanism for the development of insulin resistance and gestational diabetes. Follow-up studies with larger sample sizes are warranted.

Similar content being viewed by others
References
Cunningham FL, Bloom KJ, Hauth SL, Rouse JC, Spong DJ, CY Williams Obstetrics, ed. (2010) M.H. 23nd ed. USA
Hill M (2005) Mater Physiol 107–31.
Badon SE et al (2017) Healthy lifestyle during early pregnancy and risk of gestational diabetes mellitus. Am J Epidemiol 186(3):326–333
Ruchat SM, Hivert MF, Bouchard L (2013) Epigenetic programming of obesity and diabetes by in utero exposure to gestational diabetes mellitus. Nutr Rev 71(Suppl 1):S88–S94
Fasshauer M, Bluher M, Stumvoll M (2014) Adipokines in gestational diabetes. Lancet Diabetes Endocrinol 2(6):488–499
Bozkurt L et al (2018) Adiponectin and leptin at early pregnancy: association to actual glucose disposal and risk for gdm-a prospective cohort study. Int J Endocrinol 2018:5463762
Ouchi N et al (2011) Adipokines in inflammation and metabolic disease. Nat Rev Immunol 11(2):85–97
Catalano PM et al (2006) Adiponectin in human pregnancy: implications for regulation of glucose and lipid metabolism. Diabetologia 49(7):1677–1685
Ahlsson F et al (2013) Adipokines and their relation to maternal energy substrate production, insulin resistance and fetal size. Eur J Obstet Gynecol Reprod Biol 168(1):26–29
Ortega-Senovilla H et al (2011) Gestational diabetes mellitus causes changes in the concentrations of adipocyte fatty acid-binding protein and other adipocytokines in cord blood. Diabetes Care 34(9):2061–2066
Saucedo R et al (2011) Relationship between circulating adipokines and insulin resistance during pregnancy and postpartum in women with gestational diabetes. Arch Med Res 42(4):318–323
de Gennaro G et al (2019) The role of adipokines in the pathogenesis of gestational diabetes mellitus. Gynecol Endocrinol 35(9):737–751
Abell SK et al (2017) The association between dysregulated adipocytokines in early pregnancy and development of gestational diabetes. Diabetes Metab Res Rev 33(8):e2926
Bellos I et al (2019) Serum levels of adipokines in gestational diabetes: a systematic review. J Endocrinol Invest 42(6):621–631
Franz M et al (2018) Maternal and neonatal omentin-1 levels in gestational diabetes. Arch Gynecol Obstet 297(4):885–889
Aktas G et al (2014) Association between omentin levels and insulin resistance in pregnancy. Exp Clin Endocrinol Diabetes 122(3):163–166
Kafalidis G et al (2013) Adipokines vaspin and omentin-1 are up-regulated in large for gestational age infants at term. Cytokine 62(1):70–74
Brandt B et al (2015) Omentin, an adipokine with insulin-sensitizing properties, is negatively associated with insulin resistance in normal gestation. J Perinat Med 43(3):325–331
Schaffler A et al (2005) Genomic structure of human omentin, a new adipocytokine expressed in omental adipose tissue. Biochim Biophys Acta 1732(1–3):96–102
Yang RZ et al (2006) Identification of omentin as a novel depot-specific adipokine in human adipose tissue: possible role in modulating insulin action. Am J Physiol Endocrinol Metab 290(6):E1253–E1261
Pan HY, Guo L, Li Q (2010) Changes of serum omentin-1 levels in normal subjects and in patients with impaired glucose regulation and with newly diagnosed and untreated type 2 diabetes. Diabetes Res Clin Pract 88(1):29–33
Tan BK et al (2008) Omentin-1, a novel adipokine, is decreased in overweight insulin-resistant women with polycystic ovary syndrome: ex vivo and in vivo regulation of omentin-1 by insulin and glucose. Diabetes 57(4):801–808
de Souza Batista CM et al (2007) Omentin plasma levels and gene expression are decreased in obesity. Diabetes 56(6):1655–1661
Pan X et al (2019) Omentin-1 in diabetes mellitus: a systematic review and meta-analysis. PLoS ONE 14(12):e0226292
As Habi A et al (2019) The association between omentin and diabetes: a systematic review and meta-analysis of observational studies. Diabetes Metab Syndr Obes 12:1277–1286
Rudra CB et al (2008) A prospective analysis of recreational physical activity and preeclampsia risk. Med Sci Sports Exerc 40(9):1581–1588
Matthews DR et al (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28(7):412–419
Armellini F et al (1990) The contribution of sonography to the measurement of intra-abdominal fat. J Clin Ultrasound 18(7):563–567
Armellini F et al (1993) Total and intra-abdominal fat measurements by ultrasound and computerized tomography. Int J Obes Relat Metab Disord 17(4):209–214
Elsaid NH et al (2018) Serum omentin-1 levels in type 2 diabetic obese women in relation to glycemic control, insulin resistance and metabolic parameters. J Clin Transl Endocrinol 13:14–19
Cai RC et al (2009) Expression of omentin in adipose tissues in obese and type 2 diabetic patients. Zhonghua Yi Xue Za Zhi 89(6):381–384
Komosinska-Vassev K et al (2019) Circulating C1q/TNF-related protein 3, Omentin-1 and NGAL in obese patients with type 2 diabetes during insulin therapy. J Clin Med 8(6):805
Yan P et al (2011) Changes of serum omentin levels and relationship between omentin and adiponectin concentrations in type 2 diabetes mellitus. Exp Clin Endocrinol Diabetes 119(4):257–263
Tan BK et al (2008) Decreased plasma omentin-1 levels in Type 1 diabetes mellitus. Diabet Med 25(10):1254–1255
Motawi TMK et al (2018) Serum levels of chemerin, apelin, vaspin, and omentin-1 in obese type 2 diabetic Egyptian patients with coronary artery stenosis. Can J Physiol Pharmacol 96(1):38–44
Dayem SM, Battah AA, Shehaby AE (2015) Cardiac affection in type 1 diabetic patients in relation to Omentin. Open Access Maced J Med Sci 3(4):699–704
Nurten E et al (2018) Omentin-1 and NAMPT serum concentrations are higher and CK-18 levels are lower in children and adolescents with type 1 diabetes when compared to healthy age, sex and BMI matched controls. J Pediatr Endocrinol Metab 31(9):959–969
Barker G et al (2012) Omentin-1 is decreased in maternal plasma, placenta and adipose tissue of women with pre-existing obesity. PLoS ONE 7(8):e42943
Briana DD et al (2011) Omentin-1 and vaspin are present in the fetus and neonate, and perinatal concentrations are similar in normal and growth-restricted pregnancies. Metabolism 60(4):486–490
Tsiotra PC et al (2018) Circulating adipokines and mRNA expression in adipose tissue and the placenta in women with gestational diabetes mellitus. Peptides 101:157–166
Moreno-Navarrete JM et al (2011) Circulating omentin as a novel biomarker of endothelial dysfunction. Obesity (Silver Spring) 19(8):1552–1559
Auguet T et al (2011) New adipokines vaspin and omentin. Circulating levels and gene expression in adipose tissue from morbidly obese women. BMC Med Genet 12:60
Tang YL et al (2017) Circulating omentin-1 levels in women with polycystic ovary syndrome: a meta-analysis. Gynecol Endocrinol 33(3):244–249
Lamain-de Ruiter M et al (2017) Prediction models for the risk of gestational diabetes: a systematic review. Diagn Progn Res 1:3
Funding
No funding was obtained for this study.
Author information
Authors and Affiliations
Contributions
SP: project development, data analysis, manuscript writing. BG: project development, data collection, manuscript writing. MW: project development, data collection, manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors do not have conflicts of interest or financial disclosures.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Papatheodorou, S., Gelaye, B. & Williams, M.A. Association between omentin-1 and indices of glucose metabolism in early pregnancy: a pilot study. Arch Gynecol Obstet 305, 589–596 (2022). https://doi.org/10.1007/s00404-021-06197-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-021-06197-2